New research has changed our perception and management of common injuries
In the past, hip joint abnormality was attributed solely to osteoarthritis, but magnetic resonance imaging (MRI) and hip arthroscopy have shown that labral injuries, chondral injuries, rim lesions, synovitis and tears of the ligament teres are common causes of hip, groin and low-back pain. Tears of the acetabular labrum (Box 1) occur as a result of trauma, and more commonly in patients with dysplasia, pelvic instability and degeneration.1 Loading of the hip in hyperextension and external rotation is the mechanism most commonly associated with tearing of the anterior acetabular labrum. Dance, golf, hockey and soccer are associated with a higher incidence of hip injuries.2
The history of a patient with a labral tear ranges from a traumatic event to insidious onset. In more than half of injuries, the patient cannot recall a specific incident.2 Falls and twisting injuries are commonly reported, but other mechanisms include running, direct blows and high-energy trauma sustained from motor vehicle accidents or falls from heights.2 The lumbar spine and groin are the most common sites of pain in patients aged 16–56 years with hip disorder. Commonly, the presentation is subtle, characterised by dull, activity-induced or positional pain that typically fails to improve with time.1 The patient may complain of a catching pain or clicking sensation. Examination findings include a limp, an audible or palpable click during passive flexion-extension, and pain on passive flexion and internal rotation of the hip.
X-ray, arthrography and conventional MRI have all been found to be inadequate in diagnosis.3-5 In the last decade, gadolinium-enhanced magnetic resonance arthrography has been widely used to detect labral abnormalities, although more recent studies 6,7 have suggested that the sensitivity of this procedure may be somewhat less than first reported.3,8 More recently, fast spin-echo proton-density weighted MRI sequences taken in the plane of the hip joint have been shown to be more accurate.9
Intra-articular injection of local anaesthetic combined with examination of the hip before and after injection can be useful in determining the hip as the source of pain.6
Hip arthroscopy is both a diagnostic (gold standard) and therapeutic tool, although it is technically more difficult than arthroscopy of other joints. Distraction of the hip of about 10–15 mm is required to access the hip joint, and most complications, such as neuropraxias, are caused by traction.
In a number of case series, arthroscopy has been shown to be of benefit in recent traumatic labral injury,10-12 but gives disappointing results in chronic hip pain, which is probably associated with degenerative change, and chondral lesions of the acetabulum.13
Overuse knee injuries are the most common musculoskeletal conditions presenting to general and sports medical practices.14-16 Overuse knee pain is usually anterior, inferior or retropatellar, and the most common condition responsible for this pain is patellofemoral pain (PFP).
In PFP, the pain may be localised, but is most likely to be generalised around the patella, and non-specific. It may be precipitated by an increase in the frequency or intensity of repetitive loaded activities (eg, running, walking up and down hills or stairs, squatting). Tenderness is usually localised to the retropatellar area and pain reproduced on step-up, step-down or squat.
Researchers have identified that individuals with PFP have a delayed onset in the activity of the vastus medialis obliquus (VMO) muscle, relative to the lateral quadriceps muscle (vastus lateralis).17,18
Patellofemoral pain is not a self-limiting condition, and physiotherapy generally includes several components: retraining the VMO component, stretching, mobilisation, massage, general conditioning, taping/bracing, foot orthoses, balance training, and hip muscle training. This approach, with its emphasis on training the VMO in a weightbearing position in conjunction with taping of the patella (Box 2), and first described by Australian physiotherapist Jenny McConnell,19 has gained widespread acceptance in Australia and increasingly internationally.
Five systematic reviews of randomised controlled trials, three of which were methodologically sound, have found this multimodal physiotherapy program to be of benefit in relieving anterior knee pain.20-24 In another randomised controlled trial, a multimodal intervention resulted in an earlier onset of VMO (relative to the vastus lateralis) and improved knee flexion during stair ambulation.25-27
Patients with PFP often exhibit reduced core stability (strength and control of the lumbo–pelvic–hip region), which may increase the load on the patellofemoral joint through increased femoral internal rotation and knee valgus. This is often assessed in the clinic using the “step-down or single-leg squat test” (Box 3). The limited research in this area suggests that hip muscle strength is reduced in PFP,28 and most multimodal interventions include a component of hip strengthening and control exercises.
