An 81-year-old woman was fitted with a single-chamber pacemaker for atrial fibrillation and symptomatic bradycardia (Microny SR 2425T, Pacesetter, Sylmar, Calif, USA; silicone lead 1402 T, Siemens, Sylmar, Calif, USA).
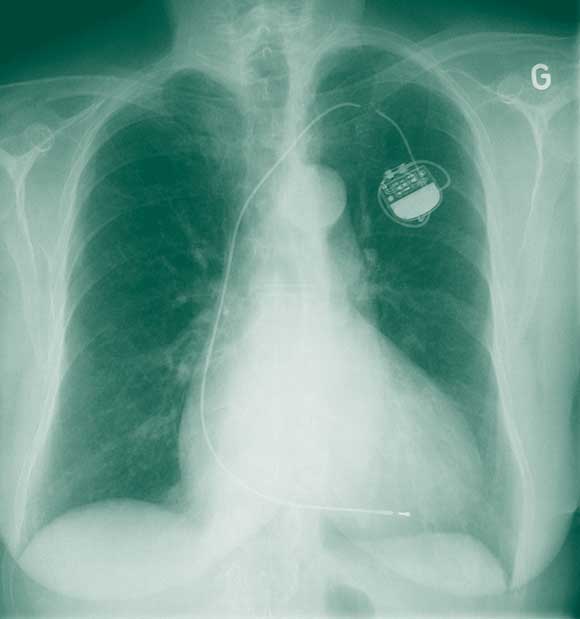
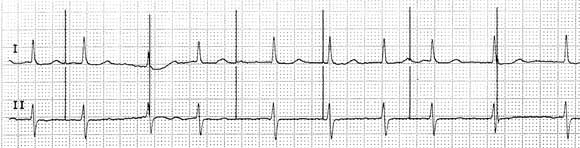
Seven years later, she presented with fatigue and presyncope of 1 week’s duration. She had also noticed contractions of the pectoral muscles on the left side of the chest. An electrocardiogram (Box 1) showed evidence of ventricular undersensing and non-capture, and a chest x-ray (Box 2) revealed complete fracture of the pacemaker lead. The pacemaker was replaced, and a new lead implanted using the cephalic vein cutdown approach.
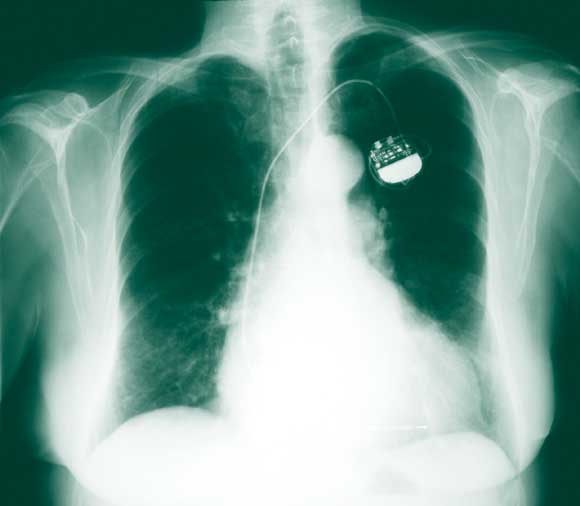
The patient’s medical record indicated that, 8 months previously, when she developed a cough, a chest x-ray had been performed by her physician. At around the same time, a routine check of the function of her pacemaker indicated that it was functioning normally. Re-examination of the x-ray revealed signs of lead erosion (Box 3) which had gone unnoticed. Thus, despite significant damage to the lead, pacemaker function may be unaffected.
Friction of the lead, most often against the clavicle and the first rib (known as subclavian crush) can damage the lead. The incidence of fracture of pacemaker leads is about 1.0%–2.5% and increases with the age of the lead.1 A way of avoiding this complication is to introduce the lead into the axillary or cephalic vein rather than via subclavian vein puncture.2,3
Routine chest x-rays should be performed to monitor the condition of pacemaker leads, especially where they cross the clavicle. We recommend an annual chest x-ray for pacemaker-dependent patients. This may identify lead damage that may not be apparent during a standard pacemaker check, and thus, potentially, avoid syncope or sudden death.
1 Electrocardiogram on admission showing pacing spikes with evidence of ventricular undersensing and non-capture
- Stephane L Noble1
- Haran Burri2
- Henri Sunthorn3
- Department of Cardiology, University Hospital of Geneva, Geneva, Switzerland.
- 1. Jacobs DM, Fink AS, Miller RP, et al. Anatomical and morphological evaluation of pacemaker lead compression. Pacing Clin Electrophysiol 1993; 16 (3 Pt 1): 434-444.
- 2. Antonelli D, Rosenfeld T, Freedberg NA, et al. Insulation lead failure: is it a matter of insulation coating, venous approach, or both? Pacing Clin Electrophysiol 1998; 21: 418-421.
- 3. Weiner S, Patel J, Jadonath R, et al. Lead failure due to the subclavian crush syndrome in a patient implanted with both standard and thin bipolar spiral wound leads. Pacing Clin Electrophysiol 1999; 22 (6 Pt I): 975-976.