New guidelines and funding for this preventable disease have been long awaited
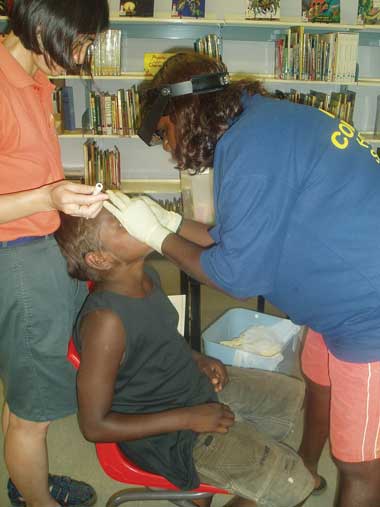
In line with its Vision 2020 initiative, the World Health Organization adopted a resolution to eliminate blinding trachoma by 2020. To achieve this goal, WHO recommends the SAFE strategy (Surgery, Antibiotics, Facial cleanliness and Environmental improvement) for countries implementing trachoma control programs. Australia is the only developed country of the 57 trachoma endemic countries listed by WHO.1
Trachoma was endemic and a significant cause of blindness in many parts of the Western world, including Australia, until the early 1900s. As housing, hygiene and living conditions improved, trachoma disappeared from most parts of Australia.2 However, these improvements are yet to occur in remote Aboriginal populations in Australia, where trachoma is still endemic.
Why is Australia the only developed country with endemic trachoma? Firstly, the socioeconomic determinants of trachoma (ie, poverty and overcrowded living conditions) are highly prevalent among Aboriginal people living in remote areas. Secondly, Australia’s trachoma control efforts have been patchy and inconsistent since the National Trachoma and Eye Health Program finished in 1978.3 In the absence of a national approach, some trachoma-endemic states or areas have prioritised trachoma control and have implemented programs based on the 1993 WHO trachoma control guidelines, while others have not. Furthermore, while all current programs include periodic trachoma screening and antibiotic treatment, very few include the “S”, “F” and “E” components. Thirdly, epidemiological data on trachoma, an essential element of any control program, are difficult to obtain and interpret because each trachoma control program has its own data collection system, and data from different regions and states are not collated. Trachoma is not a nationally notifiable disease. Thus, despite availability of a highly effective one-dose treatment (azithromycin) provided free through remote Indigenous health clinics and regional population health units since 1998, trachoma transmission continues.
Recent molecular epidemiological research from the Northern Territory showed different Chlamydia trachomatis strains in coastal compared with inland communities, indicating that trachoma transmission may occur more within communities or within groups of neighbouring communities rather than between far-flung, distant communities.4 In contrast, a similar Western Australian study showed that most WA trachoma strains were of the Ba Apache type, which circulated in both coastal and central communities across the length and breadth of WA and was identical to one of the NT strains.5 This finding is consistent with anecdotal reports of high levels of mobility of Indigenous people within and between regions, and suggests that the effectiveness of trachoma control activities may be improved by enhanced inter-regional coordination (eg, conducting trachoma screening and treatment at the same time in all affected areas).
Key recommendations of the Guidelines for the public health management of trachoma in Australia6
Trachoma control should be the responsibility of government-run regional population health units, working in collaboration with primary health care services and Aboriginal community representatives.
Regional population health units should collect trachoma data in accordance with the minimum national trachoma dataset.
In regions where trachoma is endemic but trichiasis prevalence is unknown, the burden of trichiasis should be quantified.
In areas where trachoma or trichiasis is or has been endemic, Aboriginal and Torres Strait Islander people aged 40–54 years should be screened every 2 years and those aged 55 years and older should be screened annually for trichiasis as part of an adult health check.
The minimum target group for active trachoma screening should be Indigenous children aged 5–9 years living in communities/towns where trachoma is endemic.
All children found to have active trachoma and their household contacts aged 6 months and older should be treated with single-dose azithromycin.
Antibiotic treatment of affected people, household contacts and community members (when required) should be completed within 2 weeks of screening.
Where population mobility is high, all screening and treatment activities within the region should be completed in as short a timeframe as possible to minimise the likelihood of reinfection and to achieve higher population coverage.
