Health services across Australia are being challenged by rising demand caused by ageing populations, the high prevalence of chronic diseases and increasing patient expectations.1 Our public health services show many symptoms of strain, with growing queues and longer waiting times for access to care in emergency departments and for elective surgery. Here, we describe the emergence of a new and effective response to this situation.
Throughout the 1990s, health service models employed both in Australia and overseas had predicted a decline in demand for inpatient beds and an increase in demand for day-only beds and outpatient procedures in public hospitals,2 resulting in reductions in bed availability. However, in more recent years, the actual trend has been towards higher demand for inpatient beds. The number of older patients using inpatient hospital beds has increased to the extent that they now use about 50% of all inpatient bed-days (Tony Dunn, Director, Data Analysis and Performance Evaluation Branch, NSW Health, personal communication). In addition, the complex, chronic nature of many of the illnesses of older patients means that they stay in hospital longer (Tony Dunn, personal communication), increasing pressure on the availability of inpatient beds. Occupancy rates are over 95% in many hospital wards,3 placing pressure on bed access for elective surgery, resulting in regular postponement of elective surgery and lengthening surgery waiting lists. This is particularly the case in winter months when demand for inpatient beds is at its highest (Tony Dunn, personal communication).
As well as delays in access to care, the challenges in ensuring safety and quality across the whole health care system are substantial. Worldwide, study after study has demonstrated that events compromising patient safety occur in around one in five to one in 10 of all hospital admissions.4,5 This compares poorly with contemporary industrial quality standards of 3.6 errors per million parts produced.6 The universally high incidence of events that compromise patient safety means that they cannot simply be attributable to individual failings or to the funding and structural characteristics of the health systems involved.
NSW Health and Flinders Medical Centre (FMC) in South Australia, the locations in which the redesign work that is the subject of this supplement is occurring, are not alone in facing these challenges. The same problems have been identified in other health services in Australia,7 and overseas (eg, the United Kingdom, Ireland, the United States8-10). In the UK, the government has led a major program of reform to improve patient access to health services and to reduce adverse events. In 2001, it established the Modernisation Agency which developed approaches to redesigning health care delivery. Some of these approaches have been used in the programs developed by NSW Health and FMC. The Institute of Healthcare Improvement in the US10 promotes similar approaches to redesigning patient journeys in hospitals across the country.
NSW Health is the largest health service in Australia. It comprises eight Area Health Services (AHSs) across the state. In the 2004–05 financial year, it serviced a population of 6.9 million with an annual expense budget of over $11 billion, and with a full-time equivalent staff of about 93 000. In that same period, the service recorded 1.4 million public hospital admissions and two million visits to public hospital emergency departments (EDs).3
The public health system in New South Wales was showing clear signs of strain (Box 1). Before the introduction of the Clinical Services Redesign Program in NSW in 2005,11 congestion in hospital EDs had been growing, with resultant delays and difficulties for patients in accessing care. Many patients each day were being kept waiting on stretchers outside the ED for over an hour.12
Triage times for patients in the Australasian Triage Scale categories 3 and 4 are the best indicators of the efficiency of EDs, as patients in these triage categories account for the bulk of emergency presentations at EDs. The targets for these two categories had not been met before clinical process redesign initiatives in NSW public hospitals.12
In the years 2002–2005, ED patients who needed to be admitted to hospital experienced access block of 40%–50%, and reaching 60% in some hospitals — NSW Health’s target was less than 20%. An access block of 50% on an average winter afternoon in NSW public hospitals means that about 400 people are being kept waiting in EDs for admission. Patients were often admitted to inappropriate wards (ie, they were “outliers”, who are empirically observed to have a longer length of stay), which exacerbated access block in other parts of the hospital (Box 2). Patients in need of elective surgery procedures were often waiting longer than 12 months (10 000 patients in 2004), while those with cases classified as urgent by their surgeons were waiting longer than 30 days (4000 patients in 2004).
Underlying all this has been the relentless pressure resulting from an ageing population. The proportion of people aged 65 years and older in NSW will increase from 13.6% to about 20% between 2006 and 2026,13 and demand for health services will increase accordingly. Although people aged 70 years and over represent only 9.7% of the population, they account for 41.6% of all public hospital use (Tony Dunn, Director, Data Analysis and Performance Evaluation Branch, NSW Health, personal communication). In conjunction with the ageing of the population, there will be future increases in the number of people with chronic diseases such as diabetes. For instance, the proportion of Australians with diabetes is expected to more than treble between 2000 and 2051.14
FMC is a 500-bed teaching general hospital in the southern suburbs of Adelaide. It provides the whole range of acute services required by a population of about 300 000 people. Smaller community hospitals and the private health care system also service that population. Within this de-facto consortium of care providers, the primary role played by FMC is the provision of time-urgent, complex care. Over 70% of patients who require an overnight stay are admitted as emergency cases, and over 40% of patients presenting at FMC’s ED are subsequently admitted.15
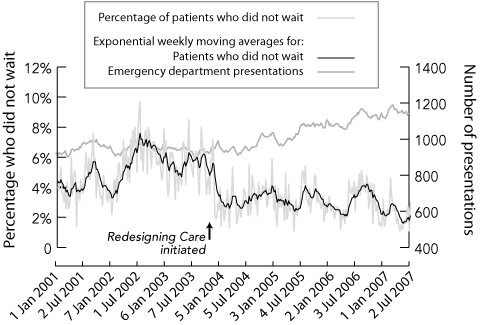
Before the launch of the Redesigning Care program in 2003,16 FMC was showing similar signs of strain and stress to those described above. However, the congestion within its ED was so severe that there was increasing evidence of a major problem with the provision of safe care within that department and elsewhere in the hospital. This provided a particularly powerful impetus for developing an improvement program.
