The Australian Government budget for the 2006–07 financial year has an unprecedented provision for the implementation of chronic disease self-management education and training activities over the next 5 years. Major initiatives are outlined in Box 1.
The focus on self-management is not surprising given the burden of chronic disease in Australia and the shift in health policy towards patient-centred care. Chronic disease now contributes to over 70% of the disease burden in Australia, a figure that is expected to increase to 80% by 2020.4 The Australian Government has initiated a major focus on chronic disease through the National Chronic Disease Strategy, National Service Improvement Framework and the Blueprint for Chronic Disease Surveillance.1 At the policy level, self-management has risen to prominence through the National Chronic Disease Strategy. It is identified as one of four key action areas along with prevention across the continuum, strengthening early detection and early treatment, and integration and continuity of prevention and care.4 Current evidence suggests that patients with effective self-management skills make better use of health care professionals’ time and have enhanced self-care.5,6 Systematic reviews of the effectiveness of many self-management programs indicate clear clinical benefits for patients with conditions such as diabetes and hypertension, but not for arthritis (Box 2). However, such reviews are limited by the heterogeneity of interventions and outcomes.7-9
Governments have focused on formal self-management education programs to help patients engage in self-care. An example is the recent $36.2 million Australian Government Sharing Health Care Initiative, which explored the suitability of a range of education interventions (Box 3).10 Clear policy directions and the allocation of resources are positive steps towards integrating such activities within the health care system, but Australian policymakers need to take heed of outcomes from educational interventions in other countries if the proposed programs are to be viable.
In the UK, the attempt, since 2002, to integrate the Expert Patients Programme (EPP), an adaptation of the Stanford University chronic disease self-management program (Box 3), into the National Health Service (NHS) has had limited success.11,12 It was anticipated that the EPP would be a valuable option in the health care setting to help health professionals and patients to better manage chronic conditions.13 This seemingly has not been achieved. Future directions, outlined in a recent UK government white paper, Our health, our care, our say, provide for the transition of the EPP into a commercial community interest company to develop, market and deliver self-management programs.14 It is intended that the company will generate new and diverse programs that respond better to patient needs, as the recruitment of eligible patients from diverse backgrounds (eg, ethnic minorities and socially deprived groups) has, so far, been limited.12,14 Furthermore, the company will deliver programs in settings in which NHS organisations have been slow to engage.14
Contributing to the limited uptake of the EPP has been the lack of engagement by health care professionals, particularly general practitioners, who are primary conduits for patients with chronic conditions to enter self-management programs.12 Failure to effectively communicate the potential benefits of the EPP to GPs has resulted in difficulties in recruiting a sustainable number of patients to participate in programs and ensuring access for traditionally marginalised groups.12 As part of new health care reform in the UK, primary practices that actively support patient self-care strategies will gain additional resources.14
Barriers to engagement by health care professionals include uncertainty of the benefits of self-management programs and limited local evidence on the impact of such programs on patients’ self-care abilities.12 This information appears to be necessary to convince both patients and professionals of the worth of the program. Similar difficulties have been documented in the US private health care sector, where incorporation of self-management programs within Kaiser Permanente (a health maintenance organisation) met with resistance from health care professionals because the scope and purpose were not well understood.15
Another factor that has limited the reach of self-help programs is the low profile of self-management within the broader community. Reliance on social marketing alone to raise awareness and encourage patient self-referral to programs is labour-intensive and time-consuming and does not sufficiently engage marginalised sectors of the community.12 This has led to concerns that self-management activities are increasing social inequities, as people with limited education and low economic resources are not being reached.16
In the UK and the US, where attempts have been made to widely implement self-management education programs, the Stanford program has been used.12,15 However, trials have not provided convincing evidence of the generalisability of the program, given that men and ethnic groups are greatly under-represented in most studies.9,17 In terms of the latter, such issues are beginning to be addressed through cultural adaptation of the program.18 However, as evidenced by the EPP, reliance on one type of program clearly has limitations and fails to utilise other available interventions (Box 4). Evaluation of the Australian Sharing Health Care Initiative has shown that educational interventions with the greatest health impact are those with a flexible approach to both delivery and program content.10
The current national policy focus and resource allocation towards chronic disease prevention and management provide a unique opportunity for real advancement in Australian public health. Self-management education programs are a vehicle for helping patients develop skills and techniques to enhance self-care of their chronic conditions. Based on what we have learnt from international experience, success will be dependent on several factors (Box 5). Engagement of and endorsement by health care professionals will be critical to ensuring that there are sufficient numbers of people who have the capacity to attend and sustain programs and benefit from them.
