The digital rectal examination (DRE) is an integral skill in clinical examination. It can be used to identify abnormalities of the anus and rectum, including rectal tumours, to characterise the prostate and assess gynaecological conditions, and to assess anal tone as part of a neurological or orthopaedic examination.1 A third of rectal cancers are palpable on DRE, while an abnormal prostate on DRE may have a positive predictive value for prostate cancer of up to 30%.2,3 Omitting a DRE may delay referral of patients with a potentially resectable carcinoma.4 Thus, DRE is an essential skill for all medical students to acquire.
Concern has arisen in Australia and overseas that medical students are no longer acquiring the skill of DRE before they graduate. In the United Kingdom, surveys suggest that the number of DREs performed by medical students during clinical training fell between 1990 and 2000, from a median of 11–30 to three to five.5,6 We undertook a survey of Australian medical students to assess their experience of learning DRE, as well as their attitudes, including any perceived barriers to learning this technique.
The questionnaire comprised 27 questions, including basic demographic data. Five of the questions, on the number of DREs performed and the number of abnormalities palpated (Box 1), had been used in a previous survey of teaching about DRE at the University of Oxford medical school.5
Results were analysed using the EpiCalc 2000 computerised statistical package (version 1.02).7 The χ2 test was used to calculate P values when comparing between studies, while Student’s t test was used to compare groups within the study.
Questionnaires were completed by 222 of the 256 students (87%), representing all University of Melbourne clinical schools: Austin Hospital (77/89 students), Royal Melbourne Hospital (79/88) and St Vincent’s Hospital (66/79). Respondents had a median age of 24 years and comprised 100 women and 122 men.
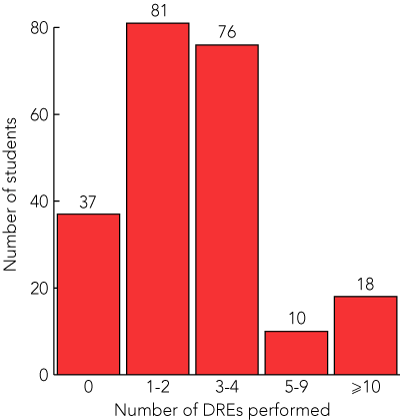
The number of DREs performed by the students is shown in Box 2. The median number was two, while 37 students (17%) had performed none, and 17 (8%) had performed 10 or more. There were no statistically significant differences in number of DREs performed by clinical school, sex or age (P > 0.05).
The number of times students had palpated a prostate and various abnormalities on DRE is shown in Box 1; 63% of students had palpated a prostate, 24% a prostate cancer, 19% a rectal tumour, and 11% faecal constipation.
The rotations in which DRE was performed included general surgery (134 students, urology (70), colorectal (59), general practice (35), emergency (26), obstetrics and gynaecology (26), general medicine (17), and an overseas elective (9).
Of the 185 students who had performed one or more DREs, 92% said they were supervised most of the time (defined as responses “all the time” or “more than half the time”), while 80% had their findings confirmed most of the time (97, all the time and 51, more than half the time).
Seventy-five per cent of the 185 students said they obtained patient consent most of the time, but rarely obtained written consent (8% obtained it most of the time). Seventy-eight students (42%) had performed DREs on anaesthetised patients.
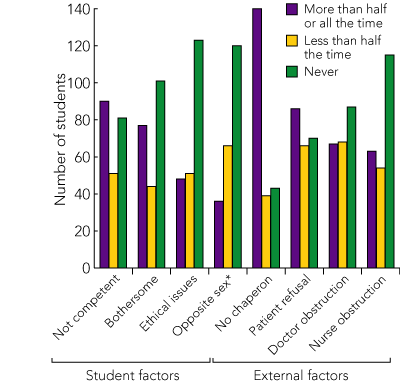
Reasons given for not performing DREs are shown in Box 3. The predominant reason was not having a doctor “chaperon” (63% said this was a reason “all the time” or “more than half the time”), followed by not feeling competent at DRE (41%), patient refusal (39%), too bothersome to organise a DRE (35%), and perceived obstruction by doctors (30%) and nurses (28%). Ethical opposition to unnecessary DRE (22%), being of the opposite sex as the patient (16%), and fear of being reported by patients and disciplined for “doing the wrong thing” (15%) were less common impediments.
