Suicide rates in Australia increased steadily during the 1990s, peaking in 1997 with a rate of 15 deaths per 100 000 population.1 Subsequently, the national rate appeared to plateau, with fewer deaths reported in 2002.2 In the Northern Territory, however, the age-adjusted rate of suicide has been consistently higher than the national rate since 1996, and is still rising.2-4 Only 1% of Australians live in the NT, and its demography differs substantially from that of the rest of Australia: 70% of its people live in rural areas;5 the population is relatively young (in 2002, the median age of residents was 29.9 years, 6 years lower than the national median of 35.9 years);5 Aboriginal and Torres Strait Islander people comprise nearly 30% of the population (compared with less than 4% in other Australian jurisdictions); and there are more males than females (NT Government, unpublished data).
Data were obtained from three sources: Australian Bureau of Statistics (ABS) death registration data, NT Department of Health and Community Services population data, and NT Coroner’s Office data. All deaths recorded in the ABS death registration database for the period 1981–2000 were included in our analysis. The NT Registrar of Births, Deaths and Marriages and other jurisdictional registrars collected the initial death data, including age, sex, Indigenous status and cause of death. The ABS classified the cause of death using ICD-9 (the International classification of diseases, ninth revision) for deaths registered from 1981 to 1996 and ICD-10 (10th revision) for deaths registered from 1997 to 2000. Suicide deaths were identified using ICD-9 codes E950–E959 and ICD-10 codes X60–X84. The reliability of Indigenous status in death registration data in the NT was consistently high over the study period.6,7
Deaths suspected of being due to suicide are always the subject of a coronial investigation and are not registered until investigations are complete and a cause of death is assigned. The NT Coroner used a legal basis of proof for the consideration of suicide for the period covered by our study. A finding of suicide was made when it was considered that the deceased intentionally contributed to his or her own death.8 Because of the late registration of these and other deaths, ABS death registration data were not available for all deaths occurring in 2000. To obtain complete data for suicides from 2000 to 2002, the NT Coroner’s Office granted permission for us to use individual files to collect information on the number of cases and certain factors associated with them. At the time of data collection, coronial investigations were complete for all NT deaths occurring from 2000 to 2002. Information was extracted from the Coroner’s files, under strict confidentiality and privacy conditions, with the aid of a survey instrument based on the coding instrument from the Western Australian Coroner’s database on suicide.9
Annual age-adjusted death rates by year of occurrence and Indigenous status were calculated using ABS death registration data (for 1981–1999) and NT Coroner’s Office data (for 2000 to 2002). Age standardisation was used to control for differences between the age structures of the NT and Australian populations. The 1991 Australian estimated resident population was used as the standard population.10 Suicide death rates by age group, Indigenous status and sex were calculated for the period 1981–2002.
Our article is based on data collected for the development of a suicide prevention program rather than for research.11 No individuals or communities were identified, and, therefore, there were no issues relating to confidentiality or privacy that required ethical approval prior to publication.
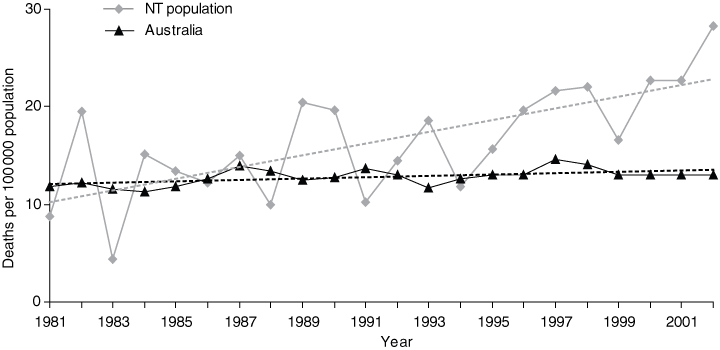
Over the 22-year period 1981–2002, there were 577 deaths due to suicide in the NT, with the overwhelming majority (504 [87%]) being in males. Seventy-five per cent of all suicides were among non-Indigenous people, who comprise 72% of the NT population. In the early 1980s, the suicide rate in the NT was similar to the Australian rate. Between 1981 and 2002, the NT rate rose significantly overall, with an average annual increase of 4.4% (P < 0.001), so that by 2000 it was nearly twice the national rate of 13.0 deaths per 100 000 population (Box 1).
