Perinatal care of the extremely low gestation and extremely low birthweight infant has improved. Although the boundary of viability has been challenged and has shifted over the past two decades,1-4 there is substantial risk of long-term neurodevelopmental disabilities in very premature babies who survive.5-9 A number of international guidelines on managing premature babies at the threshold of viability, formulated predominantly by physician expert panels, have been published. These guidelines acknowledge that, within boundaries set by birthweight and gestational age, there is a discretionary zone (a “grey zone”) in which attitudes of parents and clinicians play an important role (Box 1).10-14
The debate on management of neonates at the threshold of viability is an emotive and complex issue that involves families, clinicians and other health care professionals.15-19 In view of this, and in contrast with previously published guidelines prepared by expert panels, it was considered desirable to conduct a consensus workshop to bring together the views of multiple stakeholders, including consumers. The workshop, with participants from New South Wales and the Australian Capital Territory, had two aims:
To produce consensus statements to support clinicians and parents in dealing with the challenging scenarios encountered at the borderlines of viability; and
To agree on accurate, meaningful and consistent information across NSW and the ACT for clinicians, parents and prospective parents of extremely premature infants.
In planning the workshop, the organising group was cognisant of adult learning principles.20 All participants would be actively involved and have experience of the dilemma in practice. It was crucial to achieve meaningful consensus by involving as many well informed stakeholders as possible, with a spread of urban and rural professionals as well as parents. Each of the 10 tertiary neonatal intensive care units in NSW and the ACT were invited to send professional delegates from five disciplinary groups (fetomaternal obstetrics, midwifery, neonatology, neonatal nursing, and developmental teams/other allied health professionals). Representation was also invited from parental groups, professional associations, medical and nursing colleges, and rural or regional clinical practices.
Follow-up assessments of the surviving children were performed at 2–3 years of age, corrected for prematurity. Most children were assessed at a tertiary centre, but about 10% who lived too far from a major hospital were assessed by their paediatrician or general practitioner. Assessments consisted of a neurological examination and a standardised psychological assessment (the Griffiths Mental Development Scales21 and the Bayley Scales of Infant Development, second edition22).
Categories of functional disability23 were defined as:
None/minimal: developmental quotient above 1 SD below the mean;
Mild: developmental delay (developmental quotient between 1 SD and 2 SD below the mean), or mild cerebral palsy;
Moderate: developmental delay (developmental quotient between 2 SD and 3 SD below the mean), moderate cerebral palsy (able to walk with the assistance of aids), or sensorineural or conductive deafness requiring amplification with bilateral hearing aids or unilateral/bilateral cochlear implant;
Severe: developmental delay (developmental quotient more than 3 SD below the mean), bilateral blindness with visual acuity < 6/60 in the better eye, or severe cerebral palsy (unable to walk with the assistance of aids).
Statistics on births at 220 to 256 weeks’ gestation in NSW and the ACT are shown in Box 2. Infants born between these gestational ages who were not admitted to a neonatal intensive care unit (NICU) did not survive. With increasing gestational age, an increasing number of infants were born alive and admitted to an NICU.
With increasing gestational age, the proportion of infants diagnosed with mild, moderate or severe functional disability decreased. A comparison was made to a control group of 460 singleton term infants without a major congenital anomaly assessed at 3 years of age using the same assessment methods.24 Extremely premature infants were more likely than term infants to have a mild (13% v 2%), moderate (10% v 1%) or severe (16% v 0.5%) functional disability.
Final consensus statements derived from the workshop are shown in Box 3, Box 4 and Box 5. It was established early (voting results not shown) that factors including planned pregnancy, assisted conception, maternal age, maternal illness, antenatal complications and fetal conditions or compromise carried significant weight in the decision-making process. It was acknowledged that unexpected births outside tertiary perinatal centres are even more complex than births in major centres. The local team’s skills, time factors and transport logistical issues have a pivotal impact on the likelihood of a favourable outcome.
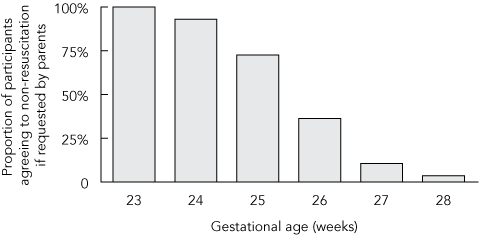
Participants were asked the highest gestational age at which they would agree, if requested by parents, not to initiate resuscitation: 100% would agree at 230–6 weeks; 72% at 250–6 weeks; and 36% at 260–6 weeks. The break-even point appears to be between 250 and 266 weeks’ gestation, below which there was a majority trend towards agreeing not to resuscitate (Box 6).