This survey found that while final-year students at the University of Melbourne medical school had been taught DRE, this did not translate into their practising the technique on patients. The median number of DREs performed was two, and 17% of students had performed none. The most often cited reason for not practising DRE was lack of a doctor chaperon. Difficulty organising DREs and perceived doctor and nurse obstruction were also commonly cited. Less than a quarter of students had palpated a prostate cancer, and less than a fifth a rectal tumour. There was a trend for students to feel more confident about DRE if more were practised.
The number of DREs performed compared unfavourably with the number found in a similar survey of final-year students at the University of Oxford medical school in 2000.5 This postal survey of 100 students (response rate, 71%) found that 58% of students had performed five or more DREs (versus 13% in our study), while 23% had performed 10 or more DREs (versus 8% in our study). However, the number of DREs performed by UK medical students may be decreasing, as a 1990 study in a London medical school found the median number of DREs performed to be 11–30.6 We have no historical Australian data with which to compare our results.
We found that 52% of students said their DRE findings were always confirmed by a supervising doctor, a higher proportion than found at Oxford (31% of students).5 However, only 19% of our students had palpated a rectal tumour, compared with 45% and 83% in the Oxford study and earlier London study, respectively,5,6 and only 24% of our students had palpated a prostate cancer, compared with 53% in the Oxford study.5
The balance between patients’ rights and the need of medical students to practise skills is never without concern. Our study results are consistent with previous findings suggesting that students are aware of ethical issues in relation to performing invasive examinations.10 In a British study, a quarter of intimate examinations were performed without patient consent.8 Students at our institution would appear about average in terms of gaining consent compared with students in overseas studies.8-10
Questionnaires are valid instruments for assessing knowledge, attitudes and behaviour.11 Although our questionnaire was not externally validated (indeed, no externally validated DRE questionnaire exists), it included five questions used in a previous survey of DRE to allow comparison.5 Conducting the study in person, by individuals not involved in assessing students, is likely to increase the accuracy of responses. While logbooks might provide more reliable data, they are time-consuming and expensive to keep and still open to inaccuracies. Finally, although we surveyed students from a single medical school, they had received their clinical teaching at hospitals across the State, broadening the applicability of the results.
Our clinical schools appear to be teaching DRE, but failing to give students the opportunity to practise it. An option is practising DRE after graduation, but how much this happens is influenced by attitudes acquired during training.12 Strategies are needed to help students acquire the skill of DRE before they graduate. The curriculum at the University of Melbourne has now been changed to emphasise practice of DRE and communication with patients about the examination.
Other possible strategies include:
Campaigns to encourage doctors and nurses to supervise students performing DRE. All teaching units must involve both doctors and nurses in teaching DRE and regularly re-emphasise its importance. Staff development educators, as used in nursing training to help staff actively foster students’ learning experiences,13 may also have a role.
A logbook quota system similar to that commonly used for procedures such as inserting intravenous lines and suturing.
Formal assessment of skill in DRE using a plastic model, as is done for gynaecological examination.
Appointment of teaching associates in DRE. Teaching associates are used for other types of intimate examination. They are trained in lecturing, simulation on models (including themselves), and communication, and provide tutorials, practice and immediate feedback to students on performance.14 A competency-based approach with assessment by trained supervisors has been shown to result in rapid acquisition of other clinical skills.15
The results of our study should stimulate critical appraisal of teaching and remind practitioners of their role in the medical “apprenticeship”. The quality of skills passed on depends on the enthusiasm and guidance of those who have gone before.
1 Palpation of prostate and abnormalities on digital rectal examination (DRE) among 222 final-year medical students
|
Never |
1–2 |
3–5 |
> 5 |
|||||||||||
How many times have you confidently felt a prostate on DRE? |
82 (37%) |
86 (39%) |
39 (17%) |
15 (7%) |
|||||||||||
How many times have you felt a clinically malignant prostate on DRE? |
169 (76%) |
48 (22%) |
3 (1%) |
2 (1%) |
|||||||||||
How many times have you felt a rectal tumour on DRE? |
179 (80%) |
40 (18%) |
2 (1%) |
1 (1%) |
|||||||||||
How many times have you felt faecal constipation? |
198 (89%) |
21 (9%) |
2 (1%) |
1 (1%) |
|||||||||||
- Nathan Lawrentschuk1
- Damien M Bolton2
- University of Melbourne, Austin Hospital, Melbourne, VIC.