The Council of Australian Governments’ health services package has prioritised the enhancement of federal and state government primary care programs and services to reduce inefficiencies.1 However, the diversity of organisations and health care professionals involved in providing programs and services across states and territories requires a localised rather than a uniform approach to enhance service coordination.
Models such as Primary Care Partnerships, as adopted in Victoria, have facilitated the formation of alliances among health care agencies and professionals in both metropolitan and regional settings. These partnerships vary in structure and size, covering between two and four municipal/regional areas.19 Funding is provided to support partnership formation, establishment of structured referrals and information management processes to maximise patient access to services and programs. Such a model could be adapted to improve service coordination and facilitate education and training among health care professionals to support chronic disease management. However, networks would also need to encompass local acute sectors to ensure continuity of care. Funding from both federal and state governments could be devolved to dedicated coordinating agencies within the formal networks (eg, community health centres) to pool resources and oversee effective information transfer across networks to enhance a multidisciplinary care approach. Such formal networks would serve as a platform to help integrate self-management education programs across sectors.
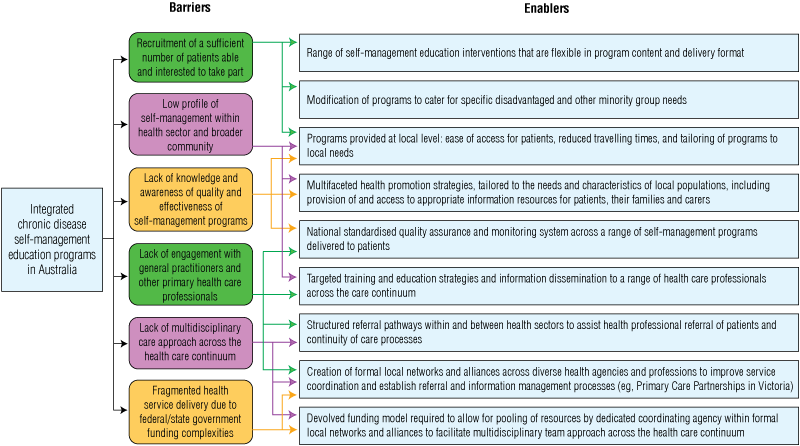
Another important factor for optimising uptake of a range of self-management programs at the local level would be raising awareness among health care professionals and fostering their confidence in the quality of the programs. This is being addressed through a component of the Sharing Health Care Initiative, which is expanding a national quality and monitoring system using the Health Education Impact Questionnaire. The questionnaire, developed by the University of Melbourne, gathers and distributes information on the key indicators of successful self-management courses (Box 6).20 The data will provide local evidence on patient outcomes — an important factor in achieving the endorsement of health care professionals. Key barriers to and enablers for integration of self-management programs in Australia are highlighted in Box 7.
1 Australian Government 2006–07 budget initiatives relating to chronic disease self-management
$250 million over 5 years as part of the Australian Government’s health services package, Promoting good health, prevention and early intervention, with patient self-management to be one of five key programs included in the package. This will be complemented by an additional $250 million from states and territories.1
$14.8 million over 4 years to continue to fund awareness and educational strategies promoting effective management and self-management of arthritis and osteoporosis. These activities will be supplemented by the development and implementation of clinical guidelines and a national data and monitoring program.2
Over $250 000 allocated for the 2006–07 financial year for a new education, training and support program targeted at general practitioners, general practice nurses, allied health workers and other professionals.3
3 Chronic disease self-management education programs used in the Australian Government’s Sharing Health Care Initiative10
Stanford University chronic disease self-management program
Six-week (2.5 hours per week) generic program
Courses led by trained lay leaders and health care professionals
Group-based format
Content includes how to manage pain and fatigue; understanding medication use; managing anger, fear and frustration; solving health-related problems; and better communication with doctors
4 Examples of self-management education interventions
Coaching patients On Achieving Cardiovascular Health (COACH) program |
|||||||||||||||
UK National Health Service’s Expert Patients Programme online |
|||||||||||||||
5 Factors essential for advancing chronic disease self-management education programs in Australia
Effective training and information for general practitioners and other health care professionals that provide local and international evidence on the effectiveness of self-management programs across disease and care continuums
Provision of a suite of self-management education interventions that are flexible and cater for patient needs across the disease continuum
A robust standardised quality assurance and monitoring system to enhance confidence that programs delivered are achieving valuable outcomes for patients
Delivery of programs at the local level (rather than institutionally based) to encourage community ownership and enhance sustainability
Standardised referral processes across health and community settings to improve coordination and access to programs
- Joanne E Jordan1
- Richard H Osborne2
- Arthritis Foundation of Victoria Centre for Rheumatic Diseases, Department of Medicine, University of Melbourne, Melbourne, VIC.
