Detailed history taking and observation leads to diagnosis
Parenting should be one of life’s enriching experiences, but for some parents it is frustrating, exhausting and disappointing. Puzzled and distressed by their child’s behaviour, they may turn to their general practitioner for help.1 Often the behaviour needs to be understood as a variation of normal — temper tantrums in 2–3 year olds or resistance to parental rules in 14 year olds — but for a significant number the “difficult behaviour” is a symptom of an underlying issue to be identified and addressed. According to Australian studies, some 18% of children have a significant social and emotional problem needing professional help; a conservative 10% of children struggle with learning difficulties; and a further 5%–8% experience one of the forms of attention deficit disorder. These problems are generally more common in boys, with a ratio of 3–4 : 1.2 Increasingly, parents are asking for help with unravelling such issues, a task which can require additional skills and resources.
Consider the following clinical scenario:
Jack is an 8 year old. His parents describe how they first sought help when their son was 4 years old. At that time, his main problem seemed to be overexuberance. He would throw himself onto furniture and people when he was overexcited. Some foods, noise and television seemed to make him worse. He needed guidance to start tasks as well as to complete them, and both his family and his kindergarten teachers thought that he was underachieving. He tended to avoid fine motor skills, particularly drawing and writing, and seemed to have difficulty managing Lego blocks. He found it hard to socialise appropriately with other children, and would sometimes have outbursts of temper, particularly when thwarted, and would cry frequently. Initially, his parents were given behavioural advice and Jack was engaged in an occupational therapy program to help with fine motor and perceptual skills.
Now, at the age of 8 years, his parents report that the situation worsened when he started school, with teachers in Year 1 and Year 2 finding that he could not settle to complete tasks, and needed prompting to stay focused. His teachers suspect that he is much more able than others in his year, but he is continuing to underachieve and still experiences problems with socialisation. He is very interested in geography and world political events. His parents also mention that they are concerned because he seems to be developing facial and shoulder girdle twitching.
The possible diagnoses are manifold! — attention deficit hyperactivity disorder (ADHD); conduct disorder or oppositional defiance disorder; learning disability; anxiety and/or depression; abuse; attachment disorder; autism; gifted and talented; tic disorder.
In general, behavioural disorders can be considered as emotional (anxiety, depression, obsessive–compulsive disorder), disruptive (oppositional defiance disorder, conduct disorder, ADHD) or developmental (speech/language delay, reading delay, autistic spectrum disorders, intellectual disability).3
Detailed history taking as well as observation of a child’s appearance and performance provides most of the information needed for diagnosing behavioural problems.
General medical history: Ask the parents about pre-, peri- and postnatal events, and the child’s general health and medical history, noting particularly any history of seizures and any medications used.
Developmental history: It is essential to know what is normal. The Stycar Chart of Developmental Sequences provides a helpful summary of developmental stages.4,5 Some of the key reassuring features of normal development are summarised in Box 1, and indications of possible developmental difficulties are summarised in Box 2.5 Note especially the age of social smiling, whether the child pointed to items of interest, language use and the age of meaningful words and phrases, and the time and nature of play, particularly pretend play, and play that includes other people. Difficulties in these domains are suggestive of autistic spectrum disorder. It is also useful to enquire about the child’s ability to follow instructions and complete tasks, as in learning and attentional problems.
Family history: Take into consideration the parents’ relationship (single, separated, de facto or married), the family size and “blend” (ie, family arrangements after remarriage), the family’s socioeconomic circumstances, the parents’ level of education and whether one or both parents are employed. What is their parenting style? Has the family always lived in the same place or moved around?
