. . . a workforce of trained doctors working within clinical teams, who provide most front-line medical management and care for patients.1
Be fit to look after patients with acute medical problems;
Have been exposed to a range of medical career options;
Have developed a range of professional “life skills” essential for working in a health care profession, such as:
These aims could be seen as relevant to the concerns expressed in this Journal about Australian postgraduate training.2
Box 1 summarises the former arrangements for UK medical training, while Box 2 illustrates the new arrangements that will be in force from August this year.3 The main features of these new arrangements are:
A 2-year Foundation program (F1 and F2), during which trainees will normally take up a series of 4-month supervised posts in a variety of specialties in medicine, the community and surgery to help them choose a specialty earlier.
A national curriculum and national system of workplace-based assessments comprising a specified number of local case-based discussions, direct observations of procedural skills, 360-degree assessments (whereby 12 nominated colleagues rate the trainee’s performance along a series of prespecified dimensions) and mini-clinical evaluation exercises.
Immediate competitive entry into limited numbers of specialist and general practice training programs or, if unsuccessful, into fixed-term specialist training (as opposed to the former self-determined series of 6-month posts in a variety of specialties, followed by competitive entry into specialist training programs).
A Certificate of Completion of Training (as opposed to the former Certificate of Completion of Specialist Training).
An approved national curriculum for each specialty and associated workplace-based assessments and national knowledge and clinical tests.
Establish and secure standards of postgraduate medical education and training in relation to assessment, curriculum, training environments and selection;
Administer direct entry to the specialist and general practitioner registers;
Regulate, inspect and approve all aspects of the design, delivery and outcomes of postgraduate training;
Recommend trainees for entry to the appropriate General Medical Council register; and
Develop and promote postgraduate medical education and training.4
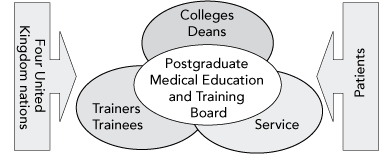
Key relationships for the PMETB are shown in Box 3. However, as the statutory body, the PMETB has the ultimate authority.
It is to be expected that changes in public services to improve cost-effectiveness will be introduced largely through the political process. However, other reasons might also be extant. Thus, in the UK, it had been noted by the Chief Medical Officer that basic specialist training (the senior house officer [SHO] grade) was a disorganised period within otherwise structured postgraduate training, and that there was a lack of curriculum and assessments in the preregistration house officer (first postgraduate year) and SHO (about the second and third postgraduate years) grades.5 Research had shown general satisfaction with higher specialist training, although some concern about the breadth and extent of clinical experience was also being expressed.6
. . . MMC aims to provide the right numbers of doctors to meet changing service needs . . . Modernising Medical Careers is . . . a key enabler for other flagship programmes in the Department of Health.7
At the same time, mainly in response to workforce pressures, UK medical schools had increased in number and size and, partially as a function of European regulations, on 7 March 2006 through the Department of Health website, the government announced changes in visa regulations for international medical graduates which in effect mean that they are no longer able to train in the UK. This is currently being opposed through legal challenge by the British Association of Physicians of Indian Origin.8
Initial responses to the proposed changes were not all positive, and a petition to parliament was proposed by the British Medical Association (BMA),9 supported by the BMA Junior Doctors Committee10 as follows:
MMC represents a huge threat to medical training. It is a political process, rushed through with minimal thought and consideration, loved by politicians, but irrelevant to patients and doctors.
It may be that the process of change management might have been better managed,11 which would have caused less anxiety on the part of existing trainees.12 Nonetheless, their concerns were concrete.
An initial evaluation of the Foundation pilot program showed that the policy of providing wider experience of specialties to enable earlier specialty choice did not meet with the success intended.13 By the end of the Foundation years, only 57% had made their specific career choice. However, two factors have mitigated this finding: firstly, many deaneries (regional postgraduate organisations responsible for implementing postgraduate medical education) have now implemented psychometric career choice guidance14 such as Sci59 Online;15 and secondly, where appropriate, medical Royal Colleges have designed curricula, now progressing through PMETB approval processes against specified curriculum standards.16 These have a common stem during the initial years of specialty training, and then allow trainees to be selected into their subspecialties at a later stage. Although this might not fit the original MMC vision of a run-through grade, it is a structure that is appropriate.
