Divisions of General Practice are primarily structured to support general practice and are involved in delivering practical outcomes in the health care system across the country. They have great potential for contributing to the evidence base for primary health care in Australia by undertaking appropriate and relevant general practice-based research. Despite this, a 2004 survey by General Practice Divisions Victoria found that few Victorian Divisions had been engaged in primary care research in that year.1
Collaborating with the university sector is one way for Divisions to build capacity in research expertise. Divisions frequently seek advice about research and evaluation from academic sources: 75% of the 120 Divisions in 2003 and 2004 sought advice from university academic departments, and 38% of Divisions had formal reciprocal arrangements with universities in those years.2
Researchers from universities frequently approach Divisions to gain support for and assistance with research projects by promoting the project to local general practices or actively engaging and supporting general practitioners and patients in research activities.3-5 Divisions have identified that further engagement with universities has been hindered by misunderstandings about what constitutes research, uncertainty about the purpose and nature of the research relationship between the sectors, and a perceived lack of relevance, incentives and benefits for Divisions.6
Forging links between academics and practitioners is one of the challenges for academic medicine worldwide.7 One strategy is to give practitioners more control over the research agenda relevant to their sector. In the United Kingdom, Primary Care Trusts (PCTs), the organisations responsible for managing primary care at local level, have a critical role in increasing the amount of appropriate health services research and developing a research culture. However, a study found that PCT staff did not consider research an integral part of their everyday work.8 They identified that organisational infrastructure and working environment would be important in developing research capacity,9 as well as access to academic support, training and development opportunities. Good relationships between primary care organisations and key partners such as research networks and academic units provide a sound basis for wider strategic development of research.10
In the first stage of the study, between September and October 2004, we used a strategic sampling process11 to invite participants interested in collaborative research from universities and Divisions. Sampling sources were the 2002–2003 annual survey of Divisions,12 the websites of Divisions, university departments, items published in the PHC RIS newsletter GPinfonet by departments, funded by the Research Capacity Building Initiative of the Primary Health Care Research, Evaluation and Development Strategy, presentations from General Practice and Primary Health Care Research conferences, and state and national meetings of the Divisions Network since 2001. In addition, we invited expressions of interest from Divisions and university sectors through the October 2004 ADGP newsletter and a PHC RIS email list.
During October 2004, three researchers recorded and hand-noted semi-structured telephone interviews with all participants. Interviews covered participants’ research context, capacity and partnerships. Themes were identified using a grounded conceptualisation process.11 Analysis continued until saturation (the process by which no new themes were appearing) occurred. More detail is available in our 2005 project report.13
Twenty-one people agreed to participate, three of whom were recruited by the expression of interest process. Participants included practitioner–researchers, executives and a program manager from Divisions; and university researchers, program managers and academic heads of departments. Participants were from all states and territories. Their characteristics are shown in Box 1.
Operational Division participant: Without research the organisation would not have the necessary data to prioritise funds, access and respond to community needs that arise, evaluate what works elsewhere in the region or respond authentically to community identified issues.
Operational Division participant: There is respect for where each organisation is coming from, that is, their skills and knowledge and what they bring to contribute to the partnership. The Division may not have research skills, but has knowledge of local needs and skills in dealing with members and an understanding of general practice.
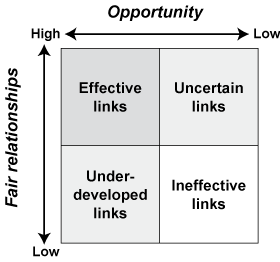
To construct a typology of the interactions, we used the previously described concept of “ideal types”,14 in which social actors (those who participate in and thus constitute social structures) interact around constructions of normative (or pure) types of interactions. These types represent the models, or range, of potential interactions, constructed from the interview themes, forming a basis by which we can better understand the relationship. We identified four types which characterise the current relationship between opportunity and fair relationships (Box 2).
Overseas work has shown that research is more likely to be relevant to practice if researchers and practitioners are engaged in productive partnerships. Locally owned and driven programs produce more useful research questions and data that are more valid for practitioners and policymakers.15 Research impact is maximised with greater involvement of stakeholders from early stages.16 Both sectors stand to benefit from collaborative research partnerships through gaining insights, expanding their roles, and improving the quality, relevance and usefulness of research.17 Clearly then, we should be creating an environment where links between Divisions and universities tend towards “effective links”. Our findings highlight five areas of practical importance for enhancing effective links between Divisions and universities: (i) gaining research and evaluation experience in Divisional contexts; (ii) leadership and funding support for the creation of effective links; (iii) addressing barriers to establishing links including cultural and funding differences; (iv) equitable partnership processes and relationships assisted by clear frameworks of engagement and protocols; and (v) improving the sustainability of links.
The federal government also has a stake in the development of effective research links between universities and Divisions of General Practice. Firstly, it is the major funder of research (both directly and through the National Health and Medical Research Council and the Australian Research Council), and the Department of Health and Ageing funds the Divisions Program and the Primary Health Care Research Evaluation and Development Strategy.18 Secondly, the planned implementation of the Research Quality Framework19 in Australia is designed to improve the assessment of the quality and impact of publicly funded research. The health-care impact of primary-care research is likely to be maximised through effective collaboration between universities and Divisions, for the reasons outlined above. Thus, universities, the Divisions and the federal government should all be striving to develop effective research links.
Received 1 March 2006, accepted 15 May 2006
- Elizabeth C Kalucy1
- Christopher M Pearce2,3
- Barbara Beacham4
- Belinda L Lowcay5
- Rachel E Yates2
- 1 Primary Health Care Research and Information Service, Flinders University, Adelaide, SA.
