Are we doing enough to target children in need in Australia?
Based on the most stringent definition of poverty (the lowest decile of gross income), 80% of Australian children (< 15 years of age) did not experience poverty over the period 1995–1997; of the 20% who did, only 1% were in persistent poverty in this period.1
However, despite Australia’s material wealth and the generally high level of education, many indicators of health and wellbeing in children and adolescents are discouraging. The rates of developmental and behaviour disorders in children are high2,3 (15% of those aged 4–12 years have emotional or behavioural problems4); the rate of children in out-of-home care (currently 4.2 per 1000) has been rising consistently since national data collection began in 1996;5 and a third of deaths in children aged 1–4 years have preventable causes (transport fatalities, drowning and assault). In teenage girls pregnancy rates are high, and suicide rates in young Australian males have quadrupled over the past 30 years.2 Children seeking asylum in Australia face multiple challenges in accessing health care despite complex health needs, including experience of trauma and effects of prolonged detention.6
Child health is a barometer of social ill health and highlights the discrepancies between children from different backgrounds. Preschoolers from low socioeconomic backgrounds are more likely to experience developmental delay, injuries and hospitalisations and are less likely to have been breastfed, to be fully immunised, and to attend good quality childcare facilities. Adolescents from disadvantaged backgrounds are at higher risk of poor literacy, behaviour disorders, unwanted pregnancy and attempted suicide.
In Australia, many of these indicators are most noticeable in Aboriginal and Torres Strait Islander children. For example, age-adjusted hospitalisation rates for injury among Indigenous children are consistently higher than the rates among non-Indigenous children, particularly for burns, assault and poisoning, in rural areas and among males.
There is a growing body of literature both in Australia and internationally documenting the association between socioeconomic status and mortality, with disadvantaged groups experiencing higher death rates for most major causes of death at all ages,7,8 and mortality rates rising stepwise as children’s level of disadvantage worsens (Box 1).9 It has been calculated that each year in Australia 1500 deaths of children aged 0–14 years can be attributed to socioeconomic disadvantage.10,11 In Aboriginal and Torres Strait Islander children, average death rates remain 2.5 times those in non-Indigenous children.3 There is also evidence that mortality inequalities have widened over time in Australia.9,12
Health inequality itself may play a role in undermining the health of the most disadvantaged groups, possibly through mechanisms such as psychosocial distress, reduced sense of wellbeing, lack of hope, and social exclusion.
On the other hand, wealthier groups in Australia are more able to implement healthy lifestyle behaviours, use preventive health services and take advantage of social policies to improve their health.3 Paradoxically, patients of lower educational and occupational status are the lowest users of preventive care services, and general practitioners spend less time with them, reporting being overwhelmed by the seriousness and extent of their problems.13,14
The determinants of child health are complex and operate at many levels, including global forces, government policies, the health care system, psychosocial factors, individual health behaviours, and biological reactions. These factors also interact with each other to determine the pathway to health (or disease), particularly if they occur at developmentally crucial times. Current understanding suggests that adverse environments in early life, interacting with a child’s genetic and temperamental predisposition, result in biological changes (such as neuronal connections) that determine coping, resilience and health outcome in adult life.15 This creates some pressure on society to “get it right”, as children in adverse circumstances are being programmed in a way that sets patterns of health for later life. Simple solutions, such as targeting behaviour change or welfare programs, are less likely to be as effective as action at all levels, including societal and cultural change.16
Attempts to understand the complex relationship between health outcomes and their determinants have led to the concept of social capital. Defined as “the social cohesion of a community, and the sense of belonging” that individuals feel,17 social capital represents the degree to which people feel they can request assistance from their neighbours, allow their children to play outside in safety, and participate in community activities. Social capital results in independent improvements in health indicators: higher behavioural scores in children, reduced school dropout rates, less criminality, and lower smoking rates among women.18 Although the precise pathways are poorly understood, the evidence suggests that creating opportunities for community networking is empowering and plays a role in improving child health in poor communities. Social capital programs based in schools have improved mental health outcomes and reduced risk-taking behaviours.19 A systematic review of the qualitative evidence suggests that good family relationships, friendships and neighbourhood networks help to mitigate the impact of disadvantage on the wellbeing of children and young people.20
Undermining the social capital of Australian society is the marginalisation of certain groups. In Australia, considerably less progress has been made than in other countries (such as New Zealand and Canada) in addressing health inequalities between Indigenous and non-Indigenous people. In addition, the sense of hope and of having a valued role in society, which are determinants of health, may be less in Australian Indigenous groups compared with Indigenous people elsewhere.21
It has been argued that “institutional racism” is inherent in our health services, and takes the form of inadequate funding (which is not commensurate with the extra health need), inequitable Medicare primary health care spending on Indigenous groups, lack of access to Medicare for some asylum seekers, and culturally insensitive health services.22
In addition to the economic, cultural and literacy barriers faced by many people in accessing health care, children face specific challenges in that they are reliant on advocates to act in their interests. Many community services have complex eligibility criteria and long waiting lists, and children in the most vulnerable situations, such as those in foster care or living in impoverished or unstable family situations, are most likely to be further disadvantaged.
