In recent years, there have been anecdotal reports of a sharp increase in demand for hospital emergency department (ED) services during the Christmas and New Year period in the New South Wales public health system (NSW is the most populous state in Australia with a population of 6.5 million1). There has been speculation that this has resulted from reduced availability of general practitioners during the holiday period. There is sparse literature on this phenomenon in Australia, except for a study of seven Sydney EDs that reported a small increase in low-acuity (“potential GP-type”) patients during the 2002–2003 holiday period.2
This phenomenon has been informally reported and debated overseas,3-10 but, to our knowledge, has not been comprehensively quantified. In the northern hemisphere, the holiday season is reported to be associated with increased demand for hospital services for cardiac and respiratory illness and injuries.11-13 The coincident influenza season may be an exacerbating factor in the northern hemisphere, but not in Australia.
Data were obtained from the NSW ED Data Collection (EDDC), a database of patient management information entered routinely in most NSW urban and larger rural and regional public hospital EDs. The EDDC captures about three-quarters of all NSW ED visits.14 It contains a deidentified record of every ED visit to participating hospitals, and includes data describing time milestones during the patient’s transit through the ED, and the patient’s age, sex, source of referral, mode of arrival, treatment acuity based on triage category, and discharge status.
We defined the Christmas and New Year period (“holiday period”) as the 28 days from 18 December to 14 January. The remainder of the year was defined as the “non-holiday period”. “More urgent” visits were those involving patients assigned a triage category15 on presentation of 1 (immediately life-threatening), 2 (imminently life-threatening) or 3 (potentially life-threatening). “Less urgent” visits were those involving patients assigned triage category 4 (potentially serious) and 5 (less urgent). “Admitted” visits were those involving patients with a discharge status of admission to an inpatient ward, admitted and transferred to another hospital, died in the ED, or were dead on arrival (if recorded). “Non-admitted” visits were the remainder. Treatment time was defined as the interval between first being seen by a clinician after triage and being ready for discharge. Geographic locations of the EDs were grouped according to the Accessibility and Remoteness Index of Australia (ARIA),16 which categorises each locality in Australia based on road distance to certain levels of goods and services. We classified the locality of each ED into urban (ARIA categories: “highly accessible” and “accessible”) and rural (“moderately accessible”, “remote” and “very remote”) areas. “GP-type visits” were defined using the Australasian College for Emergency Medicine (ACEM) criteria,2 and involved patients who: were self-referred; were assigned a less urgent triage category (4 or 5); did not arrive by ambulance; presented between 08:00 and midnight; had a treatment time of less than 60 minutes; and were subsequently discharged from the ED.
To compare ED activity in the holiday period with the non-holiday period, we used Poisson regression, appropriate for analysis of count data.17 It has the advantage that the parameter estimates from the models can be easily converted by exponentiation into relative risk ratios, which in turn can be interpreted as a percentage change in the dependent variable (weekly counts of ED visits) when comparing one subgroup of the independent variable with the other (holiday versus non-holiday period). We also included a linear time trend in the model to account for long-term changes such as population size and natural growth in ED activity.
We used this technique to conduct a “short-term” and a “long-term” analysis:
There were 44 EDs common to both analyses.
All analyses were performed with SAS, version 8.02 (SAS Institute, Cary, NC, USA).
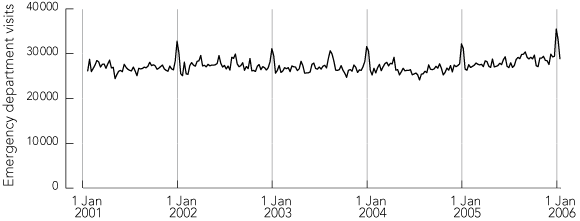
Between 2001 and early 2006, there were 7 163 497 visits to the 49 EDs. In each year, the highest weekly counts of visits occurred during the holiday period, and there was an overall upward trend in ED visits during 2005 (Box 1). The average weekly count during the holiday period was 2555 visits higher than that during the non-holiday period, representing an increase of 9% (95% CI, 7%–11%; P < 0.001) after adjusting for linear time trend (Box 2). Visits involving patients who were not admitted, whose visits were less urgent, who did not arrive by ambulance, had a shorter treatment time and arrived between 08:00 and midnight and showed even greater increases during the holiday period relative to the non-holiday period.
There were 1 433 254 visits in the short-term analysis of 48 EDs from 15 January 2005 to 14 January 2006. Overall, about a fifth were GP-type, with the proportion of GP-type visits decreasing markedly with age, and being much higher in rural areas (Box 2).
