Cataract surgery is one of the most frequently performed surgical procedures in Australia.1,2 While the private health system shoulders much of the burden for those who can afford it, many people access health care in public hospitals, where patients may have to wait long periods for clinic appointments and surgery.
In an attempt to improve access to care, a specialist nurse-led cataract clinic was introduced in the Department of Ophthalmology at Flinders Medical Centre in 2003. It was proposed that an ophthalmic nurse practitioner could assess patients for visually disabling cataract and provide specialist postoperative care for cataract surgery patients, as has occurred elsewhere.3,4 The intention of the clinic was twofold. Firstly, it would expedite direct transfer to the surgeon of patients who would benefit from cataract surgery, thus reducing waiting times and freeing up ophthalmology clinic appointments for other patients. Secondly, it would provide continuity of care for public cataract patients.
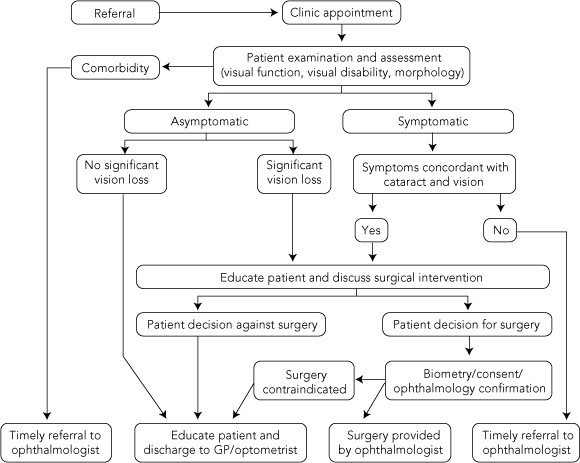
An ophthalmic nurse practitioner is an advanced clinician who has received authorisation from the state nursing board and the place of employment to work in an autonomous practice role. The clinic structure and protocols were designed in conjunction with senior ophthalmologists in the Department. The preoperative management protocol is summarised in Box 1. (Details of the postoperative management protocol are available from the authors on request.) All patients were under the care of one consultant, with surgery performed by the consultant or his fellow. Specific protocols formulated included the preoperative assessment, postoperative assessment and quality assurance mechanisms. Vicarious liability was covered by the institution of employment and under the Department of Health Professional Indemnity and Insurance Program while working within the scope of practice as a nurse practitioner. Our study was approved by the Flinders Medical Centre Ethics Committee.
At the clinic appointment, patients were given a full ocular examination and answered a cataract-specific visual disability questionnaire. Informed consent was obtained. Included in the assessment was a full medical history and VA evaluation. VA was tested on logMAR (logarithm of the minimal angle of resolution) charts using a forced-choice paradigm, five-error termination rule and by-letter scoring. A complete ocular examination, including slit-lamp and fundal check with 90D lens and binocular indirect ophthalmoscopy, was performed (essentially screening for ocular comorbidity). The Lens Opacities Classification System III was used on every patient to quantify cataract.5 The level of cataract was compared with visual performance and visual disability to determine whether the pattern was consistent.
The cataract-specific visual disability screening questionnaire (Box 2) was designed to provide a rapid qualitative assessment of the presence or absence of visual disability. The questions were drawn from the Visual Disability Assessment.6 Two broad questions (1 and 11) were included to tap any patient-specific issues. The purpose of the questionnaire was not to provide a visual disability score but to compile a checklist of potential visual difficulties. The questions were repeated after cataract surgery to determine whether disability had been reversed.
A masked diagnosis and management comparison between the ophthalmic nurse practitioner and the ophthalmologist was made at the commencement of the clinic for 1 month, then at 6-monthly intervals, again for a period of 1 month. The results from months 1, 7 and 13 are shown in Box 3.
the quality of care provided by the clinician;
explanations given by the clinician;
waiting times for the clinic appointment and surgery;
the visual outcome after surgery; and
the overall service provided by the clinic.
Respondents were asked to rate each item on a five-point scale from “very satisfied” to “very dissatisfied”.
The results of pre- and postoperative quality assurance assessments are shown in Box 3. There was complete concordance between nurse practitioner and ophthalmologist assessments. No patients had undetected ocular comorbidity, and all 20 patients referred for comorbidity were correctly diagnosed and appropriately referred.