Anterior cruciate ligament (ACL) injuries are a matter of serious concern for sportspeople in terms of treatment costs, time lost from sport and the increased risk of subsequent osteoarthritis. These injuries are most commonly seen in sports that involve sudden changes of direction, such as football, netball, basketball and skiing. Most are non-contact injuries, and occur either during a cutting manoeuvre or on landing from a jump. Landing on a straight leg is a high risk situation, and occurs frequently in netball and football.
The causes of ACL injury have been extensively studied. In AFL football, ground hardness, grass type (couch) and boot studs have been shown to be associated with ACL injury. Efforts to rectify this include watering grounds, avoiding couch grass and having less foot fixation.29 It is too early to assess their effectiveness.
Women are about three times more likely than men to have ACL injury, possibly because of factors including the effect of differences in hormone levels on ligament strength and stiffness, neuromuscular control, lower limb biomechanics, ligament strength and fatigue.30,31 Differences in neuromuscular control, especially in reduced activation of hamstring muscles32,33 and landing from a jump with less hip and knee flexion than men,32 have been shown to be important factors in the differences between the sexes.
Given the apparent importance of neuromuscular factors in the aetiology of ACL injuries, particularly in women, programs to improve neuromuscular control have been implemented. They aim to improve awareness and knee control during standing, cutting, jumping and landing.34 They have focused on proprioceptive balance-board exercises,35 plyometric training,36 avoidance of high risk behaviour and positioning,37 landing techniques38 or a combination of these.34,38,39 A number of these studies have shown a reduction in ACL injuries of up to 89%.
An ACL-deficient knee is not compatible with moderate-to-high-level sporting activity, especially in sports that involve sudden changes of direction. Arthroscopic-assisted reconstruction of the anterior cruciate ligament after rupture is a common procedure performed by sports orthopaedic surgeons in Australia. Current topics of debate include choice of graft, graft positioning, graft fixation and postoperative rehabilitation. Available ACL grafts include hamstring tendons (semitendinosis and gracilis), patellar tendon, quadriceps tendon, allograft and synthetics. Hamstring and patellar tendon grafts are by far the most common grafts used, and there appears to be no difference in outcomes.40,41 An excellent Australian study comparing the two techniques showed little or no difference in terms of functional outcome, despite greater laxity measurements in patients in the hamstring tendon group. The principal differences between the two graft types in this study, as in others, were increased pain on kneeling and increased extension deficits in patients in the patellar tendon group.42 Allografts appear to be as effective as autografts,43 but problems with availability and cost, as well as theoretical concerns about disease transmission, make this a less popular choice of graft. Synthetic ligaments have been shown to be unsuccessful in the long term.44,45
Any treatment of articular cartilage injuries must both relieve symptoms and prevent osteoarthritis. This requires reconstitution of hyaline cartilage with its complex layered architecture. Current surgical methods for treating chondral defects include microfracture, osteochondral autograft and autologous chondrocyte implantation.
Microfracture (mesenchymal stem cell stimulation): 1 mm holes are punched into exposed subchondral bone, gaining access to the underlying marrow. Pluripotential stem cells then form a “superclot” and differentiate into fibrous and chondral-like cells. This will result in formation of type 1 collagen with characteristics akin to hyaline cartilage. Advantages include the ability to perform this as an arthroscopic rather than open procedure, rapid rehabilitation and low cost. The main disadvantage is the inferior performance of type I collagen over 2 years.46-48
Autologous chondrocyte implantation (ACI): Autologous chondrocytes are harvested from an area of healthy cartilage and cultured with the use of growth factors to promote chondrocyte growth and differentiation; they are then reimplanted to the chondral defect and held in place beneath a periosteal patch to synthesise and maintain normal chondral matrix. The advantage is the higher degree of hyaline-like (rather than fibrous) cartilage, with possible long-term prevention of osteoarthritis. Disadvantages include high cost, the open procedure involved (with higher morbidity), technically difficult surgery and availability.49 A recent systematic review concluded that the completed clinical trials did not yield any evidence that ACI was superior to other therapeutic alternatives, although the follow-up periods were very short.50
Currently, tissue engineering techniques are being investigated in a number of areas in orthopaedics. Chondral regeneration and osteoarthritis, meniscal regeneration, fracture non-union, prosthetic bioimplantation and ACL reconstruction create the most interest. Most research is directed towards achieving the “holy grail” of a single arthroscopic procedure that reproduces hyaline cartilage with an intact layered architecture.