Children are a powerless group within society, and it is relatively easy to violate their rights. This is obvious in sexual exploitation or prolonged detention of children seeking asylum, but in more subtle forms is pervasive throughout society. An example includes the difficulty in achieving legislation banning physical punishment in the United Kingdom — society’s most vulnerable citizens thus have less protection from assault than adults.23
Even children from privileged backgrounds are largely excluded from decision making, and are generally regarded as incomplete and incapable adults. This is distinct from regarding children as people who function responsibly and appropriately, given their age, and who can provide valuable insights into their own needs, especially those who have experienced adverse events, illness or disability. UK research has highlighted the lack of prioritisation of children’s needs in the restructuring of health care trusts, and the scanty consultation and participation of chronically ill or disabled children in the development of health services.24,25 The NSW Commission for Children and Young People has demonstrated some early success in consulting with children on their submissions regarding public education and young driver safety,26 in line with mounting evidence that children can contribute effectively to health service development.27,28
Counteracting the negative factors are resilience and protective factors that promote child wellbeing and support the development of self-regulation and child competence. These operate at three levels:
society and environment — supportive and inclusive environments, economic security, effective public health programs;
family, school and neighbourhood — parental and family cohesion, family friendly workplaces, a close bond with at least one consistent caretaker in the early years, access to appropriate services; and
the child — physical and mental health, resilience, good language and communication skills, effective problem solving skills, and positive cultural identity.29,30
Societal problems directly affect how children present in the consultation room. Australian researchers have drawn attention to the links between mental health and behavioural problems in children and adolescents, and socially disorganised communities.19 Lack of social capital is strongly associated with child abuse.31 Suicide in young males is closely linked to unemployment rates.32 Children living in jobless families are more likely to present with developmental and educational difficulties. Asthmatic children who live in families where there is tension and conflict are more frightened by their symptoms than other children with asthma.3
Box 2 provides some examples of health inequalities, together with related national strategies and roles for individual health professionals.
One of the challenges is that health care in Australia largely takes place in an individualistic renumeration system based on patients voluntarily seeking care. Many Divisions of General Practice and profession leaders are committed to extending the GP’s patient-centred clinical role to improving the health of practice populations. However, barriers include the absence of targeted government funding for disadvantaged groups, the Medical Benefit Schedule rewarding mainly episodic care rather than preventive care, and the lack of formal responsibility by practices for a specified practice population (as occurs in New Zealand and the UK).37 This creates little opportunity for improving the health of communities, and engaging with community development programs. While this may not be regarded by health care professionals as their area of expertise, without targeting pre-existing health determinants, such as unemployment or poverty, little can be done in the consulting room to address the battery of problems some patients have on presentation.
State government policy appears to recognise that empowering communities by improving women’s educational status, and creating employment opportunities and community development programs will remove some of the determinants of poor health. However, translating these policies into practice, and improving health indicators have proved challenging, and evidence of improvements in child health or health inequity is limited.
