Skin cancer is a significant and growing health issue in Australia. In 2001, non-melanoma skin cancer (NMSC) was both the most common cancer in Australia and the most expensive to treat.1 Melanoma is the third most common cancer in both men and women.2
Skin cancer management in Australia has traditionally been shared between general practitioners and specialists. Surgical excision is the recommended treatment for all primary melanoma and most NMSC, although various non-surgical treatments are appropriate for some NMSC subtypes. Direct suture can be used to close most excisions, but the size or anatomical site of some lesions dictates the use of skin flaps or skin grafts.3,4
Substantial concerns have been raised about the use of skin flaps in primary care settings, particularly skin cancer clinics.5,6 There has been heated debate in the medical and general media, with allegations of inappropriate, low-quality and unnecessary surgical procedures being carried out.7 To inform the debate, we describe here the changing patterns of surgical treatment of skin cancer among GPs and specialists. Specifically, we compare the rates of skin cancer excisions and surgical repairs done by GPs and specialists over a 5-year period, to determine whether GPs were responsible for a disproportionate level of flap repairs relative to their rates of skin cancer excisions.
The MBS item numbers (as defined and categorised in the Australian Government MBS8) were grouped into three categories:
Excision of histologically confirmed NMSC (items 31255–31295);
Excision of histologically confirmed melanoma (items 31300–31355);
Surgical repairs: all graft repairs (items 45439, 45445, 45448 and 45451) and all flap repairs (simple and small [item 45200]; complicated or large [item 45203]; or flaps to repair defects on the eyelid, nose, lip, ear, neck, hand, thumb, finger or genitals [item 45206]).
These item numbers are used by all doctors for claiming the service fee from Medicare.
We calculated the total number of NMSC excisions, melanoma excisions, flap repairs and skin grafts done by GPs and specialists in each state and territory, and for all of Australia. To adjust for population differences over time and between states, we also calculated the rate of use of each procedure per 1000 Australian people, based on population figures from the Australian Bureau of Statistics.9 Confidence intervals for these rates were derived assuming a binomial likelihood function.
Separate linear regression models examined changes in overall annual rates of skin cancer excisions and surgical repairs over time, and compared changes in GP and specialist rates. Student’s t tests of the estimated line gradients were used to determine whether changes were significant. In comparing GP and specialist rates, a dichotomous indicator variable was created. For each excision and repair variable, regression models were repeated with the inclusion of this indicator variable and an indicator variable × time interaction. The indicator variable allowed for different baseline intercept values between GP and specialist groups, and the indicator variable × time interaction allowed for different changes in rates over time between GP and specialist groups. The usual approach would be to also adjust these regression models for important population demographic factors that might act as confounders — for example, the age and sex distribution over time and between states and territories. However, we could not make such adjustments, as the Medicare data did not include patients’ age and sex details. Finally, we calculated the ratio of skin cancer excisions to flap repairs for GPs and specialists and compared the change for both groups between 2001 and 2005. Confidence intervals for these ratios were derived using computer simulation (size, n = 100 000) assuming a binomial likelihood function for rates of excisions and flap repairs. Statistical significance was defined at the 5% level for all comparisons.
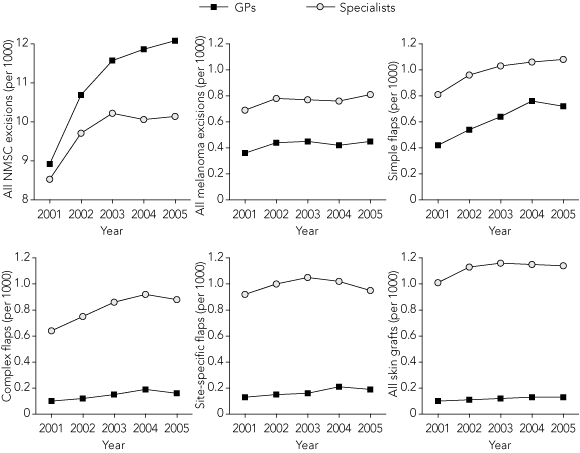
The number of NMSCs excised by GPs increased from 173 170 (51.1% of all excisions) in 2001 to 245 560 (54.4% of all excisions) in 2005, representing a mean annual increase of 0.75/1000 people, from 8.92/1000 people in 2001 to 12.08/1000 people in 2005. Over the same period, specialists’ mean annual excision rate increased by 0.36/1000 people, from 8.53/1000 people in 2001 to 10.14/1000 people in 2005 (Box 1). The estimated mean annual increase in the rate of NMSC excisions for GPs was significantly greater than that for specialists (P = 0.003) (Box 2).