The mainstream popularity of orthoses was tied to the running boom in the United States in the late 1970s and early 1980s, and the explosion of overuse injuries, attributed to inadequate footwear, or, the new catch phrase, “faulty biomechanics”. However, many of the studies linking foot mechanics directly to musculoskeletal pain are based on conjecture, expert opinion, or case series.51 Although orthotic therapy is reported as successful, such reports are often based on subjective or empirical data,52 and are surprising, given the variability in properties and placement of the orthotic inserts used.
While the mode of action of orthotic therapy is not fully understood, it should not be discounted. By far the most credible theory for orthotic function today is that orthoses provide altered sensorimotor or proprioceptive feedback to the brain, which then produces protective reactions through muscular and neurological responses.53,54 This may explain why the success of orthotic therapy is very operator dependent, so that physicians should refer to podiatrists who are knowledgeable, ethical, and not locked into “standard” orthotic treatment protocols for complex problems.
Evidence-based guidelines*
Arthroscopy is an effective treatment for recent traumatic labral injury (evidence level IV).10-12
Multimodal physiotherapy interventions are effective in the treatment of patellofemoral pain (evidence level I).55-58
Neuromuscular training decreases the incidence of ACL injuries in females (evidence level III).59
Hamstring and patellar tendon grafts are by far the most common grafts used, and there appears to be no difference in outcomes (evidence level III-1).40
Autologous chondrocyte implantation must currently be considered as a technology under investigation whose effectiveness is yet to be determined in well designed and conducted clinical trials (evidence level I).60
Evidence according to National Health and Medical Research Council levels of evidence.60
Research in sport biomechanics may take the form of analysing movement to do such things as:
Identify critical variables for successfully performing a skill, such as the tennis serve, baseball pitch or field hockey flick;
Identify the source of joint power in an Australian Rules kick for greater distance;
Identify the cause of back injuries in cricket, or shoulder injuries in throwing or hitting sports;
Quantify the loading at the knee during side-stepping in football codes;
Evaluate the benefits of sand-walking for stability, particularly in the elderly.
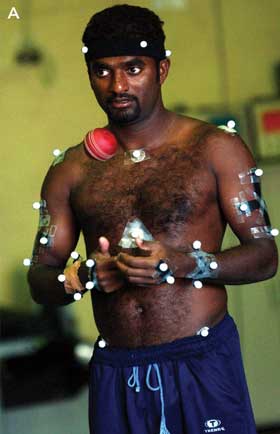
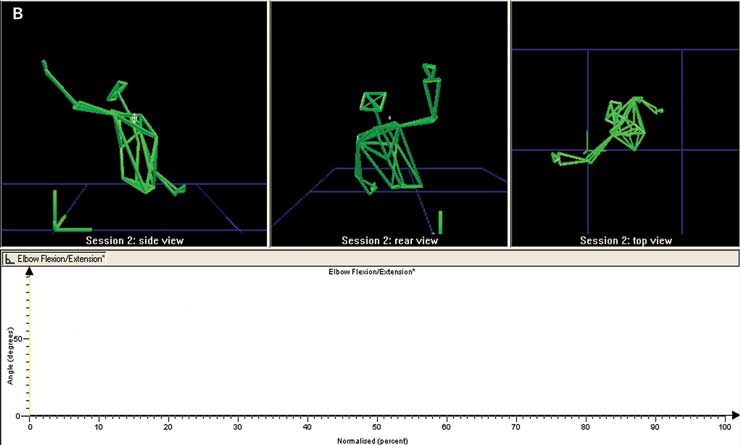
The sport biomechanist has also become embroiled in the technological advances of sports like cricket, where a bowler’s action may now be placed under the scientific microscope (Box 4). This research has been aided by advances such as the optoreflective motion analysis system (replacing the high speed camera) and computers and models with ever more storage and processing speed. Optoreflective analysis can record movement to within 1°, compared with high speed video systems with error levels of more than 3°.