Professor Stanley, Chief Executive Officer of the Australian Research Alliance for Children and Youth, asserts that the response of governments to societal problems tends to target solutions too close to the outcomes (building prisons rather than intervening early to reduce crime). In addition, when the approach focuses on individual factors (personal health risk) rather than population factors (tobacco production, advertising and distribution, and social factors affecting consumption), the result is a general shift in problems from rich to poor people (tobacco smoking), thus widening discrepancies.43 Initiatives that have been successful in rapidly improving health status alter mean population exposure (such as fluoridation of water to improve dental health), although for many interventions disadvantaged groups also require specific targeting. The way forward may lie in engaging the most disadvantaged communities, building on communities’ own resources and skills in developing resilience, and developing ways of working collaboratively to address health and broader issues.
Evidence that social capital, and thus child health, can be improved by early intervention and home visiting programs has driven the introduction in the past decade of government initiatives such as the Stronger Families and Communities Strategy: communities for children (a federally funded partnership with local community organisations [in 2000]),44 Families First (NSW [in 1998]),45,46 Best Start (Victoria), Pathways for Families (South Australia), Family CARE program (Queensland Health) and others in Australia and overseas. These programs generally aim to support parents of young children, encourage early childhood learning and development, and assist communities to become more child friendly through various interventions (including combinations of home visiting, improving access to health and early education services, fathering and culture-specific programs, and community capacity building initiatives).
Initially, home visitation programs in early childhood in the United States targeted child abuse, but unexpected positive effects were seen in maternal and child health. Box 3 presents some of the early findings in this area.
The local programs are generally multisectoral (including departments of education, community, health, disability and housing), an acknowledgement that social and environmental factors have more influence on child health outcomes than health interventions, drugs or other treatments. They also recognise that modifying early environments is a more powerful way of producing change than later interventions. The rationale is that the child’s social and emotional development is highly correlated with his or her sense of belonging and connectedness to family and school, and that educational development is affected by participation in quality early childhood development programs. This draws on the evidence that preschool experience reduces the gap in achievement between disadvantaged and advantaged children in the early years of school, and has long term academic benefits.49,52,53 Importantly, studies have demonstrated the greatest benefits in children from more deprived backgrounds (Box 3).47
Overseas studies have shown that the more effective home visiting programs employ nurses rather than paraprofessionals. The nurses begin visiting during pregnancy, and visit frequently and for long enough to establish a therapeutic alliance with the families. At least two and probably three components produce the greatest effects: an effective program model, the right visitor type, and a target population that is in need and sees the value of the service being offered.54
For an individual medical practitioner, community home visiting programs are “out there”. How do we bring “social capital” into the clinical environment, and can an individual doctor play any role in enhancing the community connectedness of his or her patients? Perhaps the first steps involve simply:
acting as a resource and provider of effective health promotion material;
informing people about support groups;
making the hospital, clinic or consulting room available for community members as a meeting place; and
facilitating contact between parents of, for example, disabled children, so they can rally together for services.
Harris suggests that practitioners should coordinate and organise preventive activities, possibly through practice nurses, and actively liaise with community and population health organisations to provide complementary interventions.14 Some practitioners may extend their role to advocating on behalf of groups of vulnerable children, making representations to the local council for safe playgrounds or roads crossings, encouraging the local schools to become asthma friendly, and ensuring the rights of children in care or in institutions are being respected (see Box 4).
Groups of professionals can be successful advocates and it is encouraging to note the policy statements of the Royal Australasian College of Physicians (RACP) about social justice issues, including “Children and the media”, and “Ethics of research in children”. In a recent “Inequity and health” policy statement, the RACP emphasises that the substantial and systematic health inequalities that exist in Australia reflect unjust differences in opportunity, access to services and material resources. They call on the government for a coordinated response to health inequities, and on health organisations to develop explicit plans for dealing with health inequities.
Few would refute that all children regardless of their ethnicity or background have a right to health and to realise their potential. If allocation of resources “to the maximum extent of their availability” is required in order to meet our obligations under the UN Convention on the Rights of the Child, are we doing enough to target children in need in Australia?
