In 1992, after a decade of adverse publicity and a series of public inquiries into mental health services, all Australian governments adopted a National Mental Health Policy.1,2 The Policy, implemented through a series of five year National Mental Health Plans,3-5 became known as the National Mental Health Strategy.
In 2005, we again have adverse publicity, three national inquiries under way or planned (which directly or indirectly arose from criticisms of mental health services), and growing professional disquiet about the adequacy of mental health care. What has happened in the last decade to get us into this situation?
In 2002, total spending on mental health services was $3.1 billion, a 65% increase in real terms since 1993.6 As a proportion of overall health expenditure, this is similar to mental health expenditure in other developed countries. In terms of a service-costing approach, specialised mental health services accounted for 6.4% of Australia’s recurrent health expenditure in 2001–02.6 Using an alternative disease-costing approach, the Australian Institute of Health and Welfare (AIHW) estimated that Australia spent 6.2% of recurrent health expenditure on mental health care in 1993–94.7 This is comparable to 6.6% in the Netherlands and 7.3% in the United States, although comparison between countries is difficult because of the differing ways expenditure and services are counted. The AIHW analysis also shows that the proportion of health expenditure for mental health rises to 9.6% if substance abuse and dementia are included. It has been argued that, as mental disorders and substance abuse contribute 13% of Australia’s disease burden, 9.6% of health expenditure is insufficient.8 There have been claims to the contrary,9 but, in fact, there are no reliable international benchmarks by which to judge Australia’s relative investment in mental health.
The total increase in government spending of 65% on mental health services between 1993 and 2002 was made up by increases in federal expenditure of 128% and state and territory expenditure of 40%. While the 65% increase appears impressive, it only paralleled growth in overall government health spending during the decade.6
Growth at the national level masks important differences between local communities. By 2002, 10 years into the Mental Health Strategy, significant disparities in per capita spending on mental health continued between states and territories, with the difference between the highest and lowest spending jurisdictions decreasing only marginally over the decade (Box 1). The differences in spending between the states and territories translates into a wide variation across Australia in the level of mental health services available.
The changes that followed the introduction of the Mental Health Strategy needed to address the legacy of 30 years of deinstitutionalisation, which saw the number of psychiatric beds decrease from 30 000 to about 8000, with limited development of community services, and a doubling of Australia’s population.10,11
Under the Mental Health Strategy, the size and number of stand-alone psychiatric hospitals continued to decline, but with agreement that they be replaced by acute beds in general hospitals and a range of community-based services, including residential accommodation. Another difference from the situation in the period before the strategy was implemented was the requirement for states and territories to maintain or increase their mental health budgets (a “maintenance of effort clause” in the Health Care Agreements), though this requirement was only for the life of the First and Second National Plans (1993–2003). While increasing in actual dollar terms, the relative role of federal funding, which allowed states and territories to establish community and other services, has decreased over time and more of the new services are being funded by states and territories (Box 2). For every federal dollar allocated to states and territories under the Strategy, combined state and territory funding of mental health increased by $4.60.6
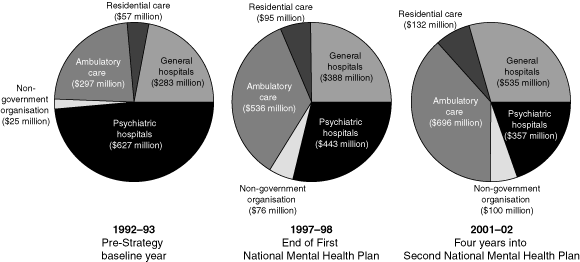
The change in the mix of mental health services over the decade has been substantial. In 1993, only 29% of state mental health resources were directed toward community-based care; 73% of psychiatric beds were located in stand-alone hospitals, and these consumed half of the total spending by the states and territories on mental health care. By 2002, this had changed to 51% of state mental health resources for community-based care, and 39% of psychiatric beds in stand-alone hospitals consuming 29% of state mental health resources. In 1993, 55% of all acute psychiatric beds were in general hospitals, increasing to 82% by 2002 (Box 3).
