Randomised controlled trials published in 1991 and 1992 from the United Kingdom1 and Hungary2 provided firm evidence that increased intake of folic acid in the periconceptional period — usually regarded as the month before pregnancy and the first 3 months of pregnancy — reduces the risk of having a baby with a neural tube defect (NTD) by about 72%. The Women’s and Children’s Hospital in Adelaide participated in the UK international trial, the results of which promised a rare opportunity for primary prevention of a group of severe birth defects.
Many countries started to promote periconceptional folate intake by informing women that their risk of having a baby with an NTD could be reduced if they consumed 0.4 mg of folic acid daily (or 0.5 mg, the content of the tablet in Australia) in the periconceptional period. The amount recommended is greater than the median amount of folic acid (0.2 mg) consumed daily by Australian women of reproductive age3 and difficult to achieve by diet alone. Western Australia started promoting folate in 1992.4 The South Australian campaign in October 1994 to August 1995, coordinated by the Women’s and Children’s Hospital and the South Australian Department of Health (SA Health), provided information about folate and the prevention of NTDs to health professionals and the community.5
In 1995, voluntary fortification of specified foods with folic acid was approved in Australia, allowing up to 50% of the recommended daily intake of folic acid (ie, 0.1 mg) to be added per reference quantity (generally, a normal serving or equivalent specified quantity). From 1996, increasing numbers of foods were fortified with folic acid, mainly breakfast cereals, fruit juices and milk. The Women’s and Children’s Hospital has continued to distribute folate information sheets and has a folate telephone message, and occasionally disseminates newspaper and television messages. The personal health record provided by child health services for each baby at birth and SA Health’s pregnancy information website (http://www.health.sa.gov.au/PREGNANCY/DesktopDefault.aspx?tabid=45) also contain information about folate. The Australian Government began promoting folate in September 1997.
In this report, we document changes in knowledge about folic acid’s role in the prevention of NTDs among women of reproductive age, and changes in the prevalence of NTDs in a state with a previously stable total prevalence in 1966–1991.6
Surveys of about 400 women of reproductive age in each year from 1994 to 1996 to evaluate the “Folate before pregnancy” promotion campaign.
A 1998 survey involving 2077 women, including 292 who were pregnant or had given birth in the preceding 3 years.7
A 2001 survey of 923 women, including 159 who were pregnant or had given birth in the preceding 3 years.8
The South Australian Monitoring and Surveillance System (SAMSS), implemented by SA Health in July 2002 to monitor population trends in key health issues on a regular monthly basis through about 600 CATI interviews per month9 (509–730 women in the reproductive age group each year in the years 2003–2007).
Pregnancies resulting in births of babies with NTDs were ascertained from the South Australian perinatal data collection of births (live births and stillbirths of at least 400 g birthweight or 20 weeks’ gestation), which have been required to be notified to SA Health under legislation since 1986. Terminations of pregnancy for NTDs were ascertained from notifications under specific abortion legislation introduced in 1970.6 The South Australian Birth Defects Register10 collates all these data, including rare cases detected late (before the child’s fifth birthday). Cases of NTDs are validated through review of perinatal and postneonatal death certificates; medical, ultrasound, maternal serum screening, cytogenetics and autopsy reports; and, where necessary, case records and consultation with the clinicians and/or pathologists involved.