Queensland GPs’ rate of NMSC excisions per 1000 people was nearly twice that of their Queensland specialist colleagues, about 2.5 times that of their New South Wales GP colleagues and about 5 times that of their GP colleagues in Victoria. These ratios were relatively stable for both 2001 and 2005. Queensland specialists also excised at significantly higher rates than their specialist colleagues in other jurisdictions (Box 1).
GPs excised 7010 melanomas in 2001 (34.3% of all cases), increasing to 9146 (35.8% of all cases) in 2005. GPs’ excision rate was 0.36/1000 people in 2001 and 0.45/1000 people in 2005. In comparison, specialists’ excision rate was 0.69/1000 people in 2001 and 0.81/1000 people in 2005 (Box 1). There was no difference in the average annual rate of change over time between GPs and specialists (P = 0.25) (Box 2).
There was considerable variability among states in rates of melanoma excisions by GPs. In particular, Queensland GPs had excision rates of 0.68/1000 people in 2001 and 0.82/1000 people in 2005, nearly double the national rate for GPs and similar to the national rate among specialists (Box 1).
The number of flap repairs done by GPs increased from 12 452 (21.3% of all cases) in 2001 to 21 758 (26.9% of all cases) in 2005, while the number done by specialists increased from 46 098 in 2001 to 58 984 in 2005 (Box 1). GPs’ flap repair rate increased by a mean of 0.12/1000 people per year, from 0.64/1000 people in 2001 to 1.07/1000 people in 2005 (P = 0.03). The flap repair rate among specialists increased by a mean of 0.13/1000 people per year, from 2.37/1000 people in 2001 to 2.90/1000 people in 2005 (P = 0.04). There was no difference in the estimated mean annual rate of change of flap repairs over time between GPs and specialists (P = 0.83) (Box 2).
Queensland GPs and specialists both had substantially higher rates of use of skin flaps than their colleagues in other states and territories. Specifically, Queensland GPs’ flap repair rate increased from 1.50/1000 people in 2001 to 2.96/1000 people in 2005, compared with a national rate increase of 0.64/1000 people in 2001 to 1.07/1000 people in 2005. Similarly, Queensland specialists’ flap repair rate increased from 3.20/1000 people in 2001 to 4.83/1000 people in 2005 — substantially higher than rates among their colleagues in other states and territories (Box 1).
Overall, the annual rate of graft repairs done by GPs was considerably lower than that of specialists (P < 0.001) (Box 2). Queensland GPs and specialists, however, both had substantially higher rates of graft repairs than their respective colleagues in other states and territories (Box 1).
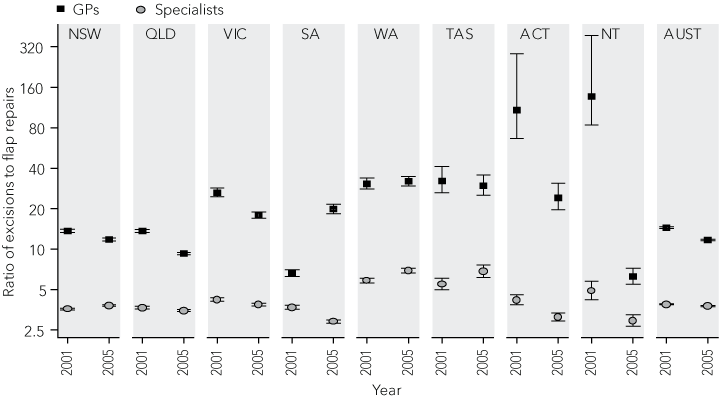
Nationally, the number of excisions per flap repair done by specialists was relatively stable, at about 3.8–3.9. In contrast, the excision to flap ratio for GPs fell from 14.1 in 2001 to 12.1 in 2005 (P < 0.001) (Box 3). In 2001, GPs in Queensland and NSW (the states with the highest level of skin cancer surgery activity) both excised 14.1 skin cancers per flap repair. In 2005, NSW GPs excised 12.1 skin cancers per flap repair, while their Queensland colleagues excised 9.2 skin cancers per flap repair (P < 0.001) (Box 3).
