Within certain guidelines, sport is beneficial for the young, the old, and those affected by cardiovascular disease

The roles of sport and physical activity in children, people with cardiac disease, and older people deserve special attention. Physical activity provides important benefits at both ends of the age spectrum. Further, increasing rates of childhood obesity, the ageing population, and the prevalence of cardiac disease in our community dictate the need for exercise guidelines for people in these groups. Here, we outline the benefits and risks of physical activity, and provide guidelines for prescribing exercise in these population subgroups.
Preventing obesity: There has been a marked decline in sports participation among Australian children since 1985, when 86% of children aged 5–14 years were active in sport. In 2003, these levels had fallen to 69% of boys and 54% of girls.1,2 During this same period there has also been an increase in the incidence of childhood overweight and obesity.
Obesity affects 19%–23% of Australian children and adolescents.3 Obesity in adolescence is associated with increased risk of mortality from all causes (independent of adult weight).4 To date, exercise interventions aimed at reducing childhood obesity have been disappointing. Preventing obesity through daily physical activity appears to be a more rewarding approach.
Bone mineral accrual: Recent research suggests that the greatest bone mineral accrual occurs when weight-bearing exercise is performed in the early pubertal years5 (evidence level II; based on the National Health and Medical Research Council system for assessing evidence6). Inactivity during these years may result in children failing to realise their potential for peak bone mass.
Lipid profile and insulin sensitivity: The incidence of type 2 diabetes in children and adolescents is increasing.7 Aerobic exercise improves insulin sensitivity in overweight children (evidence level II),8 and may produce beneficial changes in blood lipid profiles (increased level of high-density lipoprotein [HDL] and decreased level of low-density lipoprotein [LDL]) in children. Cross-sectional studies in young athletes show a positive correlation between aerobic fitness (VO2 peak) and HDL levels.9 With life expectancy potentially falling for the first time in many years because of the effect of the obesity epidemic on adult disease, measures need to be taken earlier to improve insulin sensitivity and blood-lipid profiles.10
Case study 1 — heel pain in an obese child
Provisional diagnosis: Sever disease (traction apophysitis of the calcaneum).
Management: There is a need to reduce pain, but not to recommend reduced activity, given his obesity. Therefore, the aim would be to reduce impact loading (modified training). It is usually not necessary to stop training altogether (evidence level IV).13 Swimming and cycling could be substituted for running sports.
Recommendations would include applying ice to the heel after exercise, wearing shoes which raise the heel (to unload apophysis), and beginning a calf-stretching program (evidence level IV),13 as well as giving advice about diet.
How much is too much? There are few sports with evidence-based guidelines on this issue. In baseball, however, it was observed that many promising pitchers in the junior baseball leagues were not progressing to senior ranks because of upper limb overuse injuries.11,12 As a result of these findings, there are now strict guidelines on how many balls it is safe to pitch at various ages. Unfortunately, guidelines for other children’s sports are based on “best practice” rather than scientific evidence. Improved injury surveillance in children’s sport will help in the development of such guidelines.
Fractures: Peak fracture risk in children coincides with the adolescent growth spurt in both sexes. This is thought to be the result of increased cortical bone turnover at this time of high calcium demand for longitudinal bone growth.14 While weight-bearing activity in childhood may be protective against fractures in adult life, participating in sports at higher levels is associated with increased risk of fracture in prepubertal children.15
a higher surface-area to body-mass ratio, so that children absorb more heat from the environment (and, conversely, experience greater heat loss in a cold environment);
lower exercise efficiency, producing more heat for a given work load;
a higher sweating threshold and lower sweat rate;
slowness to acclimatise; and
a tendency to dehydrate, requiring reminders to drink while exercising.
Implementation of injury prevention strategies requires injury surveillance data in children’s sport. One area where successful preventive strategies have been implemented as a result of injury data is in the sport of rugby union. Changes in the scrummaging rules were made in Under-19 rugby in response to a review of spinal cord injuries, which showed an increased number of paralysing injuries in Australian schoolboy rugby since the introduction of the power scrum.16
Weight training in children has always been a controversial topic. Its detractors say that it is injurious and does not produce strength improvements in the pre-adolescent child. However, studies now show that weight training can produce strength gains, even in prepubertal children, and that the injury risk is low when training is well supervised (evidence level III-2).17
Strength gains in prepubertal children are thought to be a result of neuromuscular adaptations in the absence of muscle hypertrophy. High-repetition (13–15 repetitions), moderate-resistance programs produce greater increases in strength than low-repetition (6–8 repetitions), high-resistance programs (evidence level III-2).18
Part of the controversy surrounding weight training in children stems from confusion as to the difference between weight training and weight lifting. Weight lifting is a competitive sport where maximal lifts are performed and is unsuitable for children before adolescence.19 Weight training (also called strength training or resistance training) involves repetitive submaximal muscle contractions with the aim of improving strength.