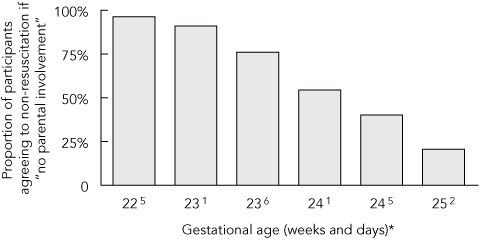
An alternative scenario attempted to remove the influence of parental request (by hypothesising a situation prior to meeting the parents). Over 90% of participants said they would not wish to initiate resuscitation at 230–6 weeks. This fell to 40% at 245 weeks, and only 20% said they would not wish to offer active treatment at 250–6 weeks (Box 7).
Participants were asked to rank the influence of certain factors on making a decision about whether to resuscitate an infant born with a known gestation of 234 weeks. Parental wishes and condition at birth were ranked as the most important issues (Box 3). Other factors included birthweight and absence of congenital abnormality. The availability of resources was ranked the least important factor. Neonatal events that would influence the offering of withdrawal of intensive care included Grade III and Grade IV brain haemorrhage (ie, major intraventricular and/or parenchymal haemorrhage) (ranked highest), ventilator dependence at 36 weeks, and the presence of necrotising enterocolitis requiring surgery.
The incidence of prematurity is currently 6.7% in NSW and the ACT.25 The risk of birth within the gestational grey zone defined in the workshop is 1 in 100, which is higher than the risk for Down syndrome, about which mothers are more likely to receive counselling. The workshop participants overwhelmingly endorsed an effort for general education in the community regarding premature births (Box 4).
The agreed grey zone was identified as between 230 and 256 weeks. The fact that gestational age assessment is not always accurate may confound management decisions. When other serious fetal conditions exist, the management principles recommended here could apply beyond this gestational range. Counselling on the options of active resuscitation and treatment within the grey zone should take into account the infant’s condition at birth, serious anomalies and other relevant factors. It is not appropriate to discuss health care resource implications during counselling. Institutions should develop decision-support management policies and procedures that are culturally sensitive and appropriate for the family and local community (Box 5).
The perinatal care of women and their babies at the borderlines of viability is a complex issue that deserves much ethical debate and consideration.24-29 The risk of infant death or survival with long-term sequelae increases acutely with each weekly (and even daily) reduction in gestational age at birth.7-9 In contrast to guidelines developed by expert panels,10-14 our consensus workshop was conducted as an interactive forum involving well informed members of multidisciplinary perinatal care teams as well as community representatives and parent advocates.
In our workshop, the debate focused on perinatal scenarios and was based on the best antenatal estimation of gestational age rather than birthweight. While it is accepted that female premature infants generally have better outcomes, this factor was not included in discussions, as sex is not usually known before birth. Poor condition at birth correlates with early mortality and morbidity.30,31 Given the uncertainties surrounding very premature births, workshop participants stressed the importance of appropriate counselling in clinical practice and developing management plans before birth.
We took the approach of establishing a grey zone of borderline viability. The grey zones defined in previous guidelines (ranging from 22 to 28 weeks) are summarised in Box 1. Common to all guidelines, parental involvement was emphasised. Each suggested the use of institutional or local outcome data to establish more precise management guidelines within the grey zone. There are inherent pitfalls in generalisation using non-local NICU outcome data, as unique local factors may influence survival and long-term outcome. For example, a US study showed that non-white infants were more likely to survive than white infants, although they did not have a better developmental outcome.7 Furthermore, NICU collaborative networks that receive data contributions from multiple geographically distant centres show differences in outcome between centres.32
A complicating factor in the debate about management of extremely premature infants is that clinicians, nurses and parents tend to have differing views about the advisability of active intervention and the health-related quality of life of surviving children. Studies surveying parents of very premature infants and surviving teenage children who had themselves been extremely low birthweight infants (less than 1000 g) have shown that consumers (parents and teenagers) are more likely than health professionals to believe that treatment was worthwhile.33-37 Australian surveys38-41 indicate that neonatologists, neonatal nurses and obstetricians tend to underestimate survival and overestimate likely disabilities. Of the three, neonatologists’ estimates of outcomes are closest to the true picture.
Another issue is the degree to which outcomes are influenced by clinicians’ attitudes. It has been shown in a population-based comparison of two perinatal management strategies that proactive management is associated with better survival of infants born in the grey zone gestational age range.42 The workshop participants considered ongoing audit of outcomes and regular updates of information as essential.