During the holiday period, there were an average additional 3494 visits each week to these 48 EDs, and 1353 additional GP-type visits (Box 2). Therefore, GP-type visits represented 39% of the additional visits. The proportion of GP-type visits during the holiday period (21%) was slightly higher than that of the non-holiday period (19%), and this pattern was evident in each age group, and in both urban and rural areas.
To our knowledge, this is the first formal study of the impact of the holiday season on ED activity. This study used routinely collected patient management information from a large number of EDs over several years. It also included a wide range of ED types, from large urban tertiary teaching hospitals to regional hospitals. It is therefore likely to be broadly representative of NSW ED activity. This study also provides valuable information on GP-type activity in EDs with wider relevance than previous, smaller studies.2,18,19 We found that the proportion of GP-type visits was highest for children, and declined with patients’ age. The proportion of GP-type activity in rural EDs was about twice that in urban EDs.
Another limitation is that we could not identify which patients could genuinely have been handled by GPs. Therefore, we had to use an indirect method of identifying these visits from the available data items. There is no generally agreed definition of ED visits that could have been managed by GPs, and a number of definitions have been used.2,18-21 One approach is based only on less urgent triage categories,21 but this has been discredited because patients in these categories often require longer consultation time, more imaging and pathology tests, and have a much higher admission rate than patients seen in general practice.2 They also have a substantial mortality rate after admission to the hospital.22 Other studies have identified common features of GP-type visits, including being self-referred, not arriving by ambulance, being assigned triage category 4 or 5, and being subsequently discharged from the ED.2,18,19 The ACEM definition we used2 was the most comprehensive available because it took into account the patient’s time of presentation and total treatment time. However, this definition is still limited because the treatment time can be affected by the seniority of treating clinicians, prevailing ED workload and turnaround time of investigations. Furthermore, the ED arrival time criterion makes no distinction between weekdays, weekends and public holidays, when GP availability could vary.
Our results suggest that ED workload during the holiday period is strongly sensitive to the supply of GP services. This is supported by the generally lower counts of GP consultations billable under Medicare in December and January.23 However, GP-type visits accounted for only 39% of the overall additional holiday visits, so other explanations are required. One possibility is that the additional ED visits may result from a real increase in the incidence of disease and injury during the holiday period. Another possibility is that reduced services over the holiday period by other health care providers, including specialists, hospital outpatient services and community-based care programs, place more burden on EDs.
- Wei Zheng1
- David J Muscatello1
- Adam C Chan2
- 1 Centre for Epidemiology and Research, New South Wales Department of Health, Sydney, NSW.
- 2 Emergency Department, St George Hospital and Community Health Services, South Eastern Sydney and Illawarra Area Health Service, Sydney, NSW.
We used administrative data routinely collected in the Emergency Department Data Collection (EDDC) in New South Wales. EDDC is freely available to all employees working for the NSW Department of Health and Area Health Services. All authors work for NSW Health and we did this study during the course of our work. Therefore, we did not receive any funding to conduct this study.
- 1. Australian Bureau of Statistics. 2006 census data. http://www.abs.gov.au/websitedbs/d3310114.nsf/home/Census+data (accessed Sep 2007).
- 2. Australasian College for Emergency Medicine. The relationship between emergency department overcrowding and alternative after-hours GP services. Melbourne: ACEM, 2004. http://www.medeserv.com.au/acem/open/documents/after_hoursgp.pdf (accessed Aug 2006).
- 3. Liu E, Wong E. Demand for accident and emergency services during public holidays. Hong Kong: Legislative Council Secretariat, 2006. http://www.legco.gov.hk/yr97-98/english/sec/library/967in01.pdf (accessed Jun 2006).
- 4. Emergency staff set for hectic holiday. Canterbury Healthline [Internet] 2001; Dec: issue 60. http://www.cdhb.govt.nz/communications/healthline/issue60.pdf (accessed Jun 2006).
- 5. Salazar A, Corbella X, Sanchez JL, et al. How to manage the ED crisis when hospital and/or ED capacity is reaching its limits. Report about the implementation of particular interventions during the Christmas crisis [letter]. Eur J Emerg Med 2002; 9: 79-80.
- 6. Rouse A. GP surgeries were hard to contact over Christmas [letter]. BMJ 1999; 218: 1422.
- 7. Tanner B. I will be in my surgery on Christmas Day if ministers and researchers are at work too [letter]. BMJ 1999; 319: 513.
