There is mounting evidence that compensation status influences patient outcomes.1-5 In a meta-analysis of 211 studies, 83% showed worse outcomes in compensated patients.2 Most studies have focused on injuries such as whiplash, and chronic and non-specific low back pain. Few have investigated the effect of compensation on outcomes after severe traumatic injury. A prospective cohort study of 120 patients with distal radius fractures identified compensation (involved in litigation or workers compensation) as a predictor of pain and disability at 6 months.5 Studies of non-neurotrauma and polytrauma found worse outcomes for patients covered by workers compensation,1,6 whereas a study of unilateral lower extremity fractures found no association with compensable or litigation status.7
In Australia, orthopaedic injury is the most common form of trauma requiring hospitalisation, with fractures recorded for 36% of admitted injured patients.8 Most orthopaedic trauma is due to transport accidents or falls. In Victoria, 46% of patients with orthopaedic trauma admitted to Level 1 trauma centres are covered by the Transport Accident Commission (TAC) “no-fault” compensation scheme.9 This scheme provides payment for medical treatment, rehabilitation services, disability services, income assistance, travel and household support services.
The aims and methods of the registry have been published elsewhere.9,10 Briefly, the VOTOR captures information from the medical record and hospital information systems and from patient interviews during the hospital stay and 12 months after injury. From the registry, we obtained patient demographics, injury event details, diagnoses according to the Abbreviated Injury Scale codes, and the Injury Severity Score (ISS). The in-hospital interview provided information on marital status, highest level of education, whether the patient was working or studying before injury, and pre-injury health status in the week before injury as measured by the 12-item Short Form Health Survey (SF-12) for physical component summary (PCS-12) and mental component summary (MCS-12) scores.11 Outcomes at 12 months after injury were collected by telephone interview, which assessed living status (eg, at home or in rehabilitation); current SF-12 scores; and return to work or study.
Analyses were performed using SPSS version 14.0 (SPSS Inc, Chicago, Ill, USA). Descriptive statistics were used to summarise the characteristics of each patient group. We used χ2 analysis to compare groups (ie, responders versus non-responders, compensable versus non-compensable) for categorical variables. Mann–Whitney and independent t tests were used to compare groups on continuous variables, depending on data distributions. P < 0.05 was considered significant. Pre-injury and 12-month post-injury PCS-12 and MCS-12 scores were compared with Australian population norms12 using means and 95% confidence intervals for each age group. Overlapping intervals were taken to represent no significant differences.
Box 1 shows the demographic and pre-injury profile of the patients. Non-compensable patients were older than compensable patients (P < 0.001).
There were differences between patient groups for injury cause, ISS, the profile of injuries sustained, and the destination following discharge from the acute hospital (Box 2). Almost 75% of compensable patients also sustained non-orthopaedic injuries, compared with 26.5% of non-compensable patients (P < 0.001). Compensable patients were more likely to have a serious head injury (OR, 3.1; 95% CI, 1.8–5.4) and a higher ISS (P < 0.001). The cause of injury reflects the criteria for TAC compensation, with all patients sustaining their injuries in transport-related incidents. A small proportion (14%) of non-compensable patients also sustained their injuries in transport-related incidents, but did not meet the criteria for TAC compensation. There was an association for discharge destination (P < 0.001), with a higher proportion of compensable patients (49%) discharged to in-patient rehabilitation centres and most non-compensable patients (82%) discharged directly home (Box 2).
The median time for completion of the pre-injury SF-12 was 7 (interquartile range, 3–13) days after injury. There was no difference in the pre-injury PCS-12 or MCS-12 scores across the groups (Box 1). At follow-up, compensable patients had lower PCS-12 (P < 0.001) and MCS-12 (P < 0.001) scores than non-compensable patients.