We thank the Clinical Deans of the three clinical schools of the Faculty of Medicine, University of Melbourne, for allowing us to perform the study: Associate Professor B Crotty (Austin Hospital), Dr C Penfold (Royal Melbourne Hospital), and Associate Professor W Beswick (St Vincent’s Hospital). We would also like to thank the students for participating.
None identified.
- 1. Browse N. An introduction to the symptoms and signs of surgical disease. London: Edward Arnold, 1991: 415-418.
- 2. Makinen T, Tammela TL, Hakama M, et al. Prostate cancer screening within a prostate specific antigen range of 3 to 3.9 ng./ml.: a comparison of digital rectal examination and free prostate specific antigen as supplemental screening tests. J Urol 2001; 166: 1339-1342.
- 3. Carvalhal GF, Smith DS, Mager DE, et al. Digital rectal examination for detecting prostate cancer at prostate specific antigen levels of 4 ng/ml or less. J Urol 1999; 161: 835-839.
- 4. Dixon AR, Thornton-Holmes J, Cheetham NM. General practitioners’ awareness of colorectal cancer: a 10 year review. BMJ 1990; 301: 152-153.
- 5. Turner KJ, Brewster SF. Rectal examination and urethral catheterization by medical students and house officers: taught but not used. BJU Int 2000; 86: 422-426.
- 6. Hennigan TW, Franks PJ, Hocken DB, Allen-Mersh TG. Influence of undergraduate teaching on medical students’ attitudes to rectal examination. BMJ 1991; 302: 829.
- 7. Brixton Health. EpiCalc 2000. Version 1.02 [computerised program]. Brixton, UK: Brixton Books, 2000.
- 8. Coldicott Y, Pope C, Roberts C. The ethics of intimate examinations — teaching tomorrow’s doctors. BMJ 2003; 326: 97-101.
- 9. Beckmann CR, Spellacy WN, Yonke A, et al. Initial instruction in the pelvic examination in the United States and Canada, 1983. Am J Obstet Gynecol 1985; 151: 58-60.
- 10. Hicks LK, Lin Y, Robertson DW, et al. Understanding the clinical dilemmas that shape medical students’ ethical development: questionnaire survey and focus group study. BMJ 2001; 322: 709-710.
- 11. Johnston JM, Leung GM, Fielding R, et al. The development and validation of a knowledge, attitude and behaviour questionnaire to assess undergraduate evidence-based practice teaching and learning. Med Educ 2003; 37: 992-1000.
- 12. Hennigan TW, Franks PJ, Hocken DB, Allen-Mersh TG. Rectal examination in general practice. BMJ 1990; 301: 478-480.
- 13. Voignier RR, Freeman LH. Helping staff help students. J Nurs Staff Dev 1992; 8: 165-169.
- 14. Popadiuk C, Pottle M, Curran V. Teaching digital rectal examinations to medical students: an evaluation study of teaching methods. Acad Med 2002; 77: 1140-1146.
- 15. Martin M, Vashisht B, Frezza E, et al. Competency-based instruction in critical invasive skills improves both resident performance and patient safety. Surgery 1998; 124: 313-317.





Abstract
Objective: To assess the attitudes of final-year medical students to digital rectal examination (DRE) and their experience of performing DRE during clinical training.
Design: Questionnaire-based survey.
Setting and participants: All students in the final year of medical school at the University of Melbourne in 2003.
Outcome measures: Agreement with statements about attitude to DRE; number of DREs performed and abnormalities palpated; and ratings of frequency of supervision and perceived barriers to performing DRE.
Results: 222 of 256 students (87%) responded. Almost all (97%) believed that DRE is an essential requirement for a medical practitioner, and 94% that they should have the skill before graduating, while 92% said they had been taught how to perform it. The median number of DREs performed was two, with 17% of students performing none. Sixty-three per cent had palpated a prostate, 24% a prostate cancer, 19% a rectal tumour, and 11% faecal constipation. Half the students (52%) felt they could give a reasonable or confident opinion based on their DRE findings. The most often cited reason for not performing DREs was the lack of a doctor to act as a supervisor.
Conclusions: A concerted effort is needed from academics, supervising doctors and students to improve medical students’ proficiency in performing DRE and confidence about their findings.