Contrary to popular belief, the overall number of acute beds in Australia increased by 6% over 1993–2002.6 Long-stay beds have been exclusively targeted for reduction, and have decreased by 52%, equivalent to about 2300 beds. Development of 24-hour residential services to replace long-term hospital beds has been patchy, with most expansion occurring in Victoria. Nationally, the growth in 24-hour residential services is equivalent to only one quarter of the reduction in long stay beds.6
The need to improve the quality, as well as expand the quantity, of mental health services was one of the goals of the Mental Health Strategy. Service standards, one part of a quality and safety framework, were developed12 and are now used by health service accreditation agencies. By June 2003, almost 90% of all public mental health services had begun the process of having their services reviewed in terms of the standards, and almost half had completed a review against these standards.
The role of non-government organisations (NGOs) has expanded over the past decade with the recognition they could deliver some services more efficiently or more effectively than the government or the private sector. In 1993, less than 2% of resources were allocated to non-government programs aimed at providing support for people with a psychiatric disability in the community. This increased three-fold over the 10 years, and now accounts for 5.5% of total state mental health expenditure.
The services that NGOs provide are affected by the policies and programs of government agencies such as housing, education and training, employment, justice, police, community and disability services. These agencies have a role in assisting with the recovery of people with psychiatric disability.13 An attempt to align the policies and programs of these government departments so that they complemented the Mental Health Strategy was made when relevant Ministers endorsed findings of the Mental Health Forum on Intersectoral Linkages.14 Little evaluation of this component of the Strategy has been undertaken, and the achievements have been limited.10
The private psychiatric hospital sector is also growing.6 In 2002, it provided 23% of all psychiatric beds (an increase from 14% in 1993) and employed 11% of the mental health workforce (an increase of 80% since 1993). Health insurance funding of private psychiatric hospitals grew by 17% over the 10 years, which, combined with the estimated $38 million per year injected by the private health insurance rebate, resulted in an increase in the number of private beds (38%), patient days (59%) and separations (270%).
However, private outpatient psychiatric services are shrinking. Expenditure on private psychiatrists, funded through the Medicare Benefits Schedule (MBS), grew by 6% annually in the decade before the Strategy. This growth rate slowed significantly and, by 1996–97, had begun to reverse. Total federal expenditure on private psychiatrists has been declining by 2%–3% per year since then.
The reasons for this decline are believed to be the increased number of psychiatrists working part time, and private psychiatry diversifying its payment sources (with the expansion of Department of Veterans’ Affairs and workers compensation payments for mental disorders). More psychiatrists are also working in the public sector, in which there was a 37% growth in medical staff between 1993 and 2002.
Expansion of community and non-hospital residential services was responsible for most of the 25% increase in the clinical workforce over the decade. All mental health professional provider groups grew, but there was a shift in the staffing mix, with medical and allied health staffing showing the greatest percentage increase and staff shortages most notable in nursing and psychiatry.6
To improve the quality of care, 12 National Practice Standards have been identified which define the attitudes, knowledge and skills which all mental health professionals should have, and which complement discipline-specific skills.15 These are to be implemented during the life of the Third National Mental Health Plan.
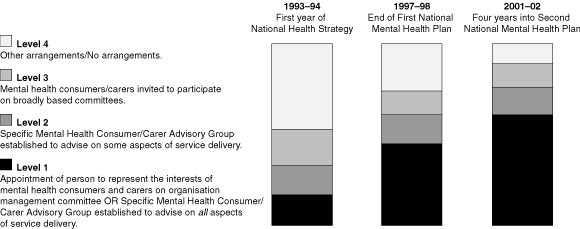
Involving consumers and carers in service delivery and planning was also a key part of the National Strategy. Federal funding was contingent on the establishment of community advisory groups in every jurisdiction. While this was initially done as a token gesture in some services to secure funding, it has, over time, become more accepted, and participation rates of consumers and carers have increased considerably (Box 4).
The Mental Health Council of Australia <http://www.mhca.com.au> was established in November 1997 as a focal national body representing most of the key stakeholders in the mental health sector. It provides advice to governments, representing the interests of its member organisations, along with monitoring and analysing national mental health policy, resource allocation and outcomes. It has proven to be independent and effective in carrying out these tasks.