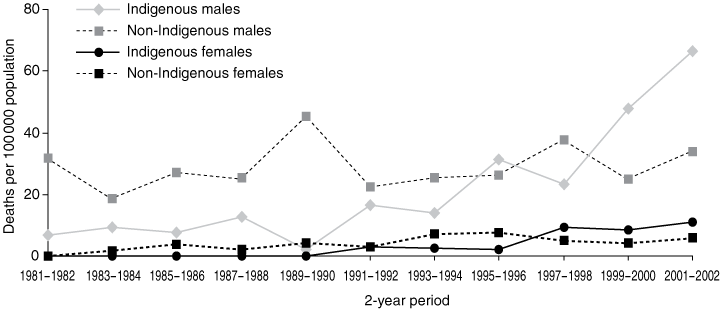
During the 1980s, the age-adjusted suicide rate for NT Indigenous males was about a third that of NT non-Indigenous males, and no suicide deaths were reported for the female Indigenous population (Box 2). However, over the period 1981–2002, the overall rate of suicide increased significantly among both Indigenous males and females, with annual average increases of 17.4% (95% CI, 12.9%–20.8%) for males and 25.8% (95% CI, 12.2%–41.0%) for females. The corresponding annual average increase was 1.2% (95% CI, 0.9%–2.9%) for non-Indigenous males and 5.7% (95% CI, 1.0%–10.8%) for non-Indigenous females.
By 2001–2002, NT Indigenous rates of suicide appeared to be substantially higher than non-Indigenous rates, although the difference was not statistically significant owing to small numbers. The 2001–2002 NT Indigenous male suicide rate of 66.3 deaths per 100 000 population was eight times higher than the corresponding rate in the 1980s and three times higher than the 2001–2002 rate for all Australian males (P < 0.05) (Box 2).
During the 1980s, the suicide rates for NT non-Indigenous males were significantly higher than the corresponding Australian rates (P < 0.05) and the rates for all other population groups in the NT (Box 2). But, unlike the Indigenous male suicide rate, the non-Indigenous male rate remained relatively stable in the 1990s. The 2001–2002 rate of 34.0 deaths per 100 000 population was about 1.5 times higher than the corresponding Australian rate, although the difference was not statistically significant (P > 0.05).
For the period 1981–2002, NT Indigenous males aged 25–44 years had the highest suicide rate of all Indigenous groups (49.5 deaths per 100 000 population) (P < 0.05) (Box 3). Indigenous males aged 10–24 years had the second highest rate (27.3 deaths per 100 000 population), and relatively few deaths were recorded for males aged 45 years and over.
In contrast, the risk of suicide appeared to increase with age among NT non-Indigenous males (Box 3). The rate for those aged 65 years and over was the highest for non-Indigenous males (54.9 per 100 000 population), but the rate may be exaggerated due to small numbers.
Between 2000 and 2002, 105 of the 141 suicide deaths (74%) in the NT were of Top End residents, who comprise 77% of the NT population. Of these 105 people, 61 (58%) had been single, widowed, divorced or separated (Box 4). In comparison, 53% of the Top End population aged 15 years and over were in this category in 2001.5 Of those completing suicide, 43 (41%) were unemployed, compared with just 4% in the Top End population (NT Government, unpublished data). Of those in employment, 28 (56%) had an occupation involving physical work, compared with just 12% in the Top End population.5
The two age groups at highest risk of suicide appear to be Indigenous males aged under 45 years and non-Indigenous males aged 45 years and over. This is similar to findings reported for Queensland, where Indigenous males in younger age groups were at greatest risk and rates for all Indigenous males were twice those reported for all Queensland males.12 The methodological differences between the Queensland study and the present study are unlikely to affect the magnitude of the difference between the various population groups.
Although NT annual suicide rates were based on small numbers and were subject to some instability, they distinctly highlight certain trends (Box 1, Box 2). But caution must be exercised in making any generalisations from our findings, given the unusual age distribution of the NT population, the relatively high proportion of Indigenous people in the NT, and the high proportion of the NT Indigenous population living in remote and very remote areas (ABS, unpublished data). A strength of our study is that it provides a more complete picture of Indigenous suicide than is possible in many other Australian jurisdictions. This is because the level of accuracy in identifying Indigenous people in routine data collections is very high in the NT and substantially better than in other Australian jurisdictions.6,7
The finding that 49% of Top End residents who completed suicide had a diagnosed mental illness or a history of attempted suicide is of concern. This result, while lower than the rate previously reported for the NT (60% of suicide cases in 1991–1998),13 is higher than that reported for Western Australia (40%) during the period 1986–1997. This may represent a real difference or may simply reflect differences in data recording.9 The significant association, reported elsewhere, between self-harm behaviour and subsequent suicide in the Indigenous population appears to be a relevant issue in the NT context.13
A recent national study by Trewin and Madden found that Indigenous males aged 25–44 years were three times more likely to be hospitalised for severe mental illness (such as schizophrenia or delusional disorders) than men in the general Australian population.14 This group had the highest suicide rate in our study.