Our results show that a nurse-led cataract clinic can function safely and efficiently and lead to good visual and patient satisfaction outcomes. Although responsible for the care of only a small proportion of the cataract surgery patients at Flinders Medical Centre, the nurse-led cataract clinic made a strong impact on the access to care for public patients. This is demonstrated by the reduction in waiting times for the initial clinic appointment and for surgery. The total waiting time for surgery was below the suggested target of Dunn and colleagues based on a survey of English cataract patients, who considered that a waiting time of 3 months or less for cataract surgery was “acceptable” and waits of over 6 months were “excessive”.7 This definition of acceptable and excessive waiting time has been adopted in the United Kingdom.8
One of the causes of clinic appointment waiting lists is referrals of patients who do not require surgery. A quarter of all patients attending the nurse-led cataract clinic were discharged from the clinic, usually because of lack of visual disability. As has been reported previously, some patients who are not yet visually debilitated are referred early to the public health system on the assumption that the wait for an appointment will be so long that they will be debilitated by the time they are seen.9 However, this often does not transpire. Lash10 suggests that improving the communication with primary care providers should increase awareness and reduce the amount of referrals of patients not requiring surgical intervention.
The results of our audit show that all patients attained 0.2 logMAR (6/9.5) or better postoperative VA and reduced visual disability. However, as the visual disability screening questionnaire elicits only the presence or absence of disability, low levels of disability may have been under-reported.11 Our results are better than cataract surgery outcomes in other studies: typically, 85% of eyes have a best-corrected acuity of 6/12 after surgery.12 This is a reflection of our selection process, which removed all patients with ocular comorbidity from the nurse-led clinic.
Our satisfaction survey revealed overwhelming patient satisfaction with the quality of care and visual outcomes, consistent with other studies of nurse-led clinics.13-15 However, satisfaction rates reflect factors not related to the clinic and are readily confounded by many factors (eg, clinician gender, patient age and health status).16,17 Reports of patient satisfaction with cataract surgery outcomes are consistently high, and driven by visual disability outcomes.18,19 However, other factors such as the adequacy of information given pre- and postoperatively are also important.20
An additional attraction of nurse-led clinics is their potential cost-effectiveness compared with medical-practitioner-led clinics. Key determinants of cost effectiveness are the years of training required,21 practitioner’s salary, time taken when consulting, costs of further clinical investigations and the cost of consumables. An ophthalmology registrar would gain competence after approximately 11 years (assuming efficient progression): basic degree (3 years), postgraduate medical degree (4 years), internship (2 years) and ophthalmology training (2 years, assuming he or she would be competent in cataract care halfway through training). An ophthalmic nurse practitioner would gain competence after approximately 8 years: Bachelor of Nursing (3 years), practical nursing experience (2 years), Ophthalmic Nursing Certificate (6 months), Master of Nursing (2 years) and setting up a hospital appointment (6 months). The salary for the nurse practitioner ($29 per hour) might be more than the junior registrar (junior to senior range $27–$35 per hour) who would otherwise perform the same role. However, a nurse practitioner might be more familiar with the specific clinic environment and more experienced in managing patients with ophthalmic conditions. Therefore, the average time for a consultation might be shorter without sacrificing quality of care. Similarly, the experienced nurse practitioner might be more efficient in use of consumables and investigations. On balance, it is likely that the nurse-led and registrar-led models would run at a similar cost and both might be considerably cheaper than a consultant-led clinic. There might be cost-effectiveness gains for the nurse practitioner model because of differences in length of training. However, for this to be assessed fully an additional specific study would be required.
2 Visual disability screening questionnaire*
1. Do you think you have a problem with your vision?
2. Do you have difficulty reading the newspaper?
3. Do you have difficulty reading the telephone book?
4. Do you find it difficult to see the TV?
5. Do you find it difficult to see the TV subtitles?
6. Have you had any falls in the street or at your home (eg, stairs, kerbs, uneven ground)?
7. Do you have any problems with driving during the day?
8. Do you have any problems with night-time driving?
9. Do you have any difficulty recognising faces?
10. Are there any hobbies that are made difficult by your poor vision?
11. Any other difficulties experienced in regards to your vision?
* Patients were asked to answer “yes” or “no” to each question.
- Bradley J Kirkwood1
- Konrad Pesudovs2
- Paul Latimer3
- Douglas J Coster4
- Department of Ophthalmology, NHMRC Centre for Clinical Eye Research, Flinders Medical Centre and Flinders University, Adelaide, SA.
Konrad Pesudovs is supported by a National Health and Medical Research Council (NHMRC) Sir Neil Hamilton Fairley Fellowship. Our project was supported by an NHMRC Centre of Clinical Research Excellence grant.
None identified.
- 1. Metropolitan Health and Aged Care Services, Department of Human Services. Victorian Ophthalmology Service Planning Framework. Discussion paper. Melbourne: Department of Human Services, 2004. Available at: http://www.health.vic.gov.au/ophthalmology/ophthservice_planning_%20discpaper.pdf (accessed Jan 2006).
- 2. Brian G, Taylor H. Cataract blindness — challenges for the 21st century. Bull World Health Organ 2001; 79: 249-256.
- 3. Herbert EN, Gibbons H, Bell J, et al. Complications of phacoemulsification on the first postoperative day: can follow-up be safely changed? J Cataract Refract Surg 1999; 25: 985-988.