Mental health legislation is the responsibility of state and territory governments. However, Australia’s commitment to the United Nations (UN) Principles for the Protection of Persons with Mental Illness and the Improvement of Mental Health Care16 resulted in this becoming a benchmark for state and territory legislation. A Rights Analysis Instrument was developed by the Federal Attorney-General’s Department to assess compliance of state and territory mental health legislation with the UN principles.17 All states and territories have used this instrument to assess their legislation and have passed new legislation or amended their Mental Health Acts accordingly.
Protecting funding and measuring service activities (eg, occupied bed days, number of patients seen) does not tell us what outcomes are achieved. One of the more ambitious aims of the Strategy has been to introduce individual consumer outcome measures into routine clinical practice in both public services and private hospitals. All states and territories, through information development funding agreements with the federal government, submit de-identified, patient-level outcome data, referred to as the “National Outcomes and Casemix Collection”.18 A similar process exists for the private sector. Details of the outcome measures are at <http://www.mhnocc.org>.
By July 2003, 95% of the private hospital sector was collecting outcome measures on a routine basis and 60% of the public sector had begun collecting outcome measures. However, improving the quality of the data will be a challenge, and considerable work is needed to make these measures meaningful to clinicians in routine clinical practice and to build a culture which values outcome information within the mental health sector.
In 1997, the Australian Bureau of Statistics surveyed 10 600 households to assess mental health morbidity, disability and service use at the population level. This survey found, similarly to other countries, that 18% of the Australian population meet the criteria for mental disorder or substance abuse in a 12-month period, and that these cause considerable disability. Only 38% of those meeting the criteria received treatment from a health professional,19 and general practitioners delivered most care. Two further epidemiological surveys, of low prevalence disorders20 and child and adolescent disorders,21 also found considerable unmet need and disability. Around the same time, the Australian Burden of Disease Study showed that the largest population disease burden, within the mental disorders, was attributable to anxiety disorders, mood disorders and substance abuse.22
This type of research paved the way for a greater focus on common mental disorders such as anxiety and depression. Initiatives in mental health promotion and illness prevention were introduced under the Second National Mental Health Plan.4 In general practice, incentive payments were introduced, access to education and training was increased, more allied health services were introduced and changes were made to the MBS to promote better care of people with these disorders.23 A recent report by the AIHW shows that GPs deliver over 10 million mental health-related consultations annually, more than double the attendances in the specialist mental health public sector.24
Given the current disquiet about service delivery, has the direction of reform been the right one? Several evaluations of the Strategy,25-27 a recent review by the Canadian Senate28 and a prevailing view in the mental health sector8 support the directions of the Mental Health Strategy. If the policy directions are right, what is not right?
The main criticism has been of a perceived failure to implement the policy directions of the Strategy.8 However, the evidence summarised in this article indicates that the service system is being reformed in the agreed directions. While the redevelopment has been uneven, with disparities in funding and services continuing between the states and territories, change in many areas has been substantial.
Are the data on services reliable? Is all the money that governments say they spend on mental health actually spent there? With the withdrawal of the “maintenance of effort” clause for mental health services in the 2003-08 Health Care Agreements, there is less accountability for the dollars spent, and there have been unsubstantiated reports of mental health budgets being spent in other areas of health. In the absence of detailed independent audits of each health service’s accounts (an approach not taken anywhere in the health system), it is not possible to provide a definitive answer to these questions. But it is relevant to acknowledge the substantial effort that is put into validating national mental health expenditure trends — arguably more than in any other area of the health industry. It is our view that, even if the expenditure data as reported by health services contain some inaccuracies, these are unlikely to be substantial.
The key question therefore is not whether national policy settings are incorrect, or whether policy directions have been implemented, but whether the pace and extent of change has been enough. There are indications that it has not. Consumers, carers and advocates point to persisting problems with access to acute care, continuity of care and the availability of rehabilitation services.8 Compared with 10 years ago, these groups are now highly vocal, have greater expectations and are rightfully demanding a better deal from the health system. Coupled with this, there are indications that the significant unmet need highlighted by the 1997 mental health population surveys19-21 is beginning to surface, with more individuals now seeking treatment. All states and territories report increased demand for mental health care,6 with recent data showing a 7% increase in overnight admissions to acute psychiatric units between 1998–99 and 2002–03.24 While there are financial costs in meeting this demand, the personal, social and economic consequences of not doing so are likely to be much greater.29,30
In a world where the health dollar is finite, it is essential to ask whether the 65% increase in mental health spending since 1993 has given us a comparable return on investment, measured in terms of increased quantity and quality. The reality is we do not know and this, in our view, is a critical problem. Unlike other areas of health care, little attention has been given to ensuring efficiency in public sector mental health service delivery. Achieving value for money remains one of the key issues to be tackled in our national mental health reform.