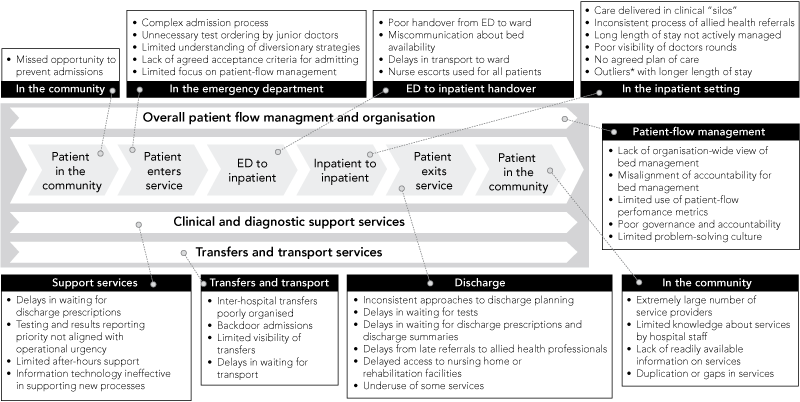
The growing demand for health care outlined above is external to health services, and is therefore beyond their control. Concentrating solely on the difficulty of external forces can simply induce a sense of helplessness that is unwarranted. Within health services, there are substantial opportunities to improve the safety, quality and accessibility of the care provided. Box 3 illustrates a typical patient journey through a hospital and shows the kinds of problems and disconnections between the components of care that interfere with the provision of an effective, well coordinated patient journey through the health system.
Typical examples of the problems and disconnections follow.
Poor communication, with care delivered in clinical “silos”, and miscommunication and adverse events usually occurring at the interfaces of these silos. Decisionmakers are often not able to be contacted as needed; for example, decision making for surgical patients in ED can often be delayed because surgical staff are busy in theatre.
Poor alignment of activities; for example, delivery of a meal, a physiotherapist visit and an investigation all happening simultaneously.
Imperfect alignment of laboratory and imaging services with patient requirements, and lack of a robust prioritised approach to laboratory workload to optimise overall hospital patient flow.
Poor interface between specialist teams and ED staff.
Staff not being rostered according to the requirements of patients. A typical example is the “9 to 5” rostering which still dominates for various staff in service areas such as ED, even when patient arrivals and the business of the ED peak in late afternoon to early evening. This mismatch of patient demand and staff supply results in minimal staff having to deal with maximal activity. This causes further frustration for staff, worsening of patient queues and increases the risk of adverse events.
ED staff needing to “shop around” for an inpatient team to take responsibility for a patient (often older) who is difficult to “sell”.
Lack of a common understanding by both staff and patients of the expected patient pathway and date of discharge, which inhibits better planning of preparatory work before discharge. Particularly problematic is the poor compliance with documenting an estimated date of discharge. This is compounded by senior nurses and registrars not being empowered to discharge patients. Processes for smooth discharge, such as preparation of discharge prescriptions, are often not well planned. For example, a junior doctor is called at late notice to write prescriptions for a patient ready for departure, but the doctor is busy with other tasks and does not complete the prescriptions until after the pharmacy has closed, thus resulting in a delay in the patient’s departure.
Decision making in wards tends to happen only “9 to 5” Monday to Friday.
Suboptimal processes for accessing services delivered in the community. Only certain professions, rather than the multi-skilled team, are authorised to perform the tasks required to “move the patient along”. All of these factors result in unnecessary delays in discharging patients from acute facilities into the community, causing a damming of patient flow “downstream” that exacerbates the “upstream” congestion in the ED.
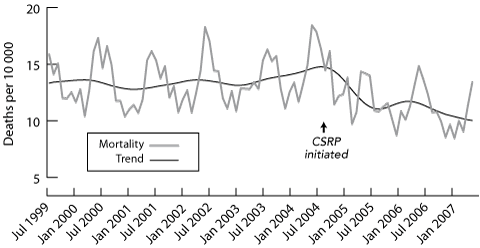
The application of clinical process redesign in NSW Health and at FMC has greatly improved the delivery of care in the face of significantly increased demand. In NSW, emergency admission performance (Box 4) and the number of patients waiting more than 12 months for surgery (Box 5) have greatly improved, while death rates in EDs have fallen (Box 6). At FMC, there have been similar improvements in access to emergency care (Box 7).
