The health department in Queensland, like departments in most other states in Australia, is faced with challenges related to delivering health services to patients in regional and remote areas. In Queensland, most specialist health services are in the south-east corner of the state. Therefore, most patients living in rural and remote areas have to travel great distances if a specialist appointment is required. At an annual cost of about $30 million, Queensland Health assists regional patients by subsidising travel costs.1
Ear, nose and throat (ENT) services are among the specialist services offered at the Royal Children’s Hospital (RCH) in Brisbane. Specialist ENT services are delivered in a number of ways. The most common method is for patients to attend a specialist appointment in person at the RCH. Alternatively, patients may have the opportunity to see a specialist during regional outreach clinics, held infrequently in district hospitals, which are usually much closer to the patient’s home. Other less common options include the use of telemedicine, either as a videoconference appointment (real-time telemedicine), or a specialist’s review of prerecorded information (eg, digital images, video clips, clinical histories and audiograms) collected by a primary health care provider (store-and-forward telemedicine).2,3
The use of telemedicine as a means of reviewing patients in rural Queensland is a way of overcoming the inconvenience of long-distance travel and time away from home. After initial work that demonstrated the feasibility of tele-otoscopy for patients in remote areas,4,5 we showed the potential value of telemedicine for assessing children before transfer to the specialist hospital, saving families at least one journey to Brisbane.1 Outcomes, including patient satisfaction and a reduction in family costs, distances travelled, and time off work for parents of these patients, are all substantially improved with the use of telemedicine.6,7
A full history of the patient’s presenting problem was taken by the ENT surgeon during each telemedicine consultation. A detailed ENT examination was performed using the telemedicine audiovisual equipment. The equipment consisted of a video-otoscope (Flexible Microvision ENT Camera, Inline Systems, Sydney, NSW) connected to the local videoconference system (ViewStation FX, Polycom, Sydney, NSW). An accessory device, which provided a diffuse light source for examination of the oral cavity, was available for interchange with the otoscopic attachment. The regional paediatrician in Bundaberg was responsible for using the video-otoscope (Box 1) and obtaining images of the ears, nose and throat — under the remote guidance of the ENT specialist, who could offer advice and comments (Box 2). Information, such as results of hearing tests and x-rays, photographed with a video document camera, could be transmitted via videoconference. Consultations were conducted from the telemedicine studios at the Centre for Online Health at the RCH, by using digital telecommunication lines (ISDN) at a bandwidth of 384 kb/s.
Permission to conduct this study was granted by the ethics and management committees at the RCH.
In all cases, a diagnosis was recorded during the videoconference by the consulting ENT surgeon (Box 3). The most common diagnosis was recurrent tonsillitis, which accounted for 26 of the 97 diagnoses.
During the videoconference, the ENT specialist recorded a management plan for all cases (Box 3).
The one patient who had a different diagnosis after review had an initial diagnosis of unilateral perforated tympanic membrane and serous otitis media involving the other ear. After face-to-face review, about 6 months after the initial videoconference, the patient received a diagnosis of bilateral perforated tympanic membranes. Of the five patients who had surgery different from that suggested at the videoconference, four had minor alterations, including or excluding adenoidectomy, tonsillectomy and grommet insertion (Box 4). The remaining patient underwent myringoplasty for a perforated tympanic membrane after conservative management failed.
Our study shows that clinical assessments of children with potential ENT-related conditions can be conducted via videoconference with reasonable confidence. The high concordance for diagnosis and management decisions is very encouraging. Previous studies have investigated the feasibility of store-and-forward telemedicine applications, including the transmission of video clips, still digital images and audiometry results, and overall concordance has been between 80% and 84%.3,8-10
Apart from our own experience of providing a real-time tele-otology service to patients in Bundaberg,1 there are no other reports of tele-otology in Queensland. Tele-otology studies in Alaska, Scandinavia and Western Australia have been reported,4,5,8,9 mainly in relation to the transmission of pre-recorded still images of the ears, nose and throat. The use of videoconferencing to transmit ENT images to a specialist for an opinion has been shown to be technically feasible, but there remains limited evidence to justify clinical effectiveness and cost-effectiveness.
The Alaskan study investigated the accuracy of assessments made by two independent observers. A series of still video-otoscopic images were collected from a group of 40 patients requiring tympanostomy tube follow-up. Interobserver concordance was about 84% for the telemedicine application, which was reported to be similar to the interprovider concordance observed when patients were examined face-to-face.8
In WA, researchers investigated whether prerecorded information (including a clinical history, still otoscopic images, audiometry and tympanometry) could be used to make accurate diagnoses and management decisions. One specialist conducted all face-to-face consultations and was also responsible for reviewing the prerecorded information one month later. This study reported concordance ranging from 72% to 85% between assessments during the initial face-to-face appointment and decisions made after review of the prerecorded information.9
In previous work, we compared decisions made by a single specialist who saw patients and then reviewed prerecorded information (including video clips and limited history) at least 2 months later. With the prerecorded information, very limited histories were available for review — if any at all. Overall agreement was about 80%.3 We suspect that one of the reasons for the higher concordance in the current study may be that the specialist was able to undertake a complete patient history and ask specific questions during the videoconference appointment, rather than rely on information collected by another clinician.
