The first major report of falls from ladders as a significant cause of mortality and morbidity was published in 1981.1 Single-centre studies in Australia2,3 and overseas studies4-7 have all concluded that falls from ladders result in significant mortality and morbidity, demanding focused injury prevention efforts. Understanding the epidemiology of falls from ladders is crucial for developing targeted prevention strategies with the greatest potential for reducing incidence.
Data on all patients who presented to the ED of a Victorian public hospital after a fall from a ladder during the study period were obtained from the Victorian Emergency Minimum Dataset (VEMD). It is estimated that more than 80% of ED presentations are included in this dataset.8 Data on injured patients classified as major trauma were obtained from the Victorian State Trauma Outcome Registry and Monitoring (VSTORM) Group database. Inclusion criteria for the VSTORM database have been previously described,9 and include any of the following: death due to injury; an Injury Severity Score > 15; urgent surgery; or an intensive care unit stay of more than 24 hours requiring mechanical ventilation. VSTORM collects data on all major trauma cases for Victoria, and data quality checks are performed against other databases including Victorian Admitted Episode Data, Death Registry and Hospital databases. All VSTORM cases were admitted through the ED. In both datasets, ladder-related falls were identified by the inclusion of the word “ladder” in the text narrative of the injury event and “fall” as the recorded cause of injury.
Stata (StataCorp, College Station, Tex, USA) was used for all analyses. Population estimates for Victoria were obtained from the Australian Bureau of Statistics.10 Descriptive statistics were used to summarise the profiles of ED presentations and major trauma cases. Population-based incidence rates (95% CIs) were calculated for each 12-month period based on the total population at the end of June 2002, 2003, 2004 and 2005. A Poisson regression model was used to test for a dose–response effect of increasing incidence over the 4 years by assuming a linear increase in the logarithm of the rate with increasing calendar years. The incidence rate ratio (IRR) and 95% CIs were calculated; a P value < 0.05 was considered significant.
During the study period, 4553 patients presented to Victorian public hospital EDs with injuries from falling from a ladder. Of these, 160 patients were classified as major trauma cases on the basis of VSTORM inclusion criteria. Box 1 shows the profile of ladder-related falls presentations to EDs and cases classified as major trauma. The vast majority of patients presenting to EDs and sustaining major trauma from ladder falls were men.
Presentations to the ED for ladder falls were most common in the 50–59-years age group (Box 1). Forty per cent of ED presentations, and 70% of major trauma cases involved people aged 50 years or more. A fall from a height greater than 1 metre was the most common mechanism of injury, accounting for 59% of ED presentations and 91% of major trauma cases. About 20% of ladder-related falls resulting in ED presentations and major trauma occurred while people were working for income. Over a quarter of people presenting to EDs after ladder-related falls (1191; 26.1%) were admitted to hospital (this excludes ED short-stay admissions). Overall, there were 16 deaths (0.3% of people falling from ladders) and all were related to a fall from a height of over a metre (Box 1).
Box 2 shows the population-based rates for ED presentations and major trauma from ladder-related falls over the 4 years to 30 June 2005. Since 2001, there has been a significant increase in the incidence of falls resulting in major trauma (P < 0.001; IRR, 1.33; 95% CI, 1.15–1.54) and emergency department presentations (P < 0.001; IRR, 1.05; 95% CI, 1.02–1.08).
The incidence of ED presentations and major trauma in patients aged less than 50 years and 50 years or more is shown in Box 3. Since July 2001, there had been a significant increase in the incidence of ED presentations (P < 0.001; IRR, 1.10; 95% CI, 1.06–1.14) and major trauma cases (P < 0.001; IRR, 1.41; 95% CI, 1.19–1.67) related to ladder falls in those aged 50 years or more. The rate of ladder-related falls leading to ED presentations and major trauma for those less than 50 years has not changed.
