Patients with symptoms of a transient ischaemic attack (TIA) have an annual stroke risk of 1%–15%.1 Almost half the subsequent strokes occur in the first month after the TIA.2-4 The Northern California cohort study found a 10.5% risk of stroke after 90 days, with 50% of patients suffering a stroke within 2 days of the initial symptoms.2
When patients with TIA present to an emergency department (ED), the decision whether to admit them for assessment and treatment is based on the clinician’s perception of both the stroke risk and the benefits of admission. The choice may depend on the quality and availability of outpatient TIA services. Best care of TIA has been uncertain, although recent studies suggest early comprehensive assessment and treatment effectively reduce subsequent stroke and stroke unit admissions.5,6 Highly resourced and rapidly accessible acute TIA clinics are rare: only 10% of Australian hospitals currently offer outpatient TIA services.7 At most locations, rapid and comprehensive assessment of TIA is available only through hospitalisation.
Risk scoring systems, including the Californian and ABCD2 scores, were developed to identify TIA patients most likely to benefit from rapid assessment and treatment.8-10 Initial studies in the United States and United Kingdom suggest that high, moderate or low risk of subsequent stroke can be determined by age, blood pressure, and duration and type of TIA symptoms, particularly limb weakness.8-10 The benefit of scales such as ABCD2 to aid admission or discharge decisions in Australia remains uncertain.
The study was conducted in a large defined metropolitan and rural region of Sydney and its surroundings, the South Western Sydney Area Health Service (SWSAHS), which has since been amalgamated into the Sydney South West Area Health Service. In 2001, the region had a population of 796 95011 served by six public hospitals: a principal referral hospital (Liverpool Hospital), and three metropolitan and two rural hospitals. Two of the six offered acute specialised neurological inpatient care during the study period. There were 825 541 ED attendances in the region between January 2001 and December 2005.
Patients at Liverpool Hospital were further investigated to determine the in-hospital stroke rate and to investigate any association between ABCD2 score and the decision to admit or discharge the patient. All ED TIA presentations were matched with the hospital’s separation records, using the person identifier and arrival date. Medical records of all admitted patients who had an ICD-10-AM separation diagnosis of stroke were reviewed to confirm that stroke occurred during the hospital admission. In addition, all available electronic ED files were obtained from the ED Information System for ED TIA patients and reviewed for stroke risk factors as a basis for calculating an ABCD2 score.8
Box 1 shows the adjusted logistic regression analysis for the two groups in the two follow-up periods. The discharged group had higher occurrence of stroke, recurrent TIA and all events (stroke and TIA) combined in the first 28 days after TIA than the admitted group. However, there was no significant difference in occurrence of stroke, recurrent TIA or all events combined between the two groups over the 29-day to 1-year follow-up period. Overall, the cumulative 1-year event rate (stroke or TIA) was 7.33% for the admitted group and 9.46% for the discharged group (odds ratio [OR], 1.3; 95% CI, 0.98–1.7; P = 0.10).
Further analysis by selected patient and hospital characteristics is shown in Box 2. Patients in MOS Categories 4 and 5 (discharged group) had a significantly higher event recurrence at 28 days compared with those in MOS Category 1 (admitted to ward). No significant differences were found in event recurrence for the other selected characteristics, except age 55–64 years for recurrence within 28 days (P = 0.02) and widowed marital status for recurrence at Day 29 to 1 year (P = 0.03). Nor did the presence of a neurology department in the hospital significantly affect event recurrence.
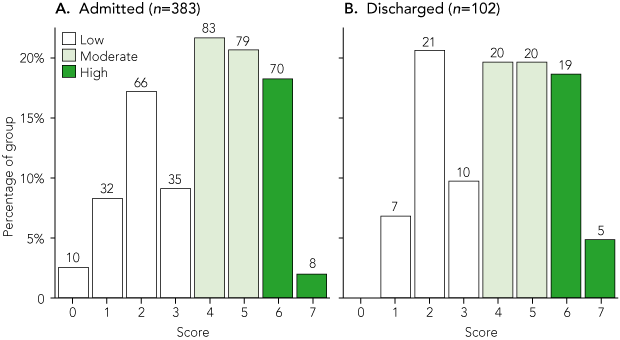
ABCD2 scores were calculated for 383 (71%) of the patients admitted to Liverpool Hospital and 102 (68%) of those discharged from the ED. No difference was found between the admitted and discharged groups in the proportions with low, moderate or high stroke risk (Box 3). Among those with moderate–high risk (ABCD2 ≥ 4), 28-day all event (TIA or stroke) recurrence was 8/64 (13%) in those who were discharged compared with 5/240 (2%) in those who were admitted (OR, 6.7; 95% CI, 2.0–17.7; P < 0.001). As there were no recurrences in the discharged group after 28 days, no difference between groups was evident at 12 months. In patients with low risk (ABCD2 score ≤ 3), the 28-day all event recurrence rate did not differ between groups: 3/143 (2%) in the admitted group compared with 1/38 (3%) in the discharged group.