Alcohol was involved in 56% of suicide cases, compared with 44% in a previous study of the same population in the 1990s.13 This suggests either a strengthening of the association between alcohol consumption and suicide and/or more complete testing and recording of information by the Coroner’s Office. In total, alcohol and/or drug use was recorded in 71% of suicide cases in the Top End in 2000–2002. This finding is higher than that reported in WA, where 29% of male and 21% of female suicide cases were associated with current substance misuse.9 The association between alcohol misuse and suicide is well recognised.15 This is of particular concern for the NT, where the per capita consumption of alcohol is the highest of any Australian state or territory.16
Cannabis use in the NT is also significantly higher than in the rest of Australia.17 Cannabis misuse is also likely to be more widespread in remote Australian communities than previously reported.18 There are reports of a significant association between psychiatric issues and substance misuse, and Indigenous people are four times more likely than the total Australian population to be admitted to hospital with psychiatric illness as a result of psychoactive substance misuse.14 The relationships reported elsewhere between cannabis use and depression, and cannabis use, psychosis and anxious arousal in association with substance intoxication or withdrawal, may all be factors contributing to suicide in the NT context.18-21
Issues pertinent to suicide in rural areas may provide some insight into the findings of our study. “Compositional”, “contextual” and “collective” variables22 may all have an impact on suicide in rural settings, and the meaning and further influence of suicide within a disadvantaged remote Indigenous community may also play a role.22,23
1 Age-adjusted suicide death rates (number of deaths per 100 000 population) by year and Indigenous status, Northern Territory and Australia, 1981–2002
Age-adjusted suicide rate (number of deaths per 100 000 population), NT and Australia, 1981–2002
2 Age-adjusted suicide death rates (number of deaths per 100 000 population [95% CIs]) by sex, Indigenous status and 5-year period, Northern Territory and Australia, 1981–2002
NT age-adjusted suicide rates by sex, Indigenous status and 2-year period, 1981–2002
3 Suicide death rates (number of deaths per 100 000 population [95% CIs]) by sex, Indigenous status and age group, Northern Territory and Australia, 1981–2002
Received 17 January 2006, accepted 12 July 2006
- Mary-Anne L Measey1
- Shu Qin Li1
- Robert Parker1
- Zhiqiang Wang2
- 1 Northern Territory Department of Health and Community Services, Darwin, NT.
- 2 School of Medicine, University of Queensland, Brisbane, QLD.
We would like to acknowledge the invaluable assistance provided by the NT Coroner’s Office and by the former Deputy Coroner, Lyn McDade, in particular. We would also like to thank Lindy Garling for her assistance with collecting information from the Coroner’s Office.
None identified.
- 1. Hoogland S, Pieters R. Suicide in Australia, a dying shame. Sydney: Wesley Mission, 2000.
- 2. Australian Bureau of Statistics. Causes of death, Australia, 2002. Canberra: ABS, 2003. (ABS Cat. No. 3303.0.)
- 3. Australian Bureau of Statistics. Suicides, Australia, 1921–1998. Canberra: ABS, 2000. (ABS Cat. No. 3309.0.)
- 4. Australian Bureau of Statistics. Information paper: suicides 2001. Revised ed. Canberra: ABS, 2003 (ABS Cat. No. 3309.0.55.001.)
- 5. Australian Bureau of Statistics. Census second release (summary publication), 2001. Northern Territory. Canberra: ABS, 2002. (ABS Cat. No. 2046.0.)
- 6. Plant AJ, Condon JR, Darling G. Northern Territory health outcomes, morbidity and mortality 1979–1991. Darwin: NT Department of Health and Community Services, 1995.
- 7. Li SQ, Guthridge SL. Mortality in the Northern Territory, 1981–2000. Part 1: key indicators and overview. Darwin: NT Department of Health and Community Services, 2004.