The incidence of ladder-related ED presentations and major trauma cases grouped by whether or not patients were working for income at the time of their fall over the period of the study is illustrated in Box 4. While the incidences of ED presentations and major trauma cases from ladder falls in the workplace have not changed significantly, there was a significant increase in the incidence of ladder-related major trauma (P < 0.001; IRR, 1.40; 95% CI; 1.19–1.65) and ED presentations (P < 0.001; IRR, 1.09; 95% CI, 1.06–1.12) over the 4 years of the study.
Our population-based study shows that ED presentations following ladder falls increased significantly in 2001–2005. In particular, there has been a significant rise in serious injury from ladder falls, especially in Victorians aged 50 years and over and in people using ladders for non-work related purposes. Our findings also support the results of a recent single-centre Australian study that found an increasing number of falls from ladders at home and involving the elderly.3
There has not been a strategic approach to prevention of injuries related to falls from ladders outside the workplace. The cause of falls in any age group is a combination of intrinsic and extrinsic factors once a person is exposed to the risk. We propose the framework shown in Box 5 (based on a National Health and Medical Research Council publication11) for categorising the causes of falls from ladders. Each factor in Box 5 can be used to direct strategies for preventing falls. Various programs aimed at reducing falls at home exist, and a similar approach could be used to target falls from ladders.
Climbing ladders at home is a risk behaviour that requires targeted modification. Home visits by occupational therapists have been used successfully to reduce low falls after hospital discharge.12 Home environment assessments, installation of safety devices and educational programs have also been used to significantly reduce falls among the elderly.13,14
Risk assessment through interviews combined with feedback and counselling sessions have been successful strategies.15 Education in small groups results in more behavioural changes than individual education.16 A recent report on the “Stepping On” program, which included home environmental safety assessments and education in small groups to reduce the risk of falls in the elderly, showed a 31% reduction in falls in the intervention group.17 Ladder falls differ from low falls in that most of the successful interventions for prevention of repeated low falls occur after an initial fall, which allows targeted education messages. More general educational programs could be provided through community health centres, local councils, sporting and cultural groups.
1 Profile of presentations to emergency departments and major trauma cases resulting from ladder falls in Victoria (2001–2005)
2 Incidence (95% CI) of falls from ladders leading to emergency department presentations and major trauma in Victoria, 2001–2005
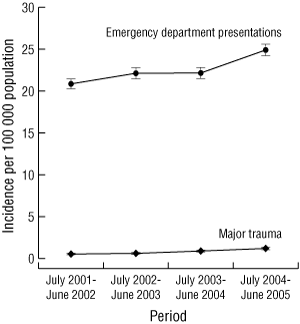
3 Incidence (95% CI) of falls from ladders leading to emergency department presentations and major trauma in patients aged < 50 years and ≥ 50 years in Victoria, 2001–2005
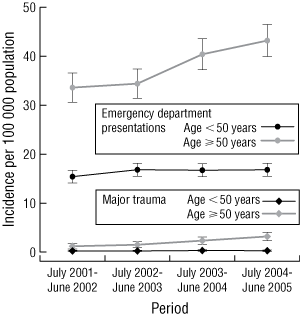
4 Incidence (95% CI) of emergency department presentations and major trauma related to ladder falls in Victoria (2001–2005) by activity at the time of injury
Received 18 April 2006, accepted 18 September 2006
- Biswadev Mitra1
- Peter A Cameron1,2
- Belinda J Gabbe2
- 1 Emergency and Trauma Centre, The Alfred Hospital, Melbourne, VIC.
- 2 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
Belinda Gabbe was supported by a Public Health Fellowship from the National Health and Medical Research Council. We thank: Mr Andrew Hannaford from the Victorian State Trauma Outcomes Registry and Monitoring Group for help with the database search of the Victorian State Trauma Registry; Ms Angela Clapperton from Victorian Injury Surveillance and Applied Research System for providing data from the Victorian Emergency Minimum Dataset; and Associate Professor Rory Wolfe at the Department of Epidemiology and Preventive Medicine, Monash University, Melbourne for help with the statistical analysis.
None identified.
- 1. Coleman PJ. Epidemiologic principles applied to injury prevention. Scand J Work Environ Health 1981; 7 Suppl 4: 91-96.