Further investigation of patients at Liverpool Hospital identified only one admitted patient who had an in-hospital stroke, suggesting a very low risk of early stroke with hospital admission. The higher recurrence of early stroke or TIA in discharged patients was not explained by higher ABCD2 scores in this group, as the distribution of low, moderate and high risk scores was similar in the admitted and discharged groups. Among patients with a moderate–high risk ABCD2 score (≥ 4), those discharged had a significantly higher 28-day rate of stroke or TIA recurrence than those admitted.
A likely reason for the poor early outcomes of the discharged group is delay or omission of appropriate investigation and treatment. Admitted patients are more likely to receive early comprehensive investigation and early initiation of stroke prevention measures, including investigation-guided antithrombotic choices, treatment of vascular risk factors, and intensive lifestyle modification. Early comprehensive investigation and treatment appears to account for improved TIA outcomes in two recent, single-centre studies of outpatient TIA services in the UK and France.5,6
US and UK guidelines recommend TIA patients be assessed and investigated within 7 days.12,13 Many of our discharged group had TIA recurrence or stroke within 2 days (as has been previously reported2), and thus a 7-day window before intervention may be too long for optimal benefit. Our study suggests that direct hospital admission delivers favourable early outcomes for TIA. Referral to a rapidly accessible and comprehensive TIA service or clinic,5,6 possibly guided by risk stratification, may be an alternative to hospital admission. However, the type of quickly accessible and heavily resourced TIA services assessed in these two studies5,6 are rare in Australia. Further studies, preferably multicentre and randomised, are needed to address the relative benefit of comprehensive emergency TIA clinics versus urgent hospital admission. Until then, the perception that TIA patients can be safely discharged from the ED may be inappropriate.
The usual caveats for a non-randomised, observational and retrospective study apply to our results, including a risk of bias. In any TIA study, the proportion of TIA mimics is likely to be significant,14-16 and the subsequent proportion of stroke events is dictated by the proportion of mimics. Accuracy of medical record coding of TIA as a diagnosis is a potential confounder. There is no highly sensitive or specific diagnostic test to determine whether TIA symptoms represent a thromboembolic warning of stroke. An over-diagnosis of TIA can result in a lowered apparent risk of subsequent events, but our analysis of a large subgroup in the study suggests that the characteristics of admitted and discharged groups are very similar. A small proportion of patients may have been “lost” through presentations to EDs outside the region. Nonetheless, the risk of a subsequent cerebral ischaemic event within 28 days in the discharged group is only slightly lower than that reported in previous studies, including the recently published FASTER (Fast Assessment of Stroke and Transient Ischaemic Attack to Prevent Early Recurrence) trial (about 7%–10% stroke risk at 3 months).2,17 The event risk in the admitted group is similar to the reduced risk seen after rapid assessment in the EXPRESS and SOS-TIA studies (about 1%–2% stroke risk at 3 months).5,6
1 Multivariable analysis for event recurrence (stroke or TIA) within 28 days and at 29 days to 1 year, by whether admitted to hospital or discharged home
Recurrence at Day 29 to 1 year |
|||||||||||||||
2 Bivariate analysis for event recurrence (stroke or TIA) within 28 days and at 29 days to 1 year, by selected characteristics
Received 27 November 2007, accepted 2 April 2008
- Elias E Kehdi1
- Dennis J Cordato1
- Peter R Thomas1
- Roy G Beran1
- Cecilia Cappelen-Smith1
- Neil C Griffith1
- Ibrahim Y Hanna1,2
- Alan J McDougall1
- John M Worthington1
- Suzanne J Hodgkinson1,3
- 1 Neurology Department, Liverpool Hospital, Sydney, NSW.
- 2 Neurology Department, Campbelltown Hospital, Sydney, NSW.
- 3 School of Medicine, University of New South Wales, Sydney, NSW.
None identified.
- 1. Sacco RL. Risk factors for TIA and TIA as a risk factor for stroke. Neurology 2004; 62 (8 Suppl 6): S7-S11.
