Adverse events caused by medication have been estimated to harm 1% to 2% of patients admitted to hospitals in the United States, United Kingdom and Australia.1-3 Most incidents that result in harm to patients originate in the prescribing process.4 Human error is a frequent factor.5
The intern year is a time for consolidating medical school education through continued learning and acquisition of knowledge and skills under direct supervision. More prescribing errors occur in the first year after graduation than in all other years.6 In an American study, 45% of interns reported having made at least one clinical error; 29% were prescribing errors, of which 15% were fatal.7
Although a particular action or omission may be the immediate cause of an incident (described as an active failure or error),8 closer analysis usually reveals a series of events and departures from safe practice, known as an error chain.5 The notion of a single root cause, although widespread, is an oversimplification.8,9 A structured process, which uses human psychology methods, is available for analysis of errors.8,10 This analysis method considers the individual’s working environment, including the team and the organisation.
A clinically meaningful prescribing error occurs when, as a result of a prescribing decision or prescription writing process, there is an unintentional significant (1) reduction in the probability of treatment being timely and effective or (2) increase in the risk of harm when compared with generally accepted practice.11
Semistructured face-to-face interviews incorporating a questionnaire were conducted to assess the causes of the prescribing error. The process was adapted, with permission, from the methods of Vincent et al8 and Dean et al.12 Interviews took between 15 and 115 minutes (average, 44 minutes) and used the process outlined in Box 1.
We (a senior physician and two senior pharmacists) analysed and coded the transcripts independently, using Vincent et al’s framework of error-producing factors.8 Consensus was achieved through discussion.
We identified latent factors underlying the errors, by thematic analysis.
The 21 errors that were analysed are described in Box 2. They occurred on admission to hospital (3), during the inpatient stay (9), and on discharge (9). Antithrombotic and antibiotic drugs accounted for half the errors.
Causes of the errors, presented in accordance with Reason’s model of accident causation, are shown as holes in layers of Swiss cheese to indicate the four levels in which failures occur, enabling an accident to penetrate barriers and defences, resulting in harm to the patient (Box 3).5
We identified at least one active failure, or error, in each incident (Box 2).
Interns cited two or more underlying or influencing factors contributing to each error (Box 2). In new-prescribing errors, a median of 5 (range, 3–5) different factors were mentioned. In represcribing errors, the median was 3 (range, 2–5). Details of different components of the error-producing factors were identified from analysis of the transcripts (Box 4).
Team factors were present in 16 incidents. They were associated with supervision, communication and responsibility. Poor supervision was a primary theme in nine new-prescribing errors but only three represcribing errors. Interns frequently (in 14 errors) mentioned communication about medication, with comments such as “dialogue is very one-way” and “there’s not much discussion or opportunity to learn”.
Quotations illustrating specific factors are shown in Box 5.
All errors were associated with a varying combination of environment, team, individual, task, patient and latent factors, in a system with porous defences. We found that, while almost all errors were influenced by environment factors, factors associated with new-prescribing errors and represcribing errors were different, which was not the case in previous studies of error causation.1,12,13
New-prescribing errors involved inexperienced interns, who were tired, hungry, and distracted, prescribing for patients with complex disorders. Team factors, in particular lack of supervision, were also more frequently associated with new-prescribing errors. Represcribing errors were often related to the task, including the design and location of the medication chart. Therefore, the view that a single intervention in isolation will prevent most prescribing errors is simplistic.14
Our results confirm those of others that improving drug knowledge may decrease the risks of new-prescribing errors.14-18 However, a lack of drug knowledge was a partial cause of only one represcribing incident. Interns need to be able to apply drug knowledge to allow them to tailor therapy to an individual patient. Safe-prescribing skills and awareness of medication errors is required by all members of the health care team,19,20 and should be a core component of undergraduate and postgraduate training programs, as outlined in the new curriculum framework for junior doctors.21 Practical safe-medication practice training that improves the safety of medical students’ prescribing should be a core component of prescribing education.14,20
The primary focus of the intern year is to produce competent, independent practitioners through an apprenticeship, with training in a range of supervised posts.22 In this study, there was an assumption by interns that senior staff would check their prescriptions. Often, this did not happen. Our findings reinforce those from the UK, where a culture exists in which new prescribing is seen by senior and junior staff as focused on drug selection, and represcribing as a low-risk chore for which training or supervision is not required.12,17
The complexity of prescribing is not appreciated by the novice, and the novice’s lack of deeper understanding does not appear to be understood and supported by supervisors. Interns often have insufficient knowledge to appreciate when they need to seek advice. Deference to a hierarchical structure is a well recognised risk in all complex teams, and junior staff need to have the skills and feel able to confirm and clarify directions.23
Supervision should take account of all prescribing risk factors, including the patient’s complexity, the intern’s competence, the specific medications being prescribed and the availability of guidelines. This must be within a culture in which prescribing is seen as an important, high-risk intervention. Institutions must develop an environment in which prescribing errors can be constructively discussed and analysed, and learning from errors should occur at an individual, team and organisation level.12
Electronic prescribing with decision support offers a partial solution,24,25 but an effective system is not currently widely available in Australia.26 Standardised medication charts and systems incorporating decision support and forcing functions have been developed and should be implemented to reduce prescribing errors.27 With a standard chart in place, students can be trained to use one system, and the risks of error due to unfamiliarity with chart design can be reduced.17
Nursing staff provide a critical defence by reviewing medications before administration, but training in safe medication is also required.28 Pharmacists detect errors and improve the safety of prescribing.29 Their role of reviewing prescriptions and contributing to prescribing decisions must be further developed.13
The prescribing errors identified have happened before and will happen again unless changes at many levels are made. Prescribing skills and awareness of medication errors must be developed through training. Standardised medication charts reduce errors and are being implemented across Australia, and guidelines should be redesigned and readily available. A cultural shift, in which prescribing is seen as important, must occur, with continual senior review and tailored supervision of interns in an atmosphere that encourages clarification and learning.
