Aboriginal mental health policy requires that services should be provided through Aboriginal and mainstream health service partnerships that build the capacity of Aboriginal health workers in mental health.1-4 The Regional Aboriginal Integrated Social and Emotional (RAISE) Wellbeing program in the Northern and Far Western region of South Australia complies with this policy through a service partnership between the Aboriginal Health Service (Pika Wiya) and three mainstream health services: a community mental health team, a hospital mental health liaison, and an “outback” community counselling service. The program commenced in February 2003 and aims to improve mental health services to Aboriginal people by linking workers across these organisations. Recurrent funds include $70 000 from the SA Department of Health and $10 000 from the Northern and Far Western Regional Health Service, and a one-off project allocation of $80 000. A partnership development project officer and a regional social and emotional wellbeing program manager (Aboriginal mental health) have been employed, and an existing Aboriginal mental health worker’s employment has been increased from half-time to full-time. The mainstream Regional Health Service and the Aboriginal Health Service have provided other staffing and service support and infrastructure. The Northern and Far Western Regional Health Service administers the program funds, the staff funded by the program work from the Aboriginal Health Service, and governance is through a joint-organisation management committee.
These were identified as known problems of access to care, policy direction favouring shared service responsibility (as mentioned above) and, in the past few years, allocation of some additional resources for mental health. Problems with local Aboriginal people’s access to mental health care had been consistently reported for over 5 years, including a lack of mental health staff in the Aboriginal Health Service, mainstream service inflexibility, and inadequate service coordination particularly around discharge planning.5-7 An increase in funds to the region over recent years from the SA and federal health departments (for RAISE Wellbeing and other mental health programs) has provided resources for a service partnership to help solve the problem. New positions in the region include a regional mental health program manager, principal mental health clinician, staff psychiatrist, hospital mental health liaison nurse, partnership development project officer, Aboriginal mental health worker, and the staffing of an “outback” community counselling service with a mental health brief.
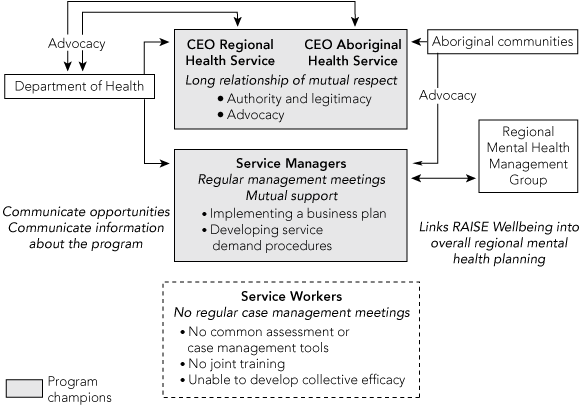
Linkage processes were the relationships between health service staff and the formal protocols and process for communication. The relationship between key individuals across the organisational hierarchy provided the foundation for the partnership (Box 1). The two chief executives in the region, from the Aboriginal Health Service and the Regional Health Service, respectively, who had been in their positions for some years, described their relationship as one of mutual respect. Along with service managers, they were seen as program champions who gave authority to the partnership and who acted as advocates with the local Aboriginal communities and with the SA Department of Health. The relationship between service managers and Department of Health policy officers was described as the communicating link with the central bureaucracy, so that opportunities such as future funding and support emanating from the central bureaucracy could be made known to the local program staff. However, a long vacancy in the position of Department of Health Aboriginal mental health policy officer created a “slow down” in this communication. This was evident in the local service managers’ uncertainty about to whom in the bureaucracy they should then channel their communications.
The service managers described their relationship as mutually supportive, which, along with their commitment to Aboriginal health, helped in implementing the program business plan. These managers meet formally to oversee the program and they also sit on a Regional Mental Health Program Management Group, which means that RAISE Wellbeing is linked into overall regional mental health planning. They have developed procedures to deal with crisis demands and staff shortages by resource sharing across the teams, and they are working on developing common culturally responsive mental health risk-assessment and care-management tools.
At the grass roots level the relationship between workers in the respective teams was considered important for collaborating on client care. It was at this level, however, that some early tension arose about the program focus and worker role. This manifested as concern from some in the community mental health team about a change in the project officer role (from linkage development to a focus on management of the mental health team in the Aboriginal Health Service) due to vacancies in that team. Hence, linkage developments slowed until an additional project officer was employed to work solely on these linkages and not on service delivery. There was also criticism from the Aboriginal Health Service that the community mental health team was inflexible and, conversely, there was concern from the community mental health team about the mental health knowledge and skill level of Aboriginal health workers.