Determine whether learning difficulties have been experienced by family members, as there is frequently a genetic basis to learning difficulties.6,7 Postnatal depression or other mental health problems in the family can interfere with secure attachment and the subsequent development of self-regulation and language.8-10 Parental separation or divorce frequently causes distress, confusion and disruption, especially if associated with conflict and access disputes. Domestic violence or drug and alcohol abuse, even if passively observed, can adversely affect emotional security.11,12
Social history: Consider the child’s social engagement with friends and peers, interest in people, and history of aggression or experience of being bullied. Aggression in early childhood can lead to antisocial behaviour at school.12-14
Education history: Ask about the child’s experience and performance from child care onwards through to kindergarten, preschool, and each year of primary school. Note the attainments in reading, spelling and mathematics, as well as attention to tasks and work completion. Bullying by peers or teachers is regretfully common, and the fear and anxiety engendered can interfere with learning.15-17
Emotional history: Note mood, eating and sleeping habits, interests and activities. There is growing evidence of the importance of brain development, especially from the time of late pregnancy through to the first 3 years of life. Brain development is affected by an interplay of genetic and environmental factors, and strongly influenced by the hypothalamic–pituitary–adrenal axis, especially in times of stress (eg, insecure attachment, trauma, abuse). The UK Government study of inequalities in health, reviewing all of the evidence about early childhood and health, concluded by quoting from Kuh et al, “Follow up through life of successive samples of births has pointed to the crucial influence of early life on subsequent mental and physical health and development”.18,19 According to McCain and Mustard, positive play-based experiences in early years influence brain development and set neurological pathways that affect health, learning and behaviour throughout life.20
Behavioural questionnaires can be of great value in providing a more objective profile of a child from the teacher’s as well as the parents’ perspective. Commonly used questionnaires for ADHD include: the ADHD Rating Scale-IV (home, school and self-reporting)21 (A similar scale, SNAP-IV, together with instructions for scoring, is available for free download at <http://www.adhd.net>.); Connors’ Rating Scales (Revised);22 and the Child Behaviour Checklist (CBCL-Achenbach),23 which includes evidence for anxiety, depression and antisocial disorder as well as attentional factors. These questionnaires provide an opportunity to gather information from the school as well as the home.
A tool commonly used by psychologists to explore social, adaptive and behavioural abilities (age, 1–19 years) is the Vineland Adaptive Behaviour Scales. These are especially useful if autistic spectrum disorder or intellectual disability is being considered.24
School reports can provide information as to the child’s general academic progress, application and behaviour. Teachers’ concerns about disorganisation, inattentiveness, failure to complete work and underachievement over a period of more than a year provide helpful additional information if one of the forms of attention deficit disorder is being considered. It can also be helpful to see how the child rates in attainment tests that rank individual ability against peer populations.
For children who are underachieving or have specific areas of learning difficulty, formal psychometric testing should be sought from an educational psychologist. The most commonly used psychological test for preschool children is the Wechsler Preschool and Primary Scale of Intelligence, and for school-aged children the Wechsler Intelligence Scale for Children.25
There are also attainment tests of reading and mathematics that can provide more specific information as to a child’s progress.
To exclude other possible explanations for a child’s behaviour problems, physical and neurological examinations must always be carried out. Note particularly:
Vision: Use the Snellen 6-metre test for those of school age, and the Stycar 3-metre test or the Dunedin 4-metre test with confusion bars (or equivalent) for those in preschool.26,27
Hearing: In children with language delay, sensory neural and conductive hearing competency needs to be assessed, and this may require referral to an audiological service.
Syndrome and/or chromosomal anomalies: Neurocutaneous markings and dysmorphic features may point to either a syndrome and/or a chromosomal anomaly (eg, neurofibromatosis, fragile X syndrome, fetal alcohol syndrome, and tuberous sclerosis).
Motor skills: In the absence of “hard” neurological signs, difficulty with gross motor skills such as hopping, skipping, and tandem walking may reflect hypotonia or lax ligaments.
Fine motor competency can be assessed by a child’s ability to do up buttons and tie shoe laces, and in cutting, threading, pegboard proficiency and drawing. At a screening level, some useful information can be obtained by noting a child’s ability to copy a range of geometric and block shapes (Box 3). The Goodenough Draw-a-Man Test is also helpful as an indicator of cognitive development (Box 4).28,29
Neurological signs: Hyperventilation for more than 1 minute may identify the presence of absence seizures. Check the fundi oculi for signs of raised intracranial pressure, and exclude signs of long-tract dysfunction or evidence of cerebellar or parietal lobe deficits. Immature or “clumsy” coordination is commonly associated with developmental, learning and attentional problems, but is not diagnostically specific.
