Summary measures of population health can be used to assess and compare levels of health; to identify the diseases, injuries and risk factors contributing most to ill health; and to evaluate the health gains from interventions.1 Life expectancy at birth is a useful summary measure for the mortality patterns of populations. In the 20 years between 1983 and 2003, Australians experienced a marked increase in life expectancy at birth, rising from 72 to 78 years in men and from 79 to 83 years in women.2 However, over a similar period, the life expectancy at birth of Australia’s Indigenous population was up to 20 years lower than that of the general Australian population.3,4
In the Northern Territory between 1981 and 2000, age-standardised mortality rates for Indigenous people were two to three times higher than those for non-Indigenous people. In some age groups, particularly between 40 and 50 years, mortality rates of Indigenous people were up to nine times higher, signifying extensive premature mortality among middle-aged Indigenous people.3
Since the late 1970s, demographers have developed a decomposition technique to assess the factors contributing to differences in life expectancy.5,6 The technique has been used to describe the contribution of causes of death to the change in life expectancy in Australia between 1971 and 1981,7 and the contribution of the reduction in major cardiovascular diseases, malignant neoplasms, injuries and AIDS-related mortality to the gains in life expectancy in 1985–1994.8
More recently, Vaupel and Romo have summarised the decomposition method for life expectancy.9 To our knowledge the contribution of specific causes of death to differences in life expectancy between the Indigenous and non-Indigenous population in Australia has not previously been examined.
The period studied was the 20 years from 1 January 1981 to 31 December 2000 inclusive. NT unit record death data were extracted for causes of death by sex, age and Indigenous status on the basis of date of death and state of residence, from the Australian Bureau of Statistics (ABS) mortality dataset. The underlying causes of death were coded by the ABS using the International classification of diseases, 9th and 10th revisions (ICD-9 and ICD-10). It has been shown previously that the overall quality of the medical cause of death data was of a sufficiently good standard from a public health perspective to broadly inform health policy.10 In the NT, considerable effort has been made to validate and identify Indigenous status in historical death data by using commonly used Indigenous community and family names,11 and completeness of Indigenous death identification data was considered acceptable for trend analysis.3,12 Under-identification of Indigenous status for the NT is reported as being the lowest in Australia, and coverage of Indigenous deaths the highest.13,14 Constant annual death counts suggest that coverage has remained relatively stable in the NT.14
Population data comprising yearly estimated resident population counts for the NT by sex, Indigenous status and 5-year age group were obtained from the ABS. Annual Indigenous population counts were derived using ABS experimental estimates of the Aboriginal and Torres Strait Islander population.15
During the 20-year study period, 7217 Indigenous people died among an annual population of around 56 200 (estimated resident population in 2000) and 6701 non-Indigenous people died among an annual population of around 139 400. To increase the stability of the data, we pooled the deaths and population data into four 5-year periods. All-causes life expectancy at birth for males and females within the NT Indigenous and non-Indigenous populations over four intervals (1981–1985, 1986–1990, 1991–1995, and 1996–2000) were calculated using Chiang’s method for constructing abridged life tables.16
Using a conversion table from the Global burden of disease and injury (GBD) series,17 we mapped each cause of death into GBD groups and categories (Box 1). We chose the GBD classification because, in this system, causes of death are aggregated in a way that underpins socioeconomic development and epidemiological transition.18 This approach differs from the conventional method, which involves aggregating causes of death into ICD chapters on the basis of body system. There are three broad groups in the GBD classification. Group I comprises communicable diseases, maternal causes, conditions arising in the perinatal period and nutritional deficiencies; Group II comprises non-communicable diseases; and Group III comprises unintentional and intentional injuries.
We then applied the Vaupel and Romo9 decomposition method to discrete abridged life tables for the Indigenous and non-Indigenous populations of the NT as shown in Box 2.
The gap between the life expectancy of NT Indigenous and non-Indigenous people was large for all four periods of time and did not appear to be narrowing (Box 3). The difference in life expectancy during the last 5-year period, 1996–2000, was 16.7 years for males and 19.0 years for females (Box 4 and Box 5).