- 2 Australian Divisions of General Practice, Canberra, ACT.
- 3 Whitehorse Division of General Practice, Melbourne, VIC.
- 4 Cooperative Research Centre for Aboriginal Health, Darwin, NT.
- 5 The Cancer Council South Australia, Adelaide, SA.
We thank the staff from Divisions of General Practice and university researchers who participated in our study, the Australian Divisions of General Practice for their support of the project, and Dr Bronwen Veale for her contribution to the project in 2005.
The Department of Health and Ageing funded this research, but did not influence the way the research was conducted or reported.
- 1. General Practice Divisions Victoria. Research involvement: survey of research links in Victorian Divisions — 2004. Available at: http://www.phcris.org.au/go/1 (accessed June 2006).
- 2. Kalucy E, Hann K, Guy S. Divisions: the network evolves. Report of the 2003–2004 annual survey of Divisions of General Practice. Adelaide: Primary Health Care Research and Information Service and Australian Government Department of Health and Ageing, 2005. Available at: http://www.phcris.org.au/publications/pdfs_asd/2003-04/asd03_04_report+survey.pdf (accessed Jun 2006).
- 3. Harris MF, Hobbs C, Davies G, et al. Implementation of a SNAP intervention in two divisions of general practice: a feasibility study. Med J Aust 2005; 183 (10 Suppl): S54-S58. <MJA full text>
- 4. Shearer M, Pearce C. Promoting research in Divisions — a bottom-up approach. GP & PHC research conference abstracts 2004. Available at: http://www.phcris.org.au/elib/render.php?params=1087 (accessed May 2006).
- 5. Eckermann S, Kalucy E. Building partnerships: developing the right tools. PHC RIS Infonet 2005; 10(2): 8. Available at: http://www.phcris.org.au/publications/infonet/V102_05.pdf (accessed May 2006).
- 6. Yates R, Pearce C. What’s [not] working with Divisions and research? Lunch seminar, 2004 General Practice and Primary Health Care Research Conference. Available at http://www.phcris.org.au/conference/2004/other_sessions/Lunch%20seminar.pdf (accessed May 2006).
- 7. Awasthi S, Beardmore J, Clark J, et al. Five futures for academic medicine. PLoS Med 2005; 2: e207.
- 8. Harrison R. Barriers and opportunities to developing research capacity in primary care trusts: the views of staff attached to a primary care trust. Primary Care Res Develop 2005; 6: 185-189.
- 9. Whitford D, Walker C, Jelley D, et al. Developing R&D capacity in a primary care trust: use of the R&D culture index. Primary Care Res Develop 2005; 6: 17-23.
- 10. Shaw S, Macfarlane F, Greaves C, et al. Developing research management and governance capacity in primary care organisations: transferable learning from a qualitative evaluation of UK pilot sites. Fam Pract 2004; 21: 92-98.
- 11. Denscombe M. The good research guide for small-scale social research projects. 2nd ed. Philadelphia: Open University Press, 2003.
- 12. Kalucy E, Hann K, Whaites L. Divisions: a matter of balance. Results of the 2002–2003 annual survey of Divisions of General Practice. Adelaide: Primary Health Care Research and Information Service, Department of General Practice, Flinders University, and Australian Government Department of Health and Ageing, 2004. Available at: http://www.phcris.org.au/products/asd/results/02_03.php (accessed Nov 2005).
- 13. Beacham B, Kalucy L, Veale B, et al. What supports effective links between Divisions of General Practice and universities? Opportunity and fair relationships. Project report. Adelaide: Primary Health Care Research and Information Service and Australian Divisions of General Practice, 2005. Available at: http://www.phcris.org.au/publications/pdfs/Effective_links.pdf (accessed Jun 2006).
- 14. Weber M. The theory of social and economic organization. London: Collier-Macmillan, 1947.
- 15. Greenhalgh T, Robert G, Macfarlane F, et al. Diffusion of innovations in service organisations: systematic review and recommendations. Milbank Q 2004; 82: 581-629.
- 16. Lomas J. Using “linkage and exchange” to move research into policy at a Canadian foundation. Health Aff (Millwood) 2000; 19: 236-240.
- 17. Weller DP. Does academic general practice have a future? Med J Aust 2005; 183: 92-93.
- 18. Australian Government Department of Health and Ageing. General practice research. In: General practice in Australia: 2004. Canberra: Department of Health and Ageing, 2005. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/03A249B7F2345922CA25705700 121A1A/$File/Ch05.pdf (accessed Jun 2006).
- 19. Australian Government Department of Education, Science and Training. Research quality framework. Available at http://www.dest.gov.au/sectors/research_sector/policies_issues_reviews/key_issues/research_quality_framework/default.htm (accessed May 2006).





Abstract
Objective: To find out what supports effective links between Divisions of General Practice and universities.
Design: Qualitative study based on semi-structured interviews during October 2004, from which a framework for effective linking was constructed and its validity assessed by discussion with researchers and Division staff and members at four interactive workshops held between 9 November 2004 and 5 November 2005 .
Participants: 21 participants from Divisions of General Practice and universities in Australia.
Results: Qualities conceptualised as “opportunity” and “fair relationships” were critical factors in establishing successful links between the two sectors. The relationship between these two factors describes the types of interactions that currently occur.
Conclusions: To develop effective links requires an environment that promotes adequate opportunities, and in which mutual trust can grow. This will require commitment and system change from all parties.