Asthma is common in older people; they may have had asthma as children, or it may first occur when they are older.1Asthma in older people may be associated with severe symptoms and chronic airway obstruction,2 resulting in significant functional limitations. Furthermore, older people with asthma have higher death rates than their peers.2 However, diagnosis of asthma in older people is not easy, and misdiagnosis can occur.3 Factors making the diagnosis more difficult may include comorbid conditions,1,4 cognitive or sensory impairment,5 polypharmacy,6 or lack of recognition of respiratory symptoms as asthma.
The emphasis in published reports about asthma has been on the misdiagnosis of asthma, especially in older people.2,4,6 There is also some recognition that asthma may be underdiagnosed in older people,4 and that many people with moderate or severe persistent asthma symptoms may be missing out on the benefits of effective treatment.4
We used the Northwest Adelaide Health (Cohort) Study (NWAHS) to identify the prevalence and characteristics of undiagnosed asthma in a representative population sample of older people.
Households in the north-west region of Adelaide were selected at random from the Electronic White Pages telephone directory and contacted using computer-assisted telephone interview methods. Within each household a person was selected at random and up to five call-backs were made to recruit the person selected. A sample response rate of 62% was obtained for both the telephone interview and the clinical study, resulting in a study group of 4060 people.
The telephone interviewers enquired whether respondents had ever had asthma, whether the asthma had been diagnosed by a doctor, and whether they currently had asthma. A positive response to all three questions confirmed self-reported doctor-diagnosed asthma. In addition, respondents were asked about health service use (hospital emergency visits and general practitioner visits); smoking status (current and ex-smoker); exercise (150 minutes or more of walking or other moderate or vigorous activity each week); the person’s demographic characteristics (place of birth, highest education level, household income); and their health-related quality of life (assessed using the SF-36 health-related quality-of-life questionnaire). The Selim index for severity of chronic lung disease symptoms7 was also administered.
After interview, respondents were recruited to one of two area clinics for medical assessment of health status. This included spirometry, and measurement of height and weight, which was converted to body mass index (weight in kilograms divided by height in metres squared). A person with a body mass index equal to or greater than 30 kg/m2 was considered to be obese. All clinic participants were assessed as having asthma if their asthma was clinically reversible according to European Respiratory Society criteria,8 or they reported doctor-diagnosed current asthma. This group was then classified according to whether or not their asthma had been previously diagnosed by a doctor into “previously diagnosed” or “undiagnosed”.
Data were analysed using the Statistical Package for the Social Sciences, version 11 (SPSS Inc, Chicago, Ill, USA) and Epi Info 6 (Centers for Disease Control, Atlanta, Ga, USA). Mean quality-of-life scores were calculated for the physical components summary of the SF-36 health-related quality-of-life questionnaire. Standard SF-36 quality-of-life scores were also calculated by the method of Garrat et al9 for both the physical components summary and the mental components summary to produce standard scores. The mean values for the physical and mental components summary for the north-west Adelaide population were set at zero to allow comparisons with the population mean of the physical and mental health quality-of-life scores for subjects with “previously diagnosed” and “undiagnosed” asthma.
Univariate descriptive statistical methods were used to examine the differences between groups with previously diagnosed and undiagnosed asthma.
Box 1 shows that the overall prevalence of asthma in this region was 13.8%. A slightly higher prevalence was found in those 55 years or older (14.7%) compared with those under 55 years of age (13.6%). More than a third of the 55 years and older group had undiagnosed asthma, with almost 50% of older men having significant acute bronchodilator reversibility without a previous diagnosis of asthma or chronic obstructive pulmonary disease (COPD). Box 1 also shows that lung function results (forced expiratory volume in 1 second [FEV1]), pre- and post-bronchodilator, were better in the older undiagnosed group than in the diagnosed group, and that women had better lung function results than men.
The respondents’ answers to questions about health service use in the previous 12 months showed that both the diagnosed and undiagnosed asthma groups visited their general practitioner a mean number of 8.5 times, but the diagnosed group had a slightly higher mean number of hospital emergency visits (1.9) compared with the undiagnosed group (1.4). This difference was not statistically significant.
Box 2 shows how the diagnosed and undiagnosed groups compare on other health and demographic variables. For every variable the proportions for the undiagnosed group are lower; however, the only statistically significant variable is that of “current or ex-smoker”, with a higher proportion of current and ex-smokers in the diagnosed group.