The extent to which each GBD category contributed to the life expectancy gap is shown in Box 4 and Box 5. For males (Box 4) during the first period, 1981–1985, there was considerable variation between the contributions of each category. Several categories, including cardiovascular diseases, respiratory diseases, respiratory infections and infectious diseases, contributed more than 10% each to the gap. In contrast, the contributions of both cancer and digestive diseases were negative, as the death rate due to these causes was lower for Indigenous males than for non-Indigenous males in the early 1980s.
For females (Box 5), all GBD categories except congenital anomalies contributed to the gap in life expectancy between Indigenous and non-Indigenous females during the first period, 1981–1985. The extent of their contribution ranged from 1% for several categories to 19% for infectious diseases. The contribution of cardiovascular diseases to the gap was very much less (9%) than it was for males (28%) during this period. The trend over time was very similar to that of males, with most chronic disease GBD categories, except for respiratory diseases, increasing their contribution to the life expectancy gap. By the last period, 1996–2000, cardiovascular diseases were contributing almost three times as much to the gap (24%) compared with the first period (9%), whereas the contribution of respiratory diseases halved over time.
The 95% confidence intervals indicate a sufficient sample size for a life expectancy difference between the NT Indigenous and non-Indigenous populations (Box 4 and Box 5).
The patterns demonstrated in our study are corroborated by mortality rate analyses, which have shown substantial falls in communicable disease death rates among Indigenous people over the past three decades.12 Increased mortality due to non-communicable diseases among Indigenous Australians has also been documented.3,19 The reasons for this are manifold, with a mix of social, economic and educational disadvantages, resulting in whole-of-life poor nutrition, systematic infections and adverse health behaviours in adulthood,20-22 further aggravated by poor access to primary health care services.23 The introduction of effective and sustained primary care programs to address these unmet needs for preventive, early diagnostic measures and prompt intervention is a matter of urgency.
Some underlying causes of death contributed negatively to the gap in life expectancy between Indigenous and non-Indigenous males, for example cancers, digestive diseases and intentional injury (Box 4). Li and Guthridge reported that the age-adjusted cancer death rate in NT Indigenous males was 30% below the national average in the early 1980s and became 30% above the national average by the 1990s.3 However, there were significant differences among individual cancer sites in rate ratios comparing Indigenous and non-Indigenous cancer mortality.24 Similarly, the age-adjusted death rate for Indigenous males due to chronic liver disease, the major digestive disease, was around 30% lower than non-Indigenous males in the early 1980s. For the intentional injury category, homicide death rates in Indigenous males dropped from around 50 per 100 000 during 1981–1985 to 35 per 100 000 in 1991–1995, and non-Indigenous males had relatively higher suicide mortality rates during the study period.25 Within the unintentional injury category, the major cause of death is motor vehicle traffic accidents. The upward trend in the contribution of unintentional injuries to the life expectancy gap for females is likely to be due to a small increase among Indigenous women, and a considerable decline among non-Indigenous women, in the rate of motor vehicle traffic accident deaths.25 In contrast, motor vehicle traffic accident deaths among men have declined for both Indigenous and non-Indigenous people.
A limitation of our study was the use of GBD groups, which arbitrarily separate communicable and non-communicable diseases. There is evidence to suggest that infectious and non-infectious diseases are interrelated. For example, bacterial infections of the ears, nose and skin are associated with renal and heart disease.26,27 The reverse has also been reported with non-communicable diseases such as diabetes, which has been shown to amplify the effect of infection in Indigenous communities.28
The introduction of ICD-10 in 1997 has resulted in some artefactual variation in disease coding rules. The comparability with ICD-9 has been assessed by the ABS.29 The most notable variations at a code level are asthma, rheumatic fever (resulting in a 25% and 30% decrease, respectively) and dementia (50% increase). These changes have not had a significant impact on the higher order categories applied in this study.