- 2. Johnston SC, Gress DR, Browner WS, et al. Short-term prognosis after emergency department diagnosis of TIA. JAMA 2000; 284: 2901-2906.
- 3. Hill MD, Yiannakoulias N, Jeerakathil T, et al. The high risk of stroke immediately after transient ischemic attack. Neurology 2004; 62: 2015-2020.
- 4. Lisabeth LD, Ireland JK, Risser JM, et al. Stroke risk after transient ischaemic attack in a population-based setting. Stroke 2004; 35: 1842-1846.
- 5. Rothwell PM, Giles MF, Chandratheva A, et al. Effect of urgent treatment of transient ischaemic attack and minor stroke on early recurrent stroke (EXPRESS study): a prospective population-based sequential comparison. Lancet 2007; 370: 1432-1442.
- 6. Lavallée PC, Meseguer E, Abboud H, et al. A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects. Lancet Neurol 2007; 6: 953-960.
- 7. National Stroke Foundation. National stroke audit clinical report acute services. Melbourne: NSF, 2007. http://www.strokefoundation.com.au/news/welcome/national-stroke-audit-clinical-report-acute-services (accessed Jun 2008).
- 8. Johnston SC, Rothwell PM, Nguyen-Huynh MN, et al. Validation and refinement of scores to predict very early stroke risk after transient ischaemic attack. Lancet 2007; 369: 283-292.
- 9. Cucchiara BL, Messe SR, Taylor RA, et al. Is the ABCD score useful for risk stratification of patients with acute transient ischemic attack? Stroke 2006; 37: 1710-1714.
- 10. Rothwell PM, Giles MF, Flossmann E, et al. A simple score (ABCD) to identify individuals at high early risk of stroke after transient ischaemic attack. Lancet 2005; 366: 29-36.
- 11. Sydney South West Area Health Service, NSW Health. A health profile of Sydney South West: a status report describing the population, their health and the services provided for Sydney South West Area Health Service. Health Service Planning Report No: 01/2005. Sydney: SSWAHS, 2005.
- 12. The Intercollegiate Working Party for Stroke. National clinical guidelines for stroke. London: Royal College of Physicians, 2004.
- 13. Wolf PA, Clagett GP, Easton JD, et al. Preventing ischemic stroke in patients with prior stroke and transient ischemic attack: a statement for healthcare professionals from the Stroke Council of the American Heart Association. Stroke 1999; 30: 1991-1994.
- 14. Koudstaal PJ, Gerritsma JG, van Gijn J. Clinical disagreement on the diagnosis of transient ischemic attack. Stroke 1989; 20: 300-301.
- 15. Kraaijeveld CL, van Gijn J, Schouten HJ, et al. Interobserver agreement for the diagnosis of transient ischemic attacks. Stroke 1984; 15: 723-725.
- 16. Hand PJ, Kwan J, Lindley RI, et al. Distinguishing between stroke and mimic at the bedside. The Brain Attack Study. Stroke 2006; 37: 769-775.
- 17. Kennedy J, Hill MD, Ryckborst KJ, et al; FASTER Investigators. Fast assessment of stroke and transient ischaemic attack to prevent early recurrence (FASTER): a randomised controlled pilot trial. Lancet Neurol 2007; 6: 961-969.





Abstract
Objective: To compare outcomes at 28 days and 1 year between patients admitted to hospital and those discharged after presenting to the emergency department (ED) with transient ischaemic attack (TIA).
Design and setting: All TIA presentations to EDs in a large metropolitan and rural region of Sydney and its surroundings, New South Wales, between 2001 and 2005 were extracted from state health department databases and followed up over 1 year. Admission and discharge data and subsequent TIA or stroke presentations were identified.
Main outcome measures: TIA recurrence or stroke.
Results: Of 2535 presentations to an ED with TIA during the 5-year period, 1816 patients were admitted to hospital (71.6%) and 719 were discharged from the ED (28.4%). At 28 days, the discharged group had significantly higher rates of recurrence than the admitted group for all events (TIA or stroke) (5.3% v 2.3%, P < 0.001), stroke (2.1% v 0.7%, P = 0.002), and recurrent TIA (3.2% v 1.6%, P = 0.01). During the 29–365-day follow-up period, there was no significant difference between the discharged and admitted groups for all events (4.2% v 5.1%; P = 0.37), stroke (1.3% v 2.5%; P = 0.06) or recurrent TIA (2.9% v 2.6%; P = 0.65).
Conclusion: Patients with an ED diagnosis of TIA may benefit from admission to hospital through a reduced risk of early stroke.