The full spectrum of UVR can be classified into three groups, based on wavelength: ultraviolet A (UVA) (400–315 nm), ultraviolet B (UVB) (315–280 nm) and ultraviolet C (UVC) (280–100 nm).
Over 98% of solar UVR exposure is in the form of UVA. It penetrates the skin more deeply than UVB or UVC, but is less associated with DNA damage.1,2 This may mean that UVA is least likely to produce skin malignancies.
UVB accounts for less than 2% of our solar UVR exposure, as much of it is absorbed in the upper atmosphere. UVB is responsible for most of the DNA damage within skin cells, and arguably most of the resultant skin cancers.1,2
UVC exposure is insignificant for most people, as solar UVC is readily absorbed in the atmosphere before reaching the earth’s surface. Knowledge of the effects of UVC on skin is less clear, but it may be as dangerous to skin as UVB.2,3
Arc welding produces the full spectrum of UVR. The short distance between the arc and the welder’s skin may not be sufficient to absorb most of the UVB and UVC. Arc welders may therefore be at significantly increased risk of developing actinic skin and ocular damage, including malignancy, particularly if they have inadequate protection (Box 1). Furthermore, thermal burns from hot metal can occur when welding and contribute to this risk.4
A literature search was conducted in December 2003 using the PubMed (www.ncbi.nlm.nih.gov/PubMed) and Blackwell Synergy (www.blackwell-synergy.com/servlet/useragent?func=showHome) electronic databases. The key search terms used were basal cell carcinoma, squamous cell carcinoma, skin cancer, melanoma, weld, welding, arc, radiation and ultraviolet. We searched for all relevant material over the past 30 years.
Of the five articles we found that commented on cases of skin cancer possibly attributable to welding, only one was a case–control study of the risk of skin cancer from arc welding. This study, by Emmett et al,5 observed that welders often had skin erythema and small scars from burns, but did not find a link between welding and the development of skin cancer. Several features of the study are noteworthy. The researchers studied only one workplace, which was described as having “well run welding operations which use and enforce current safety standards”. The welders “predominantly welded mild steel”. Their average age was relatively young (43 years), and they had been working for the same employer for an average of 16.9 years (Box 2). As skin cancer often occurs decades after the significant UVR exposure, it is conceivable that the UVR skin damage experienced by workers in the study by Emmett et al had not yet manifested as malignancy. Furthermore, the study did not include examination for naevi. At the time, the relationship between atypical naevi and melanoma was not understood. We now recognise that multiple atypical naevi are associated with a significantly greater risk of developing melanoma.6
The evidence linking welding with ocular melanoma is more established. Case–control studies have shown that arc welders are at increased risk of developing ocular melanoma. Some have postulated that the increased exposure to UVR is the probable (but not definite) cause (Box 3).8-10
Factors that increase UVR exposure while welding include working close to the arc; increased arc energy, arc duration or electrical current; welding aluminium (as opposed to other metals, such as stainless steel or iron); and using argon as the shielding gas (rather than helium).11
UVR is produced by arc welding processes that include manual metal arc welding, gas tungsten arc welding, and gas metal arc welding (which emits the most radiation and is generally used for welding aluminium). It should be noted that not all welding processes involve striking an arc. Other forms of welding (eg, oxyacetylene, friction stir, resistance, friction, laser and electron-beam welding) produce minimal UVR.
Suitable means of protection from UVR exposure while arc welding include wearing protective gloves together with clothing that covers the arms and forearms down to the gloves. However, the radiant heat from welding can be quite uncomfortable, and welding on a hot day compounds the problem. Discarding heavy welders’ clothing and gloves in favour of short-sleeved shirts (unbuttoned at the top) exposes the hands, forearms, neck and manubrium to a considerably increased level of UVR (Box 3).
Wearing protective clothing while welding is a hindrance not only for full-time welders. Other tradespeople who perform welding occasionally (eg, motor mechanics) find it inconvenient to put on protective clothing, while sculptors and tradespeople doing highly intricate work also experience difficulty in achieving fine detail when wearing heavy clothing and thick gloves.
Furthermore, while welders are invariably trained in health and safety issues, assistants or other workers in the vicinity may not be aware of the possible risks.
Although there remain many unanswered questions regarding arc welding and skin cancer risk, certain principles should be considered in managing patients with skin cancer:
When patients with skin cancer deny a significant history of sun exposure, arc welding should be considered as a possible cause.
Welders should be advised about skin protection (using a combination of appropriate clothing and sunscreen) when welding. Some readily available sunscreens have broad-spectrum coverage that includes the full range of UVR. Workers welding aluminium should be advised that they are at greatest risk of exposure to artificial UVR and need heavy protection.
Large, well designed studies are needed to resolve the uncertainty about the risk of skin cancer from arc welding operations. Issues that should be considered in any future study include:
Examining senior career workers, who are likely to have accumulated greater welding UVR exposure;
Investigating workers using a variety of arc welding processes, welding parameters, shielding gases and metals;
Observing part-time welders who do not adequately protect themselves;
Examining for atypical naevi as well as actinic keratoses, non-melanoma skin cancer and melanoma, with histological confirmation of any suspicious lesions;
Consideration of other factors, such as skin type and background actinic damage from solar UVR.