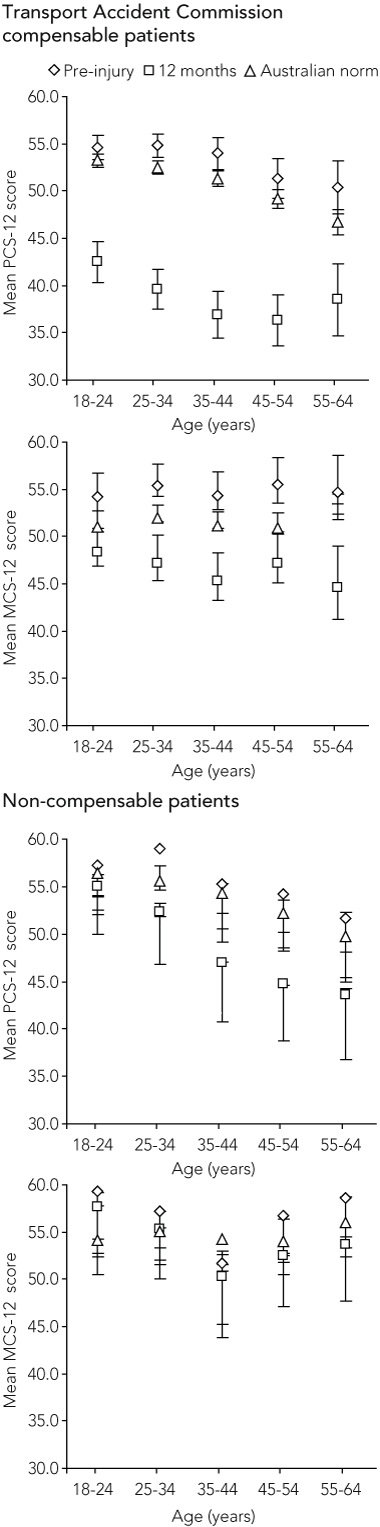
Box 3 summarises the SF-12 results for the two groups. Compensable patients had mean pre-injury PCS-12 scores above, but similar to, the population norms. By 12 months after injury, PCS-12 scores had not returned to pre-injury levels and were below population norms in every age group. A similar pattern was seen for non-compensable patients. Compensable patients reported pre-injury mental health status scores above population norms. At follow-up, MCS-12 scores remained below population norms for compensable patients. This pattern was not seen for non-compensable patients.
The residual disability 12 months after injury is consistent with other reports,6,13-16 and suggests that the aim of rehabilitation — return of the patient to the pre-injury state — had not yet been achieved. Our results are consistent with the evidence that outcomes are worse in compensable patients. Reasons proposed for the poorer health outcomes of compensable patients include the psychosocial environment of the patient before injury, the traumatic nature of the injury event, greater severity of injury, the psychosocial environment of the patient following injury, the patient’s experience within the compensation system, and illness behaviour directed towards secondary gain.1,2,4,17,18 Many of these explanations are speculative and difficult to study, but some inferences from the VOTOR data can be made.
Pre-injury MCS-12 scores did not differ for compensable and non-compensable patients. However, whether the SF-12 measures the key issues of psychosocial environment or is sensitive enough to detect finer differences between groups is unknown. A previous study found an association between traumatic origin and higher levels of pain and emotional distress among patients with chronic pain.18 As all injuries in our study were traumatic, it is unlikely that this fully explains the differences identified. The nature of the traumatic event may be more important. All compensable patients in our cohort were injured in road trauma, whereas the non-compensable patients were predominantly injured in falls. The strong correlation between compensable status and mechanism of injury precluded adjustment for this variable in the multivariate analysis. Whether the mechanism of injury or the provision of compensation was more important in explaining the poorer outcomes in the compensable group could not be determined. While a controlled trial randomising compensation status in transport-related cases would answer the question of causation, it would not be ethically or legally possible to undertake in this setting.