ADHD is now well established as a genetic, neurobiochemical and developmental disorder for which both the Diagnostic and statistical manual of mental disorders (DSM-IV) and the International classification of diseases have clear criteria. The DSM-IV criteria require at least six of the stated inattentive symptoms to have been present for a minimum of 6 months, and a minimum of six of the hyperactivity–impulsivity symptoms. The symptoms need to be present before the age of 7 years, and to be present in two or more settings, with clinical evidence of impairments socially, academically or occupationally. Currently, in DSM-IV, three subtypes are recognised (hyperkinetic/impulsive, inattentive and combined).30 A summarised version of the DSM-IV criteria for ADHD is given in Box 5. The Connors’ Rating Scales and the ADHD Rating Scale-IV (already mentioned) are based on DSM-IV criteria.
It is particularly useful to note whether a child is not handling multiple stimuli, noise or crowded situations, does not like change, is not well self-regulated or organised, and is often underachieving compared with his or her known ability. Functionally, the problem relates to deficits with “working memory” or “executive functions”.32
It is well recognised that children with ADHD may have additional comorbid conditions (including tic disorder and autism) that also need careful evaluation and management. A recent review by Marsha and Rappley is recommended reading.33 The proportion of children with ADHD who have comorbid conditions has been given as: specific learning difficulties, about 25%; depression, up to 30%; anxiety, about 20%; conduct disorder, 15%.34
Dyslexia is a term that refers to a specific learning difficulty with reading, and is defined as reading capacity 2 years or more behind expected levels for general ability. Dyslexia is related to language and perception rather than to vision. There can also be specific learning difficulties with mathematics, spelling and handwriting. Not all children with specific learning difficulties have other developmental problems such as ADHD, and not all children with ADHD have specific learning difficulties. However, they are commonly associated and need to be considered in the overall assessment.6,7
Autistic spectrum disorder (also known as “pervasive developmental disorders”) affects up to 2.5/1000 children, with a male:female ratio of 3:1. It is characterised by deficits in communication and social interaction, accompanied by repetitive or restricted activities or interests. The early warning signs are reduced eye regard, absence of pointing, delayed language, absence of or delay in pretend play, odd or repetitive rituals, disinterest in people and lack of awareness of the feelings of others.30,35
The criteria given by DSM-IV for diagnosing oppositional defiant disorder and conduct disorder are summarised in Box 6. Oppositional defiant disorder is more likely to be present in younger children and conduct disorder in older children — they are probably gradients of the same disorder. Both imply behaviour that is aggressive and antisocial in a wide context. However, care must be taken not to confuse these conditions with normal variations and behaviours associated with developmental stages (especially toddlers and early adolescents).30
These disorders are beyond the scope of this article, but are well described for GPs in Child psychiatry by Goodman and Scott.3 Some of the features suggestive of the first three of these disorders are:
Anxiety: Separation difficulties, school refusal, phobias and fears interfering with function, panic episodes, social avoidance, tics, eating and sleeping difficulties.
Depression: Excessive tearfulness, mood change, loss of pleasure or interest in activities, social withdrawal, self-blame, self-harm, decline in school grades, and suicidal talk or thoughts.
Abuse: Unaccounted for and repeated injuries, failure to thrive, “frozen watchfulness”, withdrawn responsiveness, emotional lability, bullying, sexualised play, sexual precociousness, apathy, and poor school grades.
