Many epidemiological studies of breastfeeding in developed countries have found a relationship between socioeconomic status and duration of breastfeeding.1-5
In a previous study, using data from the 1995 Australian National Health Survey (NHS),6 we demonstrated that a considerable socioeconomic gradient existed in Australia, both for initiation of breastfeeding and for rates of breastfeeding at 6 months.7 At 6 months, 37.4% (95% CI, 32.5%–42.3%) of infants in the most disadvantaged socioeconomic quintile were breastfed, compared with 52.7% (95% CI, 47.8%–57.6%) in the least disadvantaged quintile.
In the past few years, three other national surveys in Australia have included questions about breastfeeding — the 20018 and 2004–059 NHSs and the Longitudinal Study of Australian Children.10
The measure of socioeconomic status used in our analysis was the Index of Relative Socio-economic Disadvantage (IRSD), based on the area of residence of the child. The IRSD, which includes measures of income, education and occupational status, is part of the Socio-Economic Indexes for Areas (SEIFA) classification.11 Subjects were allocated to one of five SEIFA categories, from the lowest quintile (areas having the lowest incomes and highest proportion of unskilled workers) to the highest quintile (areas having the highest incomes and highest proportion of professional/skilled workers). The IRSD is a summary measure of general socioeconomic conditions in a census collection district, based on data from the latest available census. IRSD scores are standardised by the Australian Bureau of Statistics to have a mean of 1000 and a standard deviation of 100 across all collection districts in Australia. The distribution of index scores is generally similar across the states, except that the Northern Territory has a higher proportion of disadvantaged areas and the Australian Capital Territory has a lower proportion of disadvantaged areas than Australia as a whole.12 The SEIFA classification was the only measure of socioeconomic status that could be validly compared across the three NHSs.
There was little change in the initiation and duration of breastfeeding between the 1995 and 2004–05 NHSs in Australia (Box 1). The overall breastfeeding initiation rate was 86.0% in 1995 compared with 87.8% in 2004–05. In 1995, the overall proportions of infants breastfeeding at 3, 6 and 12 months were 63.1%, 46.6% and 21.3%, respectively, compared with 64.4%, 50.4% and 23.3% in 2004–05.
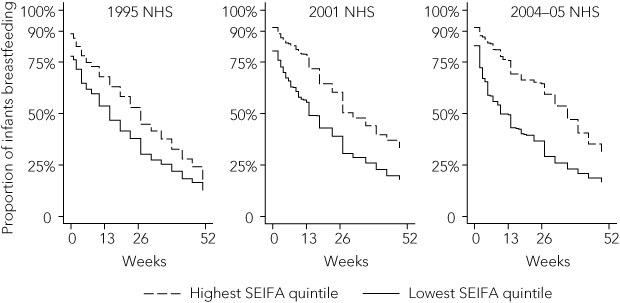
In 1995, for each increase in SEIFA quintile, the odds of breastfeeding at 6 months increased by 13% (odds ratio [OR], 1.13 [95% CI, 1.07–1.19]), whereas in 2001, the comparative odds increased by 21% (OR, 1.21 [95% CI, 1.12–1.30]), and in 2004–05, the comparative odds increased by 26% (OR, 1.26 [95% CI, 1.17–1.36]). Similar gradients were observed for breastfeeding at 3 months and 12 months. The widening difference in breastfeeding rates according to SEIFA category between 1995 and 2004–05 is presented graphically in Box 2.
In general, people with higher incomes are more likely to adopt healthy behaviour such as exercising, eating a healthy diet and quitting smoking.13-15 Lower-income families have less capacity to make such changes. Women from lower-income families are less likely to breastfeed for a number of reasons, including less family support for breastfeeding, less ability to seek help with breastfeeding problems, less flexibility with working arrangements, and concerns about breastfeeding in public.16-19 Moreover, women in lower SEIFA quintiles are more likely to interact socially with women who are less inclined to breastfeed, such as those who are younger, less educated, overweight/obese or smokers.20-22 As formula-fed infants are more likely to become ill and be admitted to hospital, these findings indicate increasing health inequalities in Australian children.23
Policymakers need to act on increasing health inequalities.14 Breastfeeding support and promotion in Australia need to focus on groups with low rates of breastfeeding. Peer support programs have been effective in other countries24,25 and should be trialled in Australia. Peer support involves women who are similar to the women they are supporting — for example, teenage women supporting teenage women. The Australian Breastfeeding Association provides mother-to-mother support, but as the counsellors tend to be middle-class and are trained to provide breastfeeding advice, they are not peer supporters as generally defined.
