Clinical record
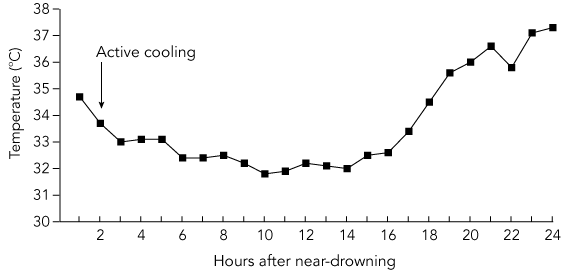
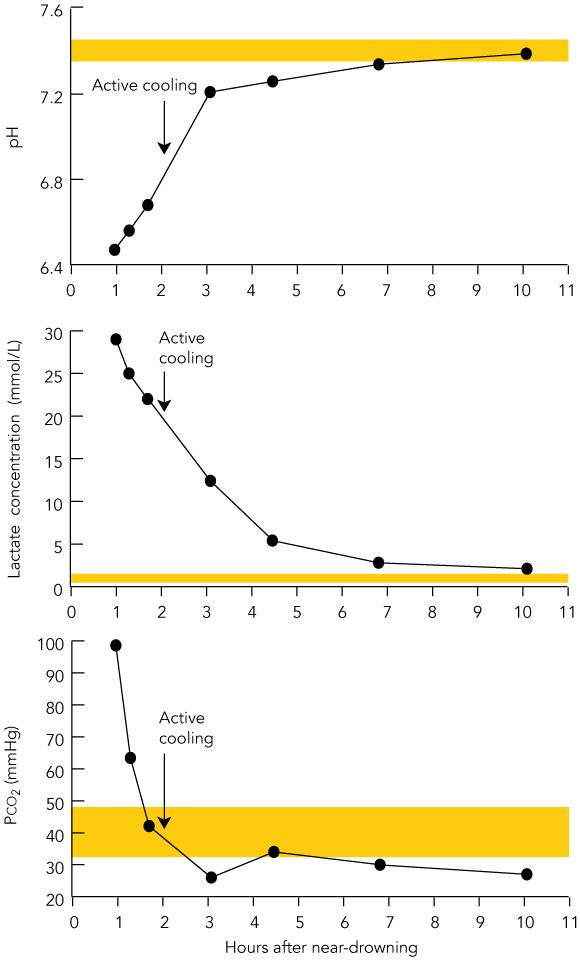
A 46-year-old English tourist became distressed when caught in a strong rip while swimming at a Sydney beach. An off-duty lifesaver dragged him to shore, where he was found to be apnoeic but had a weak pulse. After a minute of mouth-to-mouth ventilation, his pulse was lost, and chest compressions were begun. Ten minutes after cardiac arrest an ambulance arrived, and a wide complex bradycardia with no pulse was documented. During resuscitation, a total of 3 mg adrenaline, 70 mmol sodium bicarbonate and 1.5 mg atropine was administered. At 26 minutes after the cardiac arrest, the patient regained a pulse and was noted to be in atrial fibrillation. By this point, he was intubated and ventilated. On arrival in the emergency department, his systolic blood pressure was 90 mmHg, pulse rate was 136 bpm and irregular, and core temperature was 34.7°C. Auscultation of the chest revealed coarse bilateral crackles. His pupils were fixed and dilated. Initial arterial blood gases showed a severe mixed respiratory and metabolic acidosis, with a temperature-corrected pH of 6.47 (reference range [RR], 7.35 to 7.45), Pco2 of 98.6 mmHg (RR, 32.0–48.0 mmHg), Po2 of 104 mmHg (RR, 83.0–108 mmHg), arterial lactate level of 29 mmol/L (RR, 0.5–1.6 mmol/L), base excess of –28.1 mmol/L (RR, –2.0 to 2.0 mmol/L), and HCO3 level of 7.1 mmol/L (RR, 22–32 mmol/L). Chest radiography showed changes consistent with aspiration pneumonitis. The ventilator was adjusted to hyperventilate and reverse the respiratory component of the acidosis. Computed tomography of the head and neck revealed no abnormalities. It was decided to use controlled hypothermia to limit further hypoxic brain injury. The patient was packed in ice, and cooled intravenous fluids were administered, aiming for a core temperature of 33°C for a period of 12 hours (Box 1). The patient’s condition improved rapidly. The heart reverted to sinus rhythm spontaneously within a few hours, with no subsequent electrocardiograph or biochemical evidence of myocardial injury. The metabolic and respiratory acidosis normalised over the 10 hours after injury (Box 2). After 12 hours of hypothermia, cooling was ceased, and his core temperature was allowed to rise to 37°C. He was extubated on Day 3 after admission and discharged from hospital on Day 7. Neuropsychological assessment performed 2 weeks after the injury (including Wechsler Memory Scale Three and Delis–Kaplan Executive Function System) revealed relatively intact cognitive function, although there was moderate impairment in new learning ability and capacity for visuospatial information, and slowed information processing. This may be consistent with hypoxic brain injury, but, alternatively, might have been present before the accident. Repeat assessment 5 months after the accident (in the United Kingdom) revealed normal psychometric performance, with persisting impairment of visuospatial processing and organisational abilities. The patient and his family reported he was functioning just as he was before the injury, performing domestic duties and caring for his elderly mother. |
|||||||||||||||
The World Health Organization reported 409 272 drowning deaths worldwide in the year 2000, making this the second leading cause of unintentional injury death globally, after road traffic accidents.1 The burden of near-drowning morbidity has not been defined but is likely to be high.