A child with developmental, behavioural or learning difficulties is likely to need the assistance of professionals from several different disciplines (including teachers, educational and clinical psychologists, speech pathologists, occupational therapists and physiotherapists) who can complement the efforts of medical practitioners. The family may need the help of a social worker. Some children, especially those in preschool and primary school, may benefit from referral to a child development centre where such a multidisciplinary team can assist in further assessment of the problem and provide guidelines for early intervention. If such a centre is not accessible or desirable, a paediatrician with additional training in developmental and behavioural paediatrics, together with a clinical psychologist or a speech pathologist, may be a helpful private sector alternative.
Children with severe or dangerous behaviour problems may require referral to child and adolescent mental health services or to a private child psychiatrist. Waiting times, especially in the public sector, can be a disadvantage because of the greater effectiveness of early intervention.36
Strategies for both home and school management may be required with consideration of remedial education or academic extension. For those with ADHD, the National Health and Medical Research Council has provided helpful management guidelines for home and school.37 Medication may also be required and is likely to be initiated by a specialist, although shared care with a GP is available in some states, especially in rural areas. This is likely to be effective in most children, although a “multimodal” approach is recommended.38,39
The important role of the GP is summarised in Box 7.
In these complex conditions, inevitably a plethora of approaches both to diagnosis and management are advocated. Some of the unproven strategies that are used are chiropractic back or cranial manipulation, multivitamins, fish oil and primrose oil preparations, eye tracking exercises and developmental optometry, and electroencephalogram biofeedback. These unproven therapies can also be quite expensive.40,41
Jack was assessed using the Wechsler Intelligence Scale for Children, and identified as being of superior intelligence with no evidence of specific learning difficulties. His school reports were monitored to assess his academic progress and behaviour; he was continuing to underachieve, and his disruptive class and social behaviour was also continuing. DSM-1V questionnaires obtained from home and school indicated that he fulfilled the criteria for the combined form of ADHD and had clinically significant anxiety.
Initial introduction of slow-release methylphenidate produced an immediate beneficial effect, with the need for an afternoon supplement of standard methylphenidate on some occasions. He shifted to the longer lasting slow-release form (Concerta), with even better outcomes, and is currently progressing very well at home, at school and socially. The facial and shoulder girdle twitching has resolved.
For Jack, medication together with parental support was found to be sufficient without the need for additional counselling or therapy.
Evidence-based practice tips
Children with ADHD are likely to be helped by a multimodal approach that includes medication (II).38,39
Early intervention is likely to improve outcome, especially in children with social or emotional problems without a biological basis (III-2).12,36
Children’s early brain development affects health, learning and behaviour throughout life (consensus review).9,20
Behavioural or emotional problems affect some 18% of young people; 10% have learning difficulties, and 5%–8% have attentional problems, with boys being more affected than girls (consensus review).2,11,12,16
Levels of evidence (I–IV) are derived from the National Health and Medical Research Council’s system for assessing evidence.42
1 Reassuring signs of developmental progress5
Gross motor achievements
Walking by 10–14 months
Climbing by 2½ years
Throwing and kicking a ball by 2 years
Pedalling a tricycle by 3 years
Hopping by 4 years
Skipping by 6 years
Fine motor achievements
Stacking three or four blocks by 18 months
Completing simple form boards by 2 years
Threading beads by 3½ years
Cutting a piece of paper by 3 years
Copying geometric shapes by 4 years
Tying shoelaces by 5 years
Printing legibly by 6 years
Speech and language achievements
Speaking single words by 12 months
Making word combinations by 2 years
Making clear, simple sentences and being interested in books and stories by 3 years
Making conversation clear to others by 3 or 4 years
Reading by 5 to 6 years
Social achievements
Dressing by 2 years
Self-feeding using cutlery by 3 years
Being toilet-trained by 3½ years
Playing cooperatively in groups by 3 years
Playing team games by 7 years
From Parry TS. Modern Medicine 1998; 41: 56-63. Reproduced with permission.