Motion analysis systems include a wide range of camera and software alternatives that capture and track marker movement, create an anatomically-based image, then determine, for example, the angles, velocities, moments and powers for the movement analysed.
These data may then be linked with data from other exercise scientists, sport physicians and physiotherapists for research or therapeutic purposes. A team approach to research is essential if performance is to be optimised while keeping athletes relatively free of injury.
This is an exciting time in sports medicine. We are moving swiftly towards evidence-based medicine, and away from the somewhat empirical basis of the past, while innovations such as tissue engineering and gene therapy are evolving as exciting therapies of the future.
1 Tear of the acetabular labrum
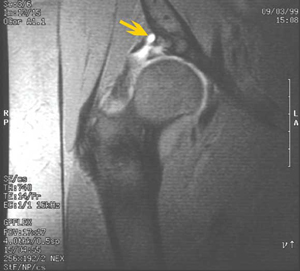
T2 fat-saturated magnetic resonance image showing labral tear (lower white area) and paralabral cyst (arrow).
2 Taping of the patella in the McConnell program
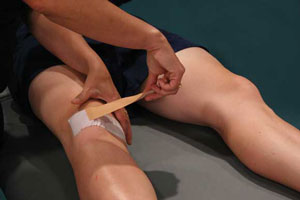
Taping to displace the patella medially. Tape is applied to the lateral aspect of the patella, pulled medially and attached to the medial knee soft tissues. Skin and subcutaneous tissues should be creased, indicating that sufficient medial force has been applied. If successful, the tape should immediately reduce the patient’s pain during aggravating activity by at least 50%.
Case study — knee pain aggravated by activity in a young woman
A 22-year-old woman presents with a 4-year history of anterior knee pain aggravated by running and aerobics. The day after participating in these activities, she describes difficulty with stair ambulation and even with sitting for extended periods (eg, driving the car or at the desk at work). She has had no previous trauma or knee surgery, no referred pain or difficulties with sites proximal or distal to the knee.
On examination, she had tenderness on palpation of the medial and lateral patellar facets. All other knee examination findings were normal. She had generalised quadriceps muscle weakness, more pronounced in the medial component (vastus medialis obliquus [VMO]). Her calf muscles also appeared to be weak.
She appeared to walk with a large amount of femoral internal rotation. This was accompanied by pelvic rotation and tilt. Her knee excursion seemed limited, especially during early stance in the walk cycle. Her foot was somewhat pronated and appeared to be quite unstable through her midfoot during stance. This was associated with a valgus knee motion.
A one-leg squat test reproduced her pain and showed reduced stability on the weight-bearing leg, with an increase in pelvic tilt, femoral internal rotation and knee valgus.
Her plain radiographs were unremarkable, although the femoral trochlea may be a little shallow.
Based on her history and examination, she appeared to have patellofemoral pain resulting from her loaded weight-bearing activities (running and aerobics).
She required a treatment regimen that would:
reduce pain (avoid aggravating activity, tape, mobilisation, massage, bracing, electrotherapy);
improve the coordination and then strength of her quadriceps (especially the VMO), calf and hip muscles (extensors, abductors and external rotators); and
change the loading profile of the patellofemoral joint through gait re-education and a graduated loading program (which would allow for return to running and aerobics).
After 3 weeks of treatment, she had no peripatellar tenderness and could perform a one-leg squat without pain. She then began a graduated running program, returning to her previous level of activity after 3 weeks of gradual increase in running speed and distance.
If a trial of conservative management had not been successful, then the effectiveness of the interventions would have to be assessed. She may require biofeedback (usually surface electromyography) to allow her to fully activate the VMO, and possible gait retraining. The effectiveness (ie, pain reduction) with the tape and/or brace may need revision. Imaging may assist with assessment of the bony alignments and/or bone, cartilage or soft tissue status.
3 Patient performing the single-leg squat

During a single-leg squat or a step-down test, patients are asked to squat down slowly on one leg, as far as they can without losing their balance. The practitioner looks for signs of reduced core stability: lateral trunk tilt/rotation; pelvis tilt/rotation; knee valgus; or reduced balance.