GPs have significantly increased their use of flap repairs in recent years. However, the increase was from a low base. The rise may reflect increasing skills in excising and repairing large complex lesions and lesions in cosmetically sensitive sites, and thus may be entirely appropriate. However, it has also been suggested that flap repairs are being done by GPs in skin cancer clinics when a direct sutured closure would be more appropriate and less costly to the health care system.10 Our data can not differentiate between these possibilities.
Medicare has mechanisms in place to identify fraud and potentially inappropriate clinical practice.6 It also provides regular information and updates to interested groups at meetings and seminars. We argue for increased vigilance of this type. We also support an expansion in the educational and training opportunities for doctors working in primary care skin cancer medicine to ensure the highest standards of clinical care and billing of services.
There was considerable variation between states in our results — most notably reflected in the higher rates of excisions and repairs done by Queensland GPs and specialists. Queensland GPs’ rates were more reflective of the national rates of specialists than that of their GP colleagues in other states — they did 68% of all skin cancer excisions and 38% of the flap repairs, compared with 51% and 25%, respectively, done by their NSW colleagues. This may be due to the underlying population of providers — NSW has 110 dermatologists (1.6/100 000 population), compared with 43 (1.1/100 000 population) in Queensland, only three of whom practice in the far north of the state. Consequently, Queensland GPs may have to undertake procedures that their colleagues in other states would normally refer to specialists.11,12 The higher rates in Queensland could also reflect a higher incidence of skin cancers in that state, or differing demographics of the population.
Our findings should not be misinterpreted as reflecting the prevalence of skin cancer in Australia. Our data are case reports of excisions and surgical repairs billed to Medicare, and inevitably contain multiple entries for individual people. Moreover, a significant number of NMSCs would not be included in our analysis because of being treated by non-surgical means. An accurate estimate of the incidence of NMSC is difficult, as NMSC is not notifiable to cancer registries. Based on extrapolation from national household survey data,2 about 374 000 people were treated for NMSC in 2002, which is comparable to the 400 550 NMSC excisions reported in our study. Our total of 20 414 melanomas excised in 2001 is more than twice the figure of 8885 melanomas reported by cancer registries in 2001.2 This is probably largely because Medicare data include both invasive and in-situ melanoma, while cancer registries report only invasive melanoma.
Our analysis was prompted by allegations that doctors working in skin cancer clinics are responsible for an “explosion” in skin cancer procedures, particularly flap repairs. Although we could not determine the effect of skin cancer clinics on patterns of skin cancer surgery, we found that GPs are responsible for a growing proportion of NMSC and melanoma excisions and flap repairs. However, the number of flap repairs has grown from a relatively low base and, overall, the rate of change for GPs is not different from that for specialists. The markedly different patterns of care in Queensland are interesting and warrant further study.
1 Numbers and rates of NMSC excisions, melanoma excisions and surgical repairs per 1000 Australian people performed by general practitioners and specialists, by state and territory, 2001 and 2005
Received 31 January 2007, accepted 19 July 2007
- Deborah A Askew1
- David Wilkinson1
- Philip J Schluter2
- Kerena Eckert1
- 1 Discipline of General Practice, School of Medicine, University of Queensland, Brisbane, QLD.
- 2 Faculty of Health, Auckland University of Technology, Auckland, New Zealand.
None identified.
- 1. Australian Institute of Health and Welfare. Health system expenditures on cancer and other neoplasms in Australia, 2000–01. Canberra: AIHW, 2005. (AIHW Cat. No. HWE 29; Health and Welfare Expenditure Series No. 22.) http://www.aihw.gov.au/publications/hwe/hsecna00-01/hsecna00-01.pdf (accessed Jul 2007).
