Falls are a significant burden on the health care system, with a substantial proportion of the associated health care costs occurring in residential aged care facilities (RACFs).1 RACF residents have an elevated risk of falls due to high numbers of comorbidities; however, reduced physical activity,2 safer environments and increased supervision may actually reduce fall risk in this setting.3
Identifying people at risk of falls in RACFs is complex, and risk assessment tools developed for community and acute hospital settings cannot be translated to RACFs.4 Previous studies have shown that falls occur more frequently in mobile5,6 and physically active nursing home residents.7 As part of the Fracture Risk Epidemiology in the Elderly (FREE) study,3,8 we reported a non-linear association between standing balance and falls, with low fall rates in those with the worst balance as well as those with the best balance. The FREE study also found that many fall risk factors in those who could stand were either not evident or were actually protective in those who could not stand, further indicating that fall risk identification in RACF residents is not straightforward. None of the currently available screening tools for RACFs can be considered definitive for predicting residents at risk of falls, as they have not been adequately validated in large populations.
The study sample comprised 2005 people who took part in the FREE study between June 1999 and June 2003.3,8 Participants were recruited from randomly selected RACFs (898 participants from 80 nursing homes and 1107 participants from 50 intermediate-care hostels) in northern Sydney, New South Wales. The participation rate of eligible residents (ie, those not exclusively confined to bed) was 44.8% for nursing home residents and 55.2% for hostel residents. Participants were aged 65–104 years (mean ± SD, 85.7 ± 7.1 years), and 1532 (76.4%) were women. About half of the population (1033; 51.5%) had experienced at least one fall during the previous year.
Resident assessment by a research nurse, self-report, care provider interviews, and medical records were used to determine the presence of medical conditions. Medication use, urinary incontinence, falls history, and use of assistive devices were documented from residents’ medical records. Cognitive status was assessed with the Mini-Mental State Examination.9
Standing balance was assessed using a static balance test.10 Participants were classified into five grades: 1 = unable to stand on the floor for any period without support from another person or a walking aid; 2 = unable to maintain balance on the floor for 30 s; 3 = able to maintain balance on the floor for 30 s but unable to maintain balance on a medium-density foam rubber mat (70 cm × 60 cm × 15 cm thick) for any period of time; 4 = able to maintain balance on the floor but unable to maintain balance on the foam rubber mat for 30 s; and 5 = able to maintain balance when standing on the floor and the foam mat for 30 s each. Twelve residents did not complete the static balance test and were excluded from the analysis.
Participants’ sit-to-stand ability was measured by assessing their ability to rise from a standard-height (0.43 m) chair with arm rests.11 Participants were graded on a four-point scale: 1 = unable; 2 = able with the help of another person; 3 = able with the use of arm support; and 4 = able without the need for arm support.
All residents were followed up for a period of 6 months or until death, if sooner. Falls were ascertained from incident reports and medical records and were classified using the Kellogg definition.12 Forty-seven residents died within 3 months without having a fall and were excluded from the analysis.
Of the 1946 residents assessed, 813 (41.8%) fell once or more during the 6-month follow-up period. Of these, 410 fell twice or more, and 460 suffered at least one fall that resulted in an injury.2
Univariate analyses showed that the risk of experiencing at least one fall during the prospective period significantly increased with age, and was higher in nursing home residents and in those who had fallen in the past year. Factors associated with falls included poor static balance and sit-to-stand ability, greater illness severity, impaired cognitive status, Parkinson disease, urinary incontinence, knee osteoarthritis, use of a walking aid, and use of many medications (Box 1).
Stepwise logistic regression analysis identified four significant independent risk factors for falls: nursing home residence, impaired balance, a history of falls in the past year, and urinary incontinence (Box 2). In a second step, impaired balance was dichotomised based on examination of a receiver operating characteristic (ROC) curve as the inability to stand on a foam mat (static balance grades 2–3). The model significantly predicted falls (χ2 = 159.5, df = 4, P < 0.001) and accounted for 14% of the variance in faller status, with 80% of the non-fallers successfully predicted, 44% of the fallers successfully predicted, and 65% overall faller status successfully predicted.
Fewer risk factors were evident for the residents who could not stand unaided (Box 1). In this group, residents with a history of falls and those who were taking more medications had an increased risk of falls. Nursing home residence, increased care levels and reduced ability to rise from a chair were associated with fewer falls.
The logistic regression analysis identified three significant independent risk factors for falls: hostel residence, a history of falls in the past year, and use of many medications (Box 3). In a second step, the number of medications was dichotomised based on an ROC curve inspection, with the cut-off point at nine or more medications. The model significantly predicted falls (χ2 = 31.43, df = 3, P < 0.001) and accounted for 11% of the variance in faller status, with 97% of the non-fallers successfully predicted, 16% of the fallers successfully predicted, and 67% overall faller status successfully predicted.
