There has been long-running debate about the legal status of cannabis use in a number of countries, including Australia,1-5 driven in part by concerns about an association between cannabis use and psychosis.6,7
This debate has been complicated by insufficient distinction being made between:
enduring psychotic disorders, such as schizophrenia (a clinically recognised syndrome that is chronic and recurring);8
psychotic disorders that are brief in duration, generally lasting no more than a month; and
drug-induced psychotic episodes or symptoms, thought to be directly attributable to ingestion of a drug, which remit after abstinence or acute withdrawal.8
There is good epidemiological evidence of a significant association between cannabis use and the risk of meeting criteria for schizophrenia.9,10 This does not necessarily imply that cannabis use causes schizophrenia in people who would otherwise not have developed it.11,12 There is also good evidence to suggest that cannabis use is a more important risk factor for psychotic symptoms among those with a family history of, or pre-existing, schizophrenia.10,13 Research has also suggested the potential for high doses of cannabis to trigger a short-lived psychotic episode; however, the evidence remains limited.10,14
We believe that examination of the possible relationship between cannabis use and mental health needs to be framed in the context of rates of use, rates of mental health problems, and comparison with other drugs, like methamphetamine, which also induce psychotic symptoms.15-17
Data were extracted from the National Hospital Morbidity Database (NHMD) for the period July 1993 – June 2004. The NHMD is managed by the Australian Institute of Health and Welfare (AIHW), and data are collected from all state and territory health authorities. Hospital separations refer to the reason for a patient’s stay in hospital based on his or her medical records after treatment has been completed, rather than the reason for admission. Data are coded according to the World Health Organization’s International classification of diseases (ICD).18 ICD-9-CM (ninth revision, clinical modification) was used in all jurisdictions until 1998; ICD-10-AM (tenth revision, Australian modification) was used from 1999 in South Australia, Western Australia, and Queensland, and in other jurisdictions in 1998.
The AIHW’s 2004 National Drug Strategy Household Survey (NDSHS)19 employed a multistage, stratified sampling methodology, in which the sample (n = 29 445; response rate, 48%) was stratified by geographic region, with oversampling of smaller jurisdictions. The selected respondent in each household was the person with the next birthday, and who was aged 12 years or older. The sampling frame was designed to provide (within each geographic stratum) a close-to-random sample of households. However, the resulting samples required weighting to correct for imbalances arising in the design and execution of the sampling.
Numbers of drug-induced psychosis separations per million population were standardised to the relative size of the population using the Australian Bureau of Statistics estimated Australian resident population figures, by age group, at 30 June of each year for 1993–2004, to produce “age-specific” rates.20
The number of separations with drug-induced psychosis as the primary problem among those aged 10–49 years increased from 55.5 per million population in 1993–1994 to 253.1 per million population in 2003–2004. This increase was most marked among older age groups: the age-specific rate increased fivefold among those aged 20–29 years, sixfold among those aged 40–49 years, and eightfold among those aged 30–39 years, compared with the rate among those aged 10–19 years, which was less than doubled (Box 1). Across this period, age-specific rates of drug-induced psychosis separations were consistently highest among those aged 20–29 years.
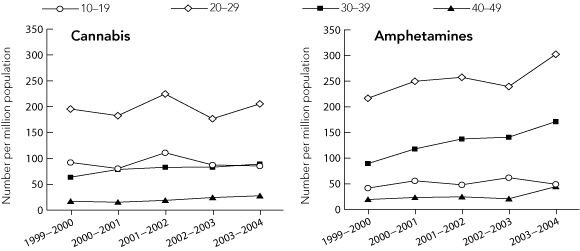
From 1999–2000 to 2003–2004, amphetamines accounted for the largest proportion of all drug-induced psychosis separations, ranging from 41% in 1999–2000 to 55% in 2003–2004, while cannabis accounted for 39%–45% of separations over this period. The number of both cannabis- and amphetamine-induced psychosis separations per million population was highest among the 20–29-year age group (Box 2). Age-specific rates among the 10–19-year age group were lower for amphetamine-induced psychosis than for cannabis-induced psychosis (41.6–61.9 and 80.5–111.1 separations per million population, respectively). Age-specific rates for cannabis-induced psychosis remained relatively stable across all age groups, compared with steady increases for amphetamine-induced psychosis. From 1999–2000 to 2003–2004, amphetamines accounted for an increasing proportion of drug-induced psychosis separations among older age groups (from 47% to 62%), while cannabis consistently accounted for around 60% of drug-induced psychosis separations among the youngest age group.
Although hospital separations due to both cannabis- and amphetamine-induced psychosis (raw numbers and age-specific rates) were highest among those aged 20–29 years (Box 3), these figures do not take into account the relative number of users of the drugs. The number of hospital separations in 2003–2004 due to cannabis- and amphetamine-induced psychosis per million users of each drug showed a distinctly different age pattern. The estimated number of cannabis-induced psychosis separations per million cannabis users was highest among the youngest age groups. In contrast, the estimated number of amphetamine-induced psychosis separations per million amphetamine users was highest among the older age groups.