The following linkage protocols have been or are being developed:
memoranda of understanding between the organisations;
a partnership business plan; and
an expectation written into job descriptions that staff will participate in partnership activities.
The intention is to eventually pool all the funds for Aboriginal mental health from the Aboriginal and mainstream mental health services, so that service delivery is provided mainly from the Aboriginal Health Service but with governance of the business plan retained by the interorganisation management group. As yet, however, there are no common processes for communicating about client care across the partnership. The Aboriginal Health Service mental health team (medical staff excepted) expressed concern that they are not allowed to write in the hospital case notes because they are not employees of the hospital and do not have hospital practice rights. Recent negotiations are addressing this. Also still to come are formal processes for developing partnership care plans or conducting case reviews for quality assurance, and as yet there has been no cross-cultural mental health training for staff. Most discussion about client matters has occurred on an as-needed and informal basis. Management and policy officer informants wanted more regular and structured communication between staff from the four organisations, so that care protocols would then evolve. These protocols are important because, as one policy officer put it — from a low capacity base in Aboriginal mental health, it is unrealistic to expect that organisational change and service improvement will simply come about “osmotically” by employing staff in partnership positions.
The factors limiting sustainability were recognised as inadequate data about the program and the time required for a service innovation to become established practice. The positive factors were the fit of the program with current policy and organisational plans, as well as the linkage processes in place (described in the previous section).
Informants commented that program and client data were important for communicating progress among the partners, for identifying where program changes were required, and for managers communicating this information to the Department of Health (source of funds). One policy officer’s advice was that the political decision to continue funding required the value of the program to be visible; that is, it had to be seen to address government Aboriginal mental health priorities. This was a problem, as managers had very few data in a form that was useful for planning or to demonstrate the value of the program. Information was available on client use within each service, but none that would quantify client work across organisations in the partnership.
Although RAISE Wellbeing has been funded at a modest level for over 2 years, progress has been from a low base with interruptions mainly caused by staff vacancies. Service system changes have yet to be adequately developed and embedded. A similar project reported that up to 4 years were required simply to establish the relationship processes for effective collaboration.8 More generally, 5 years is considered to be the time required to ensure the sustainability of health program interventions.9 The positive indicators for sustainability are that the program sits well with the mission of the partner organisations, it has local management champions, and it adds onto existing programs.10,11 Facilitating and inhibiting factors for sustainability are listed in Box 2.
Driving the establishment of the program was the positive policy context for collaboration, the consistent reporting of service access problems, and new resources for mental health. The improved mental health staffing in the region meant that there was capacity for a service partnership, and the linkage processes enabled this partnership to develop. Relationships at the executive and senior management levels provided stability at the top, gave the partnership legitimacy, and provided a link to the Department of Health (while there was an Aboriginal mental health policy officer), so that there was Departmental understanding of the local program. Meetings between service managers enabled the development of a business plan and procedures to deal with service demand.
On the deficit side, common mental health assessment and care-management tools that would provide linkages in mental health care have not been developed. This is partly because regular case-management meetings and training for service staff have not occurred. However, it would be unrealistic to expect that these could solely be developed locally when interorganisational care-management tools and training in Aboriginal mental health do not exist nationally. The reliance, in part, on time-limited project funds has left the program with an uncertain resource future. The lack of data available to managers has compromised their ability to convince decision makers that the program is an effective strategy for dealing with an urgent problem. These data could also provide reinforcement to the partners about whether their strategies were proving successful.12 It was not simply the fault of the program that it could not do these things, but rather the time delays in recruiting staff in rural locations, the lack of good community mental health data systems across organisations generally, and the longer time that seed funding is required for such programs to become operational.13,14
In addition to the threat posed by resource uncertainty, two internal threats appear relevant to the sustainability of RAISE Wellbeing. These are (i) the capacity to maintain focus, and (ii) the extent to which partnership members collectively agree on the legitimacy of the program goals and have confidence in each other’s skills (collective efficacy).15 Partnerships work when there is a defined team focus, a common approach, goal predictability, role clarity and respect.16,17 In rural and cross-cultural work, role ambiguity is more the norm, with a generalist approach as workers cross role boundaries out of need.18-20
With vulnerable communities, service focus can be driven by crisis response to profound needs that are often immediate and often not predictable.15 Long-term goals can be put on hold as crises are dealt with, such as occurred with the change in project officer focus to service management. Organisational partnerships have been found to work best when they have a structure and processes through which to reach agreement about treatment goals and approaches.14,21 The RAISE Wellbeing partners have so far relied heavily on staff relationships. At the level of service staff, more regular and structured communication, as well as joint training in cross-cultural mental health care, would enable these staff to test their level of agreement (collective efficacy) about common care-management tools, and then “road test” practice over time to determine what additional service improvements could be negotiated.
