Australia has a high prevalence of asthma by international standards. The most recent national data are that 14%–16% of children and 10%–12% of adults have a diagnosis of asthma that remains a current problem.1 There has been a focus on asthma care through the six-step Australian Asthma Management Plan, first published more than a decade ago,2 and widely disseminated to general practitioners through the work of the National Asthma Council (NAC). This work has included publishing the Asthma management handbook3 and proformas for written asthma action plans.
Funding was announced in the 2001 federal budget for a general practice asthma initiative through the Practice Incentives Program (PIP) to support improved asthma care and use of the Australian Asthma Management Plan. The funding ($22.7 million over 4 years for general practice aspects) supports GPs implementing the Asthma 3+ Visit Plan developed by the NAC’s General Practitioners Asthma Group.4 The Asthma 3+ Visit Plan introduces a “contract for care” between GPs and patients with asthma, which includes plans for regular review of asthma symptoms and treatment.
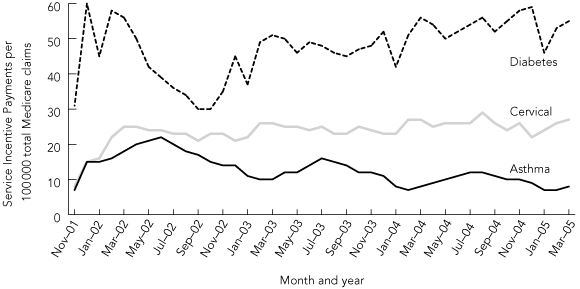
The proportion of practices signed up for diabetes and cervical screening incentives has followed a very similar pattern. However, claims for the SIP-asthma have been declining compared with cervical screening and diabetes SIP claims (Box 1).
Of the 147 responding GPs, 134 (91.2%) were aware of the Asthma 3+ Visit Plan and 66 (44.9%) had used the plan in their practice. Younger GPs, vocationally registered GPs, those in group versus solo practice, and those in practices with a nurse more frequently reported having used the Asthma 3+ Visit Plan, but the impact of none of these factors was statistically significant. There was a direct relationship between use of the six-step Australian Asthma Management Plan and use of the Asthma 3+ Visit Plan. Of the GPs who used the six-step plan, 55 (54.5%) had used Asthma 3+ compared with 8 (20.0%) who had never used the six-step plan (χ21 = 13.8; P < 0.05).
A high level of confidence in certain aspects of asthma care was associated with use of the Asthma 3+ Visit Plan (Box 2).
Certain characteristics of the practices where GPs worked had some bearing on their use of the Asthma 3+ Visit Plan, as shown in Box 3.
There is evidence that proactive care, combined with written asthma action plans and training in self-management, improves outcomes for adults with asthma.6 The Asthma 3+ Visit Plan has not been the subject of controlled evaluation in adults, but the impact of the plan has been examined in a cluster randomised trial in children.7 This study found an increase in asthma-related consultations, written asthma action plans and completed Asthma 3+ Visit Plans in the intervention group. The study also provided evidence of better asthma control, with smaller reductions in FEV1 (forced expiratory volume in 1 second) after cold air challenge, fewer emergency department attendances for asthma, and less speech-limiting wheeze in the intervention compared with the control group. Furthermore, the study reported that the delivery of interventions was variable, with only 28% of children in the intervention group actually completing the Asthma 3+ Visit Plan and another 20% partially completing it.
Thus, the Asthma 3+ Visit Plan can improve asthma care, but completing the plan is problematic, even in a clinical trial setting. For the plan and the incentives that support it to be effective, there needs to be participation all round, with the practitioner and practice needing to adapt to this organised approach, and patients needing to be willing to complete the contracted visits and make the necessary self-management changes to improve control of their asthma. The HIC data shown in Box 1 suggest that achieving all this is proving difficult, with a lower and declining number of claims for the GP asthma incentive compared with the diabetes and cervical screening incentives.
Our study shows that although there is a high level of awareness and a substantial number of GPs have used the Asthma 3+ Visit Plan, the workload and paperwork, and the perceived administrative burden of the incentive are seen as major barriers to implementation. This appears to be an example of where “red tape” associated with an incentive payment is detracting from the value of the program, and raises the question of whether there is a limit to the number of single-condition incentive programs that can be sustained in general practice. The administrative burden of incentive programs has been the subject of debate,8 and our findings provide further evidence that administrative bureaucracy is a barrier to the success of such programs. Simplifying the administrative requirements, and having a more integrated chronic disease incentive program that includes a number of conditions, should be considered.