A study in the UK modelled the health effects if all children had health outcomes similar to those of the most privileged.55 The results showed a more than 50% reduction in hyperkinetic disorders and child abuse, and a 40% reduction in educational disability and mental disorders. Improving health outcomes is unlikely to be achieved by health interventions alone, but rather by collaborative economic and political approaches extending beyond the health sector.
We are faced with the challenge of improving child health through reducing inequity, building safe and resilient communities, addressing discrimination, and reducing marginalisation of certain population groups.
We are only beginning to understand the complex chain of influences that result in adverse outcomes, and we have yet to develop effective ways for health professionals to engage with community development programs. We are challenged to implement programs shown to be effective in clinical trials, and to monitor health and equity outcomes across discipline boundaries.
Some encouragement can be found in the mounting evidence that community programs make a difference to child health, the early government recognition of the importance of investing in young children, the acknowledgement that health interventions require the support of the social system, and the recent launch of an Australian national collaborative research network aiming to enhance child health and development.
Evidence-based interventions
Home visitation during the perinatal period and infancy for families of low socioeconomic status, single parents or teenage parents reduces rates of low birthweight, intentional and unintentional injuries, child behaviour problems, maternal substance abuse and welfare dependency, and increases rates of breastfeeding, immunisation and health service utilisation (I [injuries]; II [other outcomes]).47,56
Quality early childhood education improves school attendance, cognitive development in the early years, academic achievement in high school and reduces high school dropout rates. There are also long term mental health improvements and better educational, employment and income outcomes (II).47-49,52,53
High levels of school and community social capital (community connectedness) are associated with improvements in health indicators such as mental and behavioural scores in children, risk-taking behaviour in teenagers, antisocial behaviour and criminality, and smoking rates in women (III-3).18,57
Levels of evidence (I–IV) are derived from the National Health and Medical Research Council’s system for assessing evidence.58
Relevant websites
Child and Youth Health: www.cyh.com
Parenting and child and youth health; links to research updates; telephone help-lines for parents and youth.
Australian Research Alliance for Children and Youth: www.aracy.org.au/index.htm
National collaboration of researchers, policy makers and practitioners from many disciplines to build a better future
for Australia’s children and young people.
Best Start, Department of Human Services, Victoria: www.beststart.vic.gov.au
Extensive links to international resources on home visiting, early childhood literature, childhood services throughout Australia.
National Public Health Partnership: http://www.nphp.gov.au
Identifies and develops strategic and integrated responses to public health priorities in Australia. Current priorities include: healthy weight, communicable disease control, environmental health, injury prevention, child public health, information development, and workforce development and planning.
1 Childhood mortality rates9
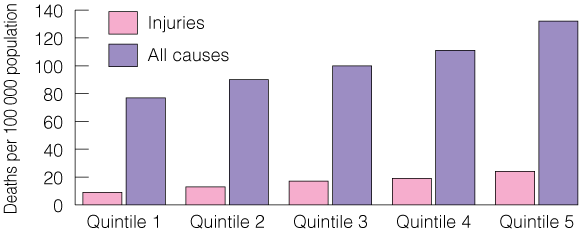
Age-standardised mortality rates for children aged 0–14 years, all causes and injury mortality, 1998–2000.
Quintile 1 = least disadvantaged; quintile 5 = most disadvantaged.