- 2. Australian Institute of Health and Welfare and Australasian Association of Cancer Registries. Cancer in Australia: an overview, 2006. Canberra: AIHW, 2007. (AIHW Cat. No. CAN 32; Cancer Series No. 37.) http://www.aihw.gov.au/publications/can/ca06/ca06.pdf (accessed Jul 2007).
- 3. Australian Cancer Network Management of Non-Melanoma Skin Cancer Working Party. Clinical practice guidelines. Non-melanoma skin cancer: guidelines for treatment and management in Australia. Canberra: National Health and Medical Research Council and Australian Cancer Network, 2003. http://www.nhmrc.gov.au/publications/synopses/_files/cp87.pdf (accessed Jul 2007).
- 4. National Health and Medical Research Council. Clinical practice guidelines. The management of cutaneous melanoma. Canberra: NHMRC, 1999. http://www.nhmrc.gov.au/publications/synopses/_files/cp68.pdf (accessed Jul 2007).
- 5. Medicare Australia. Medicare Benefits Schedule (MBS) item statistics reports. http://www.medicareaustralia.gov.au/statistics/dyn_mbs/forms/mbs_tab4.shtml (accessed Jul 2007).
- 6. Professional Services Review. Report to the professions 2005–06. Canberra: PSR, 2006. http://www.psr.gov.au/docs/publications/PSR_RTP.pdf (accessed Jan 2007).
- 7. Smith P. Call for audits of skin cancer GPs. Aust Doctor 2005; 12 August: 3.
- 8. Australian Government Department of Health and Ageing. Medicare Benefits Schedule. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/Medicare-Benefits-Schedule-MBS-1 (accessed Jan 2007).
- 9. Australian Bureau of Statistics. Australian historical population statistics, 2006. Canberra: ABS, 2007. (ABS Cat. No. 3105.0.65.001.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/3105.0.65.001Main+Features12006?OpenDocument (accessed May 2007).
- 10. Chia ALK, Shumack S. Skin cancer clinics in Australia: workload profile and performance indicators from an analysis of billing data [letter]. Med J Aust 2006; 185: 239-240. <MJA full text>
- 11. Australasian College of Dermatologists. Find a dermatologist. http://www.dermcoll.asn.au/publicASP/find_a_dermatologist.asp (accessed Jan 2007).
- 12. Australian Bureau of Statistics. Regional population growth, Australia, 2004–05. Canberra: ABS, 2006. (ABS Cat. No. 3218.0.) http://www.ausstats.abs.gov.au/ausstats/subscriber.nsf/0/50A9687C793C52E4CA25711 D000DF7C9/$File/32180_2004-05.pdf (accessed Jan 2007).





Abstract
Objective: To describe changing patterns of skin cancer surgery by Australian general practitioners and make comparisons with specialists.
Design and setting: Analysis of Medicare Australia item number reports for skin cancer excisions and for flap and graft repairs between 2001 and 2005.
Main outcome measures: GPs’ and specialists’ rates of non-melanoma skin cancer (NMSC) excisions, melanoma excisions, flap repairs and graft repairs; excision to flap ratios.
Results: NMSC excisions in Australia increased from 338 712 (2001) to 451 628 (2005), a mean annual increase of 1.11/1000 population (P = 0.04); GPs did 51.1% of excisions in 2001, increasing to 54.4% in 2005, representing a higher mean annual rate increase than in specialists (P = 0.003). Nationally, melanoma excisions increased from 20 414 (2001) to 25 580 (2005); GPs did 34.3% of excisions in 2001, increasing to 35.8% in 2005 — a similar mean annual rate increase to that in specialists (P = 0.25). Total flap repairs increased from 58 550 (2001) to 80 742 (2005); GPs did 21.3% of flap repairs in 2001, increasing to 26.9% in 2005 — a similar mean annual rate increase to that in specialists (P = 0.83). Nationally, the excision to flap ratio for GPs fell from 14 : 1 (2001) to 12 : 1 (2005); in Queensland the ratio fell from 14 : 1 to 9 : 1 over the same period.
Conclusion: GPs excise the majority of skin cancers, and the proportion excised by GPs is increasing. GPs are increasingly using skin flaps for repair, suggesting substantial changes to patterns of treatment, especially in Queensland.