- 4. Rose K, Waterman H, Toon L, et al. Management of day-surgery patients with cataract attending a peripheral ophthalmic clinic. Eye 1999; 13: 71-75.
- 5. Chylack LT Jr, Wolfe JK, Singer DM, et al. The Lens Opacities Classification System III. The Longitudinal Study of Cataract Study Group. Arch Ophthalmol 1993; 111: 831-836.
- 6. Pesudovs K, Coster DJ. An instrument for assessment of subjective visual disability in cataract patients. Br J Ophthalmol 1998; 82: 617-624.
- 7. Dunn E, Black C, Alonso J, et al. Patients’ acceptance of waiting for cataract surgery: what makes a wait too long? Soc Sci Med 1997; 44: 1603-1610.
- 8. Courtney P. The National Cataract Surgery Survey: I. Method and descriptive features. Eye 1992; 6: 487-492.
- 9. Latham K, Misson G. Patterns of cataract referral in the West Midlands. Ophthalmic Physiol Opt 1997; 17: 300-306.
- 10. Lash SC. Assessment of information included on the GOS 18 referral form used by optometrists. Ophthalmic Physiol Opt 2003; 23: 21-23.
- 11. Pesudovs K, Garamendi E, Keeves JP, Elliott DB. The Activities of Daily Vision Scale for cataract surgery outcomes: re-evaluating validity with Rasch analysis. Invest Ophthalmol Vis Sci 2003; 44: 2892-2899.
- 12. Fedorowicz Z, Lawrence D, Gutierrez P. Day care versus in-patient surgery for age-related cataract. Cochrane Database Syst Rev 2005; (1): CD004242.
- 13. Hill J. Patient satisfaction in a nurse-led rheumatology clinic. J Adv Nurs 1997; 25: 347-354.
- 14. Williams SC, Hollins D, Barden-Marshall S, Harper WM. Improving the quality of patient care: patient satisfaction with a nurse-led fracture clinic service. Ann R Coll Surg Engl 2003; 85: 115-116.
- 15. Miles K, Penny N, Power R, Mercey D. Comparing doctor- and nurse-led care in a sexual health clinic: patient satisfaction questionnaire. J Adv Nurs 2003; 42: 64-72.
- 16. Bertakis KD, Franks P, Azari R. Effects of physician gender on patient satisfaction. J Am Med Womens Assoc 2003; 58: 69-75.
- 17. Jaipaul CK, Rosenthal GE. Are older patients more satisfied with hospital care than younger patients? J Gen Intern Med 2003; 18: 23-30.
- 18. Pesudovs K, Coster D. The outcome of cataract surgery: visual disability, visual function and patient satisfaction. Invest Ophthalmol Vis Sci 1997; 38: S548.
- 19. Pager CK. Assessment of visual satisfaction and function after cataract surgery. J Cataract Refract Surg 2004; 30: 2510-2516.
- 20. Pager CK, McCluskey PJ. Public versus private patient priorities and satisfaction in cataract surgery. Clin Experiment Ophthalmol 2004; 32: 482-487.
- 21. Netten A, Knight J. Annuitizing the human capital investment costs of health service professionals. Health Econ 1999; 8: 245-255.





Abstract
Objective: To describe the implementation of a nurse-led preoperative cataract assessment and postoperative care clinic and to assess the safety, efficacy and outcomes.
Design, setting and participants: A prospective study involving 185 public patients (221 eyes) referred to the Department of Ophthalmology at Flinders Medical Centre for cataract surgery. The study was conducted between February 2003 and August 2004.
Interventions: Patients were assessed in the nurse-led preoperative assessment clinic. Those deemed suitable for cataract surgery were also assessed by an ophthalmologist and underwent cataract surgery if appropriate. The nurse managed postoperative care.
Main outcome measures: Concordance between nurse practitioner and ophthalmologist assessments; waiting times for first clinic appointment and surgery; visual acuity and degree of visual disability; patient satisfaction.
Results: 114 patients (61.6%) were assigned to see the ophthalmologist for cataract surgery. Median waiting times fell from 115 days (range, 23–268 days) to 21 days (range, 9–43 days) for initial clinic appointment, and from 44 days (range, 5–148 days) to 29 days (range, 14–154 days) for surgery. All 114 patients were listed for cataract surgery, and surgery had been performed on 121 eyes by the end of the study. After surgery, visual acuity improved by a mean of 0.45 logMAR (logarithm of the minimal angle of resolution) (SD, 0.24; range, 0.08–1.32). All patients had improved visual ability and high levels of satisfaction. Three quality assurance evaluations demonstrated full concordance between nurse and ophthalmologist assessments.
Conclusions: Implementing a nurse-led cataract assessment clinic improved access to care for public patients with cataracts. The safety and efficacy of the program and its excellent visual and patient-centred outcomes commend its adaptation and implementation to other ophthalmology departments.