The principle of non-directive counselling (and the difficulty of achieving it) was discussed during the workshop. In a recent survey regarding counselling of parents within the grey zone, substantial differences were noted between clinicians’ and parents’ perceptions.43 Although clinicians aimed to conduct counselling sessions in a non-directive way and believed they had done so, most parents perceived the experience as directive counselling.
Workshop participants agreed that consistent, transparent information should be shared between parents and members of the perinatal team. Information on survival and long-term outcomes of very premature infants was best provided in a written form available to parents. One outcome of the workshop was to update and revise — with substantial consumer input — the NSW and ACT parent information booklet for extremely premature births.44 The objective of the booklet is to provide simple and factual information written in appropriate language for parents. It is envisaged that these efforts will be of great benefit to the counselling process.
1 Summary of published guidelines on managing premature infants at the threshold of viability (ie, in the “grey zone”)
2 “Grey zone” births* and outcomes, New South Wales and Australian Capital Territory, 1998–2000
Gestational age at birth (weeks) |
|||||||||||||||
Total births in NSW and the ACT at gestational ages of 22–25 weeks |
|||||||||||||||
Infants with IVH Grade III or IV or parenchymal cysts at 6 weeks (% discharged) |
|||||||||||||||
* Births at between 22 weeks’ and 25 weeks and 6 days’ gestation.
3 Consensus statement: gestational “grey zone”
4 Consensus statement: all pregnancies
5 Consensus statement: clinical approach within the “grey zone”
- Kei Lui1,2
- Barbara Bajuk3
- Kirsty Foster4
- Arnolda Gaston3
- Alison Kent5
- John Sinn6
- Kaye Spence7
- Wendy Fischer3
- David Henderson-Smart3
- 1 Department of Newborn Care, Royal Hospital for Women, Sydney, NSW.
- 2 School of Women’s and Children’s Health, University of NSW, Sydney, NSW.
- 3 NSW Pregnancy and Newborn Services Network, Sydney, NSW.
- 4 RPA Women’s and Babies, Royal Prince Alfred Hospital, Sydney, NSW.
- 5 Centre for Newborn Care, Canberra Hospital, Canberra, ACT.
- 6 Department of Neonatology, Westmead Hospital, Sydney, NSW.
- 7 Department of Neonatology, The Children's Hospital at Westmead, Sydney, NSW.
We would like to thank the members of the Consensus Workshop Organising Committee and all workshop participants — particularly the parents, who contributed greatly to the discussions. Our external consultants included consumer groups such as Austprem, the Australian Multiple Births Association, MotherInc and Preemie-L; professional groups such as the Royal Australian and New Zealand College of Obstetricians and Gynaecologists, the Royal Australasian College of Physicians (Division of Paediatrics), the Australian College of Rural and Remote Medicine, the Australian College of Midwives, the Association of Neonatal Nurses of NSW, the Perinatal Society of Australia and New Zealand (NSW Branch); and individual consumer representatives. We also thank the hospital directors, NICU members, audit officers and follow-up teams of all tertiary neonatal units in the following hospitals: The Canberra Hospital, John Hunter Hospital, Royal Prince Alfred Hospital, Liverpool Hospital, Nepean Hospital, The Children’s Hospital at Westmead, Royal North Shore Hospital, Sydney Children’s Hospital, Westmead Hospital and the Royal Hospital for Women. Finally, we thank the babies and their families, and the nursery, obstetric and medical records staff of the obstetric and children’s hospitals in NSW and the ACT.
None identified.
- 1. Sutton L, Bajuk B. Population-based study of infants born at less than 28 weeks’ gestation in New South Wales, Australia, in 1992-3. New South Wales Neonatal Intensive Care Unit Study Group. Paediatr Perinat Epidemiol 1999; 13: 288-301.
- 2. Cust AE, Darlow BA, Donoghue DA; Australian and New Zealand Neonatal Network (ANZNN). Outcomes for high risk New Zealand newborn infants in 1998-1999: a population based, national study. Arch Dis Child Fetal Neonatal Ed 2003; 88: F15-F22.
- 3. Louis JM, Ehrenberg HM, Collin MF, Mercer BM. Perinatal intervention and neonatal outcomes near the limit of viability. Am J Obstet Gynecol 2004; 191: 1398-1402.
- 4. Serenius F, Ewald U, Farooqi A, et al. Short-term outcome after active perinatal management at 23-25 weeks of gestation. A study from two Swedish tertiary care centres. Part 2: infant survival. Acta Paediatr 2004; 93: 1081-1089.