1 Interview to identify causes of prescribing errors by interns
The questionnaire
This was based on Vincent et al’s framework of contributory factors8 and was used to identify and systematically explore any contributory factors. These factors included:
Working-environment factors
Staffing levels, skill mix and workload
Layout of workplace, ward office
Administrative and managerial support
Task factors
Poor design of equipment such as medication chart
Availability, clarity and use of protocols
Availability and accuracy of test results
Individual factors
Knowledge, skills and competence
Motivation and attitude
Physical and mental wellbeing
Team factors
Verbal and written communication
Supervision and seeking help
Team structure (consistency and leadership)
Patient factors
Condition (complexity and seriousness)
Language and communication
2 Prescribing errors and performance-influencing factors from interviews with interns and thematic analysis
3 Incident analysis framework*
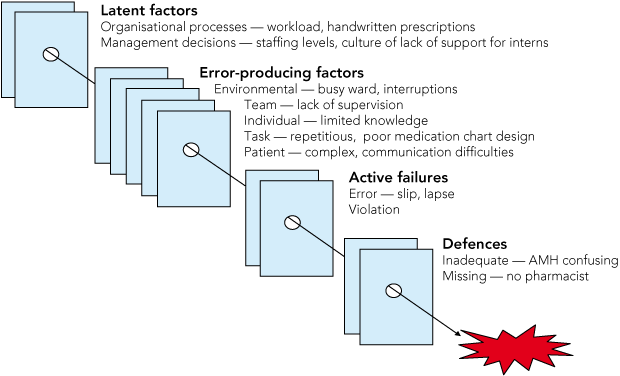 |
|
AMH = Australian medicines handbook. |
4 Factors involved in prescribing errors*
PBS = Pharmaceutical Benefits Scheme. | |||||||||||||||
- Ian D Coombes1,2
- Danielle A Stowasser1,2
- Judith A Coombes1,2
- Charles Mitchell2,3
- 1 Pharmacy Department, University of Queensland, Brisbane, QLD.
- 2 Safe Medication Practice Unit, Queensland Health, Brisbane, QLD.
- 3 School of Medicine, University of Queensland, Brisbane, QLD.
We thank all the junior doctors involved in this study and Dr Bryony Dean Franklin, University of London, for help developing the interview schedule.
None identified.
- 1. Leape LL, Bates DW, Cullen DJ, et al. Systems analysis of adverse drug events. JAMA 1995; 274: 35-43.
- 2. Neale G, Woloshynowych M, Vincent C. Exploring the causes of adverse events in NHS hospital practice. J R Soc Med 2001; 94: 322-330.
- 3. Wilson RM, Runciman WB, Gibberd RW, et al. The Quality in Australian Health Care Study. Med J Aust 1995; 163: 458-471.
- 4. Bates DW, Boyle DL, Vander Vliet MB, et al. Relationship between medication errors and adverse drug events. J Gen Intern Med 1995; 10: 199-205.
- 5. Reason J. Human error. Cambridge: Cambridge University Press, 1990.
- 6. Lesar TS, Briceland LL, Delcoure K, et al. Medication prescribing errors in a teaching hospital. JAMA 1990; 263: 2329-2334.
- 7. Wu A, Folkman S, McPhee S, Lo B. Do house officers learn from their mistakes? JAMA 1991; 265: 2089-2094.
- 8. Vincent C, Taylor-Adams ST, Chapman EJ, et al. How to investigate and analyse clinical incidents: Clinical Risk Unit and Association of Litigation and Risk Management protocol. BMJ 2000; 320: 777-781.
- 9. Vincent C. Understanding and responding to adverse events. N Engl J Med 2003; 348: 1051-1056.
- 10. Reason J. Human error: models and management. BMJ 2000; 320: 768-770.