The publication of the Guidelines for the public health management of trachoma in Australia,6 which were developed by the Department of Health and Ageing and the Communicable Diseases Network of Australia (CDNA), and the Australian Government’s allocation of $920 000 towards trachoma control over the next 3 years7 represent a long-awaited national approach to controlling this preventable disease. The states and territories will receive $470 000 of this new funding, to train health workers to implement consistent trachoma screening and control measures. The remaining $450 000 will be used to establish a national trachoma surveillance unit to enable consistent data collection on trachoma. The CDNA’s trachoma steering group, which has representatives from states and territories where trachoma is endemic, will provide expert advice regarding trachoma surveillance and control.
The guidelines cover trachoma screening, control and data collection (Box). They recommend that trachoma control, including data collection and reporting, should be the responsibility of, and coordinated by, government-run regional population health units, working in collaboration with primary health care services and Aboriginal community representatives. The guidelines stress the importance of implementing all four components of the SAFE strategy. In accordance with one of the resolutions of the 2003 Global Scientific Meeting on Trachoma, the guidelines recommend single-dose azithromycin for all children and all adult household contacts of affected people when childhood active trachoma prevalence is 10% or greater.8 Monitoring of azithromycin resistance is recommended.9
The guidelines are consistent with the spirit of, but do not replicate, the WHO guidelines because high level evidence from randomised controlled trials or meta-analyses of randomised controlled trials exists only for one component (Surgery) of the WHO’s SAFE strategy, and because it is considered important that Australian guidelines reflect Australian experiences of trachoma control.10
Not all stakeholders may agree with the recommendations. Some may dispute the need, given the magnitude of death and ill health in Aboriginal communities due to diabetes, heart disease, mental illness and injury, to channel health resources towards a condition that they believe rarely or no longer results in blindness.11 Others may consider the guidelines too conservative to be able to eliminate blinding trachoma by 2020. Despite these criticisms, the guidelines will at least establish, for the first time, a national minimum best-practice approach for the public health management of trachoma, which if implemented can only strengthen Australia’s efforts towards controlling and eliminating trachoma. Furthermore, they provide yet more impetus for further and broader initiatives to address socioeconomic deprivation, the underlying cause of continued trachoma transmission in Australian Aboriginal communities.
- 1. World Health Organization, Edna McConnell Clark Foundation. Primary health care level management of trachoma. WHO/PBL/93.33. Geneva: World Health Organization, 1989.
- 2. Taylor HR. Trachoma in Australia. Med J Aust 2001; 175: 371-372. <MJA full text>
- 3. Taylor V, Ewald D, Liddle H, Warchivker I. Review of the implementation of the National Aboriginal and Torres Strait Islander Eye Health Program. Canberra: Commonwealth of Australia, 2003. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-oatsih-pubs-index.htm (accessed Apr 2006).
- 4. Stevens MP, Tabrizi SN, Muller R, et al. Characterisation of Chlamydia trachomatis omp1 genotypes detected in eye swab samples from remote Australian communities. J Clin Microbiol 2004; 42: 2501-2507.
- 5. Porter MC, Mak DB, Chidlow G, et al. Molecular epidemiology of ocular Chlamydia trachomatis infections in Western Australia: implications for trachoma control. J Infect Dis 2006. Submitted.
- 6. Communicable Diseases Network Australia. Guidelines for the public health management of trachoma in Australia. Canberra: Commonwealth of Australia, 2006. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-oatsih-pubs-index.htm (accessed Apr 2006).
- 7. Abbott T. New trachoma unit to combat eye disease. Media release ABB158/05. 6 Dec 2005. Available at: http://www.health.gov.au/internet/ministers/publishing.nsf/Content/MediaReleases-1 (accessed Apr 2006).
- 8. World Health Organization. Report of the second global scientific meeting on trachoma. WHO/PDB/GET 03.1. Geneva, 25–27 August 2003.
- 9. Leach AJ, Shelby-James TM, Mayo M, et al. A prospective study of the impact of community-based azithromycin treatment of trachoma on carriage and resistance of Streptococcus pneumoniae. Clin Infect Dis 1997; 24: 356-362.
- 10. Kuper H, Solomon AW, Buchan J, et al. A critical review of the SAFE strategy for the prevention of blinding trachoma. Lancet Infect Dis 2003; 3: 372-381.
- 11. Australian Bureau of Statistics. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples, 2005. Canberra: ABS, 2005. (ABS Catalogue No. 4704.0.)





Thanks to the Kimberley community health nurses, Aboriginal health workers and community members who worked with me and taught me about trachoma control. Thanks to Aileen Plant for helpful comments on late drafts of this article.
None identified.