Subsequent articles in this supplement outline the methods of clinical process redesign, its application to both unplanned and planned arrivals at NSW hospitals, the use of an approach known as “lean thinking” in the redesign process at FMC,15 and important aspects of implementing and sustaining change in health care.
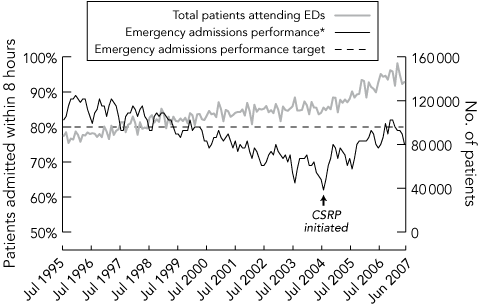
4 Emergency admission performance* in New South Wales hospitals, 1995–2007
 | |||||||||||||||
|
ED = emergency department. CSRP = Clinical Services Redesign Program. * Percentage of patients admitted through the ED who egress from the ED within 8 hours. | |||||||||||||||
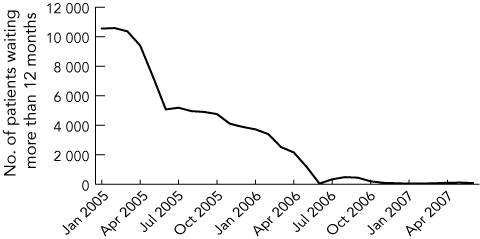
5 Number of patients waiting > 365 days for surgery in New South Wales hospitals, January 2005 to June 2007
- 1. Schofield DJ, Earnest A. Demographic change and the future demand for public hospital care in Australia, 2005 to 2050. Aust Health Rev 2006; 30: 507-515.
- 2. McKee M. Reducing hospital beds: what lessons have we learned? European Observatory on Health Systems and Policies Brief No. 6. Copenhagen: World Health Organization Regional Office, 2004. http://www.euro.who.int/observatory/Publications/20020527_16 (accessed Jan 2008).
- 3. NSW Department of Health. Annual report, 2004–05. http://www.health.nsw.gov.au/pubs/2005/pdf/ar2005.pdf (accessed Aug 2007).
- 4. Brennan TA, Leape LL, Laird NM, et al. Incidence of adverse events and negligence in hospitalized patients: results of the Harvard Medical Practice Study. N Engl J Med 1991; 324: 370-376.
- 5. Wilson RM, Runciman WB, Gibberd RW, et al. The Quality in Australian Health Care Study. Med J Aust 1995; 163: 458-471.
- 6. Mikel H. Mikel Harry on six sigma in healthcare. Interview by Guinane CS. J Healthc Qual 2006; 28: 29-36.
- 7. Victorian Department of Human Services. Patient flow collaborative 2005. http://www.health.vic.gov.au/patientflow/2005.htm (accessed Aug 2007).
- 8. UK National Health System Modernisation Agency. http://www.dh.gov.uk/en/Policyandguidance/Organisationpolicy/Modernisation/Systemreform/index.htm (accessed Sep 2007).
- 9. Irish Health Service Reform Programme. Purpose of reform. http://www.healthreform.ie/background/purpose.html (accessed Sep 2007).
- 10. US Institute for Healthcare Improvement [website]. http://www.ihi.org/ihi (accessed Sep 2007).
- 11. NSW Health. Clinical services redesign program. http://www.health.nsw. gov.au/csrp/ (accessed Jan 2008).
- 12. NSW Department of Health. Annual report, 2005–06. http://www.health. nsw.gov.au/pubs/2006/pdf/ar_2005_06.pdf (accessed Aug 2007).
- 13. Australian Bureau of Statistics. Population projections, Australia, 2004 to 2101. Canberra: ABS, 2007. (ABS Catalogue No. 3222.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/3222.02004 %20to%202101?OpenDocument (accessed Aug 2007).
- 14. Davis WA, Knuiman MW, Hendrie D, Davis TM. The obesity-driven rising costs of type 2 diabetes in Australia: projections from the Fremantle Diabetes Study. Intern Med J 2006; 36: 155-161.
- 15. King DL, Ben-Tovim DI, Bassham J. Redesigning emergency department patient flows: application of Lean Thinking to health care. Emerg Med Australas 2006; 18: 391-397.
- 16. Redesigning Care. Improving the patient journey. http://www.flinders.sa.gov.au/redesigningcare/a8_publish/modules/publish/content.asp?navgrp=overview (accessed Jan 2008).





We thank the numerous NSW Health staff who have participated in redesign projects, and Professor John Marley for his advice in preparing this article. We also acknowledge the role of Dr Deborah Lloyd in editing this article and producing this supplement.
None identified.