2 Inequalities and national strategies — some examples
Health inequality/National strategy |
Role of health professionals |
||||||||||||||
Women of lower socioeconomic status |
|||||||||||||||
National Drug Strategic Framework 1991–99 to 2001–04 (includes tobacco, alcohol and illicit drug strategies)33 |
|
||||||||||||||
Eat Well Australia: an Agenda for Pubic Health Nutrition, 2000–201034 National Aboriginal and Torres Strait Islander Nutrition Strategy and Action Plan35 |
|
||||||||||||||
Children of lower socioeconomic status |
|||||||||||||||
National Strategic Framework for Aboriginal and Torres Strait Islander Health36 National Public Health Partnership30 |
|
||||||||||||||
Draft National Injury Prevention Plan: 2004 Onwards37 |
|
||||||||||||||
National Agenda for Early Childhood38 |
|
||||||||||||||
Immunise Australia Program39 |
|
||||||||||||||
National Asthma Council40 |
|
||||||||||||||
Healthy Weight 2008 — Australia’s Future41 |
|
||||||||||||||
National Mental Health Plan 2003–200842 |
|
||||||||||||||
3 Investment in the early years of childhood, in the home and school — program characteristics and outcomes
Early home visiting
400 mothers (< 19 years old, unmarried or of low socioeconomic status) were allocated at random to a control group or to be visited by prenatal and early childhood nurses. Intervention families received home visits during pregnancy (mean, 9) and for 2 years after delivery (mean, 23).47
Intervention families had fewer subsequent pregnancies, and showed reductions in child behaviour problems, youth criminal behaviour, child abuse and neglect, maternal substance abuse and dependency on welfare services.
735 women (low income, first time mothers) were allocated at random to a control group or to receive home visits from either trained paraprofessionals or nurses.48
Visits by paraprofessionals typically produced effects about half those produced by nurses: reductions in smoking during pregnancy, longer pregnancy intervals, greater employment, and improved 2 year developmental outcomes for children.
Preschool/childcare
An analysis of observational and controlled trials of participation in early childhood and preschool programs (of diverse quality) from 13 countries.49
Preschool programs promote cognitive development in the short term; have a positive impact on school preparation, and attendance and achievement in early years of school; and reduce the achievement gap between disadvantaged and advantaged children.
Early high quality educational childcare aimed at 3- and 4-year-olds from low income families; random assignment to control and intervention groups, follow-up to age 40 years.50
Short term: Increased IQ (0.5 SD, fades over time) and achievement; smaller effects on social behaviour, self-esteem and academic motivation; improved parental health and safety habits.
Long term: Some studies show diminution in effects over time, and methodological issues limit interpretation. Others show a variety of improved mental health outcomes, reduced involvement in crime, better educational and employment outcomes; and greater likelihood of home ownership and stable adult relationships.
Parenting
Triple P — Positive Parenting Program using behavioural family interventions in preschool children with early conduct-related problems; series of randomised controlled trials.51
Results include lower levels of parent-reported child behaviour problems, lower levels of dysfunctional parenting, and a higher sense of parental competence, maintained at 1-year follow-up.
4 The extended role of the clinical practitioner
Examine social supports as extensively as other aspects of a child’s health status
Consider and promote a child’s early development as a critical period during which optimal care should be provided
Support the development of parenting programs and community support networks and assist families to make contact with others in similar situations
Work with children and families in ways that empower and support them, and inform them of their rights
Act as a resource centre for families, offering information about local services and support groups, and effective health promotion material
Develop cultural awareness and competence in working in diverse communities
Develop dedicated preventive activities within the practice, possibly through practice nurses, and support the role and importance of nurses and home visitors in activities that improve child health outcomes
Develop linkages with public health organisations and become aware of local resources and programs for disadvantaged groups
Advocate for both individual children (to access child care, appropriate education, respite care and other services) and groups of children (to influence policy and practice on investing in the early years, building social capital, child friendly legislation)
Work within professional organisations and with other professional groups to influence the views of opinion leaders, politicians and the community around tolerance and social policy
Link with other agencies outside of the health sector to develop research and policy agendas, data collection and monitoring systems around health indicators and inequalities
- 1. Abello A, Harding A. The dynamics of child poverty in Australia. National Centre for Social and Economic Modelling (NATSEM). Canberra: University of Canberra, March 2004. (Discussion Paper No. 60.) Available at: www.natsem.canberra.edu.au/publications/papers/dps/dp60/dp60.pdf (accessed Nov 2004).
- 2. Australian Bureau of Statistics. Health of children. Canberra: ABS, 2004. (Catalogue No. 4829.0.) Available at: www.abs.gov.au/Ausstats/abs@.nsf/w2.1.1!OpenView&Start=1&Count=1000&Expand=18#18 (accessed Jul 2005).