Two fall risk screening models emerged from this study: one for people who could stand unaided and one for people who could not. The stronger model was achieved in people who could stand unaided. Having poor balance or a positive score for two of three other risk factors (previous falls, nursing home residence, and urinary incontinence) produced a threefold increased risk of falling in the next 6 months. These factors have consistently been identified as important risk factors for falls.3,8,13-17
The model in people who could not stand unaided was less robust. Having had a previous fall, using nine or more medications, or residing in a hostel were associated with a twofold increased risk of falling during the follow-up period. Thus, “standard” physical risk factors do not appear to be present in this subpopulation, in accordance with previous findings.3,6,15 Measures such as providing high-level care, using alarm devices, and regular medication review may be particularly beneficial for this group.
Several fall risk screening tools for residential care have previously been published.6,18 However, their small to moderate sample sizes (ranging between 78 and 472 participants), as well as the frequent use of univariate approaches, have been insufficient to produce validated tools with acceptable sensitivity–specificity ratios. One study undertaken in Germany used multivariate modelling, similar to our approach, to construct an algorithm for predicting falls in nursing homes.6 It found that falls history, vision impairment and incontinence were fall risk factors in residents able to transfer independently from bed to a standing position, compared with risk factors of falls history and restraint use in residents unable to transfer independently. Our study builds on this work by including hostel as well as nursing home residents and by including a simple balance assessment, which assists in identifying the more mobile people at risk of future falls. Our sample size was also sufficiently large to allow investigation of multiple measures and split-half validation. The resultant screening models are quick and easy to administer and require only one inexpensive and readily available piece of equipment (a 15 cm thick, medium-density foam rubber mat).
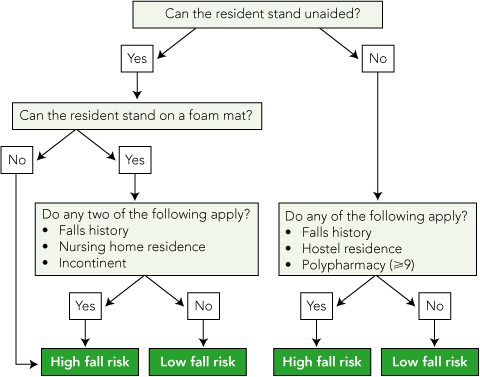
A simple algorithm, shown in Box 4, demonstrates how the screening models could be used in RACFs. By using them this way, only 56% of people who can stand unaided would need to be targeted to identify 75% of all fallers. Similarly, 77% of people who cannot stand unaided would need to be targeted to identify 87% of fallers. While these models assist in identifying most residents at risk of falls, we acknowledge that significant proportions of fallers would not be identified. Therefore, a multifaceted approach to fall prevention should be considered as part of routine care for all older people in RACFs.1 These care plans should include evidence-based strategies such as education of staff19-21 and residents,19 environmental modifications,19-21 regular medication reviews,20,21 and exercise to improve strength, balance, gait, safe transfers and walking aid use.19,20,22 Our screening model augments this care, not only by identifying residents most at risk, but also by providing information on risk factors to guide tailored intervention strategies.
As yet, no randomised controlled trials have been undertaken for fall prevention in RACFs in Australia, and disparate findings regarding the effectiveness of interventions have been published in other countries.19-23 This discordance likely reflects differences in what constitutes an RACF, staffing and casemix within RACFs, and study design and quality of interventions. The screening tools developed in this study have some clinical utility in terms of identifying at-risk fallers, but further work is required to tease out whether screening tools offer clinical efficacy and cost-effectiveness. In the absence of a consensus approach to routine assessment and intervention in RACFs, the suggested screening models offer these facilities the option of applying a validated tool to identify residents at high risk of falling.
1 Investigated risk factors for falls in people who could and could not stand unaided
Could stand unaided (n = 1569) |
Could not stand unaided (n = 377) |
||||||||||||||
Received 13 August 2007, accepted 12 March 2008
- Kim Delbaere1,2
- Jacqueline C T Close1
- Hylton B Menz3
- Robert G Cumming4
- Ian D Cameron4
- Philip N Sambrook4
- Lyn M March4
- Stephen R Lord1
- 1 Falls and Balance Research Group, Prince of Wales Medical Research Institute, University of New South Wales, Sydney, NSW.
- 2 Department of Experimental-Clinical and Health Psychology and Department of Rehabilitation Sciences and Physiotherapy, Ghent University, Ghent, Belgium.
- 3 Musculoskeletal Research Centre, Faculty of Health Sciences, La Trobe University, Melbourne, VIC.
- 4 Faculty of Medicine, University of Sydney, Sydney, NSW.
This research was conducted as part of the FREE study, which has been funded by a National Health and Medical Research Council (NHMRC) grant and the Arthritis Foundation of Australia. The analysis for this paper was funded by NSW Health. Hylton Menz is currently an NHMRC Clinical Career Development Research Fellow (ID 433049) and Stephen Lord is an NHMRC Senior Principal Research Fellow.
None identified.
- 1. Safety and Quality Council. Preventing falls and harm from falls in older people. Best practice guidelines for Australian hospitals and residential aged care facilities. Canberra: Australian Council for Safety and Quality in Health Care, 2005.