- 8. McShane M. Several points need to be clarified [letter]. BMJ 1999; 319: 513.
- 9. Houghton PG. Study seems more like investigative journalism than public health research [letter]. BMJ 1999; 319: 513.
- 10. Young G. Study was ill-considered and sensationalist [letter]. BMJ 1999; 319: 513.
- 11. Phillips DP, Jarvinen JR, Abramson IS, Phillips RR. Cardiac mortality is higher around Christmas and New Year’s than at any other time: the holidays as a risk factor for death. Circulation 2004; 110: 3781-3788.
- 12. Keatinge WR, Donaldson GC. Changes in mortalities and hospital admissions associated with holidays and respiratory illness: implications for medical services. J Eval Clin Pract 2005; 11: 275-281.
- 13. Centers for Disease Control and Prevention. Fall-related injuries during the holiday season — United States, 2000–2003. MMWR Morb Mortal Wkly Rep 2004; 53: 1127-1129.
- 14. New South Wales Department of Health. Summary of NSW public hospital data, updated April 2006. http://www.health.nsw.gov.au/hospitalinfo/perfsumm.html (accessed Jul 2006).
- 15. Australasian College for Emergency Medicine. Guidelines on the implementation of the Australasian Triage Scale in emergency departments. Melbourne: ACEM, 2005. http://www.acem.org.au/media/policies_and_guidelines/G24_Implementation__ATS.pdf (accessed Jun 2006).
- 16. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. March 2004. Canberra: AIHW, 2004. (AIHW Cat. No. PHE 53.) http://www.aihw.gov.au/publications/phe/rrrh-gtrc/rrrh-gtrc.pdf (accessed Jun 2006).
- 17. Cameron AC, Trivedi PK, editors. Regression analysis of count data. Cambridge: Cambridge University Press, 1998.
- 18. Sprivulis P. Estimation of the general practice workload of a metropolitan teaching hospital emergency department. Emerg Med (Fremantle) 2003; 15: 32-37.
- 19. Forero R, Dechnicz V, Kerecz M, et al. Utilisation rates of primary care services in an emergency department. Aust Fam Physician 1994; 23: 1105-1113.
- 20. Bezzina AJ, Smith PB, Cromwell D, Eagar K. Primary care patients in the emergency department: who are they? A review of the definition of the “primary care patient” in the emergency department. Emerg Med Australas 2005; 17: 472-479.
- 21. Dent A, Rofe G, Sansom G. Which triage category patients die in hospital after being admitted through emergency departments? A study in one teaching hospital. Emerg Med 1999; 11: 68-71.
- 22. Doherty SR, Hore CT, Curran SW. Inpatient mortality as related to triage category in three New South Wales regional base hospitals. Emerg Med (Fremantle) 2003; 15: 334-340.
- 23. Medicare Australia. Medicare Benefits Schedule (MBS) group statistics reports. http://www.medicareaustralia.gov.au/statistics/dyn_mbs/forms/mbsgtab4.shtml (accessed Aug 2006).





Abstract
Objectives: To assess changes in emergency department (ED) activity and visits to EDs that could have been managed by general practitioners (GP-type visits) in the Christmas and New Year holiday period compared with the rest of the year.
Design and setting: Retrospective descriptive and analytical comparison of New South Wales ED visits in the holiday period and the rest of the year; data were obtained from the NSW Emergency Department Data Collection database for the period 2001 to early 2006. More detailed information in 2005–2006 allowed GP-type visits to be assessed in this period only.
Main outcome measures: The change in the number and percentage of weekly ED visits during the holiday period.
Results: Between 2001 and 2006, average weekly counts of ED visits increased by 9% (95% CI, 7%–11%) during the holiday period. The holiday increase was largely accounted for by visits that were less urgent, and for patients who were not admitted, did not arrive by ambulance, had a shorter treatment time and arrived between 08:00 and midnight. In 2005–2006, average weekly counts of GP-type visits increased by 21% (95% CI, 15%–28%) compared with 8% (95% CI, 4%–12%) for ED visits overall. However, GP-type visits accounted for only 39% of the additional holiday visits. GP-type visits increased mainly for adults and more in urban than rural areas.
Conclusions: The Christmas and New Year period is the busiest time of year for NSW EDs. However, only some of the additional holiday visits can be attributed to GP-type visits. Improving access to GPs, but also to broader hospital and community-based health care services over the holiday period, should be considered for managing the excess demand.