- 3. Al-Yaman F, Bryant M, Sargent H. Australia’s children: their health and wellbeing 2002. Canberra: Australian Institute of Health and Welfare, 2002. (AIHW Catalogue No. PHE 36.) Available at: www.aihw.gov.au/publications/phe/ac02/ac02-c00.pdf (accessed Jul 2005).
- 4. Sawyer MG, Arney FM, Baghurst PA, et al. The mental health of young people in Australia: key findings from the child and adolescent component of the National Survey of Mental Health and Well-being. Aust N Z J Psychiatry 2001; 35: 806-814.
- 5. Australian Institute of Health and Welfare. Child protection Australia 2003-4. Child Welfare Series No. 36. Canberra: AIHW, 2005. (AIHW Catalogue No. CWS-24.) Available at: www.aihw.gov.au/publications/index.cfm/title/10095 (accessed Jul 2005).
- 6. Davidson N, Skull S, Burgner D, et al. An issue of access: delivering equitable health care for newly arrived refugee children in Australia. J Paediatr Child Health 2004; 40: 569-575.
- 7. Draper G, Turrell G, Oldenburg B. Health inequalities in Australia: mortality differences by socioeconomic disadvantage. Health Inequalities Monitoring Series No. 1. Canberra: Australian Institute of Health and Welfare, 2005. (AIHW Catalogue No. PHE-55.) Available at: www.aihw.gov.au/publications/index.cfm/title/10041 (accessed Jul 2005).
- 8. Marmot M. Economic and social determinants of disease. Bull World Health Organ 2001; 79: 988-989.
- 9. Draper G, Turrell G, Oldenburg B. Health inequalities in Australia: mortality. Health Inequalities Monitoring Series No 1. Canberra: Queensland University of Technology and the Australian Institute of Health and Welfare, 2004. (AIHW Catalogue No. PHE-55.) Available at: www.aihw.gov.au/publications/index.cfm/title/10041 (accessed Jul 2005).
- 10. The Royal Australasian College of Physicians. Inequity and health — a call to action. Policy statement 2005. Sydney: RACP, 2005. Available at: www.racp.edu.au/hpu/policy/inequity/index.htm (accessed Jul 2005).
- 11. McCracken K. What if New South Wales was more equal? NSW Public Health Bull 2002; 13: 123-127.
- 12. Australian Bureau of Statistics. Measuring Australia’s progress 2002. Canberra: ABS, 2004. (Catalogue No. 1370.0.) Available at: www.abs.gov.au/Ausstats/abs@.nsf/0/3eba282aaaea6cdbca256b90007da224?OpenDocument (accessed Nov 2004).
- 13. Traynor VJ, Rose VK, Harris E, et al. What role for Divisions of General Practice in addressing health inequity within their communities? [letter]. Med J Aust 2000; 173: 79.
- 14. Harris MF, Mercer PJT. Reactive or preventive: the role of general practice in achieving a healthier Australia. Med J Aust 2001; 175: 92-93. <MJA full text>
- 15. Cyander M, Frost B. Mechanisms of brain development: sculpting by the physical and social environment. In: Keating D, Hertzman C, editors. Children of the information age: developmental health as the wealth of nations. Chapter 8. New York: Guilford Press, 1999.
- 16. Sainsbury P, Harris E. Understanding the causes of health inequalities: incorporating personal, local, national, and global perspectives [guest editorial]. NSW Public Health Bull 2002; 13: 121-123.
- 17. Elliman D, Hall D. Health for all children, 4th edition. Oxford: Oxford University Press, 2003.
- 18. Waterston T, Alperstein G, Stewart-Brown S. Social capital: a key factor in child health inequalities. Arch Dis Child 2004; 89: 456-459.
- 19. Alperstein G, Raman S. Promoting mental health and emotional well-being among children and youth: a role for community child health? Child Care Health Dev 2003; 29: 269-274.