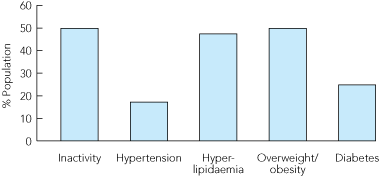
Primary prevention of cardiovascular disease: In 2001, physical inactivity was second only to tobacco smoking as a cause of total disability and death in Australia.20 Sedentary patients have a 1.5–2.0 times greater risk of cardiovascular events. Recent activity rather than being active earlier in life confers greater benefit.21 Box 1 illustrates the high prevalence of physical inactivity as a cardiovascular risk factor when compared with other well accepted risk factors.
Physical activity can provide benefits in a number of these risk factors:
Diabetes — exercise increases insulin sensitivity and reduces the incidence of type 2 diabetes.22
Obesity — activity has had a more significant impact in men than in women, and is generally more easily achieved in men; its effect is greater in overweight rather than in severely obese patients for whom mobility is difficult.
Lipids — activity lowers triglyceride levels, increases HDL levels and lowers total cholesterol levels.23
Hypertension — sustained exercise (of at least 50% of achievable activity) typically produces a 5–10 mm fall in both diastolic and systolic blood pressure, although it is less effective in those who are normotensive.
Secondary prevention of cardiovascular disease: While supervised cardiac rehabilitation programs have been shown to improve survival and well being after a cardiac event,24 there is evidence (level II) that continued exercise reduces mortality in patients after myocardial infarction.24
Habitual physical activity improves functional capacity and well being in patients with cardiovascular disease. Recent studies suggest that physical activity improves functional capacity and survival in patients with heart failure.25
Other benefits of physical activity: These include reduced risk of mortality from all causes, and improved quality of life after myocardial infarction (evidence level II).21,26 Physical activity may also reduce depression.27
Musculoskeletal injury: This is the most common adverse outcome associated with adults participating in exercise programs. Injuries occur in both men and women, affecting the lower limbs and, in particular, the knee. Sports participation is associated with a higher incidence of musculoskeletal injuries than involvement in a tailored exercise program (eg, walking, jogging).28
Sudden cardiac death or acute cardiac event: Although habitual physical activity reduces the risk of sudden cardiac death in the asymptomatic population, the increased risk of sudden death during an acute bout of physical activity is well documented.29
People with the following cardiovascular problems should be advised against exercising:
unstable angina;
dyspnoea or chest pain with low activity;
arrhythmia at rest;
uncontrolled hypertension;
severe aortic stenosis; or
uncontrolled heart failure.
Patients with established coronary artery disease should not undertake competitive sports unless they have normal left ventricular function and have received appropriate revascularisation therapy.30
Patients should be advised to stop exercising if they experience:
There are three identified levels of physical activity:
Low — no noticeable increase in breathing and heart rate with constant movement (eg, slow walking or playing bowls). One could easily whistle while undertaking a low-intensity activity.
Moderate — slight but noticeable increase in breathing and heart rate, and possible light sweating (eg, brisk walking or slow swimming). One would be able to talk during this activity, but not whistle.
Vigorous — hard breathing, such as puffing (eg, singles tennis or jogging) making it difficult to talk.
Acute cardiac disease: Following an acute myocardial infarction, a supervised cardiac rehabilitation program is recommended. There is good evidence (level II) that these supervised, exercise programs improve quality of life, reduce total cholesterol levels and reduce subsequent cardiac mortality.24
Case study 2 — angina on exertion
Regular physical activity alone could reduce his risk of death by 27%,25 and could increase his ischaemic threshold by improving his peripheral utilisation of oxygen, thus decreasing his cardiac exercise demand. However, there is no current evidence that activity changes the existing coronary artery disease.
Since the first epidemiological studies on the benefit of physical activity on cardiovascular disease, it has been well documented that physical inactivity is an important risk factor in population health.31 Further, it is estimated that as much as half of the functional decline associated with ageing is actually a result of disuse and, in the case of the decline in muscle function, is at least partially reversible by resistance training.32
the extent of any pre-existing medical condition;
the type of program provided; and
the frequency, duration and intensity of exercise (see previous section).
Masters’ competitors show great diversity across all social groups, medical status and history of sporting participation, with the rate of ageing shown to be a highly individual process.35,36
Exacerbation of cardiac ischaemia (either asymptomatic or diagnosed);
Cardiac arrhythmia, with sudden cardiac death (although the absolute risk of sudden cardiac death during any episode of vigorous exertion is extremely low29);
Dehydration and electrolyte imbalance (may be exacerbated by medications such as diuretics);
Deterioration of chronic medical condition, such as pulmonary and coronary artery disease, especially if associated with exposure to air pollution in urban environments;37 and
Musculoskeletal injury (this is the main medical cost of involvement in masters’ competitions38,39 — about one in 10 participants are injured to a degree sufficient for medical assessment; most injuries are acute and are associated with running and pivoting sports, most frequently involving the knee40).