NDSHS data describing the different patterns of use of these drugs (Box 4) suggested that younger cannabis users were more likely to report using very large quantities of cannabis per occasion of use (2–5 g; χ2 = 28.60; P < 0.001), despite having a lower frequency of use than older users (χ2 = 34.9; P < 0.001). There did not appear to be age-related differences in the frequency of amphetamine use. Older amphetamine users, however, were more likely than younger users to report injecting amphetamines (χ2 = 15.7; P < 0.005). They were also more likely to have used crystalline methamphetamine, whereas younger users were more likely than older users to report that they had used prescription amphetamines in tablet form (χ2 = 20.39; P < 0.001).
Despite the relationship between cannabis use and psychosis (particularly among young people) receiving increasing media attention,3,6,7 we found relatively stable numbers of hospital separations for cannabis-induced psychosis over the 5 years from 1999 to 2004. In contrast, hospital separations for amphetamine-induced psychosis had increased, particularly among those aged 20 years and older. This pattern was also evident among separations for drug-induced psychosis in general, suggesting that the increases over the decade to 2004 were driven by amphetamine rather than cannabis. Rates of hospital separations were proportionally higher for amphetamine users than cannabis users in all age groups. Although the total number of bed-days was higher for cannabis-related separations, there was a greater increase in the number of bed-days for amphetamine-related separations between 1999 and 2004.
The number of separations per million users of each drug revealed differences among the population of users. Hospitalisations for amphetamine users were highest among the older age groups, which may be due to the higher rates of injecting and of crystalline methamphetamine use reported among these groups in the NDSHS. Recent Australian research found that those reporting crystalline methamphetamine use were more likely than those using methamphetamine powder to be dependent; and dependent users were more likely to experience psychotic episodes.21 In other words, given their heavier patterns of use, crystalline methamphetamine users may be at elevated risk of psychotic symptoms compared with other methamphetamine users.
Despite these limitations, trends reported here are consistent with other indicators of cannabis and amphetamine use and related harm. Cannabis markets have remained fairly stable in Australia, while amphetamine markets have changed quite dramatically, with increasing use of crystalline methamphetamine and increasing numbers of methamphetamine laboratories.21-23 In addition, health professionals in each jurisdiction use the National health data dictionary24 to ensure coding consistency and comparability; a comprehensive compliance evaluation of the NHMD reported that the quality of principal diagnosis data at a national level “is considered to be very good”.25
One of the major limitations of the drug use data (NDSHS data) is that general population surveys are likely to underestimate the prevalence of dependent drug use.26 Although the NDSHS may not capture more disadvantaged amphetamine users, this is not likely to have a significant impact on the figures presented here. Most amphetamine users are irregular users of the drug, even when sentinel groups of regular ecstasy users are studied.19,21
1 Number of hospital separations for drug-induced* psychosis per million population by age group (years), Australia, 1993–2004†
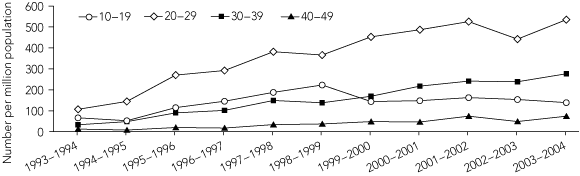
2 Number of hospital separations for drug-induced* psychosis for cannabis and amphetamines per million population by age group (years), Australia, 1999–2004†
3 Number and prevalence of drug-induced* psychosis hospital separations for cannabis and amphetamines in 2003–2004, and prevalence of use of these drugs, by age group, Australia†
* The term “drug-induced” is used for consistency with ICD-10 nomenclature; it does not imply evidence of a causal role of drugs in psychosis. † Only 2003–2004 separations data from the National Hospital Morbidity Database are included. ‡ Estimates of past year users of each drug are derived from the 2004 Australian National Drug Strategy Household Survey (NDSHS).19 § Due to restrictions on age categories, hospital separations are for those aged 10–19 years, whereas NDSHS data are for those aged 12–19 years. This may have led to an overestimate of the separations per million users for this age group; however, the number of 10–12-year old drug users is likely to be small, limiting the extent of the overestimate. | |||||||||||||||
Received 15 December 2005, accepted 9 January 2007
- Louisa Degenhardt1
- Amanda Roxburgh2
- Rebecca McKetin3
- National Drug and Alcohol Research Centre, University of New South Wales, Sydney, NSW.
This article is one of the products of the National Illicit Drug Indicators Project, which is funded by the Australian Government Department of Health and Ageing. The Department did not have any role in the study design, analysis or writing of the article. We thank Professor Richard Mattick for his comments on a final draft of the article.
None identified.
- 1. Strang J, Witton J, Hall W. Improving the quality of the cannabis debate: defining the different domains. BMJ 2000; 320: 108-110.