Cross-cultural programs often employ staff from the target community because of their knowledge and skills in working with that community. These staff often have a different set of skills and level of training compared with discipline-based health workers, and this can lead to an uncertainty about each person’s role and a lack of confidence in each person’s skills, which we found early on in the program.22,23 It is here that on-the-job training could facilitate role clarification and teamwork through reflective practice (Box 3).
This RAISE Wellbeing program case study generated in-depth information about sustaining one Aboriginal mental health service partnership. While the case study method limits generalisability, the use of an expert research advisory committee and interviews with SA policy officers provided broader input that covered more than just this program. Although both interpersonal and formal relationships between stakeholders were found to be necessary, they were not sufficient to develop and sustain the program. Of wider relevance to policy and other locations are the need for (i) agreed care-management processes and training in cross-cultural mental health to develop a sense of collective efficacy, and (ii) the effective use of data to communicate the value of a program both internally and externally.
2 Facilitators and inhibitors of sustainability of the RAISE Wellbeing program
Facilitators |
Inhibitors |
||||||||||||||
|
|
||||||||||||||
3 Responsive mental health care through reflective practice
The mental health worker referred a 28-year-old Aboriginal man to the psychiatrist for management of his psychotic episodes, but twice he failed to attend. An Aboriginal health worker was asked to assist when the client next saw the mental health worker. This time a more detailed assessment was completed that involved a reflective team-based approach with the client and his partner.
The client’s psychotic episodes were associated with heavy drinking. Over a few sessions, the mental health worker tried to advise him to reduce his drinking. This advice was not easily accepted either by the client or the Aboriginal health worker, who both felt that he could not simply be told to stop drinking with his family and mates. Discussion within the team revealed an obligatory element to the client’s drinking, and that, by refusing, he could be ostracised, which he saw as a worse outcome than the psychosis.
This challenged the mental health worker to take a wider perspective, recognising the additional loss and grief of being ostracised, which made reliance on only giving advice to the client an inadequate response. Although the problem was not yet solved, the mental health worker gained an understanding of the cultural and community-related issues, and the Aboriginal health worker learnt more about comorbidity between alcohol dependence and mental illness. The changed approach to mental health care included the following:
A proactive and reflective team-based approach to keep the client in health care.
A family-based and collaborative approach to maximise input rather than focus on the individual.
A responsive approach to the social function of the client’s behaviour.
- Jeffrey D Fuller1
- Lee Martinez1
- Kuda Muyambi1
- ; Kathy Verran1
- Bronwyn Ryan1
- Ruth Klee1
- 1 Northern Rivers University Department of Rural Health, University of Sydney, Lismore, NSW.
- 2 Spencer Gulf Rural Health School, University of South Australia, Whyalla Campus, Whyalla Norrie, SA.
- 3 Northern and Far Western Regional Health Service, Pt Augusta, SA.
Other members of the Research Advisory Committee were Cephas Stanley (Chief Executive Officer, Pika Wiya Health Service), Daniel MacKenzie (Coordinator, Flinders and Outback Regional Health Service), Kathryn Cronin (Mental Health Liaison, Pt Augusta Hospital), Harold Stewart (Senior Project Officer, Aboriginal Health Division, South Australian Department of Health), Dana Shen (Manager Aboriginal Programs, Country Division, South Australian Department of Health), and Alwyn Chong (Research and Ethics Officer, Aboriginal Health Council of South Australia). James Stanley provided administrative and research assistance. The study was funded by a research grant from the Australian Primary Health Care Research Institute of the Australian National University.
None identified.
- 1. Swan P, Raphael B. Ways forward. National consultancy report on Aboriginal and Torres Strait Islander mental health. Canberra: AGPS, 1995.
- 2. Office for Aboriginal and Torres Strait Islander Health. Social and emotional well being framework: a national strategic framework for Aboriginal and Torres Strait Islander mental health and social and emotional well being (2004-2009). Canberra: Australian Government Department of Health and Ageing, 2004 (draft).
- 3. Northern and Far Western Regional Health Service. Regional Mental Health Plan 2001-2004. Port Augusta, SA: Northern and Far Western Regional Health Service, 2001.
- 4. South Australian Aboriginal Health Partnership, Aboriginal health — everybody's business. Social and emotional wellbeing. A South Australian Strategy for Aboriginal and Torres Strait Islander People 2005-2010. Adelaide: Department of Health, 2005. Available at: https://www.library.health.sa.gov.au/Portals/0/social-and-emotional-wellbeing.pdf (accessed Oct 2005).