Evidence-based advice
Regular exercise (40 minutes, 5 days a week) without dietary change will reduce body fat in children with obesity (evidence level II).8
A school-based exercise program will improve fasting insulin levels and reduce body fat in overweight children (evidence level II).8
Exercise interventions in early puberty appear to have the most beneficial effect on bone mineral accrual (evidence level II).5
Regular physical activity improves functional capacity and survival in patients with heart failure (evidence level I).22
A supervised cardiac rehabilitation program (following acute myocardial infarction, coronary artery bypass or angioplasty) improves functional capacity and reduces risk of subsequent cardiac events (evidence level I).20
Levels of evidence (I–IV) are derived from the National Health and Medical Research Council’s system for assessing evidence.6
Medical control of pre-existing health problems should be maximised, and older people should be aware of how their medications may affect their response to exercise. Medical assessment of cardiovascular risk factors before commencing an exercise program or sporting activity is advised.
There should be appropriate graduated progression of training before competition.
People need to monitor themselves and cease the activity if there are any associated symptoms such as excessive dyspnoea, palpitations, chest pain, syncope, or fatigue. Such symptoms need to be fully assessed before return to sport.
Older people should avoid training excesses, and allow adequate recovery. They should aim for 10%–15% increments in training load.
People need to allow adequate time for acclimatisation before competing in new environments.
2 Effects of ageing versus physical activity on major organ systems33,34
- 1. Pyke JE. The Australian health and fitness survey 1985: the fitness, health and physical performance of Australian school students aged 7–15 years. Adelaide: Australian Council for Health, Physical Education and Recreation, 1986.
- 2. Australian Bureau of Statistics. Children’s participation in cultural and leisure activities. Canberra: ABS, 2004. (Catalogue No. 4901.0.)
- 3. Booth ML, Wake M, Armstrong T, et al. The epidemiology of overweight and obesity among Australian children and adolescents, 1995-97. Aust N Z J Public Health 2001; 25: 162-169.
- 4. Must A, Jacques PF, Dallal GE, et al. Long-term morbidity and mortality of overweight adolescents. A follow-up of the Harvard Growth Study of 1922 to 1935. N Engl J Med 1992; 327: 1350-1355.
- 5. McKelvie KJ, McKay HA, Khan KM, et al. A school-based loading intervention augments bone mineral accrual in early pubertal girls. J Pediatr 2001; 139: 501-508.
- 6. National Health and Medical Research Council. How to use the evidence: assessment and application of scientific evidence. Handbook series on preparing clinical practice guidelines (Table 1.3: Designation of levels of evidence). Canberra: NHMRC, February 2000: 8.
- 7. Pinhas-Hamiel O, Dolan LM, Daniels SR, et al. Increased incidence of non-insulin-dependent diabetes mellitus among adolescents. J Pediatr 1996; 128: 608-615.
- 8. Carrel AL, Clark RR, Peterson SE, et al. Improvement of fitness, body composition, and insulin sensitivity in overweight children in a school-based exercise program: a randomized controlled study. Arch Pediatr Adolesc Med 2005; 159: 963-968.
- 9. Eisenmann JC, Womack CJ, Reeves MJ, et al. Blood lipids of young distance runners: distribution and inter-relationships among training volume, peak oxygen consumption, and body fatness. Eur J Appl Physiol 2001; 85: 104-112.
- 10. Olshansky SJ, Passaro DJ, Hershow RC, et al. A potential decline in life expectancy in the United States in the 21st century. N Engl J Med 2005; 352: 1138-1145.
- 11. Lyman S, Fleisig GS, Waterbor JW, et al. Longitudinal study of elbow and shoulder pain in youth baseball pitchers. Med Sci Sports Exerc 2001; 33: 1803-1810.
- 12. Lyman S, Fleisig GS, Andrews JR, Osinski ED. Effect of pitch type, pitch count, and pitching mechanics on risk of elbow and shoulder pain in youth baseball pitchers. Am J Sports Med 2002; 30: 463-468.
- 13. Hendrix CL. Calcaneal apophysitis. Clin Podiatr Med Surg 2005; 22: 55-62.
- 14. Bailey DA, Wedge JH, McCulloch RG, et al. Epidemiology of fractures of the distal end of the radius in children as associated with growth. J Bone Joint Surg Am 1989; 71: 1225-1231.
- 15. Ma DQ, Jones G. Clinical risk factors but not bone density are associated with prevalent fractures in prepubertal children. J Paediatr Child Health 2002; 38: 497-500.
- 16. Taylor TK, Coolican MR. Spinal-cord injuries in Australian footballers, 1960–1985. Med J Aust 1987; 147: 112-118.