None identified.
- 1. Australian Government Department of Health and Ageing. COAG health services — promoting good health, prevention and early intervention. Fact sheet. Canberra: Commonwealth Government, 2006. http://www.health.gov.au/internet/budget/publishing.nsf/Content/budget2006-hfact37.htm (accessed May 2006).
- 2. Australian Government. Budget. Part 2: expense measures. Canberra: Commonwealth Government, 2006. http://www.budget.gov.au/2006-07/bp2/download/bp2_expense.pdf (accessed May 2006).
- 3. Australian Government Department of Health and Ageing. Portfolio budget statement, outcome 5: primary care. Canberra: Commonwealth Government, 2006. http://www.health.gov.au/internet/budget/publishing.nsf/Content/budget2006-portfoliobudgetstatements.htm (accessed May 2006).
- 4. National Health Priority Action Council. National chronic disease strategy. Canberra: Australian Government Department of Health and Ageing, 2006.
- 5. Barlow JH, Turner AP, Wright C. A randomised controlled study of the arthritis self-management program in the UK. Health Educ Res 2000; 15: 665-680.
- 6. Lorig KR, Sobel DS, Stewart AL, et al. Evidence suggesting that a chronic disease self-management program can improve health status while reducing hospitalisation: a randomised trial. Med Care 1999; 37: 5-14.
- 7. Chodosh J, Morton S, Mojica W, et al. Meta-analysis: chronic disease self-management programs for older adults. Ann Intern Med 2005; 143: 427-438.
- 8. Warsi A, Wang PS, LaValley MP, et al. Self-management education programs in chronic disease. Arch Intern Med 2004; 164: 1641-1649.
- 9. Warsi A, LaValley MP, Wang PS, et al. Arthritis self-management education programs: a meta-analysis of the effect on pain and disability. Arthritis Rheum 2003; 48: 2207-2213.
- 10. Australian Government Department of Health and Ageing. Sharing Health Care Initiative. Executive summary and discussion. Canberra: Commonwealth Government, 2005. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/chronicdisease-nateval (accessed May 2006).
- 11. Bury M, Ink D. The HSJ debate. Self-management of chronic disease doesn’t work. Health Serv J 2005; 115: 18-19.
- 12. Kennedy A, Gately C, Rogers A. National evaluation of the expert patients programme. Manchester, UK: National Primary Care Research and Development Centre, 2004. http://www.npcrdc.ac.uk/PublicationDetail.cfm?ID=105 (accessed May 2006).
- 13. Donaldson L. Expert patients usher in a new era of opportunity for the NHS. BMJ 2003; 326: 1279-1280.
- 14. UK Department of Health. Our health, our care, our say: a new direction for community services. London: DH, 2006. http://www.dh.gov.uk/assetRoot/04/12/74/59/04127459.pdf (accessed May 2006).
- 15. Lorig KR, Hurwicz ML, Sobel DS, et al. A national dissemination of an evidence-based self-management program: a process evaluation study. Patient Educ Couns 2005; 59: 69-79.
- 16. Foster M, Kendall E, Dickson P, et al. Participation and chronic disease self-management: are we risking inequitable resource allocation? Aust J Primary Health 2003; 9: 132-140.
- 17. Sheikh A, Netuveli G, Kai J, Panesar SS. Comparison of reporting of ethnicity in US and European randomised controlled trials. BMJ 2004; 329: 87-88.
- 18. Griffiths C, Motlib J, Azad A, et al. Randomised controlled trial of a lay-led self-management programme for Bangladeshi patients with chronic disease. Br J Gen Pract 2005; 55: 831-837.
- 19. Australian Institute for Primary Care, La Trobe University. An evaluation of the Primary Care Partnership Strategy. 2005. http://www.health.vic.gov.au/pcps/evaluation/index.htm (accessed Aug 2006).
- 20. Nolte S, Elsworth G, Sinclair A, Osborne RH. The extent and breadth of benefits from participating in chronic disease self-management courses: a national patient-reported outcomes survey. Patient Educ Couns 2006 Oct 4; [Epub ahead of print].





Abstract
Chronic disease self-management education programs aim to empower patients through providing information and teaching skills and techniques to improve self-care and doctor–patient interaction, with the ultimate goal of improving quality of life.
The recent 2006–07 federal budget allocated an unprecedented $515 million over 5 years for activation of patient self-management activities, commencing this financial year.
Previous attempts in other countries to incorporate self-management education activities into the health care sector have faced setbacks because of inadequate integration into primary care.
Engagement of health care professionals and their endorsement of self-management activities is critical to success.