A key element of the Foundation program and MMC is the implementation of a system of four different types of workplace-based continuous assessment. A full-scale evaluation of the actual feasibility and effect of this remains to be done, but results of initial unpublished evaluations of pilot assessments are shown in Box 4. Clearly, medical Royal Colleges have no role in national assessment at this non-specialist stage of training.
The pressing timescale has precluded proper piloting of some elements of the new system, such as the selection system, which still requires national clarification, and the number of programs that will be available for each specialty and, consequently, each trainee’s chance of finding themselves in the poorly understood area of fixed-term specialty training. The assessment systems are also unlikely to be fully developed, and initially will be only approved against a subset of PMETB standards for assessment.17
The introduction by the current government of private independent treatment centres, often staffed by overseas-trained doctors, which undertake basic elective surgery that was previously an important part of junior trainees’ experience. Hansard reports that:
Market-based cost models require fast patient throughput, so that seniors rather than juniors undertake procedures.
Cost pressures and new team configurations force more straightforward definable tasks and processes, often previously performed by junior doctors, on to paramedical practitioners or other extended professionals.19
Decreased hours of work (48 hours per week by 2009) in accordance with the European Working Time Directive.20
The PMETB curriculum standards do not require new curricula to be expressed in terms of competences, although it is open to medical Royal Colleges to use this type of framework if they wish, and MMC has elected to do so for the Foundation program curriculum. It has been argued that this competence model, which was originally introduced for practical vocational subjects,21 is unsuitable for the complex integrated professional performance of medicine.22 The Australian literature has been central in this debate.23 Such models facilitate the identification of discrete tasks which, as a byproduct, can be moved to other workers, but which still may be required as the basis of more complex medical performance. Further, although competence models offer a straightforward basis for blueprinting assessments, it is nonetheless true that attaining separate competences alone does not imply the fluent, integrated, judgement-based professional performance necessary for independent practice. This requires experience over and above any basic competence. In the UK, despite government wishes, total length of training in years is unlikely to alter overall, although the amount of experience within those years will decrease, and this may lead either to a period of further training, supervision or professional induction after postgraduate programs, or a greater flow of UK doctors overseas seeking the clinical experience they require for independent practice.
Box 5 summarises the lessons for action indicated from the current UK experience of changing postgraduate medical education.
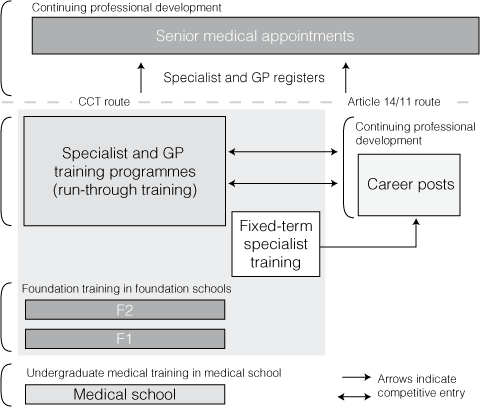
2 Modernising Medical Careers — the new structure of training in the United Kingdom as of August 2007
 | |||||||||||||||
|
The core training route would be from Foundation into specialist training programs by a competitive selection process. However, there are fewer training slots than applicants (numbers currently unclear). Those who are unsuccessful will enter fixed-term specialist training (which will offer short-term training posts) in the hope that they will be able to take up vacancies in training that arise through attrition. Foundation has workplace-based continuous assessments, as described in the text. After Foundation, the medical Royal Colleges design a system of national knowledge tests and workplace-based assessments for specialty training. These, and the curriculum, must be approved by the Postgraduate Medical Education and Training Board. Articles 11 and 14 are for doctors who have trained, at least partially, outside the European Union and demand that equivalence be demonstrated for entry onto the specialist and general practitioner registers kept by the General Medical Council. | |||||||||||||||
4 Summary of the main findings from an evaluation of Foundation pilot program workplace-based assessments*
Overall, the assessment system was valued for its educational benefit and its ability to deliver feedback to trainees.