- Peter D Brukner1
- Kay M Crossley2
- Hayden Morris3
- Simon J Bartold4
- Bruce Elliott5
- 1 Centre for Health, Exercise and Sports Medicine, University of Melbourne, Melbourne, VIC.
- 2 Simon Bartold Podiatry, Marryatville, SA.
- 3 School of Human Movement and Exercise Science, University of Western Australia, Perth, WA.
None identified.
- 1. Mason JB. Acetabular labral tears in the athlete. Clin Sports Med 2001; 20: 779-790.
- 2. Huffman GR, Safran M. Tears of the acetabular labrum in athletes: diagnosis and treatment. Sports Med Arth Rev 2002; 10: 141-150.
- 3. Czerny C, Hofmann S, Neuhold A, et al. Lesions of the acetabular labrum: accuracy of MR imaging and MR arthrography in detection and staging. Radiology 1996; 200: 225-230.
- 4. Erb RE. Current concepts in imaging the adult hip. Clin Sports Med 2001; 20: 661-696.
- 5. Santori N, Willar RN. Acetabular labral tears: result of arthroscopic partial limbectomy. Arthroscopy 2000; 16: 11-15.
- 6. Mitchell B, McCrory P, Brukner P, et al. Hip joint pathology: clinical presentation and correlation between magnetic resonance arthrography, ultrasound, and arthroscopic findings in 25 consecutive cases. Clin J Sports Med 2003; 13: 152-156.
- 7. Plotz GM, Brossman J, Schunke M, et al. Magnetic resonance arthrography of the acetabular labrum. Macroscopic and histological correlation in 20 cadavers. J Bone Joint Surg Br 2000; 82-B: 426-432.
- 8. Petersilge CA, Haque MA, Petersilge WJ, et al. Acetabular labral tears: evaluation with MR arthrography. Radiology 1996; 200: 231-235.
- 9. Mitchell B, Lee B, Brukner PD, et al. Correlation of hip arthroscopy findings and diferent MRI techniques. A review of 99 cases. J Sci Med Sport 2003; 6 (4 Suppl): 48.
- 10. Byrd JWT, Jones KS. Prospective analysis of hip arthroscopy with 2-year follow-up. Arthroscopy 2000; 16: 578-587.
- 11. Dorfmann H, Boyer T. Arthroscopy of the hip: 12 years of experience. Arthroscopy 1999; 15: 67-72.
- 12. O’Leary JA, Berend K, Vail TP. The relationship between diagnosis and outcome in arthroscopy of the hip. Arthroscopy 2001; 17: 181-188.
- 13. McCarthy JC, Busconi B. The role of hip arthroscopy in the diagnosis and treatment of hip disease. Can J Surg 1995; 38 Suppl 1: S13-S17.
- 14. Baquie P, Brukner P. Injuries presenting to an Australian sports medicine centre: a 12-month study. Clin J Sport Med 1997; 7: 28-31.
- 15. Devereaux MD, Parr GR, Lachman SM, et al. The diagnosis of the stress fractures in athletes. JAMA 1984; 252: 531-533.
- 16. Kannus P, Aho H, Jarvinen M, et al. Computerized recording of visits to an outpatient sports clinic. Am J Sports Med 1987; 15: 79-85.
- 17. Cowan SM, Bennell KL, Hodges PW. Therapeutic patellar taping changes the timing of vasti muscle activation in people with patellofemoral pain syndrome. Clin J Sports Med 2002; 12: 339-347.
- 18. Cowan SM, Bennell KL, Hodges PW, et al. Delayed onset of electromyographic activity of vastus medialis obliquus relative to vastus lateralis in subjects with patellofemoral pain syndrome. Arch Phys Med Rehab 2001; 83: 989-995.
- 19. McConnell J. Management of patellofemoral problems. Man Ther 1996; 1: 60-66.
- 20. Clark DI, Downing N, Mitchell J, et al. Physiotherapy for anterior knee pain: a randomised controlled trial. Ann Rheum Dis 2000; 59: 700-704.
- 21. Crossley K, Bennell K, Green S, et al. Physical therapy for patellofemoral pain. A randomised, double-blinded, placebo controlled study. Am J Sports Med 2002; 30: 857-865.
- 22. Eburne J, Bannister G. The McConnell regimen versus isometric quadriceps exercises in the management of anterior knee pain. Knee 1996; 3: 151-153.