We can conclude from this study that decisions about ENT surgical interventions for children assessed during videoconference clinics are in close agreement with decisions made by the same surgeon at face-to-face consultation. The way is therefore open to employ telemedicine more widely for pre-admission ENT assessment. However, like any telemedicine work, widespread application must be done carefully. In a state as large as Queensland, this has the potential to substantially reduce travel costs. In other work, we have documented large savings as a result of telepaediatrics; the avoided travel for burns follow-up has amounted to 1.4 million km over 6 years, which is equivalent to a return journey from Earth to the Moon, twice.11,12
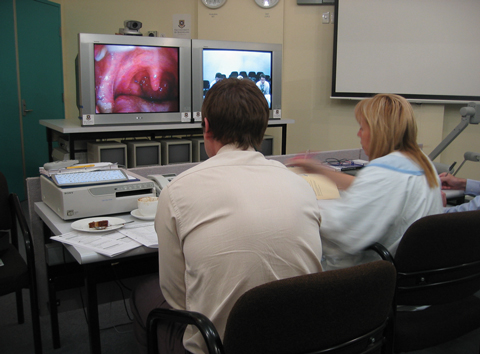
1 The regional paediatrician uses a video-otoscope to send images to the specialist via videoconference

2 Images sent via videoconference are viewed by the specialist at Brisbane’s Royal Children’s Hospital
3 Diagnoses made and management plans established during paediatric ear, nose and throat telemedicine consultations (n = 97)
Referral to general practitioner or paediatrician, and/or medication |
|||||||||||||||
4 Details of four cases where surgical management recommended during the videoconference consultations and during the face-to-face consultations were different*
Received 6 October 2007, accepted 10 January 2008
- Anthony C Smith1
- Samuel Dowthwaite2
- Julie Agnew2
- Richard Wootton1
- 1 Centre for Online Health, University of Queensland, Brisbane, QLD.
- 2 Royal Children’s Hospital and Health Service District, Brisbane, QLD.
Funding was provided by the Commonwealth Department of Health and Ageing (Medical Specialist Outreach Assistance Program).
None identified.
- 1. Queensland Health. Annual report 2002–03. Brisbane: Queensland Health, 2003. http://www.health.qld.gov.au/publications/corporate/annual_reports/annualreport2003 (accessed Jan 2008).
- 2. Smith AC, Williams J, Agnew, J et al. Realtime telemedicine for paediatric otolaryngology pre-admission screening. J Telemed Telecare 2005; 11 Suppl 2: 86-89.
- 3. Smith AC, Perry C, Agnew J, Wootton R. Accuracy of pre-recorded video images for the assessment of rural indigenous children with ear, nose and throat conditions. J Telemed Telecare 2006: 12 Suppl 3: 76-80.
- 4. Pedersen S, Hartviksen G, Haga D. Teleconsultation of patients with otorhinolaryngologic conditions. A telendoscopic pilot study. Arch Otolaryngol Head Neck Surg 1994; 120: 133-136.
- 5. Pedersen S, Holand U. Tele-endoscopic otorhinolaryngological examination: preliminary study of patient satisfaction. Telemed J 1995; 1: 47-52.
- 6. Smith AC, Youngberry K, Isles A, et al. The family costs of attending hospital outpatient appointments via videoconference and in person. J Telemed Telecare 2003; 9 Suppl 2: 58-61.
- 7. Smith AC. The feasibility and cost-effectiveness of a novel telepaediatric service in Queensland [thesis]. Brisbane: University of Queensland, 2004.
- 8. Patricoski C, Kokesh J, Ferguson S, et al. A comparison of in-person examination and video otoscope imaging for tympanostomy tube follow-up. Telemed J E Health 2003; 9: 331-344.
- 9. Eikelboom RH, Mbao MN, Coates HL, et al. Validation of tele-otology to diagnose ear disease in children. Int J Pediatr Otorhinolaryngol 2005; 69: 739-744.
- 10. Patricoski C. Alaska telemedicine: growth through collaboration. Int J Circumpolar Health 2004; 63: 365-386.
- 11. Smith AC, Kimble RM, O’Brien A, et al. A telepaediatric burns service and the potential travel savings for families living in regional Australia. J Telemed Telecare 2007; 13 Suppl 3: 76-79.
- 12. Smith AC, Patterson V, Scott RE. Reducing your carbon footprint: how telemedicine helps. BMJ 2007; 335: 1060.





Abstract
Objective: To determine agreement between diagnoses and management plans made during an initial videoconference appointment and subsequent face-to-face consultations in paediatric ear, nose and throat (ENT) surgery.
Design and setting and participants: A paediatric ENT clinic servicing patients from Bundaberg, Queensland, was conducted through the Centre for Online Health at the Royal Children’s Hospital (RCH) in Brisbane. Between January 2004 and February 2006, 152 consultations with 97 patients were carried out. We retrospectively audited patients’ charts to compare the diagnosis and management plan formulated at the initial videoconference and the eventual diagnosis and surgical management after face-to-face consultation. The clinical outcomes for children who were not recommended for surgery at the RCH were ascertained by telephone survey.
Main outcome measures: Agreement between videoconference and face-to-face consultation findings.
Results: Of the 97 patients, 75 were recommended for surgical management at the RCH. The remaining patients were either referred back to their general practitioner (9), followed up by the regional paediatrician (10) or lost to follow-up (3). At the conclusion of the study, seven patients were still awaiting surgery and were excluded. Among the 68 patients seen via videoconference and in person, the recorded diagnosis was the same in 99% of cases (67). Surgical management decisions were the same in 93% of cases (63). Telephone follow-up with paediatricians and GPs confirmed that there were no missed diagnoses or ongoing ENT-related problems in the 19 patients referred back to their care.
Conclusions: Decisions about ENT surgical interventions for children assessed during videoconference clinics are in close agreement with decisions made by the same surgeon at face-to-face consultation. The way is open to employ telemedicine more widely for pre-admission ENT assessment. However, as in any telemedicine work, widespread application requires care.