- 5. Pika Wiya Health Service. Social and emotional wellbeing. Seminar proceedings; 1999 August 9-10. Pt Augusta, SA: Pika Wiya Health Service, 1999.
- 6. Clark Y, Stewart T. A focussed step toward wellness and wellbeing in Aboriginal health. A state strategy and action plan for social and emotional wellbeing for Aboriginal people. Adelaide: South Australian Aboriginal Health Partnership, 2000.
- 7. Kowanko I, Crespigny C de, Murray H, Groenkjaer M. Better medication management for Aboriginal people with mental disorders and their carers. Bedford Park, SA: Flinders University School of Nursing and Midwifery and Aboriginal Drug and Alcohol Council (SA), 2003.
- 8. Salisbury C. A health service and Aboriginal and Torres Strait Islander partnership to develop and plan mental health services. Aust J Prim Health Interchange 1998; 4: 18-30.
- 9. Shediac-Rizkallah M, Bone L. Planning for the sustainability of community-based health programs: conceptual frameworks and future directions for research, practice and policy. Health Educ Res 1998; 13: 87-108.
- 10. Villeneau L, Hill R, Hancock M, Wolf J. Establishing process indicators for joint working in mental health: rationale and results from a national survey. J Interprof Care 2001; 15: 329-340.
- 11. Thompson B, Winner C. Durability of community intervention programs. In: Bracht N, editor. Health promotion at the community level. New advances. 2nd ed. Thousand Oaks, Calif: Sage Publications, 1999: 137-154.
- 12. Cockburn J. Adoption of evidence into practice: can change be sustainable? Med J Aust 2004; 180 (6 Suppl): S66-S67. <MJA full text>
- 13. Mak D, Straton J. Effects and sustainability of a cervical screening program in remote Aboriginal Australia. Aust N Z J Public Health 1997; 21: 67-70.
- 14. Swerissen H, Crisp B. The sustainability of health promotion interventions for different levels of social organization. Health Promot Int 2004; 19:123-130.
- 15. Johnson P, Wistow G, Schulz R, Hardy B. Interagency and interprofessional collaboration in community care: the interdependence of structures and values. J Interprof Care 2003; 17: 69-83.
- 16. Gibb CE, Morrow M, Clarke CL, et al. Transdisciplinary working: evaluating the development of health and social care provision in mental health. J Ment Health 2002; 11: 339-350.
- 17. Norman IJ, Peck E. Working together in adult community mental health services: an interprofessional dialogue. J Ment Health 1999; 8: 217-230.
- 18. Wilkinson D, Blue I, editors. The new rural health. Melbourne: Oxford University Press, 2002.
- 19. Dollard J, Stewart T, Fuller J, Blue I. Aboriginal Health Worker status in South Australia. Aboriginal and Islander Health Worker Journal 2001; 25: 28-30.
- 20. Fuller J. Community expectation of ethnic health workers: implications for best practice. Aust J Prim Health Interchange 1996; 2: 61-73.
- 21. Hoge M, Howenstine R. Organizational development strategies for integrating mental health services. Community Ment Health J 1997; 33: 175-188.
- 22. Mignore B, Boone M. Realizing potential: improving interdisciplinary professional/paraprofessional health care teams in Canada’s northern aboriginal communities through education. J Interprof Care 2002; 16: 139-147.
- 23. Fuller J. Challenging old notions of professionalism: how can nurses work with paraprofessional ethnic health workers? J Adv Nurs 1995; 22: 465-472.





Abstract
The Regional Aboriginal Integrated Social and Emotional (RAISE) Wellbeing program commenced in February 2003 as an Aboriginal mental health service partnership between one Aboriginal Health Service and three mainstream services: a community mental health team, a hospital mental health liaison, and an “outback” community counselling service.
A case study method was used to describe the drivers (incentives for program development), linkage processes (structures and activities through which the partnership operated), and sustainability of the program.
Program drivers were longstanding problems with Aboriginal peoples’ access to mental health care, policy direction favouring shared service responsibility, and a relatively small amount of new funding for mental health that allowed the program to commence.
Linkage processes were the important personal relationships between key individuals. Developing the program as a part of routine practice within and across the partner organisations is now needed through formal agreements, common care-management tools, and training.
The program’s sustainability will depend on this development occurring, as well as better collection and use of data to communicate the value of the program and support calls for adequate recurrent funds. The development of care-management tools, training and data systems will require a longer period of start-up funding as well as some external expertise.