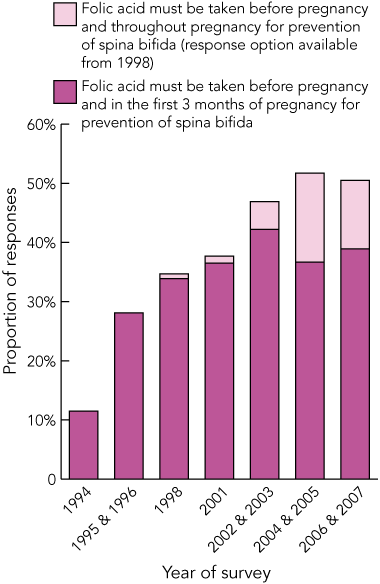
The response rate in the CATI surveys ranged from 65% to 75%. Box 1 shows that the proportion of women of reproductive age who were aware of the role of folic acid in the prevention of NTDs (specifically, spina bifida) increased from 25.5% in 1994 to 77.0% in 2006 and 2007 (χ2 test for trend for individual years, 432.76; P < 0.001). Box 2 shows that the proportion of women who knew that folate should be taken before pregnancy and in the first 3 months of pregnancy for prevention of spina bifida increased from 11.5% in 1994 to 38.9% in 2006 and 2007 (χ2 test for trend, 69.60; P < 0.001). As a few women in the surveys in earlier years responded “before and throughout pregnancy”, this response option was available from 1998 and is shown in Box 2.
Box 3 shows that, among women who were pregnant or who had recently given birth, an increasing proportion increased their daily consumption of any form of folate in the periconceptional period, from 60.6% in 1998 to 81.1% in 2006 and 2007 (χ2 test for trend, 18.74; P < 0.001). The proportion who consumed cereals fortified with folic acid increased from 14.5% to 28.9% (χ2 test for trend, 15.14; P < 0.001) and those consuming folic acid tablets increased from 37.2% to 63.7% (χ2 test for trend, 33.66; P < 0.001). However, the proportion who increased their intake of folate-rich foods showed no significant trend during this period, from 40.7% to 32.6% (χ2 test for trend, 1.53; P = 0.22).
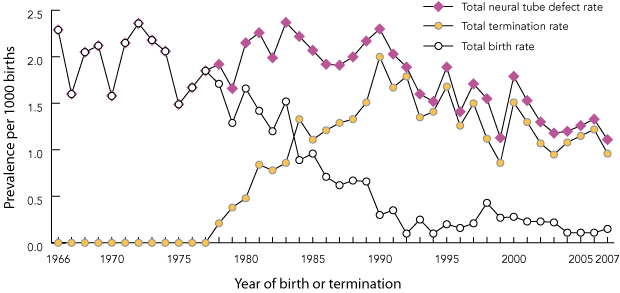
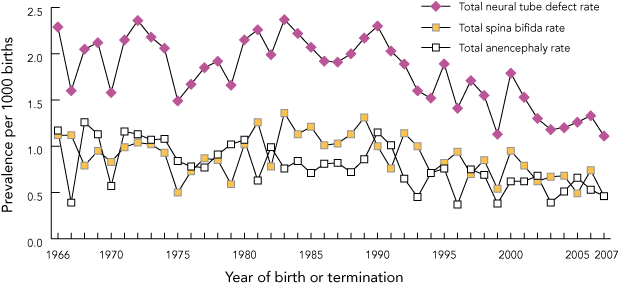
Box 4 and joinpoint analysis (Joinpoint Regression Program, version 3.3; Statistical Research and Applications Branch, National Cancer Institute, Bethesda, Md, USA) show that the prevalence of all NTDs in South Australia was stable between 1966 and 1990 and declined significantly thereafter (Poisson regression 1966 to 2007, P < 0.001). Box shows that this decline also applied individually to anencephaly (P < 0.001) and spina bifida (P < 0.01).
Two studies of folic acid intake among pregnant women attending clinics at teaching hospitals in Adelaide have been undertaken.11,12 They showed lower levels of full compliance with the consumption of folic acid tablets in the periconceptional period than did the CATI surveys of the population — 31% in 199911 and 30% in 2005.12 However, an additional 13% of women in 199911 and 43% in 200512 reported that they had tried to comply, but took lower-dosage tablets or did not take tablets for the full period. The levels of knowledge and use of folic acid supplements were high in these young pregnant public patient populations. The 1998 CATI survey, which asked about the type of folic acid tablets, also showed that some women took tablets (usually multivitamins) containing less than 0.4 mg of folic acid.7 Many of these women may have achieved an adequate daily level of 0.4 mg by consuming fortified cereals or increasing their intake of folate-rich foods.