- 20. Attree P. Growing up in disadvantage: a systematic review of the qualitative evidence. Child Care Health Dev 2004; 30: 679-899.
- 21. Ring IT, Firman D. Reducing indigenous mortality in Australia: lessons learnt from other countries. Med J Aust 1998; 169: 528-533. <eMJA full text>
- 22. Henry BR, Houston S, Mooney G. Institutional racism in Australian healthcare: a plea for decency. Med J Aust 2004; 180: 517-520. <MJA full text>
- 23. Stewart-Brown S. Legislation on smacking [editorial]. BMJ 2004; 329: 1195-1196.
- 24. Webb E. Discrimination against children. Arch Dis Child 2004; 89: 804-808.
- 25. Sloper P, Lightfoot J. Involving disabled and chronically ill children and young people in health service development. Child Care Health Dev 2003; 29: 15-20.
- 26. NSW Commission for Children & Young People. What we’re doing. Ask the children. Available at: www.kids.nsw.gov.au/ourwork/ask.html (accessed Mar 2005).
- 27. Sanz EJ. Concordance and children’s use of medicines. BMJ 2003; 327: 858-860.
- 28. Pridmore P, Stephens D. Children as partners for health: a critical review of the child-to-child approach. London: Zed Books, 2000.
- 29. Centre for Community Child Health. A review of early childhood literature. Prepared for the Department of Family and Community Services as a background paper for the National Families Strategy. Canberra: Department of Family and Community Services, 2000. Available at: www.facs.gov.au/internet/facsinternet.nsf/vIA/families/$file/early_childhood.pdf (accessed Jul 2005).
- 30. National Public Health Partnership. Work program. Available at: www.nphp.gov.au/ (accessed Jul 2005).
- 31. Vinson V, Baldry E. Spatial clustering of child maltreatment: are micro-social environments involved? Canberra: Australian Institute of Criminology. Trends and Issues in Crime and Criminal Justice, 1999: 1-6. Available at: www.aic.gov.au/conferences/children/baldry.html (accessed Jul 2005).
- 32. Morrell S, Page A, Taylor R. Unemployment and youth suicide. Economic and Labour Relations Review 2001; 12: 4-17.
- 33. Australian Government. National Drug Strategic Framework. Available at: www.nationaldrugstrategy.gov.au/framework/ (accessed Jul 2005).
- 34. Eat Well Australia: an agenda for action for public health nutrition, 2000-2010. Available at: www.nphp.gov.au/publications/signal/eatwell1.pdf (accessed Jul 2005).
- 35. National ATSI Nutrition Strategy and Action Plan. Available at: www.nphp.gov.au/workprog/signal/nutstrat.htm (accessed Jul 2005).
- 36. National Strategic Framework for Aboriginal and Torres Strait Islander Health. Available at: www.health.gov.au/internet/wcms/publishing.nsf/ Content/health-oatsih-pubs-healthstrategy.htm (accessed Jul 2005).
- 37. Draft National Injury Prevention Plan: 2004 Onwards. Available at: www.nphp.gov.au/workprog/sipp/documents/draftnipp_190804.pdf (accessed Jul 2005).
- 38. Towards the Development of a National Agenda for Early Childhood. Available at: www.facs.gov.au/internet/facsinternet.nsf/ family/early_childhood.htm (accessed Jul 2005).
- 39. Immunise Australia Program. Available at: www.immunise.health.gov.au (accessed Nov 2004).
- 40. National Asthma Council. Available at: www.nationalasthma.org.au (accessed Jul 2005).
- 41. Healthy Weight 2008 — Australia’s Future. The national action agenda for children and young people and their families. Available at: www.healthyactive.gov.au/docs/healthy_weight08.pdf (accessed Jul 2005).
- 42. National Mental Health Plan 2003-2008. Available at: www.health.gov.au/internet/wcms/publishing.nsf/Content/mentalhealth-mhinfo-nmhs-2003.htm (accessed Jul 2005).
- 43. Stanley F. From Susser’s causal paradigms to social justice in Australia? Int J Epidemiol 2002; 31: 40-45.