Assessing patients’ experiences with the compensation system is beyond the scope of the VOTOR. Almost half the compensable patients were discharged to inpatient rehabilitation, compared with only 14% of non-compensable patients. Further studies are needed to define the benefit of such programs in improving long-term outcomes. A previous study in Canada found that changing from a tort compensation system to a no-fault system resulted in significant decreases in incidence of whiplash and improved outcomes for whiplash patients.3 Our study shows that outcomes are worse even in a no-fault compensation scheme. Like other no-fault systems, the TAC system allows people who can prove fault to pursue further compensation through the courts if the injury is serious enough according to the legislation. The TAC legislation also allows for lump sum payments to people who experience permanent physical or psychological conditions. As final compensation depends on the level of disability, there is a potential for patients to overstate their limitations for secondary gain. As the VOTOR does not collect information about legal action, it was not possible to estimate this potential effect of secondary gain in explaining our findings.
The strengths of our study were the prospective design, the use of a validated health-related quality of life instrument and the focus on a broad population of patients with serious orthopaedic injuries. Nevertheless, some limitations warrant consideration. Although 69% of patients were followed up, a rate consistent with other trauma outcome studies,14-16,19,20 patients lost to follow-up tended to be young, single men whose injuries were non-compensable.
Efforts were made to adjust for potential confounders and differences between the groups. Nevertheless, the data items collected by the VOTOR are not exhaustive, and the differences seen between the groups could relate to unknown confounders. The retrospective collection of data about pre-injury status also warrants comment, as experiences after injury might influence a patient’s perception of pre-injury state.19 However, this method is commonly used because of the lack of alternative sources of information, and the data were collected soon after injury.21 Whether the multivariate analysis was sufficient to adjust for differences across the groups could be questioned.
Received 6 September 2006, accepted 15 February 2007
- Belinda J Gabbe1
- Peter A Cameron1
- Owen D Williamson1
- Elton R Edwards2
- Stephen E Graves3
- Martin D Richardson4
- 1 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
- 2 Department of Trauma Surgery, National Trauma Research Institute, Alfred Hospital, Melbourne, VIC.
- 3 Department of Medicine, University of Melbourne, Melbourne, VIC.
- 4 Department of Orthopaedics, Royal Melbourne Hospital, Melbourne, VIC.
We thank the Victorian Orthopaedic Trauma Outcomes Registry research group: Flavia Cicuttini, Donna Urquhart, Melissa Hart, Andrew Hannaford, Ann Sutherland, Deborah Harrison and Steven White. Funding was provided by the Victorian Trauma Foundation. Belinda Gabbe was supported by a Public Health Research Fellowship from the National Health and Medical Research Council.
None identified.
- 1. Zelle B, Panzica M, Vogt M, et al. Influence of worker’s compensation eligibility upon functional recovery 10 to 28 years after polytrauma. Am J Surg 2005; 190: 30-36.
- 2. Harris I, Mulford J, Solomon M, et al. Association between compensation status and outcome after surgery. JAMA 2005; 293: 1644-1652.
- 3. Cassidy J, Carroll L, Cote P, et al. Effect of eliminating compensation for pain and suffering on the outcome of insurance claims for whiplash injury. N Engl J Med 2000; 342: 1179-1186.
- 4. Paniak C, Reynolds S, Toller-Lobe G, et al. A longitudinal study of the relationship between financial compensation and symptoms after treated mild traumatic brain injury. J Clin Exp Neuropsychol 2002; 24: 187-193.
- 5. MacDermid J, Donner A, Richards R, Roth J. Patient versus injury factors as predictors of pain and disability six months after a distal radius fracture. J Clin Epidemiol 2002; 55: 849-854.
- 6. Michaels AJ, Michaels CE, Smith JS, et al. Outcome from injury: general health, work status, and satisfaction 12 months after trauma. J Trauma 2000; 48: 841-850.
- 7. MacKenzie EJ, Burgess A, McAndrew M, et al. Patient-oriented functional outcome after unilateral lower extremity fracture. J Orthop Trauma 1993; 7: 393-401.
- 8. Bradley C, Harrison J. Descriptive epidemiology of traumatic fractures in Australia. Adelaide: AIHW, 2004. (AIHW Catalogue No. INJCAT 57.)