2 Selected features suggesting the possibility of developmental difficulties5
|
Birth to 3 years |
3–5 years |
5–8 years |
||||||||||||
Gross motor skills |
Bottom shuffling Delayed walking Not climbing or fear of climbing |
Delayed or awkward running Not pedalling a tricycle Bumping into objects Excessive falling Not hopping |
Not skipping (after 6 years) Inability to throw, catch or kick a ball Inability to ride a bicycle Tripping over or falling Not being picked for team activities |
||||||||||||
Fine motor skills |
Delayed pincer grip (after 10 months) Not stacking blocks Avoiding form boards and constructional toys Avoiding pencil tasks (after 2 years) |
Difficulties with cutting or threading Avoiding puzzles and constructional toys Difficulties with dressing and buttons Finger feeding rather than using utensils |
Avoiding drawing or immature drawing Inability to colour in shapes Inability to do up shoelaces Messy or illegible handwriting Low output of written work (in terms of both quantity and quality) |
||||||||||||
Speech and language skills |
Absence of single words (by 18 months) No interest in books Reduced imaginative play (after 2 years) |
Not using developed simple sentences (by 2 years) Speech unclear to strangers Use of gestures or mime more than words (by 3 years) |
Unclear or limited sentences Speech unclear to family No interest in books or stories Delay in reading and spelling |
||||||||||||
Behaviour and social skills |
Unsettled or sleeping poorly Irritability Excessive tantrums (after 2 years) |
Unsettled sleep Persistent tantrums Inability to play with peers Inability to self-dress and unawareness of toileting skills |
Difficulty making friends Emotional lability Delayed dressing and feeding skills Reluctance or refusal to attend school |
||||||||||||
From Parry TS. Modern Medicine 1998; 41: 56-63. Reproduced with permission. | |||||||||||||||
3 Block and pencil tests5
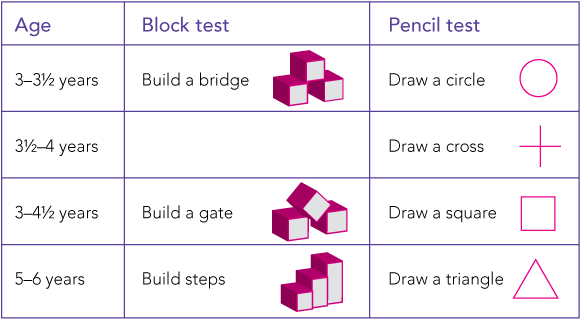
The test corresponding to the child’s age is used to screen cognitive and perceptual development. For the block test, build the structure behind a screen, remove the screen and then ask the child to copy it. For the pencil test, draw the shape on a piece of paper, without the child watching, and then ask the child to draw the same shape.
From Parry TS. Modern Medicine 1998; 41: 56-63. Reproduced with permission.
4 The Goodenough Draw-a-Man Test29
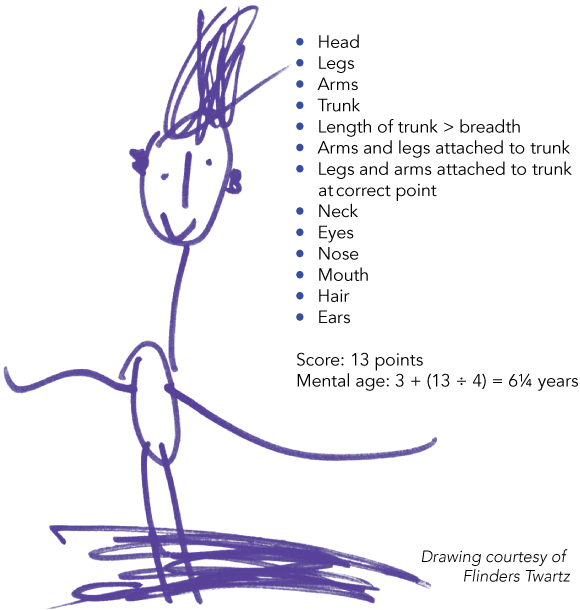
The child is asked to draw a man, and receives a point for each item drawn, with four points equating to 1 year of age. As children draw circles at 3 years, the basic score is 3 and the formula is: 3 + n/4, which gives the child’s approximate mental age (‘n’ is the number of parts drawn).