- 5. Doyle LW, for the Victorian Infant Collaborative Study Group. Outcome to five years of age of children born at 24-26 weeks’ gestational age in Victoria. Med J Aust 1995; 163: 11-14.
- 6. Hack M, Fanaroff AA. Outcomes of children of extremely low birthweight and gestational age in the 1990s. Semin Neonatol 2000; 5: 89-106.
- 7. Hoekstra RE, Ferrara TB, Couser RJ, et al. Survival and long-term neurodevelopmental outcome of extremely premature infants born at 23-26 weeks’ gestational age at a tertiary center. Pediatrics 2004; 113 (1 Pt 1): e1-e6.
- 8. Lefebvre F, Glorieux J, St-Laurent-Gagnon T. Neonatal survival and disability rate at age 18 months for infants born between 23 and 28 weeks of gestation. Am J Obstet Gynecol 1996; 174: 833-838.
- 9. Piecuch RE, Leonard CH, Cooper BA, et al. Outcome of infants born at 24-26 weeks’ gestation: II. Neurodevelopmental outcome. Obstet Gynecol 1997; 90: 809-814.
- 10. Recommendations on ethical issues in obstetrics and gynecology by the FIGO Committee for the Study of Ethical Aspects of Human Reproduction: ethical aspects in the management of newborns at the threshold of viability. London: International Federation of Gynecology and Obstetrics, 1994: 35-37.
- 11. Fetus and Newborn Committee, Canadian Paediatric Society, Maternal-Fetal Medicine Committee, Society of Obstetricians and Gynaecologists of Canada. Management of the woman with threatened birth of an infant of extremely low gestational age. CMAJ 1994; 151: 547-553.
- 12. Gee H, Dunn P. Fetuses and newborn infants at the threshold of viability. A framework for practice. BAPM Memorandum. London: British Association of Perinatal Medicine, 2000. http://www.bapm.org/media/documents/publications/threshold.pdf (accessed Aug 2006).
- 13. MacDonald H; American Academy of Pediatrics, Committee on Fetus and Newborn. Perinatal care at the threshold of viability. Pediatrics 2002; 110: 1024-1027.
- 14. American College of Obstetricians and Gynecologists. Perinatal care at the threshold of viability. ACOG practice bulletin 38. Obstet Gynecol 2002; 100: 617-624.
- 15. Campbell DE, Fleischman AR. Limits of viability: dilemmas, decisions, and decision makers. Am J Perinatol 2001; 18: 117-128.
- 16. Doroshow RW, Hodgman JE, Pomerance JJ, et al. Treatment decisions for newborns at the threshold of viability: an ethical dilemma. J Perinatol 2000; 20: 379-383.
- 17. Kraybill EN. Ethical issues in the care of extremely low birth weight infants. Semin Perinatol 1998; 22: 207-215.
- 18. Lorenz JM. Ethical dilemmas in the care of the most premature infants: the waters are murkier than ever. Curr Opin Pediatr 2005; 17: 186-190.
- 19. Lorenz JM. Management decisions in extremely premature infants. Semin Neonatol 2003; 8: 475-482.
- 20. Knowles M. The adult learner: a neglected species. 3rd ed. Houston, Tex: Gulf Publishing, 1984.
- 21. Griffiths R. The abilities of young children. A comprehensive system of mental measurement for the first 8 years of life. Henley-on-Thames, UK: Test Agency, 1984.
- 22. Bayley N. The Bayley scales of infant development. 2nd ed. San Antonio, Tex: Psychological Corporation, 1993.
- 23. The Victorian Infant Collaborative Study Group. Postnatal corticosteroids and sensorineural outcome at 5 years of age. J Paediatr Child Health 2000; 36: 256-261.
- 24. Vincent T, Bajuk B, Sutton L, et al. Study of antecedents and outcomes of severe morbidity in term neonates in New South Wales: a comparison of major disability at 1 and 3 years. Proceedings of the 5th Annual Congress of the Perinatal Society of Australia and New Zealand. Canberra: PSANZ, 2001: 139.
- 25. Roberts CL, Algert CS, Peat B, Henderson-Smart DJ. Trends in place of birth for premature infants in NSW. J Paediatr Child Health 2004; 40: 139-143.
- 26. Davis DJ. How aggressive should delivery room cardiopulmonary resuscitation be for extremely low birth weight neonates? Pediatrics 1993; 92: 447-450.
- 27. Catlin AJ, Stevenson DK. Physicians’ neonatal resuscitation of extremely low-birth-weight preterm infants. Image J Nurs Sch 1999; 31: 269-275.