There were mixed views about its likely validity.
Both trainees and assessors found the burden of time to organise and complete the required number of assessments an issue.
The need for adequate training for assessors was widely reported.
Changes to streamline paperwork were recommended.
Applicability of the tools to non-clinical specialties requires review.
Trainees were largely able to complete the required number of assessments of each type.
For most trainees, the assessments took 30 minutes or less each to complete. Direct observation of procedural skills was most frequently cited as taking longest.
25 trainees (34%) felt that time constraints were a barrier to proper implementation of the assessment system.
Preparation time for each assessment for most assessors was 10 minutes or less.
Time was the main barrier to successful implementation of the system for most assessors.
The basis of case selection for assessments was variable.
Most trainees (63; 85%) experienced problems in organising their assessments for a wide variety of reasons; time, identifying a consultant or registrar or other assessor, and the specialty offering few suitable assessment opportunities were cited most commonly.
25 trainees (34%) felt that the assessments gave an accurate picture of their competence, and 22 (30%) felt they did not.
9 assessors (39%) were confident that the assessments gave an accurate picture.
48 trainees (65%) felt that the assessment tools provided them with feedback on their performance.
Most assessors (18; 78%) felt that the assessment system had an educational benefit.
5 Summary of the main lessons from the United Kingdom changes in postgraduate medical education
Identify the problem. What is the evidence?
Tailor the solution.
Do not lose current strengths.
Look for perverse incentives that will trigger unintended behaviour (eg, taking shortcuts in assessment when there is insufficient time).
Don’t change just because others are.
2 Understand the difference between political and professional agendas
The profession should protect standards of training and practice despite external pressures.
Analyse what problem is being addressed. Whose problem is it?
Make the solution tackle the problem.
Stay detached from rhetoric and stick to a professional view.
3 Protection of adequate clinical experience is paramount
Postgraduate medical education is situated learning.24
Learning to be a doctor requires experiencing clinical practice and acquiring the knowledge and skill around it to be an independent practitioner. This takes time and cannot be fully orchestrated or greatly abbreviated.
If clinical experience is not protected, suspect an ulterior motive!
4 Beware of competence frameworks
Beware the limitations of competence-based curricula.
Competences alone do not describe professional performance, but deconstruct it.
Competence attainment is only the first stage in acquiring adequate, fluent professional performance.
5 Set clear standards (or principles)
Set these at an appropriate level.
Don’t micromanage.
Offer support and assistance to help trainees achieve the standards.
6 If you change trainees’ career structures, change their careers advice
- Janet R Grant1
- Open University, Milton Keynes, UK.
I received payment for travel and subsistence to attend the conference at which this article was first presented. I am a member of the UK Postgraduate Medical Education and Training Board, and the Centre in which I work produced the Sci59 Online psychometric instrument.
- 1. National Health Service Wales. Modernising medical careers. MMC: the facts. http://www.mmcwales.org/downloads/mmc19dec.pdf (accessed Mar 2007).
- 2. McGrath BP, Graham IS, Crotty BJ, Jolly BC. Lack of integration of medical education in Australia: the need for change. Med J Aust 2006; 184: 346-348. <MJA full text>
- 3. UK National Health Service. Modernising medical careers. http://www.mmc.nhs.uk/ (accessed Feb 2006).
- 4. Postgraduate Medical Education and Training Board. http://www.pmetb.org.uk/ (accessed Feb 2006).
- 5. Donaldson L. Unfinished business: proposals for reform of the Senior House Officer grade. 2002. http://www.mmc.nhs.uk/download/Unfinished-Business.pdf (accessed Feb 2006).
- 6. Open University Centre for Education in Medicine. Evaluation of the reforms to higher specialist training. 1996–1999. Final report. Milton Keynes: Open University, 2000.
- 7. UK National Health Service. Modernising medical careers. What is MMC? http://www.mmc.nhs.uk/pages/about (accessed Feb 2006).
- 8. BAPIO argument changes to the Immigration Rules applying IMG. http://www.aippg.net/forum/viewtopic.php?t=51444 (accessed Feb 2006).