- 23. Harrison EL, Sheppard MS, McQuarrie AM. A randomized controlled trial of physical therapy treatment programs in patellofemoral pain syndrome. Physio Can 1999; Spring: 93-106.
- 24. Whittingham M, Palmer S, Macmillan F. Effects of taping on pain and function in patellofemoral pain syndrome: a randomized controlled trial. J Orthop Sports Phys Ther 2004; 34: 504-510.
- 25. Cowan SM, Bennell KL, Crossley KM, et al. Physical therapy alters recruitment of the vasti in patellofemoral pain syndrome. Med Sci Sports Exerc 2003; 34: 1879-1885.
- 26. Cowan SM, Bennell KL, Hodges PW, et al. Simultaneous feedforward recruitment of the vastii in untrained postural tasks can be restored by specific training. J Orth Res 2003; 21: 553-558.
- 27. Crossley KM, Cowan SM, McConnell J, et al. Physical therapy improves knee flexion during stair ambulation in patellofemoral pain. Med Sci Sports Exerc 2005; 37: 176-183.
- 28. Ireland ML, Wilson JD, Ballantyne BT, et al. Hip strength in females with and without patellofemoral pain. J Orth Sports Phys Ther 2003; 33: 671-676.
- 29. Orchard J. Is there a relationship between ground and climatic conditions and injuries in football? Sports Med 2002; 32: 419-432.
- 30. Ireland ML. The female ACL: why is it more prone to injury? J Orth Sports Phys Ther 2001; 31: 655-660.
- 31. Wedderkopp N, Kaltoft M, Lundgaard B, et al. Prevention of injuries in young female players in European team handball. A prospective intervention study. Scand J Med Sci Sports 1999; 9: 41-47.
- 32. Griffin LY. Non contact ACL injuries: is prevention possible? Hormonal and neuromuscluar factors may explain prevalence in women. J Musculoskeletal Med 2001; 18: 507-516.
- 33. Huston LJ, Wojtys E. Neuromuscular performance characteristics in elite female athletes. Am J Sports Med 1996; 24: 427-436.
- 34. Myklebust G, Engebretsen L, Braekken IH, et al. Prevention of anterior cruciate ligament injuries in female team handball players: a prospective intervention study over three seasons. Clin J Sport Med 2003; 13: 71-78.
- 35. Caraffa A, Cerulli G, Projetti M, et al. Prevention of anterior cruciate ligament injuries in soccer. A soccer prospective controlled study of proprioceptive training. Knee Surg Sports Traumatol Arthrosc 1996; 4: 19-21.
- 36. Hewett TE, Stroup AL, Nance TA, et al. Plyometric training in female athletes. Decreased impact forces and increased hamstring torques. Am J Sports Med 1996; 24: 765-773.
- 37. Ettlinger CF, Johnson RJ, Shealy JE. A method to help reduce the risk of serious knee sprains incurred in alpine skiing. Am J Sports Med 1995; 23: 531-537.
- 38. Hewett TE, Lindenfield TN, Riccobene JV, et al. The effect of neuromuscular training on the incidence of knee injury in female athletes. A prospective study. Am J Sports Med 1999; 27: 699-706.
- 39. Mandelbaum BR, Silvers HJ, Watanabe DS, et al. Effectiveness of a neuromuscular and proprioceptive training program in preventing anterior cruciate ligament injuries in female athletes: 2-year follow-up. Am J Sports Med 2005; 33: 1003-1010.
- 40. Yunes M, Richmond JC, Engels EA, et al. Patellar versus hamstring tendons in anterior cruciate ligament reconstruction: a meta-analysis. Arthroscopy 2001; 17: 248-257.
- 41. Spindler KP, Kuhn JE, Freedman KB, et al. Anterior cruciate ligament reconstruction autograft choice: bone-tendon-bone versus hamstring: does it really matter? A systematic review. Am J Sports Med 2004; 32: 1986-1995.
- 42. Feller JA, Webster KE. A randomised comparison of patellar tendon and hamstring tendon anterior cruciate ligament reconstruction. Am J Sports Med 2003; 31: 564-573.