1 Service Incentive Payment claims made by general practitioners in Australia for Asthma 3+, diabetes and cervical screening from November 2001 to March 2005
2 Use of the Asthma 3+ Visit Plan by general practitioners confident or extremely confident in aspects of asthma care
Assessing asthma in patients with chronic obstructive pulmonary disease |
|||||||||||||||
Knowing when to use EPC and when to use the Asthma 3+ Visit Plan |
|||||||||||||||
3 Practice factors and use of the Asthma 3+ Visit Plan
Signed up for asthma Practice Incentives Program/Service Incentive Payment |
|||||||||||||||
Received 11 January 2005, accepted 10 May 2005
- Nicholas A Zwar1
- Iqbal Hasan2
- Elizabeth J Comino3
- Mark F Harris4
- 1 General Practice Unit, Fairfield Hospital, Sydney, NSW.
- 2 School of Public Health & Community Medicine, University of New South Wales, Sydney, NSW.
We acknowedge support from the Primary Health Care Research Network (PHReNet), which is a research-capacity-building activity of the University of New South Wales with funding from the Australian Government Department of Health and Ageing. We also thank PHReNet member GPs Olataga Doorbinnia, Hani Bittar, Judit Gonczi, Peter Edwards, Regina Greenwood, Ven Tan, Phillip Lye, and Huy An, who contributed to survey design and piloting.
None identified.
- 1. Australian Centre for Asthma Monitoring. Asthma in Australia 2003. Australian Institute of Health and Welfare Asthma Series 1. Canberra: AIHW, 2003. (AIHW Catalogue No. ACM 1.)
- 2. Woolcock A, Rubinfeld AR, Seale JP, et al. Asthma management plan, 1989. Med J Aust 1989; 151: 650-653.
- 3. National Asthma Council. Asthma management handbook. Revised and updated 2002. Melbourne: National Asthma Campaign, 2002.
- 4. Fardy HJ. Moving towards organised care of chronic disease. The 3+ visit plan. Aust Fam Physician 2001; 30: 121-125.
- 5. HIC Health Statistics. Available at: http://www.hic.gov.au/statistics/imd/forms/gpStatistics.shtml (accessed Jun 2005).
- 6. Gibson PG, Powell H, Coughlan J, et al. Self-management education and regular practitioner review for adults with asthma. Cochrane Database Syst Rev 2002; (3): CD001117.
- 7. Glasgow NJ, Ponsonby A, Yates R, et al. Proactive asthma care in childhood: general practice based randomised trial. BMJ 2003; 327: 659.
- 8. Chew M. Battling red tape [editorial]. Med J Aust 2004; 181: 60. <MJA full text>





Abstract
Aim: The Asthma 3+ Visit Plan is an initiative to promote organised asthma care in general practice. This study aimed to identify factors associated with uptake of the plan by general practitioners, and their views on barriers and facilitators to implementation of the plan.
Design: Postal survey sent to a random sample of GPs.
Participants and setting: 315 GPs in five Divisions of General Practice in metropolitan Sydney, surveyed sequentially between 1 October 2002 and 31 May 2003.
Outcome measures: Awareness and use of the Asthma 3+ Visit Plan; GP and practice factors associated with use of the plan; and GP views on barriers and facilitators to implementing the plan.
Results: The response rate was 55.7%, and 72.1% of participants were male; participants’ mean age was 50.5 years. Most GPs (91.2%) were aware of the plan and and 44.9% had used it. GP and practice factors associated with use of the plan were use of the six-step Australian Asthma Management Plan, confidence in aspects of asthma care, practice accreditation, sign-up for asthma incentives, and computerisation. Major barriers to implementing the plan were workload/paperwork and administrative complexities. Patient factors that influenced completion of the plan were their concept of the severity of their asthma, compliance with follow-up, and patient attitudes towards asthma care.
Conclusion: The perceived workload and administrative complexity of the asthma incentives are barriers to uptake. Factors relating to the illness rather than social factors are seen as the most important influences on completion of the plan by patients.