- 9. MMC discussion site. http://web.mac.com/matthewstrachan/iWeb/MMC/Docs.Vs.MMC/Docs.Vs.MMC.html (accessed Feb 2006).
- 10. Conway MA. We must act to stop MMC. Hosp Doctor 2006; 21 Sep: 13.
- 11. Gale R, Grant J. Association for Medical Education in Europe Education Guides No. 10. Managing change in a medical context. Guidelines for action. Medical Teacher 1997; 19: 239-249.
- 12. Bonner J. What’s to become of SHOs? BMJ Careers 2006; 2 Sep: 83-85.
- 13. Grant J, Chambers K, Maxted M, Owen H. Identification of career intentions as a function of Foundation programme experience. Unpublished report to the Department of Health. 2005. Executive summary. http://iet.open.ac.uk/about/oucem/index.cfm?id=5145 (accessed Feb 2006).
- 14. Gale R, Grant J. Sci45: the development of a specialty choice inventory. Med Educ 2002; 36: 659-666.
- 15. Open University Centre for Education in Medicine. Sci59 Online. 2006. http://iet.open.ac.uk/about/oucem/index.cfm?id=5835 (accessed Feb 2006).
- 16. Grant J, Fox S, Kumar N, Sim E. Standards for curricula. London: Postgraduate Medical Education and Training Board, 2005. http://www.pmetb.org.uk/media/pdf/i/a/PMETB_standards_for_curricula_(March_2005).pdf (accessed Feb 2006).
- 17. Southgate L, Grant J. Principles for an assessment system for postgraduate medical training. London: Postgraduate Medical Education and Training Board, 2004.http://www.pmetb.org.uk/media/pdf/4/9/PMETB_principles_for_an_assessment_system_for_postgraduate_medical_training_(September_2004).pdf (accessed Feb 2006).
- 18. TheyWorkForYou.com. Written answers, 13 June 2006. Health independent sector treatment centres. http://www.theyworkforyou.com/wrans/?id=2006-06-13a.67861.h (accessed Feb 2006).
- 19. Freudmann M. Surgical care practitioners are having a detrimental effect on surgical training. BMJ Careers 2006; 9 Sep: 97.
- 20. Incomes Data Services. Working time. European working time directive. http://www.incomesdata.co.uk/information/worktimedirective.htm (accessed Feb 2006).
- 21. Grant J. Principles of curriculum design. Association for the Study of Medical Education Series. Understanding medical education. Edinburgh: ASME, 2006.
- 22. Grant J. The incapacitating effects of competence: a critique. Adv Health Sci Educ Theory Pract 1999; 4: 271-277.
- 23. Gonczi A, Hager P, Athanasou J. Establishing competency-based standards in the professions. National Office of Overseas Skills Recognition (NOOSR) Research Paper No. 8. Canberra: AGPS, 1993.
- 24. Lave J, Wenger E. Situated learning. Legitimate peripheral participation. Cambridge: Cambridge University Press, 1991.






Abstract
The current changes in postgraduate training in the United Kingdom are largely driven by government rather than the profession, and are aimed at producing a medical workforce more quickly and more fit-for-purpose in a rapidly changing National Health Service.
Most aspects of the changes are, as yet, untested.
Postgraduate training now consists of a 2-year varied Foundation program, followed by selection to a longer training program within a chosen specialty (often with further selection points to different subspecialties after 2 years).
Assessment systems are a combination of workplace-based assessments and national examinations of knowledge and skill.
The changing, highly managed and partially privatised health service in the UK presents challenges in terms of providing appropriate clinical experience for training.
Postgraduate medical education is now regulated by the Postgraduate Medical Education and Training Board, which sets standards for all aspects of training, and approves curricula, programs and assessment systems.
The lessons to be learned from the UK are:
When education changes, the actual rationale should be clear.
It is important to understand the difference between political and professional agendas.
Protection of adequate clinical experience is paramount.
Competence models can “instrumentalise” medical education (ie, deconstruct integrated professional performance, attempt to micromanage, streamline, objectify and rationalise for purposes of cost or time containment or for managerial imperatives).
Standards for medical education should be clear, but not at too specific a level.
If trainees’ career structures change, careers advice must also change.