2 Number of workers with malignant skin lesions, premalignant skin lesions or marked elastosis of the skin in a factory employing welders*5
Characteristic |
Welders (n = 77) |
Non-welders exposed to welding operations (n = 75) |
Other workers in same factory† (control group) (n = 58) |
||||||||||||
Average age of worker (years) |
43 |
48 |
44 |
||||||||||||
Melanoma |
0 |
0 |
1 |
||||||||||||
Actinic keratoses |
3 |
3 |
1 |
||||||||||||
History of skin cancer removal |
1 |
2 |
1 |
||||||||||||
Total malignant and premalignant lesions present or previously removed |
4 |
5 |
3 |
||||||||||||
Marked elastosis on the face |
6 |
3 |
0 |
||||||||||||
Marked elastosis on the neck |
10 |
5 |
3 |
||||||||||||
* There were no statistically significant differences between welders, non-welders with welding exposure, and the control group. † These workers never worked in the vicinity of welding operations. |
|||||||||||||||
3 Studies linking development of ocular malignancy with exposure to UVR
Study |
Finding |
Level of evidence7 |
|||||||||||||
Holly et al8 |
Case–control study of 221 patients with uveal melanoma. Welding exposure increased risk of developing intraocular melanoma (odds ratio [OR], 2.2; 95% CI, 1.3–3.5) |
III-2 |
|||||||||||||
Guenel et al9 |
Case–control study of 50 patients with uveal melanoma. Welders had an increased risk of ocular melanoma (OR, 7.3; 95% CI, 2.6–20.1) |
III-2 |
|||||||||||||
Vajdic et al10 |
Case–control study of 290 patients with ocular melanoma. Total UVR exposure, especially before age 40, increased life risk of ocular melanoma (OR, 1.8; 95% CI, 1.1–2.8 for the highest quarter of sun exposure up to age 40) |
III-2 |
|||||||||||||
UVR = ultraviolet radiation. |
|||||||||||||||
- 1. Horneck G. Quantification of biologically effective environmental UV irradiance. Adv Space Res 2000; 26: 1983-1994.
- 2. Ultraviolet radiation. World Health Forum 1995; 16: 110.
- 3. Merryman JI. Effects of ultraviolet C radiation on cellular proliferation in p53-/- keratinocytes. J Environ Pathol Toxicol Oncol 1999; 18: 1-9.
- 4. Ewing MR. The significance of a single injury in the causation of basal cell carcinoma of the skin. ANZ J Surg 1971; 41: 140-147.
- 5. Emmett EA, Buncher CR, Suskind RB, Rowe KW Jr. Skin and eye diseases among arc welders those exposed to welding operations. J Occup Med 1981; 23: 85-90.
- 6. Kelly JW, Yeatman JM, Regalia C, et al. A high incidence of melanoma found in patients with multiple dysplastic naevi by photographic surveillance. Med J Aust 1997; 167: 191-194.
- 7. National Health and Medical Research Council. How to use the evidence: assessment and application of scientific evidence. Canberra: NHMRC, 2000. Available at: www.health.gov.au/nhmrc/publications/pdf/cp69.pdf (accessed Jun 2004).
- 8. Holly EA, Aston DA, Ahn DK, Smith AH. Intraocular melanoma linked to occupations and chemical exposures. Epidemiology 1996; 7: 55-61.
- 9. Guenel P, Laforest L, Cyr D, et al. Occupational risk factors, ultraviolet radiation, and ocular melanoma: a case–control study in France. Cancer Causes Control 2001; 12: 451-459.
- 10. Vajdic CM, Kricker A, Giblin M, et al. Sun exposure predicts risk of ocular melanoma in Australia. Int J Cancer 2002; 101: 175-182.
- 11. Lyon T. Knowing the dangers of actinic ultraviolet emissions. Welding J 2002; 81: 28-30.





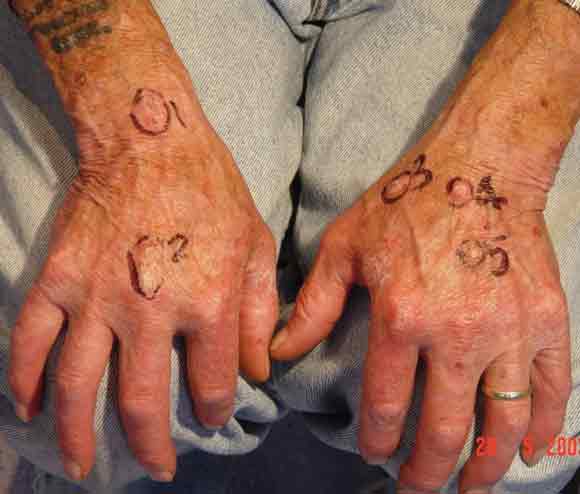

Abstract
Arc welding produces the full spectrum of ultraviolet radiation (UVR).
It is possible that welders are at greater risk of developing skin cancer than the general population, but there is a dearth of well designed studies in this area.
The only major study of the relationship between arc welding and skin cancer risk did not reveal an increased incidence of skin cancer in welders. As the welders examined were all well protected and the length-of-exposure period was limited, the findings cannot be generalised to all welders.
Studies have demonstrated that welding increases the risk of ocular melanoma.
Just as we urge the public to protect themselves from UVR, we need to consider similar advice for arc welders.