- 11. Dean B, Barber N, Schachter M. What is a prescribing error? Qual Health Care 2000; 9: 232-237.
- 12. Dean B, Schachter M, Vincent C. Causes of prescribing errors in hospital inpatients: a prospective study. Lancet 2002; 359: 1373-1378.
- 13. Lesar TS, Briceland L, Stein DS. Factors related to errors in medication prescribing. JAMA 1997; 277: 312-317.
- 14. Aronson JK. A prescription for better prescribing. Br J Clin Pharmacol 2006; 61: 487-491.
- 15. Thornton PD, Simon S, Mathew TH. Towards safer drug prescribing, dispensing and administration in hospitals. J Qual Clin Pract 1999; 19: 41-45.
- 16. Australian Council for Safety and Quality in Health Care. Second national report on patient safety: improving medication safety. Canberra: ACSQHC, 2002. http://www.health.gov.au/internet/safety/publishing.nsf/Content/F0FD7442D1F2F8DDCA2571C6000894FF/$File/med_saf_rept.pdf (accessed Nov 2007).
- 17. Barber N, Rawlins M, Dean Franklin B. Reducing prescribing error: competence, control, and culture. Qual Saf Health Care 2003; 12 Suppl 1: i29-i32.
- 18. Boreham NC, Mawer GE, Foster RW. Medical students’ errors in pharmacotherapeutics. Med Educ 2000; 34: 188-193.
- 19. Reason J. Beyond the organisational accident: the need for “error wisdom” on the frontline. Qual Saf Health Care 2004; 13 Suppl 2: ii28-ii33.
- 20. Coombes I, Mitchell C, Stowasser D. Safe medication practice tutorials: a practical approach to preparing safe prescribers. Clin Teach 2007; 4: 128-134.
- 21. Leeder SR. Preparing interns for practice in the 21st century. Med J Aust 2007; 186 (7 Suppl): S6-S8. <MJA full text>
- 22. Graham IS, Gleason AJ, Keogh GW, et al. Australian Curriculum Framework for Junior Doctors. Med J Aust 2007; 186 (7 Suppl): S14-S19. <MJA full text>
- 23. Firth-Cozens J. Teams, culture and managing risk. In: Vincent C, editor. Clinical risk management: enhancing patient safety. 2nd ed. London: BMJ Publishing Group, 2001: 355-368.
- 24. Bates DW, Gawande AA. Improving safety with information technology. N Engl J Med 2003; 348: 2526-2534.
- 25. Franklin BD, O’Grady K, Donyai P, et al. The impact of a closed-loop electronic prescribing and administration system on prescribing errors, administration errors and staff time: a before-and-after study. Qual Saf Health Care 2007; 16: 279-284.
- 26. Coombes I, Stowasser D, Mitchell C, Varghese P. Effect of computerised prescribing on use of antibiotics [letter]. Med J Aust 2004; 180: 140-141. <MJA full text>
- 27. Youngman J, Coombes I, Stowasser D, Mitchell C. The implementation of a national inpatient medication chart as a national initiative to address medication error. International Society for Quality in Health Care International Conference; 2006 Oct 22–25; London, UK. http://www.isqua.org.au/isquaPages/Conferences/London/AbstractsSlides/MON23/AFTERNOON/6%20-%20212-ABS.pdf (accessed Dec 2007).
- 28. Coombes I, Heel A, Stowasser D, et al. Identification of medication errors by nurses during a simulated ward medication safety orientation program. J Pharm Pract Res 2005; 35: 190-195.
- 29. Leape LL, Cullen DJ, Clapp MD, et al. Pharmacist participation on physician rounds and adverse drug events in the intensive care unit. JAMA 1999; 282: 267-270.





Abstract
Objective: To identify and analyse factors underlying intern prescribing errors to inform development of specific medication-safety interventions.
Design: A prospective qualitative study that involved face-to-face interviews and human-factor analysis.
Setting: A tertiary referral teaching hospital, Brisbane, Queensland, February–June, 2004.
Participants: Fourteen intern prescribers involved in 21 errors.
Method: A structured questionnaire was used to identify factors causing the errors. Transcripts were analysed on the basis of human-error theory to identify underlying themes.
Main outcome measures: Factors underlying prescribing errors.
Results: Errors were multifactorial, with a median of 4 (range, 2–5) different types of performance-influencing factors per error. Lack of drug knowledge was not the single causative factor in any incident. The factors in new-prescribing errors included team, individual, patient and task factors. Factors associated with errors in represcribing were environment, task and number of weeks into the term. Defences against error, such as other clinicians and guidelines, were porous, and supervision was inadequate or not tailored to the patient, task, intern or environment. Factors were underpinned by an underlying culture in which prescribing is seen as a repetitive low-risk chore.
Conclusion: To reduce the risk of prescribing errors, a range of strategies addressing patient, task, individual, team and environment factors must be introduced.