Rates of obesity among children have increased everywhere over the past 15 to 20 years. By 1997, about 16% of school-aged Australian boys and 18% of girls were overweight, and more than 5% of both sexes were obese, with a corresponding increase in median body mass index (BMI) and girth.1 Similar high prevalences are now evident in the preschool-age group.2 Of great concern, the increase in prevalence may be accelerating.1
Obesity is a major contributor to diabetes and cardiovascular disease, two of the national Health Priority Areas identified in the 1999 report on the burden of disease and injury in Australia.3 Most overweight and obese children will become overweight adults,4 already have risk factors for cardiovascular or diabetes-related illnesses,5,6 and face future morbidity and loss of life-years.7 Behaviour, as well as biology, is an important determinant of many adult diseases, including obesity.8 Therefore, developing healthier behaviours in childhood may be an important step in limiting adult obesity.
As for many chronic conditions, potential interventions range from universal preventive measures, through secondary (targeted) prevention, to tertiary management strategies for the child with established obesity. An effective population approach to childhood overweight and obesity is likely to require synergistic strategies across this spectrum.
How effective are universal prevention and tertiary management?
The results of universal prevention and tertiary management approaches have so far been disappointing, as evidenced by the continuing rise in prevalence of childhood overweight and obesity. Universal prevention may include public health measures aimed at institutional or structural factors beyond the control of individuals, or strategies enabling individuals to make healthier lifestyle choices.9 For children, this has so far translated mainly to school-based interventions, but only two of many trials have found such interventions successful in reducing BMI relative to controls.10,11 This may be because schools do not provide the level of access to parents needed for lasting behavioural change.12 Clearly, environmental and population strategies are vital in both schools and communities, but their effectiveness, reach and sustainability need to be improved.
At the other end of the spectrum, management of established childhood obesity is difficult, and successes are usually modest. Some progress has been made in “unpacking” effective ways of helping children modify energy intake and increase physical activity, and some family-based strategies for paediatric obesity have had durable (up to 10 years), although fairly small, impacts.13 However, the intensity and cost of these interventions is likely to limit their availability for the vast majority of families.
What is the role of secondary prevention?
Twenty per cent or more of school-aged children are overweight or mildly obese — a readily identifiable major risk factor for their future health and longevity. An effective secondary prevention program would need to regularly access virtually all these children, and only two settings meet this criterion — schools and primary care. Although some targeted school-based programs have shown limited effectiveness,14 they raise issues of stigmatisation, availability, acceptability, family involvement, and sustainability. The only other real option is primary care.
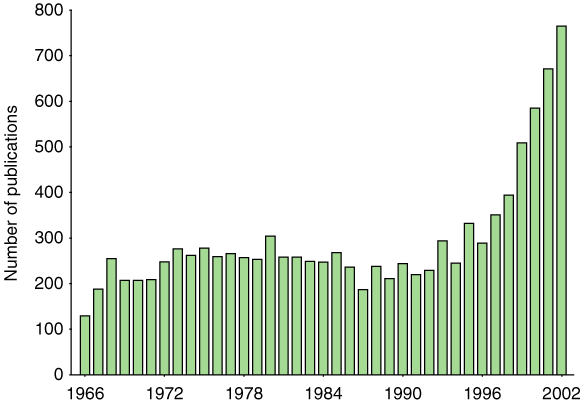
Research into a primary care approach: Tackling childhood overweight in primary care seems an unlikely issue to debate; surely we should just do it? A primary care approach has been advocated in several recent articles15-17 and (enthusiastically) in the 2003 guidelines from the National Health and Medical Research Council.18 Yet, research to demonstrate efficacy of this approach is negligible. We searched Medline in October 2003, using the MeSH heading “Obesity” (which subsumes the search term “Overweight”), with the search limited to (human and all children 0 to 18 years). This revealed a rapid and steepening increase in publications since 1995 (Box). However, limiting this search by the MeSH headings “Primary Health Care” (which subsumes “Primary Care”), “Family Practice”, and “Physicians, Family” (including the text term “general pract*”) yielded just 74 articles since 1966. Of these, 22 dealt with children aged under 18 years, only one of which reported a controlled trial — with short-term follow-up of 44 adolescents (23 in the intervention group).19
Similarly, searches in October 2003 of the Cochrane Central Register of Controlled Trials, the register of trials with an International Standard Randomised Controlled Trial Number (ISRCTN Register) and the metaRegister of Controlled Trials (the last two available at www.controlled-trials.com) revealed no relevant trials currently under way. Compared with universal and tertiary approaches, primary care trials targeting pre-adolescent school-aged children seem barely on the research radar.
Barriers to a primary-care approach: In Australia, general practitioners (GPs) are the only universally accessible and funded primary healthcare providers available to all school-aged children. Little is known about how often GPs tackle this issue in children, but, extrapolating from the experiences of obese adults (BMI ≥30 kg/m2),20 we can assume that families of most overweight or obese children are not proactively counselled. The following barriers to primary care practitioners tackling this issue have been identified:
primary care settings are not usually equipped for group interventions;
few providers feel competent in the use of behaviour-modification strategies;
the time available may not suffice to identify the targets and strategies for behavioural change;
no widely accepted successful treatment models exist; and
reimbursement for the treatment of overweight children is limited.21
The list might also include fear of harm to patients in cultures wary of eroding self-esteem and promoting eating disorders. Unlike obese adults, most of whom recognise that they should lose weight,22 parents of overweight primary school children mostly report that they are not concerned about their child’s weight,23 which may also deter GPs from taking a proactive approach. Yet, there are good reasons to try this approach.