- 2. Tsipouras S, Hendrie JM, Silvapulle MJ. Ladders: accidents waiting to happen. Med J Aust 2001; 174: 516-519.
- 3. Kent A, Pearce A. Review of morbidity and mortality associated with falls from heights among patients presenting to a major trauma centre. Emerg Med Australas 2006; 18: 23-30.
- 4. O’Sullivan J, Wakai A, O’Sullivan R, et al. Ladder fall injuries: patterns and cost of morbidity. Injury 2004; 35: 429-431.
- 5. Muir L, Kanwar S. Ladder injuries. Injury 1993; 24: 485-487.
- 6. Partridge RA, Virk AS, Antosia RE. Causes and patterns of injury from ladder falls. Acad Emerg Med 1998; 5: 31-34.
- 7. Bjornstig U, Johnsson J. Ladder injuries: mechanisms, injuries and consequences. J Safety Res 1992; 23: 9-18.
- 8. Stokes M, Ozanne-Smith J, Harrison J, Steenkamp M. Validation of an injury surveillance epidemiological data system used within emergency departments. Int J Inj Control Saf Promot 2000; 7: 219-232.
- 9. Cameron P, Finch C, Gabbe B, et al. Developing Australia’s first statewide trauma registry: what are the lessons? ANZ J Surg 2004; 74: 424-428.
- 10. Australian Bureau of Statistics. Population by age and sex, Victoria. Canberra: ABS, 2006. (ABS Cat. No. 3235.2.55.001.)
- 11. National Health and Medical Reseach Council. Falls and the older person. Series on clinical management problems in the elderly (rescinded). Canberra: NHMRC, 1999.
- 12. Cumming RG, Thomas M, Szonyi G, et al. Home visits by an occupational therapist for assessment and modification of environmental hazards: a randomized trial of falls prevention. J Am Geriatr Soc 1999; 47: 1397-1402.
- 13. Stevens M, Holman C, Bennett N, de Klerk N. Preventing falls in older people: outcome evaluation of a randomized controlled trial. J Am Geriatr Soc 2001; 49: 1448-1455.
- 14. Pardessus V, Puisieux F, Di Pompeo C, et al. Benefits of home visits for falls and autonomy in the elderly: a randomized trial study. Am J Phys Med Rehabil 2002; 81: 247-252.
- 15. Gallagher E, Brunt H. Head over heels: impact of a health promotion program to reduce falls in the elderly. Can J Aging 1996; 15: 84-96.
- 16. Ryan J, Spellbring A. Implementing strategies to decrease risk of falls in older women. J Gerontol Nurs 1996; 22: 25-31.
- 17. Clemson L, Cumming R, Kendig H, et al. The effectiveness of a community-based program for reducing the incidence of falls in the elderly: a randomized trial. J Am Geriatr Soc 2004; 52: 1487-1494.





Abstract
Objective: To describe the epidemiology of falls from ladders in a state-wide population.
Design and setting: Retrospective review of data from the the Victorian State Trauma Registry and the Victorian Emergency Minimum Dataset on patients presenting to public hospital emergency departments (EDs) with injuries due to a fall while climbing a ladder, from 1 July 2001 to 30 June 2005.
Main outcome measures: Overall trends in the incidence of ladder-related ED presentations, and in cases of major trauma, trends according to age, and trends according to activity at the time of the fall.
Results: 4553 patients presented to EDs after falls from ladders in Victoria during the study period; 160 patients had injuries classified as major trauma. There has been a significant rise in the number of presentations to EDs following falls from ladders in Victoria, with a marked increase in the number of cases involving patients aged over 50 years and those climbing ladders outside of paid working conditions. Deaths occurred predominantly in the elderly after falls from heights above 1 metre.
Conclusions: Despite knowledge of the dangers of falls from ladders, there has been a significant increase in the number of patients presenting to hospitals after ladder falls. Middle-aged to elderly patients undertaking unpaid work account for this increase. A targeted public health initiative is required to curb this trend.