The area covered is about 269 224 km2. According to Australian Bureau of Statistics census data for 2001,1 Aboriginal and Torres Strait Islander (ATSI) people represent 14.5% of the region’s total population. Over a third of the communities in the region have populations of less than 500.
Our study was the first review of data collected by the Paediatric Outreach Service.
Communities in which Torres Strait Islanders were predominant (“Torres Strait Islander communities”) (n = 2; these two communities are the referral points for all Torres Strait Islander communities, of which there are at least 10);
Communities in which Aboriginal people were predominant (“Aboriginal communities”) (n = 10); and
Communities in which neither Aboriginal people nor Torres Strait Islanders were predominant (“non-ATSI predominant communities”) (n = 5).
Ethical approval was obtained from Cairns Base Hospital Ethics Committee.
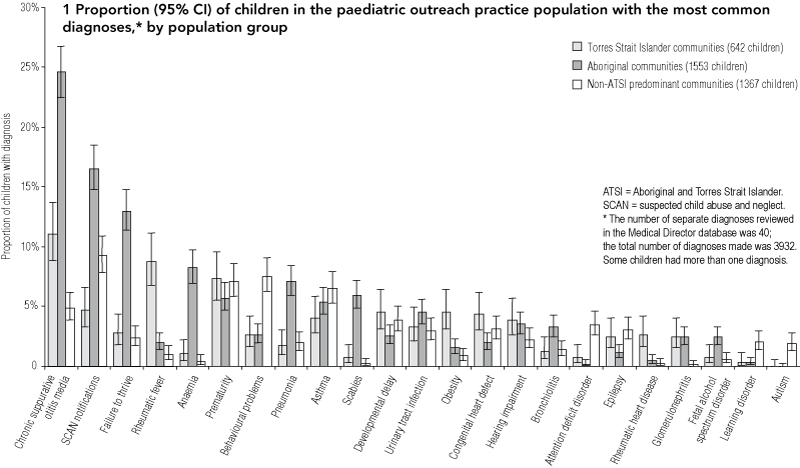
The frequencies of the 23 most common diagnoses made in the paediatric outreach practice population are shown in Box 1.
The prevalences of 10 key diagnoses (distinguished by their high prevalence and significant health implications) in children of the Aboriginal and Torres Strait Islander communities are shown in Box 2. The estimated prevalences of these diagnoses in the total Aboriginal and Torres Strait Islander paediatric populations of the communities in the outreach area (based on 2001 census data, and assuming all cases in the communities were seen by the outreach service) are also shown.
Our review of the Medical Director database provides a measure of the burden of complex and chronic disease among ATSI children in remote FNQ. Chronic suppurative otitis media, suspected child abuse and neglect notifications, and failure to thrive were the three most common reasons for referral to the outreach service (Box 1). In comparison, for the state of Queensland overall, the leading causes of disease burden among children aged 5–14 years are asthma, attention deficit disorder and depression.2 The prevalences of acute rheumatic fever, rheumatic heart disease and fetal alcohol spectrum disorder in the census paediatric population of these communities (Box 2) were as great or greater than the prevalences in other similar populations.3,4 Mental illness was under-represented in our study population, as Queensland’s Child and Youth Mental Health Service receives mental illness referrals directly. Behavioural problems were also under-represented. This may be related to the anecdotal low rate of school attendance in these communities and subsequent lack of referrals, but requires further investigation.
The estimated prevalence of chronic suppurative otitis media in all Aboriginal children in the communities visited by the service in remote FNQ was 14.7%. A 1996 World Health Organization report stated that a prevalence of over 4% for this disease was considered a public health emergency.5 Furthermore, the estimated prevalence of hearing impairment in this population was 2.0%, which has significant implications for the children’s speech development and learning potential.6
An estimated 12.8% of all children in the Aboriginal communities visited by the service were subjects of alleged abuse and neglect. In comparison, for Queensland as a whole in 2001 and 2002, 1.4% of ATSI children and 0.8% of non-ATSI children were subjects of substantiated abuse and neglect.2 Although our data do not identify substantiation, this rate of referral is likely to reflect serious social problems in these communities.
Fetal alcohol spectrum disorder had an estimated prevalence of 1.5% in the Aboriginal paediatric population. In one of the Cape York communities in the outreach area, the prevalence was 3.6%. By comparison, the highest reported prevalence outside Australia is 0.5% in South Africa.4 Fetal alcohol spectrum disorder causes lifelong disability due to intellectual impairment. In one study, no child with this condition who was followed into adulthood achieved age-appropriate socialisation or communication skills.7 In addition to existing alcohol prohibition and health education, initiatives are required to reduce alcohol consumption by pregnant women in these communities.
From our data, the estimated prevalence of congenital heart disease was 1.2% in both Aboriginal and Torres Strait Islander paediatric communities. The prevalence of rheumatic heart disease in the Torres Strait Islander paediatric population was 0.6%, and prevalence of the disease among Aboriginal adults in the Northern Territory is even higher (1.0%).3
In communities covered by the outreach service, the incidence of rheumatic fever was 2.5 cases per 1000 children per year in Aboriginal communities and 4.5 cases per 1000 children per year in Torres Strait Islander communities. These figures are much higher than the incidence of 0.002 cases per 1000 population per year for Queensland as a whole (statewide prevalence for 2001–2005, 0.88/100 000),8 but lower than rates in the NT, which has the highest reported incidence of rheumatic fever in the world (2–6 cases per 1000 children per year).3 Improvement of existing primary and secondary rheumatic fever prevention programs is necessary.