- 44. Stronger Families and Communities Strategy 2004-2008: communities for children. Available at: http://www.facs.gov.au/internet/facsinternet.nsf/aboutfacs/programs/sfsc-communities_for_children_invitation.htm (accessed Mar 2005).
- 45. Cabinet Office. Families First. A NSW Government initiative. A support network for raising children. Sydney: Office of Children and Young People, 1999. Available at: www.familiesfirst.nsw.gov.au (accessed Jul 2005).
- 46. Families First Outcomes Evaluation Framework. For the Cabinet Office of New South Wales. University of New South Wales Research Consortium, March 2002. Available at: www.sprc.unsw.edu.au/reports/Families_First_Outcomes_EvalFramework.pdf (accessed Nov 2004).
- 47. Olds DL, Eckenrode J, Henderson CR, et al. Long term effects of home visitation on maternal life course and child abuse and neglect: fifteen-year follow-up of a randomized trial. JAMA 1997; 278: 637-643.
- 48. Olds, DL, Robinson J, O’Brien R, et al. Home visiting by paraprofessionals and by nurses: a randomized controlled trial. Pediatrics 2002; 110: 486-496.
- 49. Boocock SS. Early childhood programs in other nations — goals and outcomes. Future Child 1995; 5: 94-114.
- 50. The High/Scope Educational Research Foundation. Lifetime Effects: the High/Scope Perry Preschool Study Through Age 40. Available at: www.highscope.org/Research/PerryProject/perrymain.htm (accessed Jul 2005).
- 51. Sanders MR, Markie-Dadds C, Tully LA, Bor W. The triple P – positive parenting program: a comparison of enhanced, standard and self-directed behavioral family intervention for parents of children with early onset conduct problems. J Consult Clin Psychol 2000; 68: 624-640.
- 52. Gilliam WS, Zigler EF. A critical meta-analysis of all evaluations of state-funded preschool from 1997 to 1998: implications for policy, service delivery and program evaluation. Yale University Child Study Center. Early Child Res Q 2001; 15: 441-473.
- 53. Barnett WS, Hustedt JT. Head Start’s lasting benefits. Infants Young Child 2005; 18: 16-24.
- 54. Olds D, Pettitt L, Hiatt S, et al (author reply to: Home visiting by Guterman NB, Anisfeld E, McCord M). Pediatrics 2003; 111: 1491-1494.
- 55. Meltzer H, Gatward R, Goodman R, Ford T. Mental health of children and adolescents in Great Britain. Int Rev Psychiatry 2003; 15: 185-187.
- 56. Roberts I, Kramer MS, Suissa S. Does home visiting prevent childhood injury? A systematic review of randomized controlled trials. BMJ 1996; 312: 29-33.
- 57. Resnick MD, Bearman PS, Blum RW, et al. Protecting adolescents from harm: findings from the National Longitudinal Study on Adolescent Health. JAMA 1997; 278: 823-832.
- 58. National Health and Medical Research Council. How to use the evidence: assessment and application of scientific evidence. Handbook series on preparing clinical practice guidelines. Table 1.3: Designation of levels of evidence. Canberra: NHMRC, February 2000: 8. Available at: http://www.nhmrc.gov.au/publications/synopses/cp65syn.htm (accessed Jun 2005)





Abstract
Although children in Australia generally have good health, some alarming indicators of poor health and wellbeing exist, which are related to major socioeconomic discrepancies.
The pathways connecting socioeconomic disadvantage to child health outcomes are complex and poorly understood.
Reducing social disadvantage requires strategies beyond the health arena, involving political, moral, cultural and economic initiatives.
Developing “social capital” — cohesion in communities, a sense of belonging and involvement in community affairs — may be a key strategy in improving health indicators.
Overseas studies of early intervention and home visiting programs in early childhood have shown improvements in child health and development outcomes. Similar programs have been introduced in Australia and face considerable challenges in their widespread roll-out and evaluation.
Health professionals need to develop practical ways to interact with community programs and thus improve social capital.