- 2. Lenton S. Pot, politics and the press — reflections on cannabis law reform in Western Australia. Drug Alcohol Rev 2004; 23: 223-233.
- 3. Think again on cannabis: PM. The Australian 2005; 11 Nov: Sect. 3.
- 4. Get tough on cannabis: PM. The Australian 2005; 14 Nov: Sect. 1.
- 5. Support for stiffer cannabis penalties. The Australian 2005; 23 Nov: Sect. 3.
- 6. Cannabis is worst drug for psychosis. The Australian 2005; 21 Nov: Sect. 3.
- 7. Pot psychosis? What am I saying ... er, what was I saying? The Australian 2005; 14 Nov: Sect. 10.
- 8. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Washington, DC: APA, 1994.
- 9. Degenhardt L, Hall W. Cannabis and psychosis. Curr Psychiatry Rep 2002; 4: 191-196.
- 10. Hall W, Degenhardt L, Teesson M. Cannabis use and psychotic disorders: an update. Drug Alcohol Rev 2004; 23: 433-443.
- 11. Degenhardt L, Hall W, Lynskey M. Testing hypotheses about the relationship between cannabis use and psychosis. Drug Alcohol Depend 2003; 71: 37-48.
- 12. Degenhardt L, Hall W. Is cannabis a contributory cause of psychosis? Can J Psychiatry 2006; 51: 556-565.
- 13. Henquet C, Krabbendam L, Spauwen J, et al. Prospective cohort study of cannabis use, predisposition for psychosis, and psychotic symptoms in young people. BMJ 2005; 330: 11-14.
- 14. Hall W, Degenhardt L. Is there a specific “cannabis psychosis”? In: Castle DJ, Murray R, editors. Marijuana and madness. Cambridge: Cambridge University Press, 2004: 89-100.
- 15. Connell PH. Amphetamine psychosis. Maudsley Monograph No. 5. London: Chapman and Hall, 1958.
- 16. Bell DS. The experimental reproduction of amphetamine psychosis. Arch Gen Psychiatry 1973; 29: 35-40.
- 17. Cohen SI, Johnson K. Psychosis from alcohol or drug abuse. BMJ 1988; 297: 1270-1271.
- 18. World Health Organization. The ICD-10 classification of mental and behavioural disorders — diagnostic criteria for research. Geneva: WHO, 1993.
- 19. Australian Institute of Health and Welfare. 2004 National Drug Strategy Household Survey: first results. (AIHW Cat. No. PHE 57.) Canberra: AIHW, 2005.
- 20. Bland M. An introduction to medical statistics. London: Oxford University Press, 2004.
- 21. McKetin R, McLaren J, Kelly E. The Sydney methamphetamine market: patterns of supply, use, personal harms and social consequences. NDLERF Monograph No. 13. Sydney: National Drug and Alcohol Research Centre, UNSW, 2005.
- 22. Stafford J, Degenhardt L, Dunn M, et al. Australian trends in ecstasy and related drug markets 2005: findings from the Party Drugs Initiative. NDARC Monograph No. 58. Sydney: National Drug and Alcohol Research Centre, UNSW, 2005.
- 23. Australian Crime Commission. Illicit drug data report 2003–04. Canberra: ACC, 2005.
- 24. Health Data Standards Committee. National health data dictionary. Version 13. (AIHW Cat. No. HWI 88.) Canberra: Australian Institute of Health and Welfare, 2006.
- 25. Australian Institute of Health and Welfare. National minimum data set for admitted patient care: compliance evaluation 2001–02 to 2003–04. (AIHW Cat. No. HSE 44.) Canberra: AIHW, 2006: 99.
- 26. Hall W, Ross J, Lynskey M, et al. How many dependent opioid users are there in Australia? NDARC Monograph No. 44. Sydney: National Drug and Alcohol Research Centre, UNSW, 2000.





Abstract
Objective: To examine trends in hospital separations related to “drug-induced” psychosis for cannabis and methamphetamine, in the context of patterns of cannabis and methamphetamine use in the Australian population.
Design and setting: Analysis of prospectively collected data from the National Hospital Morbidity Database on hospital separations primarily attributed to drug-induced psychosis (July 1993 – June 2004), and specifically for cannabis and amphetamines (1999–2004). Calculation of Australian population-adjusted rates of drug-induced psychosis hospital separations using estimated resident population data from the Australian Bureau of Statistics (at 30 June each year) and data on cannabis and methamphetamine use from the 2004 National Drug Strategy Household Survey.
Main outcome measures: Number of hospital separations due to drug-induced psychosis, and standardised (age-specific) rates per million population and per million users.
Results: There have been notable increases in hospital separations due to drug-induced psychosis, which appear to have been driven by amphetamine-related rather than cannabis-related episodes. The rate of hospital separations was higher for amphetamine users than for cannabis users in all age groups, and the rate increased among older amphetamine users.
Conclusions: The risk of hospitalisation for a drug-induced psychotic episode associated with amphetamine use appears to be greater than that for cannabis use in all age groups.