- 9. Urquhart D, Edwards E, Graves S, et al. Characterisation of orthopaedic trauma admitted to adult Level 1 trauma centres. Injury 2006; 37: 120-127.
- 10. Urquhart D, Williamson O, Gabbe B, et al. Outcomes of patients with orthopaedic trauma admitted to Level One trauma centres. Aust N Z J Surg 2006; 76: 600-606.
- 11. Ware J, Kosinski M, Keller S. SF-12: How to score the SF-12 physical and mental health summary scales. 3rd ed. Lincoln, RI: QualityMetric Incorporated, 1998.
- 12. Avery J, Dal Grande E, Taylor A. Quality of life in South Australia as measured by the SF12 Health Status Questionnaire: population norms for 2003: trends from 1997–2003. Adelaide: South Australian Department of Human Services Population Research and Outcome Studies Unit, 2003.
- 13. Vles W, Steyerberg E, Essink-Bot M, et al. Prevalence and determinants of disabilities and return to work after major trauma. J Trauma 2005; 58: 126-135.
- 14. Morris S, Lenihan B, Duddy L, O’Sullivan M. Outcome after musculoskeletal trauma treated in a regional hospital. J Trauma 2000; 49: 461-469.
- 15. Brenneman F, Redelmeier D, Boulanger B, et al. Long-term outcomes in blunt trauma: who goes back to work? J Trauma 1997; 42: 778-781.
- 16. Holbrook TL, Anderson JP, Sieber WJ, et al. Outcome after major trauma: 12-month and 18-month follow-up results from the Trauma Recovery Project. J Trauma 1999; 46: 765-771.
- 17. Australasian Faculty of Occupational Medicine Health Policy Unit. Compensable injuries and health outcomes. Sydney: Royal Australasian College of Physicians, 2001.
- 18. Turk D, Okifuji A. Perception of traumatic onset, compensation status, and physical findings: impact on pain severity, emotional distress, and disability in chronic pain patients. J Behav Med 1996; 19: 435-453.
- 19. Watson W, Ozanne-Smith J, Richardson J. An evaluation of the Assessment of Quality of Life utility instrument as a measure of the impact of injury on health-related quality of life. Int J Inj Contr Saf Promot 2005; 12: 227-239.
- 20. Ponzer S, Bergman B, Brisman B, Johansson L. A study of patient-related characteristics and outcome after moderate injury. Injury 1996; 27: 549-555.
- 21. Ameratunga S, Norton R, Bennett D, Jackson R. Risk of disability due to car crashes: a review of the literature and methodologic issues. Injury 2004; 35: 1116-1127.





Abstract
Objective: To determine the relationship between compensable status in a “no-fault” compensation scheme and long-term outcomes after orthopaedic trauma.
Design and setting: Prospective cohort study within two adult Level 1 trauma centres in Victoria, Australia.
Participants: Blunt trauma patients aged 18–64 years, admitted between September 2003 and August 2004 with orthopaedic injuries and funded by the no-fault compensation scheme for transport-related injury, or deemed non-compensable.
Main outcome measures: 12-item Short Form Health Survey (SF-12) and return to work or study at 12 months after injury.
Results: Of 1033 eligible patients, 707 (68.8%) provided follow-up data; 450 compensable and 247 non-compensable patients completed the study. After adjusting for differences across the groups (age, injury severity, head injury status, injury group, and discharge destination) using multivariate analyses, compensable patients were more likely than non-compensable patients to report moderate to severe disability at follow-up for the physical (adjusted odds ratio [AOR], 2.0; 95% CI, 1.3–2.9), and mental (AOR, 1.6; 95% CI, 1.1–2.5) summary scores of the SF-12. Compensable patients were less likely than non-compensable patients to have returned to work or study, even after adjusting for injury severity, age, head injury status and discharge destination (AOR, 0.6; 95% CI, 0.3–0.9).
Conclusions: Patients covered by the no-fault compensation system for transport-related injuries in Victoria had worse outcomes than non-compensable patients.