Data had to be carefully reviewed to take into consideration errors in documentation of community of residence, omission of ATSI status, and inconsistency in usage of diagnostic terms. For example, there was negligible chronic lung disease recorded in the population studied. Given that the prevalence of chronic lung disease in Aboriginal children in central Australia is 1.5%, the possibility of recording errors or misdiagnosis needs to be considered.9 Also, the high rate of suspected child abuse and neglect notifications in the non-ATSI predominant communities may partly reflect the presence of ATSI children living under adoption or in foster care with non-ATSI families. However, this cannot be confirmed due to poor recording of data on ATSI status in this population.
Our audit identified disturbingly high rates of chronic suppurative otitis media, suspected child abuse and neglect, failure to thrive, fetal alcohol spectrum disorder, rheumatic fever and rheumatic heart disease among paediatric populations in remote FNQ Aboriginal and Torres Strait Islander communities compared with other paediatric populations.2-5 These complex and chronic conditions are largely preventable, and our findings suggest deficiencies in existing primary health care activities in the region. Disease-specific preventive health initiatives as well as universal child health promotion activities in these communities need reassessment. Social and economic disparities as key contributors to these morbidities also need urgent attention. Furthermore, the data support the need for key specialist and allied health services, as part of an effective primary health care service, to manage these complex and chronic conditions.
1 Proportion (95% CI) of children in the paediatric outreach practice population with the most common diagnoses,* by population group
- Jonty Rothstein1
- Richard Heazlewood2
- Marnie Fraser2
- 1 Kimberley Aboriginal Medical Services Council, Broome, WA.
- 2 Cairns Base Hospital, Cairns, QLD.
We would like to thank Dr Carmel Nelson, Dr Alex Balzarelli, Sue Metcalf, Julia Marley, Carole Honner, Kate Gale and the Kimberley Aboriginal Medical Services Council.
None identified.
- 1. Australian Bureau of Statistics. Population distribution, Aboriginal and Torres Strait Islander Australians, 2001. Canberra: ABS, 2002: 42-44, 46. (ABS Cat. No. 4705.0.) http://www.abs.gov.au/Ausstats/abs@.nsf/ca79f63026ec2e9cca256886001514d7/7243c2de7b43332aca2568a900143cbd!OpenDocument (accessed Apr 2007).
- 2. Harper C, Cardona M, Bright M, et al. Health determinants Queensland 2004. Brisbane: Public Health Services, Queensland Health, 2004.
- 3. Carapetis JR, Wolff DR, Currie BJ. Acute rheumatic fever and rheumatic heart disease in the Top End of Australia’s Northern Territory. Med J Aust 1996; 164: 146-149.
- 4. Centers for Disease Control and Prevention (CDC). Fetal alcohol syndrome — South Africa, 2001. MMWR Morb Mortal Wkly Rep 2003; 52: 660-662.
- 5. Prevention of hearing impairment from chronic otitis media. Report of a WHO/CIBA Foundation Workshop held at the CIBA Foundation, London, 19–21 Nov 1996. London: CIBA Foundation, 1996. (WHO/PDH/98.4.) http://www.who.int/pbd/deafness/en/chronic_otitis_media.pdf (accessed Apr 2007).
- 6. Blair EM, Zubrick SR, Cox AH, on behalf of the WAACHS Steering Committee. The Western Australian Aboriginal Child Health Survey: findings to date on adolescents. Med J Aust 2005; 183: 433-435. <MJA full text>
- 7. Streissguth AP, Aase JM, Clarren SK, et al. Fetal alcohol syndrome in adolescents and adults. JAMA 1991; 265: 1961-1967.
- 8. Communicable Diseases Unit, Queensland Health. Notifiable conditions counts and rates 2001–2005 by Area Health Service and Health Service District. Brisbane: Queensland Health, 2006: 11. http://www.health.qld.gov.au/phs/Documents/cdu/31764.pdf (accessed Apr 2007).
- 9. Chang AB, Grimwood K, Mullholland EK, Torzillo PJ, for the Working Group on Indigenous Paediatric Respiratory Health. Bronchiectasis in Indigenous children in remote Australian communities. Med J Aust 2002; 177: 200-204. <MJA full text>





Abstract
Aim: To describe the pattern of disease and other health problems in children living in remote Far North Queensland (FNQ).
Design, setting and participants: Retrospective review of the FNQ Paediatric Outreach Service’s Medical Director database for the period June 2001 to February 2006. Three subpopulations were compared: children from predominantly Aboriginal communities, predominantly Torres Strait Islander communities, and other communities. All children referred to the service during the study period were reviewed.
Main outcome measures: Number of children seen and common diagnoses.
Results: 3562 children were referred during the study period, and a total of 3932 diagnoses were made; 56% of the paediatric population of the Aboriginal communities and 23% of the paediatric population of Torres Strait Islander communities were seen. Of 40 separate diseases/health problems reviewed, the three most common reasons for presentation were chronic suppurative otitis media, suspected child abuse and neglect, and failure to thrive. In the paediatric population of Aboriginal communities, the prevalence of fetal alcohol spectrum disorder was at least 15/1000 (1.5%), and in Torres Strait Islander children, rheumatic heart disease prevalence was at least 6/1000 (0.6%). Rheumatic fever rates were among the highest in Australia.
Conclusion: Rates of preventable complex and chronic health problems in Aboriginal and Torres Strait Islander children in remote FNQ are alarmingly high. Areas requiring urgent public health intervention include alcohol-related conditions and rheumatic fever.