The previous federal government proposed a “community education campaign on the benefits of breastfeeding”.26 However, the health benefits of breastfeeding are widely known and we believe it would be more useful to conduct a public education campaign aimed at the wider community — not just new parents — which includes promotion of breastfeeding in public in an acceptable way to groups that are currently uncomfortable with this issue.17,27 New mothers need support from their families, communities and workplaces in order to breastfeed. They need Baby Friendly accredited maternity hospitals,28 increased breastfeeding help in the community and paid maternity leave — not simply another government campaign extolling the virtues of breastfeeding.
1 Weighted estimates of proportions of infants breastfeeding in the 1995, 2001 and 2004–05 Australian National Health Surveys (NHSs), by SEIFA quintile
Proportion (% [95% CI]) of infants |
|||||||||||||||
SEIFA = Socio-Economic Indexes for Areas.11 * Lowest quintile has lowest incomes and highest proportion of unskilled workers. † For 2001 and 2004–05, the timepoints available in the confidentialised unit record file (CURF) were 13 weeks (3 months), 26 weeks (6 months) and 52 weeks (12 months). For 1995, the closest corresponding timepoints available in the CURF were 13–16 weeks, 25–28 weeks and 49–52 weeks, respectively. |
|||||||||||||||
2 Breastfeeding duration: weighted estimates of proportions of infants breastfeeding at 0–52 weeks in the 1995, 2001 and 2004–05 National Health Surveys (NHSs) in the lowest and highest SEIFA quintiles*
 | |||||||||||||||
|
SEIFA = Socio-Economic Indexes for Areas.11 * Lowest quintile has lowest incomes and highest proportion of unskilled workers. | |||||||||||||||
Received 20 December 2007, accepted 13 March 2008
- Lisa H Amir1,2,3
- Susan M Donath4,5
- 1 Mother and Child Health Research, La Trobe University, Melbourne, VIC.
- 2 Medical One — QV, Melbourne, VIC.
- 3 Breastfeeding Education and Support Services, Royal Women’s Hospital, Melbourne, VIC.
- 4 Clinical Epidemiology and Biostatistics Unit, Murdoch Childrens Research Institute, Melbourne, VIC.
- 5 Department of Paediatrics, University of Melbourne, Royal Children’s Hospital, Melbourne, VIC.
None identified.
- 1. Ladomenou F, Kafatos A, Galanakis E. Risk factors related to intention to breastfeed, early weaning and suboptimal duration of breastfeeding. Acta Paediatr 2007; 96: 1441-1444.
- 2. Bonet M, Kaminski M, Blondel B. Differential trends in breastfeeding according to maternal and hospital characteristics: results from the French National Perinatal Surveys. Acta Paediatr 2007; 96: 1290-1295.
- 3. Taylor JS, Risica PM, Geller L, et al. Duration of breastfeeding among first-time mothers in the United States: results of a national survey. Acta Paediatr 2006; 95: 980-984.
- 4. Gudnadottir M, Gunnarsson BS, Thorsdottir I. Effects of sociodemographic factors on adherence to breastfeeding and other important infant dietary recommendations. Acta Paediatr 2006; 95: 419-424.
- 5. Li R, Darling N, Maurice E, et al. Breastfeeding rates in the United States by characteristics of the child, mother or family: the 2002 National Immunization Survey. Pediatrics 2005; 115: e31-e37.
- 6. Australian Bureau of Statistics. National Health Survey: users’ guide, 1995. Canberra: ABS, 1995. (ABS Cat. No. 4363.0.)
- 7. Donath S, Amir LH. Rates of breastfeeding in Australia by state and socioeconomic status: evidence from the 1995 National Health Survey. J Paediatr Child Health 2000; 36: 164-168.
- 8. Australian Bureau of Statistics. National Health Survey: users’ guide, 2001. Canberra: ABS, 2001. (ABS Cat. No. 4363.0.55.001.)
- 9. Australian Bureau of Statistics. National Health Survey: users’ guide, 2004–05. Canberra: ABS, 2006. (ABS Cat. No. 4363.0.55.001.)
- 10. Nicholson JM, Sanson A; LSAC Research Consortium. A new longitudinal study of the health and wellbeing of Australian children: how will it help? Med J Aust 2003; 178: 282-284. <MJA full text>
- 11. Australian Bureau of Statistics. Information paper: Census of Population and Housing: Socio-Economic Indexes for Areas, Australia, 2001. Canberra: ABS, 2001. (ABS Cat. No. 2039.0.) http://www.abs.gov.au/ausstats/abs@.nsf/allprimarymainfeatures/09D 68973F50B8258CA2573F0000DA181?opendocument (accessed Jul 2008).