The CATI surveys showed that folate awareness was lower among women from non-English-speaking countries, those residing in rural areas and those with low household income.7-9 Studies elsewhere have also shown that knowledge is associated with older age, non-immigrant status, higher education, marriage, and planned pregnancy.13 It is estimated that over 40% of pregnancies in many countries are unplanned,5,13 and evaluations performed after folate promotion projects have found that not more than 50% of women are taking periconceptional folic acid supplements.4,13
Almost no decline in total prevalence of NTDs has been observed in most European countries after folate promotion projects.13 However, in South Australia, with folate promotion from many sources and voluntary fortification, the total prevalence fell by 40% between 1986–1990 and 2002–2007.
Mandatory fortification has now been implemented in over 40 countries. It has been associated with falls in the prevalence of NTDs in Canada (46%, ranging from 22% to 83% in different provinces),14 Chile (31%),15 Costa Rica (35% among births)16 and in the United States (20% to 32%, from several monitoring programs).17 In the US, mean daily food and total folate intake increased by about 0.1 mg per day after fortification. Among women of reproductive age, 26% to 39% (varying by race or ethnicity) achieved more than 0.4 mg daily intake of folate.17
While some have called for higher levels of fortification with folic acid18,19 and additional fortification with vitamin B12,18 others have recommended a more cautious approach,20 advising that significant reductions have already been achieved in the prevalence of low levels of serum and red-cell folate. Moreover, monitoring programs with better case ascertainment have shown a 50% reduction in prevalence of NTDs after mandatory food fortification with folate;21 a lack of data on terminations of pregnancy to determine total NTD prevalence may result in underestimates of effect. The amount by which NTD prevalence can be reduced is also dependent on the initial prevalence14,22 and on the proportion of folate-responsive cases.23
We look forward in Australia to a further reduction in NTD prevalence with mandatory food fortification, which was gazetted in September 2007 and will be enforceable in September 2009.24 It is unlikely that reduction beyond a residual level of about 0.6 NTD-affected fetuses per 1000 births can be achieved, this being the lowest level achieved internationally.22,25 There are also needs to monitor safety, including possible effects on those on anti-folate therapy, to monitor other effects such as those on cardiovascular disease risk and cancer, and issues surrounding fortification of foods with vitamin B12.
1 Knowledge that folate may prevent spina bifida if enough is taken by the mother, among women of reproductive age, South Australia, 1994–2007
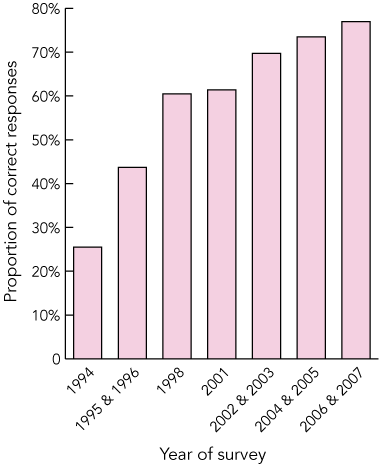
2 Knowledge of the timing of folate supplementation among women of reproductive age, South Australia, 1994–2007
3 Increase in folate intake and source of increased intake among women who had been pregnant within the previous 3 years, South Australia, 1998–2007
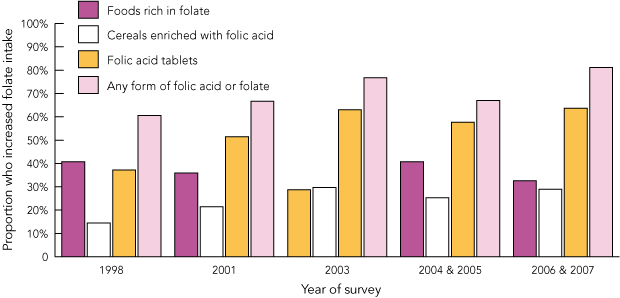
- Annabelle C Chan1,2
- Phillipa van Essen3
- Heather Scott3
- Eric A Haan3,2
- Leonie Sage1
- Joan Scott1
- Tiffany K Gill1
- Anh-Minh T Nguyen1
- 1 SA Health, Government of South Australia, Adelaide, SA.