- 28. Pinkerton JV, Finnerty JJ, Lombardo PA, et al. Parental rights at the birth of a near-viable infant: conflicting perspectives. Am J Obstet Gynecol 1997; 177: 283-288; discussion pp. 288-290.
- 29. Wilder MA. Ethical issues in the delivery room: resuscitation of extremely low birth weight infants. J Perinat Neonatal Nurs 2000; 14: 44-57.
- 30. Shankaran S, Fanaroff AA, Wright LL, et al. Risk factors for early death among extremely low-birth-weight infants. Am J Obstet Gynecol 2002; 186: 796-802.
- 31. Weinberger B, Anwar M, Hegyi T, et al. Antecedents and neonatal consequences of low Apgar scores in preterm newborns: a population study. Arch Pediatr Adolesc Med 2000; 154: 294-300.
- 32. Vohr BR, Wright LL, Dusick AM, et al; Neonatal Research Network. Center differences and outcomes of extremely low birth weight infants. Pediatrics 2004; 113: 781-789.
- 33. Pinch WJ, Spielman ML. Ethics in the neonatal intensive care unit: parental perceptions at four years postdischarge. ANS Adv Nurs Sci 1996; 19: 72-85.
- 34. Lee SK, Penner PL, Cox M. Comparison of the attitudes of health care professionals and parents toward active treatment of very low birth weight infants. Pediatrics 1991; 88: 110-114.
- 35. Saigal S, Stoskopf BL, Feeny D, et al. Differences in preferences for neonatal outcomes among health care professionals, parents, and adolescents. JAMA 1999; 281: 1991-1997.
- 36. Saigal S. Perception of health status and quality of life of extremely low-birth weight survivors. The consumer, the provider, and the child. Clin Perinatol 2000; 27: 403-419.
- 37. Streiner DL, Saigal S, Burrows E, et al. Attitudes of parents and health care professionals toward active treatment of extremely premature infants. Pediatrics 2001; 108: 152-157.
- 38. Oei J, Askie LM, Tobiansky R, Lui K. Attitudes of neonatal clinicians towards resuscitation of the extremely premature infant: an exploratory survey. J Paediatr Child Health 2000; 36: 357-362.
- 39. Gooi A, Oei J, Lui K. Attitudes of Level II obstetricians towards the care of the extremely premature infant: a national survey. J Paediatr Child Health 2003; 39: 451-455.
- 40. Mulvey S, Partridge JC, Martinez AM, et al. The management of extremely premature infants and the perceptions of viability and parental counselling practices of Australian obstetricians. Aust N Z J Obstet Gynaecol 2001; 41: 269-273.
- 41. Munro M, Yu VY, Partridge JC, Martinez AM. Antenatal counselling, resuscitation practices and attitudes among Australian neonatologists towards life support in extreme prematurity. Aust N Z J Obstet Gynaecol 2001; 41: 275-280.
- 42. Hakansson S, Farooqi A, Holmgren PA, et al. Proactive management promotes outcome in extremely preterm infants: a population-based comparison of two perinatal management strategies. Pediatrics 2004; 114: 58-64.
- 43. Keenan HT, Doron MW, Seyda BA. Comparison of mothers’ and counselors’ perceptions of predelivery counseling for extremely premature infants. Pediatrics 2005; 116: 104-111.
- 44. NSW Pregnancy and Newborn Services Network. Outcomes for premature babies. An information booklet for parents. Sydney, 2006. http://www.psn.org.au/images/stories/outcomesprematurebabies.pdf (accessed Oct 2006).





Abstract
Perinatal care at the borderlines of viability demands a delicate balance between parents’ wishes and autonomy, biological feasibility, clinicians’ responsibilities and expectations, and the prospects of an acceptable long-term outcome — coupled with a tolerable margin of uncertainty.
A multi-professional workshop with consumer involvement was held in February 2005 to agree on management of this issue in New South Wales and the Australian Capital Territory. Participants discussed and formulated consensus statements after an extensive consultation process.
Consensus was reached that the “grey zone” is between 23 weeks’ and 25 weeks and 6 days’ gestation. While there is an increasing obligation to treat with increasing length of gestation, it is acceptable medical practice not to initiate intensive care during this period if parents so wish, after appropriate counselling.
Poor condition at birth and the presence of serious congenital anomalies have an important influence on any decision not to initiate intensive care within the grey zone.
Women at high risk of imminent delivery within the grey zone should receive appropriate and skilled counselling with the most relevant up-to-date outcome information. Management plans can thus be made before birth. Information should be simple, factual and consistent.
The consensus statements developed will provide a framework to assist parents and clinicians in communication, decision making and managing these challenging situations.