- 43. Poehling GG, Curl WW, Lee CA, et al. Analysis of outcomes of anterior cruciate ligament repair with 5-year follow-up: allograft versus autograft. Arthroscopy 2005; 21: 774-785.
- 44. Bartlett RJ, Clatworthy MG, Nguyen TNV. Graft selection in reconstruction of the anterior cruciate ligament. J Bone Joint Surg Br 2001; 83: 625-634.
- 45. Pinczewski LA, Deehan DJ, Salmon LJ, et al. A five-year comparison of patellar tendon versus four-strand hamstring tendon autograft for arthroscopic reconstruction of the anterior cruciate ligament. Am J Sports Med 2002; 30: 523-536.
- 46. Miller BS, Steadman JR, Briggs KK, et al. Patient satisfaction and outcome after microfracture of the degenerative knee. J Knee Surg 2004; 17: 13-17.
- 47. Steadman JR, Briggs KK, Rodrigo JJ, et al. Outcomes of microfracture for traumatic chondral defects of the knee: average 11-year follow-up. Arthroscopy 2003; 19: 477-484.
- 48. Steadman JR, Miller BS, Karas SG, et al. The microfracture technique in the treatment of full-thickness chondral lesions of the knee in national football league players. J Knee Surg 2003; 16: 83-86.
- 49. Brittberg M, Tallheden T, Sjogren-Jansson B, et al. Autologous chondrocytes used for articular cartilage repair: an update. Clin Orthop Relat Res 2001; 391 Suppl: S337-S348.
- 50. Ruano-Ravina A, Jato Diaz M. Autologous chondrocyte implantation: a systematic review. Osteoarth Cart 2006; 14: 47-51.
- 51. van Mechelen W. Running injuries. A review of the epidemiological literature. Sports Med 1992; 14: 320-335.
- 52. Callaghan MJ, Baltzopoulos V. Anterior knee pain: the need for objective measurement. Clin Biomech 1992; 7: 67-74.
- 53. Nigg B. The role of impact forces and foot pronation: a new paradigm. Clin J Sports Med 2001; 11: 2-9.
- 54. Stacoff A, Reinschmidt C, Nigg BM, et al. Effects of foot orthoses on skeletal motion during running. Clin Biomech 2000; 15: 2054-2064.
- 55. Bizzini M, Childs JD, Piva SR, et al. Systematic review of the quality of randomised controlled trials for patellofemoral syndrome. J Orthop Sports Phys Ther 2003; 33: 4-20.
- 56. Bolga L, Malone T. Exercise prescription and patellofemoral pain: evidence for rehabilitation. J Sports Rehab 2005; 14: 72-88.
- 57. Crossley K, Bennell K, Green S, et al. A systematic review of physical interventions for patellofemoral pain syndrome. Clin J Sport Med 2001; 11: 103-110.
- 58. Heintjes E, Berger MY, Bierma-Zeinstra SMA, et al. Exercise therapy for patellofemoral pain syndrome. Cochrane Database Syst Rev 2003; (4): CD003472.
- 59. Hewett TE, Myer TD, Ford KR. Reducing knee and anterior cruciate ligament injuries among female athletes: a systematic review of neuromuscular training intereventions. J Knee Surg 2005; 18: 82-88.
- 60. National Health and Medical Research Council. A guide to the development, implementation and evaluation of clinical practice guidelines. Canberra: NHMRC, 1999.





Abstract
Magnetic resonance imaging and arthroscopy of the hip have shown that labral injuries, chondral injuries, rim lesions, synovitis and tears of the ligament teres are common causes of hip, groin and low-back pain.
Hip arthroscopy is used both as a diagnostic and therapeutic tool; it has been shown to be of benefit in recent traumatic labral injury, but disappointing in the management of chronic hip pain (which may be associated with degenerative change, and chondral lesions of the acetabulum).
The McConnell multimodal physiotherapy regimen is effective in treating patellofemoral pain.
Anterior cruciate ligament rupture is three to five times more common in women, but neuromuscular training appears to decrease its incidence.
Patellar tendon and hamstring grafts appear to be equally effective in anterior cruciate ligament reconstruction.
Articular cartilage defects remain a significant problem, and the efficacy of treatments such as autologous chondrocyte implantation is still unclear.