- 2 School of Paediatrics and Reproductive Health, University of Adelaide, Adelaide, SA.
- 3 South Australian Birth Defects Register, Children, Youth and Women’s Health Service, Women’s and Children’s Hospital Campus, Adelaide, SA.
We thank South Australian midwives, neonatal nurses, doctors and hospital staff for providing perinatal and termination data, and women who participated in the surveys. We thank the Children, Youth and Women’s Health Service for continuing folate promotion.
None identified.
- 1. MRC Vitamin Study Research Group. Prevention of neural tube defects: results of the Medical Research Council vitamin study. Lancet 1991; 338: 131-137.
- 2. Czeizel AE, Dudas I. Prevention of the first occurrence of neural-tube defects by periconceptional vitamin supplementation. N Engl J Med 1992; 327: 1832-1835.
- 3. Australian Bureau of Statistics. National nutrition survey: nutrient intakes and physical measurements, Australia, 1995. Canberra: ABS, 1998. (ABS Cat. No. 4805.0.) http://www.abs.gov.au/ausstats/ abs@.nsf/Lookup/95E87FE64B144FA3CA2568A9001393C0 (accessed Oct 2008).
- 4. Bower C, Blum L, O’Daly K, et al. Promotion of folate for the prevention of neural tube defects: knowledge and use of periconceptional folic acid supplements in Western Australia, 1992 to 1995. Aust N Z J Public Health 1997; 21: 716-721. (erratum: Aust N Z J Public Health 1998; 22: 72.)
- 5. Chan A, Pickering J, Haan EA, et al. “Folate before pregnancy”: the impact on women and health professionals of a population-based health promotion campaign in South Australia. Med J Aust 2001; 174: 631-636.
- 6. Chan A, Robertson EF, Haan EA, et al. Prevalence of neural tube defects in South Australia 1966–91; effectiveness and impact of prenatal diagnosis. BMJ 1993; 307: 703-706.
- 7. Taylor A, Dal Grande E, Starr G, Woollacott T. South Australian Health Goals and Targets Health Priority Areas Survey 2. Folate/spina bifida. Adelaide: South Australian Department of Human Services, 1999. https://www.library.health.sa.gov.au/Portals/0/sa-health-goals-and-targets-health-priority-areas-survey-2-folate-spina-bifida.pdf (accessed Oct 2008).
- 8. Dal Grande E, Gill T, Taylor A. Folate and spina bifida. Adelaide: South Australian Department of Human Services, 2002. http://www.health.sa.gov.au/pros/portals/0/folate-report-01.pdf (accessed Oct 2008).
- 9. South Australian Monitoring and Surveillance System (SAMSS). SAMSS Technical Paper Series No 1/04, August 2004. Survey methodology. Adelaide: South Australian Department of Health, 2004. http://www.health.sa.gov.au/pros/portals/0/samss-tech-paper1-method.pdf (accessed Oct 2008).
- 10. 2005 Annual Report of the South Australian Birth Defects Register. Children born from 1986 to 2005 with birth defects notified to the Register by 31st March 2006, and incorporating the Annual Report of Prenatal Diagnosis in South Australia, 2005. Adelaide: Children, Youth and Women’s Health Service, Women’s and Children's Hospital, 2008. http://www.wch.sa.gov.au/services/az/divisions/labs/geneticmed/documents/2005_sabdr_annual_report.pdf (accessed Oct 2008).
- 11. Henry A, Crowther C. Universal periconceptional folate supplementation: chasing a dream [letter]? Med J Aust 2000; 172: 407-408.
- 12. Conlin ML, MacLennan AH, Broadbent JL. Inadequate compliance with periconceptional folic acid supplementation in South Australia. Aust N Z J Obstet Gynaecol 2006; 46: 528-533.
- 13. Eichholzer M, Tonz O, Zimmermann R. Folic acid: a public health challenge. Lancet 2006; 367: 1352-1361.