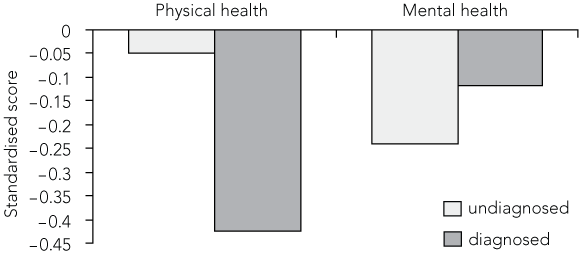
The score for the physical and mental components summary of the quality-of-life questionnaire was significantly lower for both groups compared with that for the general north-west Adelaide population. The score for the diagnosed group was also significantly lower than that for the undiagnosed group (P < 0.01) (Box 3).
Ten per cent of the undiagnosed group were categorised as having moderate-to-severe asthma symptoms on the Selim index,7 compared with a significantly higher 38% in the diagnosed group (χ2 = 22.6, 1 df, P < 0.0001).
In the subjects with undiagnosed asthma, lung function tests before and after bronchodilator suggest that significant improvements can be made in lung health. We need to know whether early identification of this group is possible, and whether medical care will improve health outcomes.
We also need to know whether appropriate strategies can be developed to raise awareness that respiratory symptoms may be due to asthma. It is important that the undiagnosed group consulted their GP as often as the diagnosed group (ie, they were known to the system but remained undiagnosed). Because of this anomaly, we need to know whether subjects in the undiagnosed group have discussed these symptoms with their doctor. If the answer is yes, we need to know whether GPs have been unable to diagnose asthma. Perhaps the symptoms of the undiagnosed subjects are less noticeable, either because they have reduced perception of bronchoconstriction or have voluntarily restricted their activities so that they do not report breathlessness.
For GPs, we need to know whether the potential for asthma in older people with respiratory symptoms is clearly established on their radar screen. In a recent focus group study in South Australia,10 where we identified these rates of undiagnosed asthma, considerable surprise was expressed that up to 50% of elderly people with asthma could be undiagnosed. GPs reported that knowing this would increase the vigilance of the profession towards the target group.
We also need to know why some GPs do not use spirometry in the diagnosis and management of airway obstruction. Is this a time and cost problem, a skill problem or are there additional factors that complicate innovation? It has been pointed out that spirometry is underutilised in general practice and may be a factor in underdiagnosis.11
1 Asthma prevalence and lung function (forced expiratory volume in 1 second [FEV1]) before and after bronchodilator by prior doctor-diagnosed status, age and sex (n = 3999)
Undiagnosed (n = 86) |
Diagnosed (n = 154) |
Total (n = 240) |
Undiagnosed (n = 96) |
Diagnosed (n = 224) |
Total (n = 320) |
Overall asthma prevalence (%) |
|||||||||
Men < 55 years (n = 1423) |
Women < 55 years (n = 1387) |
< 55 years (n = 2810) |
|||||||||||||
Asthma prevalence (%, 95% CI) |
3.3 (2.4–4.2) |
7.7 (6.4–8.0) |
11.0 (10.4–12.6) |
4.7 (3.6–5.8) |
11.5 (9.8–13.2) |
16.3 (14.4–18.2) |
13.6 (12.3–14.9) |
||||||||
Pre* FEV1 % predicted |
88.7 |
88.7 |
88.7 |
93.3 |
94.3 |
94.2 |
|
||||||||
Post* FEV1 % predicted |
101.1 |
93.7 |
96.0 |
104.7 |
100.0 |
101.4 |
|
||||||||
|
Men > 55 years (n = 540) |
Women > 55 years (n = 649) |
> 55 years (n = 1189) |
||||||||||||
Asthma prevalence (%, 95% CI) |
7.0 (4.9–7.1) |
8.0 (5.7–10.3) |
15.2 (13.2–17.2) |
4.8 (3.2–6.4) |
9.7 (7.7–11.3) |
14.6 (12.7–16.9) |
14.7 (12.7–16.7) |
||||||||
Pre* FEV1 % predicted |
79.0 |
73.3 |
75.9 |
83.4 |
84.8 |
84.3 |
|||||||||
Post* FEV1 % predicted |
91.2 |
78.2 |
84.2 |
96.9 |
90.2 |
92.4 |
|||||||||
* FEV1 was measured “pre” and “post” administration of 400 μg of a short-acting bronchodilator (salbutamol) administered via a metered-dose inhaler and large volume spacer. |
|||||||||||||||
2 Comparison of subjects with diagnosed and undiagnosed asthma by demographic and health-status variables
Variable |
Proportion |
Odds ratio |
P |