5 Diagnostic criteria for attention deficit hyperactivity disorder (summarised from the DSM-IV-TR criteria)30,31
(A) Either (1) or (2):
(1) Inattention: Six (or more) symptoms of inattention have persisted for at least 6 months to a degree that is maladaptive and inconsistent with developmental level (eg, often fails to give close attention to details or makes careless mistakes in schoolwork, work, or other activities; is often forgetful in daily activities).
(2) Hyperactivity–impulsivity: Six (or more) symptoms of hyperactivity–impulsivity have persisted for at least 6 months to a degree that is maladaptive and inconsistent with developmental level (eg, hyperactivity: often fidgets with hands or feet or squirms in seat; impulsivity: often interrupts or intrudes on others).
(B) Some hyperactive–impulsive or inattentive symptoms that caused impairment were present before age 7 years.
(C) Some impairment from the symptoms is present in two or more settings (eg, at school [or work] or at home).
(D) There must be clear evidence of clinically significant impairment in social, academic, or occupational functioning.
(E) The symptoms do not occur exclusively during the course of a pervasive developmental disorder, schizophrenia, or other psychotic disorder, and are not better accounted for by another mental disorder (eg, mood disorder, anxiety disorder, dissociative disorder).
DSM-IV -TR = Diagnostic and statistical manual of mental disorders, 4th edition, text revision.
6 DSM-IV-TR criteria for oppositional defiant disorder and conduct disorder30
For a diagnosis of oppositional defiant disorder, DSM-IV criteria specify that, over a period of 6 months, a child’s behaviour involves at least four of the following:
–often losing his or her temper;
–often arguing with adults;
–often defying adults’ requests or rules;
–often deliberately annoying other people;
–often blaming others for his or her own mistakes;
–often being touchy or easily annoyed by others;
–often being angry and resentful; and
–often being spiteful or vindictive.
For a diagnosis of conduct disorder, DSM-IV criteria specify that, over a period of 12 months, a child’s behaviour involves at least three of the following, with at least one occurring within the past 6 months:
–frequent bullying, threatening or intimidation of other people;
–often starting physical fights;
–using a weapon that could cause serious harm;
–being physically cruel to people;
–being physically cruel to animals;
–stealing while confronting a victim;
–forcing someone into sexual acts;
–setting a fire to cause damage;
–deliberately destroying another’s property;
–breaking into a car, house or other building;
–often lying to obtain favours or avoid obligations;
–stealing small items without confronting the victim;
–running away from the parental home overnight at least twice;
–often staying out at night without permission;
–often truanting from school (the last two beginning before 13 years of age).
DSM-IV-TR = Diagnostic and statistical manual of mental disorders, 4th edition, text revision.
7 The role of the general practitioner
Monitoring development of all children to allow early recognition of possible problems, and making the initial diagnosis and assessment
Referral for further specialist evaluation and collaborative management, as indicated
Development of a care plan, together with all concerned parties
Advocacy for the child in educational, welfare and justice systems
Liaison with school teachers and principals to obtain appropriate support and access to remedial and behavioural programs, with information sharing and review
Organising case conferences with care teams
Advice about availability of early intervention
Information about alternative therapies and programs
Advice about allowances, financial and respite support
Monitoring of medication, if relevant, and review of progress
Support for the parents, siblings and other family members, including respite care, if required
- Trevor S Parry1
- School of Paediatrics and Child Health, University of Western Australia, Perth, WA.
- 1. Glascoe FP. The value of parents’ concerns to detect and address developmental and behavioural problems. J Paediatr Child Health 1999; 35: 1-8.
- 2. Australian Bureau of Statistics. Western Australian child health survey: developing health and well-being in the nineties. Canberra: ABS and the TVW Telethon Institute for Child Health Research, 1995. (Catalogue No. 4303.5.)
- 3. Goodman R, Scott S. Child psychiatry. Chapter 2 — Classification. Oxford: Blackwell Science, 1997.