- 14. De Wals P, Tairou F, Van Allen MI, et al. Reduction of neural-tube defects after folic acid fortification in Canada. N Engl J Med 2007; 357: 135-142.
- 15. Castilla EE, Orioli IM, Lopez-Carmelo JS, et al; for the ECLAMC. Latin American Collaborative Study of Congenital Malformations. Preliminary data on changes in neural tube defect prevalence rates after folic acid fortification in South America. Am J Med Genet A 2003; 123A: 123-128.
- 16. Chen LT, Rivera MA. The Costa Rican experience: reduction of neural tube defects following food fortification programs. Nutr Rev 2004; 62 (6 Pt 2): S40-S43.
- 17. Bentley TGK, Willett WC, Weinstein MC, et al. Population-level changes in folate intake by age, gender, and race/ethnicity after folic acid fortification. Am J Public Health 2006; 96: 2040-2047.
- 18. Brent RL, Oakley GP. The Food and Drug Administration must require the addition of more folic acid in “enriched” flour and other grains. Pediatrics 2005; 116: 753-755.
- 19. Wald NJ, Law MR, Morris JK, et al. Quantifying the effect of folic acid. Lancet 2001; 358: 2069-2073.
- 20. Rader JI, Schneeman BO. Prevalence of neural tube defects, folate status, and folate fortification of enriched cereal-grain products in the United States. Pediatrics 2006; 117: 1394-1399.
- 21. Mills JL, Signore C. Neural tube defect rates before and after fortification with folic acid. Birth Defects Res A Clin Mol Teratol 2004; 70: 844-845.
- 22. Berry RJ, Li Z, Erickson JD, et al. Prevention of neural tube defects with folic acid in China. N Engl J Med 1999; 341: 1485-1490.
- 23. Kirke PN, Mills JL, Molloy AM, et al. Impact of the MTHFR C677T polymorphism on risk of neural tube defects: case–control study. BMJ 2004; 328: 1535-1536.
- 24. Food Standards Australia New Zealand. Amendment No. 93 (FSC 35). 13 September 2007. http://www.foodstandards.gov.au/standardsdevelopment/gazettenotices/amendment9313septemb3695.cfm (accessed Oct 2008).
- 25. Ray JG, Meier C, Vermeulen MJ, et al. Association of neural tube defects and folic acid food fortification in Canada. Lancet 2002; 360: 2047-2048.





Abstract
Objectives: To ascertain changes in: women’s knowledge of the role of folic acid in the prevention of neural tube defects (NTDs); intake of folic acid among pregnant women; and prevalence of NTDs in South Australia.
Design, setting and participants: Computer-assisted telephone interviews of South Australian households from 1994 to 2007 over a period encompassing a statewide folate promotion campaign (1994–1995), continuing folate promotion, as well as the introduction of voluntary folate fortification of foods (1996); ascertainment of the total prevalence of NTDs from births and terminations of pregnancy from 1966 to 2007.
Main outcome measures: Changes in women’s knowledge of the role of folic acid in the prevention of NTDs; changes in the prevalence of NTDs.
Results: From 1994 to 2006 and 2007, knowledge about the role of folic acid increased from 25% to 77% (P < 0.001) and knowledge that folic acid needs to be taken in the periconceptional period increased from 12% to 39% (P < 0.001). The proportion of pregnant women who increased their periconceptional intake of folate rose from 61% in 1998 to 81% in 2006 and 2007 (P < 0.001), with significant increases in the consumption of fortified cereals (from 15% to 29%) and folic acid tablets (from 37% to 64%). The total prevalence of NTDs fell from 2.06 per 1000 births in 1986–1990 to 1.23 per 1000 births in 2002–2007 (relative risk, 0.60; 95% CI, 0.48–0.74; P < 0.001).
Conclusions: Folate promotion and voluntary fortification of certain foods with folic acid were associated with increased awareness of the role of periconceptional folic acid, increased folate consumption and a reduction in the prevalence of NTDs in South Australia by 40% (95% CI, 26%–52%).