1 Per capita expenditure on specialised mental health services by states and territories, 1992–93 and 2001–02
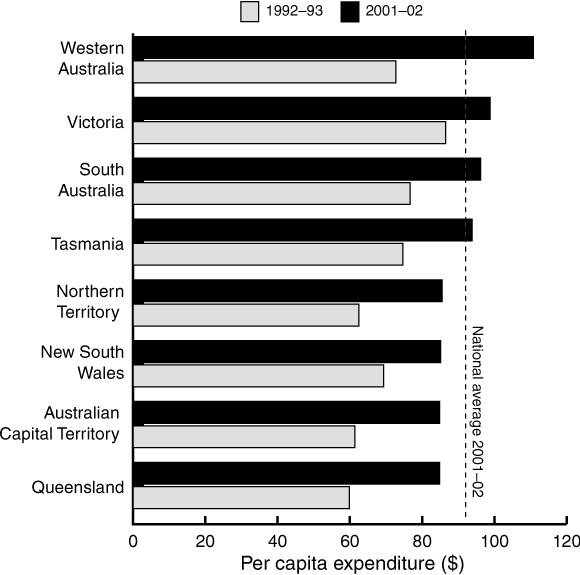
Source: Australian Government Department of Health and Ageing, 2004.6
2 Relative contribution of new funding and institutional savings to growth in community-based and general hospital services
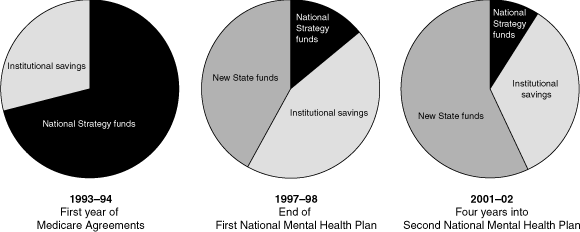
National Strategy funds refers to Australian Government grants provided to states and territories under the Medicare Agreements (1993–98) and the Australian Health Care Agreements (1998–2003). Source: Australian Government Department of Health and Ageing, 2004.6
- 1. Australian Health Ministers. National mental health policy. Canberra: Australian Government Publishing Service, 1992. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/mentalhealth-mhinfo-standards-nmhp.htm/$FILE/nmhp.pdf (accessed Jan 2005).
- 2. Whiteford HA. Australia’s national mental health policy. Hosp Community Psychiatry 1993; 44: 963-966.
- 3. Australian Health Ministers. National mental health plan. Canberra: Australian Government Publishing Service, 1992.
- 4. Australian Health Ministers. Second national mental health plan. Canberra: Australian Government Department of Health and Family Services, 1998.
- 5. Australian Health Ministers. National mental health plan 2003–2008. Canberra: Australian Government, 2003. Available at: http://www7.health.gov.au/hsdd/mentalhe/resources/pdf/mhplan.pdf (accessed Jan 2005).
- 6. National mental health report 2004. Eighth report — summary of changes in Australia’s mental health services under the National Mental Health Strategy 1993–2002. Canberra: Australian Government Department of Health and Ageing, 2004. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-pq-mental-pubs.htm (accessed Jan 2005).
- 7. Australian expenditure on mental disorders in comparison with expenditures in other countries. Canberra: Australian Institute of Health and Welfare, 2003. Available at: http://www.aihw.gov.au/publications/index.cfm/title/9997 (accessed Jan 2005).
- 8. Groom G, Hickie I, Davenport T. Out of hospital out of mind: a report detailing mental health services in 2002 and community priorities for national mental health policy for 2003–2008. Canberra: Mental Health Council of Australia, 2003.
- 9. Rosen A, McGorry P, Groom G, et. al. Australia needs a mental health commission. Australas Psychiatry 2004; 12: 213-219.