1 Global burden of disease classification for diseases and injuries17
Group I — Communicable, maternal, perinatal and nutritional conditions
Infectious and parasitic diseases
Conditions arising during the perinatal period
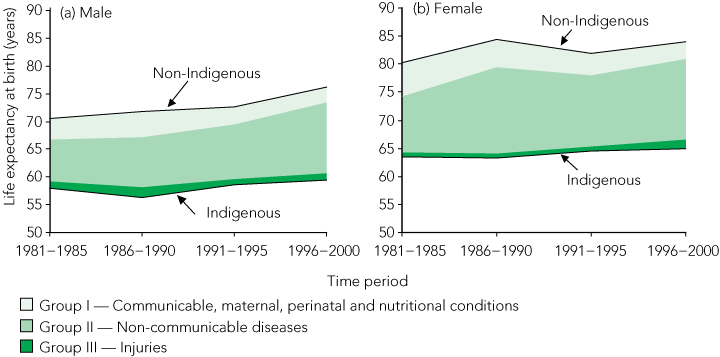
3 Trends in the life expectancy gap between Indigenous and non-Indigenous people in the Northern Territory, 1981–2000, for global burden of disease groups
4 Decomposition differences in life expectancies between Indigenous and non-Indigenous populations, males, Northern Territory, 1981–2000
- Yuejen Zhao1
- Karen Dempsey2
- Department of Health and Community Services, Health Gains Planning Branch, Darwin, NT.
None identified.
- 1. Murray CJ, Salomon JA, Mathers CD, Lopez AD. Summary measures of population health — concepts, ethics, measurement and applications. Geneva: World Health Organization, 2002.
- 2. Australian Bureau of Statistics. Australian social trends. Canberra: ABS, 2005. (Catalogue No. 4102.0.)
- 3. Li SQ, Guthridge S. Mortality in the Northern Territory: 1981 to 2000. Darwin: Department of Health and Community Services, 2004.
- 4. Australian Bureau of Statistics. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples. Canberra: ABS, 2003. (Catalogue No. 4704.0.)
- 5. Lopez AD, Ruzicka LT. The differential mortality of the sexes in Australia. In: McGlashan ND, editor. Studies in Australian mortality. Hobart: University of Tasmania, 1977. (Environmental Studies Occasional Paper 4.)
- 6. Arriaga EE. Measuring and explaining the change in life expectancies. Demography 1984; 21: 83-96.
- 7. Pollard JH. On the decomposition of changes in expectation of life and differentials in life expectancy. Demography 1988; 25: 265-276.
- 8. Conti S, Farchi G, Masocco M, et al. The impact of the major causes of death on life expectancy in Italy. Int J Epidemiol 1999; 28: 905-910.
- 9. Vaupel JW, Romo VC. Decomposing change in life expectancy: a bouquet of formulas in honor of Nathan Keyfitz’s 90th birthday. Demography 2003; 40: 201-216.
- 10. Weeramanthri TS. A medical cause of death validation study of adult Aboriginal deaths in the Northern Territory of Australia in 1992. Public Health 1997; 111: 429-433.
- 11. Plant AJ, Condon JR, Durling G. Northern Territory health outcomes, morbidity and mortality 1979-1991. Darwin: NT Department of Health and Community Services, 1995.
- 12. Condon JR, Barnes T, Cunningham J, Smith L. Improvements in Indigenous mortality in the Northern Territory over four decades. Aust N Z J Public Health 2004; 28: 445-451.
- 13. Ross K. Occasional paper: population issues, Indigenous Australians 1996. Canberra: Australian Bureau of Statistics, 1999, 15 Feb. (Catalogue No. 4708.0.)
- 14. Australian Bureau of Statistics. Deaths, Australia, 2004. Canberra: ABS, 2006. (Catalogue No. 3302.0.)
- 15. Australian Bureau of Statistics. Experimental estimates and projections, Aboriginal and Torres Strait Islander Australians. Canberra: ABS, 2004. (Catalogue No. 3238.0.)
- 16. Chiang CL. The life table and its applications. Malabar, FL: Robert E Krieiger Publishing Company, 1984.