- 4. Sheridan M. Birth to five years: children’s developmental progress. 2nd edition. Australian Council for Educational Research, 1997.
- 5. Parry TS. The clumsy child: getting to the “vibe” of the thing. Mod Med 1998; 41: 56-63.
- 6. Beitchman JH, Young AR. Learning disorders with a special emphasis on reading disorders: a review of the past 10 years. J Am Acad Child Adolesc Psychiatry 1997; 36: 1020-1032.
- 7. Shapiro BK, Accardo PJ, Capute AJ. Specific reading disability — a view of the spectrum. Timonium, Md: York Press, 1998.
- 8. Williams H, Carmichael AJ. Depression in mothers in a multi-ethnic urban industrial municipality in Melbourne. Aetiological factors and effects on infants and preschool children. J Child Psychol Psychiatry 1985; 26: 277-288.
- 9. Shonkoff JP, Phillips DA, editors. From neurons to neighborhoods: the science of early childhood development. Board on Children, Youth, and Families, National Research Council and Institute of Medicine. Washington, DC: National Academy Press, 1998.
- 10. Hipwell AE, Murray L, Ducournau P, Stein A. The effects of maternal depression and parental conflict on children’s peer play. Child Care Health Dev 2005; 31: 11-23.
- 11. Australian Bureau of Statistics. Western Australian Child Health Survey: family and community health. Canberra: ABS, and the TVW Telethon Institute for Child Health Research, 1996. (Catalogue No. 4304.5.)
- 12. Marshall J, Watt P. Child behaviour problems. A literature review of the size and nature of the problem and prevention interventions in childhood. Perth, WA: The Interagency Committee on Children’s Futures, 1999.
- 13. Tremblay RE. When children’s social development fails. In: Keating DK, Hertzman C, editors. Developmental health and the wealth of nations. Chapter 4. New York: The Guildford Press, 1999.
- 14. Tremblay RE. Development of physical aggression from early childhood to adulthood. In: Tremblay RE, Barr RG, Peters RdeV, editors. Encyclopedia on early childhood development. Quebec: University of Montreal, 2002: 1-6. Available at: www.excellence-earlychildhood.ca/documents/TremblayANGxp.pdf (accessed May 2005).
- 15. Slee PT, Rigby K. Australian school children’s self appraisal of interpersonal relations: the bullying experience. Child Psychiatr Hum Dev 1993; 23: 273-282.
- 16. Australian Bureau of Statistics. Western Australian Child Health Survey: education, health and competence. Canberra: ABS and the TVW Telethon Institute for Child Health Research, 1997. (Catalogue No. 4305.5.)
- 17. Wilkins-Shurmer A, O’Callaghan MJ, Najman JM, et al. Association of bullying with adolescent health-related quality of life. J Paediatr Child Health 2003; 39: 436-441.
- 18. Acheson D. Independent inquiry into inequalities in health. London: The Stationery Office, 1998.
- 19. Kuh D, Ben-Shlomo Y, editors. A life course approach to chronic disease epidemiology. Oxford: Oxford University Press, 1997.
- 20. McCain MN, Mustard JF (co-chairs). Reversing the real brain drain: early years study final report. Toronto: Ontario Children’s Secretariat, 1999.
- 21. DuPaul GJ, Power TJ, Anastopoulos AD, Reid R. ADHD Rating Scale-IV. New York: The Guildford Press, 1999.
- 22. Connors CK. Manual for the Connors’ Rating Scales — Revised. North Tonawanda, NY: Multi-Health Systems, 1997.
- 23. Achenbach TM. Manual for the Child Behaviour Checklist/4-18 and 1991 profile. Vermont: University of Vermont, Department of Psychiatry, 1991.
- 24. Sparrow SS, Balla DA, Cicchetti DV. Vineland Adaptive Behaviour Scales. Circle Pines, Minn: American Guidance Service, 1984
- 25. Wechsler D. Wechsler Intelligence Scale for Children: fourth edition. San Antonio, Tex: Psychological Corporation, 2003.