- 2. Tinetti ME. Factors associated with serious injury during falls by ambulatory nursing home residents. J Am Geriatr Soc 1987; 35: 644-648.
- 3. Lord SR, March LM, Cameron ID, et al. Differing risk factors for falls in nursing home and intermediate-care residents who can and cannot stand unaided. J Am Geriatr Soc 2003; 51: 1645-1650.
- 4. Oliver D, Masud T. Preventing falls and injuries in care homes. Age Ageing 2004; 33: 532-535.
- 5. Thapa PB, Brockman KG, Gideon P, et al. Injurious falls in nonambulatory nursing home residents: a comparative study of circumstances, incidence, and risk factors. J Am Geriatr Soc 1996; 44: 273-278.
- 6. Becker C, Loy S, Sander S, et al. An algorithm to screen long-term care residents at risk for accidental falls. Aging Clin Exp Res 2005; 17: 186-192.
- 7. Norton R, Galgali G, Campbell AJ, et al. Is physical activity protective against hip fracture in frail older people? Age Ageing 2001; 30: 262-264.
- 8. Chen JS, March LM, Schwarz J, et al. A multivariate regression model predicted falls in residents living in intermediate hostel care. J Clin Epidemiol 2005; 58: 503-508.
- 9. Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975; 12: 189-198.
- 10. Lord SR, Clark RD, Webster IW. Physiological factors associated with falls in an elderly population. J Am Geriatr Soc 1991; 39: 1194-1200.
- 11. Seaby L, Torrance G. Reliability of a physiotherapy functional assessment used in a rehabilitation setting. Physiother Can 1989; 41: 264-271.
- 12. Gibson MJ, Andres RO, Isaacs B, et al. The prevention of falls in later life. A report of the Kellogg International Work Group on the Prevention of Falls by the Elderly. Dan Med Bull 1987; 34 Suppl 4: 1-24.
- 13. Lord SR, Clark RD. Simple physiological and clinical tests for the accurate prediction of falling in older people. Gerontology 1996; 42: 199-203.
- 14. Ganz DA, Bao Y, Shekelle PG, Rubenstein LZ. Will my patient fall? JAMA 2007; 297: 77-86.
- 15. Thapa PB, Gideon P, Brockman KG, et al. Clinical and biomechanical measures of balance as fall predictors in ambulatory nursing home residents. J Gerontol A Biol Sci Med Sci 1996; 51: M239-M246.
- 16. Kiely DK, Kiel DP, Burrows AB, Lipsitz LA. Identifying nursing home residents at risk for falling. J Am Geriatr Soc 1998; 46: 551-555.
- 17. Perell KL, Nelson A, Goldman RL, et al. Fall risk assessment measures: an analytic review. J Gerontol A Biol Sci Med Sci 2001; 56: M761-M766.
- 18. Scott V, Votova K, Scanlan A, Close J. Multifactorial and functional mobility assessment tools for fall risk among older adults in community, home-support, long-term and acute care settings. Age Ageing 2007; 36: 130-139.
- 19. Becker C, Kron M, Lindemann U, et al. Effectiveness of a multifaceted intervention on falls in nursing home residents. J Am Geriatr Soc 2003; 51: 306-313.
- 20. Jensen J, Nyberg L, Rosendahl E, et al. Effects of a fall prevention program including exercise on mobility and falls in frail older people living in residential care facilities. Aging Clin Exp Res 2004; 16: 283-292.
- 21. Ray WA, Taylor JA, Meador KG, et al. A randomized trial of a consultation service to reduce falls in nursing homes. JAMA 1997; 278: 557-562.
- 22. Schnelle JF, Kapur K, Alessi C, et al. Does an exercise and incontinence intervention save healthcare costs in a nursing home population? J Am Geriatr Soc 2003; 51: 161-168.
- 23. Kerse N, Butler M, Robinson E, Todd M. Fall prevention in residential care: a cluster, randomized, controlled trial. J Am Geriatr Soc 2004; 52: 524-531.





Abstract
Objective: To develop screening tools for predicting falls in nursing home and intermediate-care hostel residents who can and cannot stand unaided.
Design and setting: Prospective cohort study in residential aged care facilities in northern Sydney, New South Wales, June 1999 – June 2003.
Participants: 2005 people aged 65–104 years (mean ± SD, 85.7 ± 7.1 years).
Main outcome measures: Demographic, health, and physical function assessment measures; number of falls over a 6-month period; validity of the screening models.
Results: Ability to stand unaided was identified as a significant event modifier for falls. In people who could stand unaided, having either poor balance or two of three other risk factors (previous falls, nursing home residence, and urinary incontinence) increased the risk of falling in the next 6 months threefold (sensitivity, 73%; specificity, 55%). In people who could not stand unaided, having any one of three risk factors (previous falls, hostel residence, and using nine or more medications) increased the risk of falling twofold (sensitivity, 87%; specificity, 29%).
Conclusions: These two screening models are useful for identifying older people living in residential aged care facilities who are at increased risk of falls. The screens are easy to administer and contain items that are routinely collected in residential aged care facilities in Australia.