- 17. Murray CJ, Lopez AD. Global burden of disease and injury series. Volume I: The global burden of disease — a comprehensive assessment of mortality and disability from diseases, injuries, and risk factors in 1990 and projected to 2020. Boston: Harvard University Press, 1996.
- 18. Foliaki S, Pearce N. Changing pattern of ill health for indigenous people. BMJ 2003; 7: 406-407.
- 19. Spencer JL, Silva DT, Snelling P, Hoy WE. An epidemic of renal failure among Australian Aboriginals. Med J Aust 1998; 168: 537-541. <MJA full text>
- 20. Hoy WE, Mathews JD, McCredie DA, et al. The multidimensional nature of renal disease: findings in a high risk Australian Aboriginal community. Kidney Int 1998; 54: 1296-1304.
- 21. Smith RM, Spargo RM, King RA, et al. Risk factors for hypertension in Kimberley Aborigines. Med J Aust 1992; 156: 562-566.
- 22. Guest CS, O’Dea K, Larkins RG. Blood pressure, lipids and other risk factors for cardiovascular disease in Aborigines and persons of European descent of southeastern Australia. Aust J Public Health 1994; 18: 79-86.
- 23. Byron P, Zhao Y, Guthridge S, et al. Medicare and Pharmaceutical Benefits Scheme usage patterns in the Northern Territory 1993/94 to 2003/04. Darwin: NT Department of Health and Community Services, 2005.
- 24. Zhao Y, Condon JR, Garling LS. Cancer incidence and mortality, Northern Territory 1991-2001. Darwin: NT Department of Health and Community Services, 2004.
- 25. Dempsey KE, Condon JR. Mortality in the Northern Territory 1979-1997. Darwin: Territory Health Services, 1999.
- 26. Van Buynder PG, Gaggin JA, Martin D, et al. Streptococcal infection and renal disease markers in Australian aboriginal children. Med J Aust 1992; 156: 537-540.
- 27. Carapetis JR, Currie BJ. Preventing rheumatic heart disease in Australia [editorial]. Med J Aust 1998; 168: 428-429. <MJA full text>
- 28. Phillips CB, Patel MS, Weeramanthri TS. High mortality from renal disease and infection in Aboriginal central Australians with diabetes. Aust J Public Health 1995; 19: 482-486.
- 29. Australian Bureau of Statistics. Causes of death, Australia, 2004. Canberra: ABS, 2006. (Catalogue No. 3303.0.)






Abstract
Objective: To identify the causes of the gap in life expectancy between Indigenous and non-Indigenous populations of the Northern Territory and how the causes have evolved over time.
Design and setting: Analysis of NT death data over four 5-year periods, 1 January 1981 to 31 December 2000 inclusive. A decomposition method using discrete approximations (Vaupel and Romo) was applied to abridged life tables for the Indigenous and non-Indigenous populations of the NT.
Main outcome measures: Contribution of causes of death, grouped according to global burden of disease groups and categories, to the life expectancy gap.
Results: The gap between the life expectancy of Indigenous and non-Indigenous people in the NT did not appear to narrow over time, but there was a marked shift in the causes of the gap. In terms of disease groups, the contribution of communicable diseases, maternal, perinatal and nutritional conditions halved during the 20 years to 2000. Meanwhile, the contribution of non-communicable diseases and conditions increased markedly. The contribution of injuries remained static. In terms of disease categories, the contribution of infectious diseases, respiratory infections and respiratory diseases declined considerably; however, these gains were offset by significantly larger increases in the contribution of cardiovascular diseases and diabetes for Indigenous women and cardiovascular diseases, cancers and digestive diseases for Indigenous men.
Conclusions: The main contributors to the gap in life expectancy between the Indigenous and non-Indigenous populations were non-communicable diseases and conditions, which are more prevalent in ageing populations. With the life expectancy of Indigenous people in the NT expected to improve, it is important that public health initiatives remain focused on preventing and managing chronic diseases.