- 12. Australian Bureau of Statistics. Information paper: Socio-Economic Indexes for Areas. Canberra: ABS, 1990. (ABS Cat. No 1356.0.)
- 13. Graham H. Socio-economic change and inequalities in men and women’s health in the UK. In: Nettleton S, Gustafsson U, editors. The sociology of health and illness reader. Cambridge: Polity Press, 2002: 240-255.
- 14. Marmot M. Social determinants of health inequalities. Lancet 2005; 365: 1099-1104.
- 15. Coveney J. A qualitative study exploring socio-economic differences in parental lay knowledge of food and health: implications for public health nutrition. Public Health Nutr 2005; 8: 290-297.
- 16. Mitra AK, Khoury AJ, Hinton AW, Carothers C. Predictors of breastfeeding intention among low-income women. Matern Child Health J 2004; 8: 65-70.
- 17. McIntyre E, Hiller JE, Turnbull D. Determinants of infant feeding practices in a low socio-economic area: identifying environmental barriers to breastfeeding. Aust N Z J Public Health 1999; 23: 207-209.
- 18. McIntyre E, Turnbull D, Hiller JE. Breastfeeding in public places. J Hum Lact 1999; 15: 131-135.
- 19. McIntyre E, Hiller JE, Turnbull D. Attitudes towards infant feeding among adults in a low socioeconomic community: what social support is there for breastfeeding? Breastfeed Rev 2001; 9: 13-24.
- 20. Amir LH, Donath SM. Does maternal smoking have a negative physiological effect on breastfeeding? The epidemiological evidence. Birth 2002; 29: 112-123.
- 21. Khoury AJ, Moazzem SW, Jarjoura CM, et al. Breast-feeding initiation in low-income women: role of attitudes, support, and perceived control. Womens Health Issues 2005; 15: 64-72.
- 22. Amir LH, Donath SM. A systematic review of maternal obesity and breastfeeding intention, initiation and duration. BMC Pregnancy Childbirth 2007; 7: 9.
- 23. James WP, Nelson M, Ralph A, Leather S. Socioeconomic determinants of health. The contribution of nutrition to inequalities in health. BMJ 1997; 314: 1545-1549.
- 24. Sikorski J, Renfrew MJ, Pindoria S, Wade A. Support for breastfeeding mothers: a systematic review. Cochrane Database Syst Rev 2002; (2): CD001141.
- 25. Dennis CL, Hodnett E, Gallop R, Chalmers B. The effect of peer support on breast-feeding duration among primiparous women: a randomized controlled trial. CMAJ 2002; 166: 21-28.
- 26. Australian Department of Health and Ageing. Health Budget 2007–2008. Breastfeeding — education and support. http://www.health.gov.au/internet/budget/publishing.nsf/Content/budget2007-hfact37.htm (accessed Jul 2008).
- 27. Boyd R, McIntyre E. Improving community acceptance of breastfeeding in public: a collaborative approach. Breastfeed Rev 2004; 12: 5-10.
- 28. Baby Friendly Health Initiative. Protecting, promoting and supporting breastfeeding in Australia. Current Baby Friendly accredited health services in Australia. http://www.bfhi.org.au/text/bfhi_hospitals.html (accessed Jul 2008).





Abstract
Objective: To investigate whether the relationship between socioeconomic status and breastfeeding initiation and duration changed in Australia between 1995 and 2004.
Design and setting: Secondary analysis of data from national health surveys (NHSs) conducted by the Australian Bureau of Statistics in 1995, 2001 and 2004–05. The Socio-Economic Indexes for Areas (SEIFA) classification was used as a measure of socioeconomic status.
Main outcome measures: Rates of initiation of breastfeeding; rates of breastfeeding at 3, 6 and 12 months.
Results: Between the 1995 and 2004–05 NHSs, there was little change in overall rates of breastfeeding initiation and duration. In 2004–05, breastfeeding initiation was 87.8%, and the proportions of infants breastfeeding at 3, 6 and 12 months were 64.4%, 50.4% and 23.3%, respectively. In 1995, the odds ratio (OR) of breastfeeding at 6 months increased by an average of 13% (OR, 1.13 [95% CI, 1.07–1.19]) for each increase in SEIFA quintile; in 2001, the comparative increase was 21% (OR, 1.21 [95% CI, 1.12–1.30]); while in 2004–05, the comparative increase was 26% (OR, 1.26 [95% CI, 1.17–1.36]). Breastfeeding at 3 months and 1 year showed similar changes in ORs. There was little change in the ORs for breastfeeding initiation.
Conclusion: Although overall duration of breastfeeding remained fairly constant in Australia between 1995 and 2004–05, the gap between the most disadvantaged and least disadvantaged families has widened considerably over this period.