||||||||||||
Sex (diagnosed/undiagnosed) |
|
|
|||||||||||||
Male |
49.3% |
1.0 |
P = 0.67 |
||||||||||||
Female |
50.0% |
1.13 |
|
||||||||||||
Income ≤ $20 000 |
|
|
|
||||||||||||
Diagnosed |
51.4% |
1.0 |
P = 0.73 |
||||||||||||
Undiagnosed |
49.0% |
0.91 |
|
||||||||||||
Place of birth |
|
|
|
||||||||||||
Australia |
48.1% |
1.0 |
P = 0.47 |
||||||||||||
Elsewhere |
47.5% |
0.82 |
|
||||||||||||
Education post secondary school |
|
|
|||||||||||||
Diagnosed |
39.3% |
1.0 |
P = 0.70 |
||||||||||||
Undiagnosed |
36.6% |
0.89 |
|
||||||||||||
Smoker/ex-smoker |
|
|
|
||||||||||||
Diagnosed |
63.0% |
1.0 |
P = 0.01 |
||||||||||||
Undiagnosed |
45.5% |
0.49 |
|
||||||||||||
Obese |
|
|
|
||||||||||||
Diagnosed |
34.8% |
1.0 |
|
||||||||||||
Undiagnosed |
30.2% |
0.83 |
P = 0.52 |
||||||||||||
Exercise ≥ 150 min/week |
|
|
|
||||||||||||
Diagnosed |
48.1 |
1.0 |
P = 0.47 |
||||||||||||
Undiagnosed |
47.5 |
0.82 |
|
||||||||||||
- David H Wilson1
- Sarah L Appleton2
- Robert J Adams3
- Richard E Ruffin4
- Department of Medicine, University of Adelaide, Adelaide, SA.
Richard Ruffin has generated honoraria for Adelaide University from an article he wrote in Australian Doctor and from speaker’s fees for talks for GlaxoSmithKline and AstraZeneca. He has received research support from GlaxoSmithKline.
- 1. Frith PA. Asthma in the elderly. Curr Ther (Seaforth) 1999; 40: 19-31.
- 2. Burrows B, Barbee RA, Cline MG, et al. Characteristics of asthma among elderly adults in a sample of the general population. Chest 1991; 100: 935-942.
- 3. Enright PL, McLelland RL, Newman AB, et al. Underdiagnosis and undertreatment of asthma in the elderly. Cardiovascular Health Study Research Group. Chest 1999; 116: 603-613.
- 4. Pezzoli L, Giardini G, Consonni S, et al. Quality of spirometric performance in older people. Age Ageing 2003; 32: 43-46.
- 5. Kitch BT, Levy BD, Fanta CH. Late onset asthma. Epidemiology, diagnosis and treatment. Drugs Aging 2000; 17: 385-397.
- 6. Bellia V, Battaglia S, Catalano F, et al. Aging and disability affect misdiagnosis of COPD in elderly asthmatics: the SARA study. Chest 2003; 123: 1066-1072.
- 7. Selim AJ, Xinhua SR, Fincke G, et al. A symptom-based measure of the severity of chronic lung disease. Chest 1997; 111: 1607-1614.
- 8. Quanjer P. Lung volumes and forced ventilatory flows. Eur Respir J 1993; 6 (Suppl 16): 5-40.
- 9. Garrat AM, Ruta DA, Abdalla MI, et al. The SF-36 health survey questionnaire: an outcome measure suitable for routine use within the NHS. BMJ 1993; 306: 1440-1444.
- 10. Department of Medicine, Queen Elizabeth Hospital. General Practitioner Focus Group on Asthma in the Older Person. Adelaide, Queen Elizabeth Hospital, 2004.
- 11. McIvor RA, Tashkin DP. Underdiagnosis of chronic obstructive pulmonary disease. A rational for spirometry as a screening tool. Can Respir J 2001; 8: 153-158.





Abstract
What we need to know
Are older people with respiratory symptoms aware this could be asthma?
Which explanations for undiagnosed asthma apply most commonly in older Australians with asthma?
Can we improve awareness of asthma in older people with undiagnosed asthma?
Is the possibility of asthma in older people firmly established on the general practitioners’ radar screen?
What reasons most often determine whether GPs perform spirometry in their practice?
What we need to do
Conduct a representative population study to assess whether older Australians recognise respiratory symptoms as being asthma and are reporting these symptoms.
Conduct and evaluate a pilot asthma health promotion program for older people.
Conduct a controlled therapeutic trial of people with undiagnosed asthma to assess treatment benefits and produce treatment recommendations.
Identify whether the prominence of asthma in older people can be brought to the attention of GPs.
Analyse more carefully the issues associated with innovation of office spirometry.