- 10. National mental health report 2002: seventh report – summary of changes in Australia’s mental health services under the National Mental Health Strategy 1993–2000. Canberra: Australian Government Department of Health and Ageing, 2002.
- 11. Doessel, D, Scheurer R, Chant D, Whiteford HA. Australia’s National Mental Health Strategy and deinstitutionalisation: some empirical results. Aust N Z J Psychiatry 2005. In press.
- 12. National mental health standards. Canberra: Australian Government Department of Health and Family Services, 1996.
- 13. Whiteford, HA. Intersectoral policy reform is critical to the National Mental Health Strategy. Aust J Public Health 1994; 18: 342-344.
- 14. Report of the Mental Health Forum on Intersectoral Linkages. Canberra: Commonwealth of Australia, 1995.
- 15. National standards for the mental health workforce. Canberra: Australian Government Department of Health and Ageing, Mental Health and Suicide Prevention Branch, 2002.
- 16. United Nations. The United Nations resolution 46/119 on the rights of people with mental illness and the improvement of mental health care. New York: United Nations, 1991.
- 17. Report to Australian Health Ministers’ Advisory Council National Mental Health Working Group. Application of rights analysis instrument to Australian mental health legislation. Canberra: Australian Government Department of Health and Aged Care, 2000.
- 18. National outcomes and casemix collection: an overview of clinical measures and data items. Version 1.5. Canberra: Australian Government Department of Health and Ageing, 2003.
- 19. Henderson S, Andrews G, Hall W. Australia’s mental health; an overview of the general population survey. Aust N Z J Psychiatry 2000; 34: 197-205.
- 20. Jablensky A, McGrath J, Herrman H, et al. Psychotic disorders in urban areas: an overview of the study on low prevalence disorders. Aust N Z J Psychiatry 2000; 34: 221-236.
- 21. Sawyer M, Kosky R, Graetz B, et al. The National Survey of Mental Health and Wellbeing: the child and adolescent component. Aust N Z J Psychiatry 2000; 34: 214-220.
- 22. Mathers C, Voss T, Stevenson C. The Australian burden of disease study: measuring the loss of health from diseases, injuries and risk factors. Med J Aust 2000; 172: 592-596.
- 23. Australian Department of Health and Ageing. Better outcomes in mental health. Available at: http://www.health.gov.au/internet/wcms/Publishing.nsf/Content/mentalhealth-boimhc-index.htm (accessed Jan 2005).
- 24. Australian Institute of Health and Welfare. Mental health services in Australia 2002–03. Mental Health Series No. 6. Canberra: AIHW, 2004. (AIHW Catalogue No. HSE-35.)
- 25. Evaluation of the National Mental Health Strategy: final report. Canberra: Australian Government Department of Health and Family Services, 1998.
- 26. Thornicroft G, Betts V. International mid-term review of the second national mental health plan for Australia. Canberra: Australian Government Department of Health and Ageing Mental Health and Special Programs Branch, 2002.
- 27. Evaluation of the Second National Mental Health Plan. Canberra: Australian Government Department of Health and Ageing, 2003.
- 28. Interim Report of the Standing Senate Committee on Social Affairs, Science and Technology. Mental health, mental illness and addiction. Ottawa, Canada: Senate of Canada, 2004. Available at: http://www.parl.gc.ca/38/1/parlbus/commbus/senate/com-e/soci-e/rep-e/repintnov04-e.htm (accessed Feb 2005).
- 29. Simon GE, Barber C, Birnbaum HG, et al. Depression and work productivity: the comparative costs of treatment versus nontreatment. J Occup Environ Med 2001; 43: 2-9.
- 30. Stewart WF, Ricci JA, Chee E, et al. Cost of lost productive work time among US workers with depression. JAMA 2003: 289: 3135-3144.





Abstract
We summarise the most recent data available on changes to the public and private mental health sectors from the commencement of the National Mental Health Strategy in 1993 to 2002.
There has been substantial service system change in the directions agreed by governments under the Strategy, supported by a 65% growth in government spending on mental health.
Despite this there is growing public and professional concern about deficiencies in the mental health service system. We review the current call for change in light of increased community expectations and growth in demand for services.
Given broad national and international support for Australia’s policy directions, the problems lie with the pace and extent of change and ensuring better outcomes from the increased investment in mental health care.