- 26. Sheridan M. Manual for the Stycar vision tests, revised 1976. London: NFER-Nelson Publishing, 1976.
- 27. 4.0 metre letter matching vision test with confusion bars. Dunedin, NZ: Medical School, University of Otago.
- 28. Pollak M. Textbook of developmental paediatrics. Edinburgh: Churchill Livingstone, Longmans, 1993.
- 29. Goodenough FL. Measurement of intelligence by drawings. Chicago: Harcourt, 1926.
- 30. First MB, Tasman A, editors. Diagnostic and statistical manual of mental disorders, 4th edition, text revision. DSM-IV-TR. New York: John Wiley, 2004.
- 31. Halasz G, Vance ALA. Attention deficit hyperactivity disorder in children: moving forward with divergent perspectives. Med J Aust 2002; 177: 554-557.
- 32. Barclay RA. Attention deficit hyperactivity disorder — a handbook for diagnosis and treatment. 2nd edition. Chapter 7 — A theory of ADHD: inhibition, executive functions, and time. New York: The Guildford Press, 1998.
- 33. Marsha D, Rappley MD. Attention deficit-hyperactivity disorder. N Engl J Med 2005; 352: 165-172.
- 34. Barclay RA. Attention deficit hyperactivity disorder — a handbook for diagnosis and treatment. 2nd edition. Chapter 4 — Comorbid disorders, social relations, and subtyping. New York: The Guildford Press, 1998.
- 35. Wray J, Silove N, Knott H. MJA practice essentials – paediatrics. 7. Language disorders and autism. Med J Aust 2005; 182: 354-360. <MJA full text>
- 36. Parry TS. The effectiveness of early intervention: a critical review. J Paediatr Child Health 1992; 28: 343-346.
- 37. National Health and Medical Research Council. Attention deficit hyperactivity disorder. Canberra: NHMRC, 1997. Available at: www.nhmrc.gov.au/publications/adhd/contents.htm (accessed May 2005).
- 38. Abikoff H, Hechtman L, Klein RG, et al. Symptomatic improvement in children with ADHD treated with long-term methylphenidate and multimodal psychosocial treatment. J Am Acad Child Adolesc Psychiatry 2004; 43: 802-811.
- 39. MTA Cooperative Group. National Institute of Mental Health Multimodal Treatment Study of ADHD Follow-up: 24 month outcomes of treatment strategies for attention-deficit/hyperactivity disorder. Pediatrics 2004; 113: 754-761.
- 40. Stubberfield TG, Wray JA, Parry TS. Utilization of alternative therapies in attention-deficit hyperactivity disorder. J Paediatr Child Health 1999; 35: 450-453.
- 41. Sinha D, Efron D. Complementary and alternative medicine use in children with attention deficit hyperactivity disorder. J Paediatr Child Health 2005; 41: 23-26.
- 42. National Health and Medical Research Council. How to use the evidence: assessment and application of scientific evidence. Handbook series on preparing clinical practice guidelines. Table 1.3: Designation of levels of evidence. Canberra: NHMRC, February 2000: 8. Available at: www.health.gov.au/nhmrc/publications/pdf/cp69.pdf (accessed Mar 2005).





Abstract
Brain development from late pregnancy to 3 years of age affects a child’s learning, behaviour and health throughout life.
Behavioural difficulties in children are usually symptoms of underlying problems.
Observing a child’s appearance and performance, and taking a detailed history (considering factors in the child, the home, the school and the wider environment) provide most of the information needed for diagnosing behavioural problems.
It is important to know what is “normal” for all stages of a child’s development, but equally important not to confuse behavioural difficulties with normal variations and behaviours associated with developmental stages.
Assessment and early intervention for behavioural and learning difficulties in children require a multidisciplinary team approach.
As well as the recommended “multimodal” approach for managing attention deficit hyperactivity disorder, shared care with a general practitioner is available in some states, but medication is likely to be the trigger for a positive outcome.