Acidosis, especially pH < 7.0, usually correlates with a poor outcome. However, in drowning, the prognosis is often less grim, and patient survival has been reported after pH levels as low as 6.29.2 In our patient, the acidosis had both respiratory and metabolic components. The respiratory component, caused by apnoea, was the most readily correctable with gentle hyperventilation to “blow off” excess CO2. This had a rapid effect on the pH.
The metabolic component was most probably a result of both physiological and pathological processes — the extreme muscle exertion while struggling in the surf and end-organ hypoxia as his respiration and circulation failed. In intensive care, blood lactate levels > 10 mmol/L are associated with 95% mortality.3 Our patient’s arterial lactate level was 29 mmol/L. We believe one reason for his good outcome was that the acidosis had a different aetiology to that in most intensive-care patients, in whom sepsis, hypoxia and shock predominate. This case therefore highlights the importance of continuing resuscitation efforts despite severe acidosis and fixed dilated pupils in drowning victims, as ultimate neurological recovery is still possible.
Hypothermia is not a novel therapy for near-drowning. For over four decades, favourable outcomes have been reported for victims of near-drowning in ice-cold water.4 The effects of hypothermia are thought to be mediated by a reduction in brain metabolic requirements, limiting hypoxic cellular damage.
A 1986 trial in Canada used hypothermia in near-drowned children to reduce intracranial pressure and limit brain injury.5 However, the death rate in the hypothermic group was higher than in the normothermic group, with most deaths attributed to neutropenic sepsis. This complication is now thought to occur only in children.6 The study also used lower temperatures and a longer period of hypothermia than is now recommended. This may have contributed to the poorer outcome and subsequent lack of interest in hypothermia for near-drowning. Interestingly, survivors in the study were more likely to be neurologically intact if they had been assigned to the hypothermia group. This suggests that the benefit of hypothermia may be not in preventing death but in improving neurological outcome in survivors.
Recent evidence for controlled hypothermia as a neuroprotective therapy has been published in a study assessing its benefits in treating out-of-hospital cardiac arrest.7 This study used moderate (33°C), short-term (12 hours) hypothermia. Based on the favourable outcome of this and similar studies, the 2002 World Congress on Drowning, in Amsterdam, recommended this therapy for near-drowning victims who have restoration of adequate spontaneous circulation and remain comatose.8 A recent ILCOR (International Liaison Committee on Resuscitation) advisory statement also suggested that hypothermia may be beneficial for other rhythms causing cardiac arrest in settings such as drowning.9
We suggest that, in near-drowning cases where the patient remains comatose yet has adequate circulation, controlled hypothermia is an important tool to maximise neurological recovery. Further, severe acidosis should not be seen as a poor prognostic marker and should not preclude ongoing resuscitation efforts.
- 1. Department of Injuries and Violence Prevention, World Health Organization. Facts about drowning. Available at: www.who.int/violence_injury_prevention/ (accessed Jul 2004).
- 2. Wollenek G, Honarwar N, Golej J et al. Cold water submersion and cardiac arrest in treatment of severe hypothermia with cardiopulmonary bypass. Resuscitation 2002; 52: 255-263.
- 3. Weil MH, Afifi AA. Experimental and clinical studies of lactate and pyruvate as indicators of the severity of acute circulatory failure (shock). Circulation 1970; 41: 989-1001.
- 4. Siebke H, Rod T, Breivik H, et al. Survival after 40 minutes submersion without cerebral sequelae. Lancet 1975; 1: 1275-1277.
- 5. Bohn DJ, Biggar WD, Smith CR, et al. Influence of hypothermia, barbiturate therapy and intracranial pressure monitoring on morbidity and mortality after near drowning. Crit Care Med 1986; 14: 529-534.
- 6. Bernard SA, Buist MD. Induced hypothermia in the intensive care unit. A review. Crit Care Med 2003; 31: 2041-2051.
- 7. Bernard SA, Gray TW, Buist MD, et al. Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. N Engl J Med 2002; 346: 557-563.
- 8. Bierens JJ, Knape JT, Gelissen HP. Drowning. Curr Opin Crit Care 2002; 8: 578-586.
- 9. Nolan JP, Morley PT, Hoek TL, Hickey RW. Advancement Life Support Task Force of the International Liaison Committee on Resuscitation. Therapeutic hypothermia after cardiac arrest: An advisory statement by the Advanced Life Support Task Force of the international Liaison Committee on Resuscitation. Resuscitation 2003; 57: 231-235.





None identified.