- 8. Matthews P, Foreman J. Jervis on the office and duties of coroners. 11th ed. London: Sweet and Maxwell, 1993.
- 9. Hillman S, Silburn SR, Zubrick SR, Nguyen H. Suicide in Western Australia, 1986–1997. Perth: TVW Telethon Institute for Child Health Research and Centre for Child Health Research, Faculty of Medicine and Dentistry, University of Western Australia, 2000.
- 10. Australian Bureau of Statistics. Australian demographic statistics, 1994. Canberra: ABS, 1994. (ABS Cat. No. 3101.0.)
- 11. Northern Territory Department of Health and Community Services. Northern Territory Strategic Framework for Suicide Prevention. A framework for the prevention of suicide and self-harm in the Northern Territory 2003. http://www.nt.gov.au/health/comm_svs/mental_health/framework_for_suicide_prevention.pdf (accessed Aug 2006).
- 12. De Leo D, Evans R. Suicide in Queensland 1996–1998. Mortality rates and related data. Brisbane: Australian Institute for Suicide Research and Prevention, 2002.
- 13. Parker R, Ben-Tovim DI. A study of factors affecting suicide in Aboriginal and “other” populations in the Top End of the Northern Territory through an audit of coronial records. Aust N Z J Psychiatry 2002; 36: 404-410.
- 14. Trewin D, Madden R. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples. Canberra: Australian Bureau of Statistics, 2005. (ABS Cat. No. 4704.0.)
- 15. Murphy GE. Psychiatric aspects of suicidal behaviour: substance abuse. In: Hawton K, van Heeringen K, editors. The international handbook of suicide and attempted suicide. Chichester: John Wiley and Sons, 2000.
- 16. Catalano P, Chikritzhs T, Stockwell T, et al. Trends in per capita alcohol consumption in Australia, 1990/91–1998/99. Technical report. Perth: National Drug Research Institute, Curtin University of Technology, 2001.
- 17. Australian Institute of Health and Welfare. 2001 National Drug Strategy household survey: state and territory supplement. Canberra: AIHW, 2002. (AIHW Cat. No. PHE 37.)
- 18. Clough AR, Cairney S, Maruff P, Parker R. Rising cannabis use in Indigenous communities [letter]. Med J Aust 2002; 177: 395-396. <MJA full text>
- 19. Patton GC, Coffey C, Carlin JB, et al. Cannabis use and mental health in young people: cohort study. BMJ 2002; 325: 1195-1198.
- 20. Arseneault L, Cannon M, Witton J, Murray R. Causal association between cannabis and psychosis: examination of the evidence. Br J Psychiatry 2004; 184: 110-117.
- 21. Budney AJ, Moore BA, Vandrey RG, Hughes JR. The time course and significance of cannabis withdrawal. J Abnorm Psychol 2003; 112: 393-402.
- 22. Judd F, Cooper A, Fraser C, Davis J. Rural suicide — people or place effects? Aust N Z J Psychiatry 2006; 40: 208-216.
- 23. Hunter E. Aboriginal communities and suicide. Australas Psychiatry 1996; 4: 195-199.





Abstract
Objective: To examine trends in suicide in the Northern Territory between 1981 and 2002, and demographic and other characteristics of people completing suicide in the Top End region in 2000–2002.
Design: Retrospective descriptive analysis of Australian Bureau of Statistics death registration data and data from the NT Coroner’s Office.
Setting and participants: All residents of the NT who completed suicide between 1981 and 2002.
Main outcome measures: Changes in the age-adjusted and age- and sex-specific rates of suicide in Indigenous and non-Indigenous NT residents over time; prior diagnosis of mental illness and use of alcohol or other drugs by those completing suicide.
Results: The age-adjusted suicide rate in the NT increased significantly between 1981 and 2002 (P < 0.001). Over this period, the rates among the Indigenous and non-Indigenous male populations increased by 800% (P < 0.05) and 30% (P > 0.05), respectively. Indigenous males aged under 45 years and non-Indigenous males aged 65 years and over were most at risk. In the Top End, a history of diagnosed mental illness was present in 49% of suicide cases, and misuse of alcohol or other drugs around the time of death was associated with 72% of suicide cases.
Conclusion: Our study highlights the rising rate of suicide in the NT and suggests that suicide prevention initiatives need to specifically target Indigenous and non-Indigenous males in the age groups most at risk.