- 17. Rians CB, Weltman A, Cahill BR, et al. Strength training for prepubescent males: is it safe? Am J Sports Med 1987; 15: 483-489.
- 18. Faigenbaum AD, Westcott WL, Loud RL, Long C. The effects of different resistance training protocols on muscular strength and endurance development in children. Pediatrics 1999; 104: e5.
- 19. Bernhardt DT, Gomez J, Johnson MD, et al. Committee on Sports Medicine and Fitness. Strength training by children and adolescents. Pediatrics 2001; 107: 1470-1472.
- 20. Australian Institute of Health and Welfare. Heart, stroke and vascular diseases — Australian facts 2004. Canberra, AIHW, National Heart Foundation of Australia and National Stroke Foundation of Australia, 2004: 71-73.
- 21. Thompson PD, Buchner D, Pina IL, et al. Exercise and physical activity in the prevention and treatment of atherosclerotic cardiovascular disease: a statement from the Council on Clinical Cardiology (Subcommittee on Exercise, Rehabilitation, and Prevention) and the Council on Nutrition, Physical Activity, and Metabolism (Subcommittee on Physical Activity). Circulation 2003; 107: 3109-3016.
- 22. Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 2002; 346: 393-403.
- 23. Leon AS, Sanchez OA. Response of blood lipids to exercise training alone or combined with dietary intervention. Med Sci Sports Exerc 2001; 33 (6 Suppl): S502-S515.
- 24. Jolliffe J, Rees K, Taylor RF, et al. Exercise-based rehabilitation for coronary heart disease. Cochrane Database Syst Rev 2001; (1): CD001800.
- 25. Piepoli MF. Davos C Francis DP. Coats AJ. ExTraMATCH Collaborative. Exercise training meta-analysis of trials in patients with chronic heart failure (ExTraMATCH). BMJ 2004; 328: 189.
- 26. Oldridge N, Guyatt G, Jones N, et al. Effects on quality of life with comprehensive rehabilitation after acute myocardial infarction. Am J Cardiol 1991; 67: 1084-1089.
- 27. Blumenthal JA, Babyak MA, Carney RM, et al. Exercise, depression, and mortality after myocardial infarction in the ENRICHD Trial. Med Sci Sports Exerc 2004; 36: 746-755.
- 28. Hootman J, Macera C, Ainsworth BE, et al. Epidemiology of musculoskeletal injuries among sedentary and physically active adults. Med Sci Sports Exerc 2002; 34: 838-844.
- 29. Albert CM, Mittleman MA, Chae CU, et al. Triggering of sudden death from cardiac causes by vigorous exertion. N Engl J Med 2000; 343: 1355-1361.
- 30. Briffa TG, Maiorana A, Sheerin NJ, et al. Physical activity for people with cardiovascular disease: recommendations of the National Heart Foundation of Australia. Med J Aust 2006; 184: 71-75. <MJA full text>
- 31. Paffenbarger RS Jr, Wing AL, Hyde RT. Physical activity as an index of heart attack risk in college alumni. Am J Epidemiol 1978; 108; 161-175.
- 32. Fiatarone MA, Evans WJ. The etiology and reversibility of muscle dysfunction in the aged. J Gerontol 1993; 48: 77-83.
- 33. Kavanagh T, Shephard RJ. Can regular sports participation stop the aging problem? Physician Sports Med 1990; 18; 94-104.
- 34. Kirkendall DT, Garrett WE. The effects of aging and training on skeletal muscle. Am J Sports Med 1998; 26; 598-602.
- 35. Moss N. The psychology of the ageing athlete. Clin Sports Med 1991; 10; 431-444.
- 36. Menard D, Stanish WD. The aging athlete. Am J Sports Med 1989; 17; 187-196.
- 37. Sharman JE. Clinicians prescribing exercise: is air pollution a hazard? [editorial]. Med J Aust 2005; 182: 606-607. <MJA full text>
- 38. Buckwalter JA, Lane NE. Athletics and osteoarthritis. Am J Sports Med 1997; 25; 873-881.
- 39. DeHaven KE, Lintner DM. Athletic injuries: comparison by age, sport and gender. Am J Sports Med 1986; 14; 218-224.
- 40. Matheson GO, MacIntyre JG, Taunton JE, et al. Musculoskeletal injuries associated with physical activity in older adults. Med Sci Sports Exerc 1989; 21: 379-385.





Abstract
Sports participation among children is declining.
Sport and physical activity are important in childhood for optimising bone mass and reducing obesity and insulin resistance.
Physical activity reduces cardiovascular risk factors in adults, and can improve survival in patients with cardiac failure.
Musculoskeletal injury is the most common complication of sports participation in adults — not cardiac events.
Some of the decline in function which occurs with ageing can be positively affected by regular physical activity.