Arguments for a primary care approach: Primary care interventions have been effective in adults for problems such as smoking, alcohol misuse and coronary heart disease, while primary care research on promoting physical activity in adults is promising.24 This is relevant to overweight in young children, as interventions are likely to be largely directed at parents to achieve family change. There is also evidence that relatively brief primary care interventions are as effective as more intensive interventions in promoting physical activity in adults.25
Furthermore, an educational intervention for primary care doctors was effective in achieving sustained improvements in their knowledge, skill and self-perceived competence in adolescent care.26 Finally, many primary school children attending GPs are overweight or obese, and they attend GPs frequently. For example, 35% of 6–11-year-olds in a cohort of more than 30 000 children attending American primary care practices were overweight or obese.27 In our study of 3000 Victorian children, parents reported that 55% of overweight children had attended a GP once or twice in the preceding 6 months, and 22% three or more times.28
We now understand enough about the behavioural determinants of child obesity and effective management to suggest what should be targeted, such as limiting television viewing, encouraging outdoor play, and limiting consumption of sugar-sweetened soft drinks.29 Interventions need to be brief and not resource-intensive so that they can be incorporated readily into a busy GP’s routine practice. Therefore, GPs would also need to master specific techniques for complex behaviour change, such as motivational interviewing or brief, solution-focused therapy, and be able to broach potentially sensitive issues with parents.
Over the past 24 months, the LEAP (Live, Eat and Play) team has been conducting a multipractice, randomised controlled trial for the secondary prevention of overweight and obesity in Melbourne children. Thirty-five GPs serving families across the sociodemographic range have attended LEAP training and found it useful. Among 2112 children aged 5–10 years attending these GPs, 28% were overweight or obese. The families of nearly half these children agreed to enter the study, and most completed the schedule of four pre-agreed consultations, with little evidence of psychological harm.
More problematic is diagnosis of overweight. We found that few GPs routinely weigh and measure children attending their practices, let alone ascertain BMI status, and many do not have equipment accurate enough to track changes over time. In this light, the new National Health and Medical Research Council recommendation that GPs chart the BMI of all children and adolescents every 6 months18 seems a pipe dream.
Rigorous trials are needed to determine whether secondary prevention in primary care is useful in the fight against the childhood obesity epidemic. Secondary prevention could equally be delivered by other primary healthcare professionals, such as nurses, dietitians and exercise specialists, should they achieve accessibility and funding stability equal to that of GPs. Ideally, their relative effectiveness should also be studied. Whoever delivers the care, we must know whether brief interventions to reduce BMI through logical, sustainable lifestyle changes do more good than harm, and what are the sustainability and costs of such programs.
- Melissa A Wake1
- Zoë McCallum2
- Centre for Community Child Health, Murdoch Children’s Research Institute, Melbourne, VIC.
M A W and Z M are principal investigators on the LEAP (Live, Eat and Play) randomised controlled trial (ISRCTN 45068927), funded by the Australian Health Ministers’ Advisory Council. Z M is supported by a National Health and Medical Research Council Postgraduate Research Scholarship.
None identified.
- 1. Booth ML, Chey T, Wake M, et al. Change in the prevalence of overweight and obesity among young Australians, 1969-1997. Am J Clin Nutr 2003; 77: 29-36.
- 2. Tennant S, Hetzel D, Glover J. A social health atlas of young South Australians. Adelaide: Public Health Information Development Unit, 2002.
- 3. Mathers E, Vos T, Stevenson C. The burden of disease and injury in Australia. Canberra: Australian Institute of Health and Welfare, 1999. (Catalogue No. PHE-17.)
- 4. Whitaker RC, Wright JA, Pepe MS, et al. Predicting obesity in young adulthood from childhood and parental obesity. N Engl J Med 1997; 337: 869-873.
- 5. Freedman DS, Dietz WH, Srinivasan ST, Berenson GS. The relation of overweight to cardiovascular risk factors among children and adolescents: the Bogalusa Heart Study. Pediatrics 1999; 103: 1175-1182.
- 6. Steinberger J, Moran A, Hong CP, et al. Adiposity in childhood predicts obesity and insulin resistance in young adulthood. J Pediatr 2001; 138: 469-473.
- 7. Fontaine KR, Redden DT, Wang C, et al. Years of life lost due to obesity. JAMA 2003; 289: 187-193.
- 8. Rivara FP, Whitaker R. Influencing the childhood behaviors that lead to obesity. Arch Pediatr Adolesc Med 2003; 157: 719-720.
- 9. Kumaniyika SK. Minisymposium on obesity: overview and some strategic considerations. Annu Rev Public Health 2001; 22: 293-306.
- 10. Robinson TN. Reducing children’s television viewing to prevent obesity: a randomized controlled trial. JAMA 1999; 282: 1561-1567.
- 11. Gortmaker SL, Peterson K, Wiecha J, et al. Reducing obesity via a school-based interdisciplinary intervention among youth: Planet Health. Arch Pediatr Adolesc Med 1999; 153: 409-418.
- 12. NHS Centre for Reviews and Dissemination. The prevention and treatment of childhood obesity. Effective Health Care 2002; 7: 1-12.
- 13. Summerbell CD, Waters E, Edmunds L, et al. Interventions for treating obesity in children (Cochrane Review). In: The Cochrane Library, Issue 3, 2003. Oxford: Update Software.
- 14. Summerbell CD, Ashton V, Campbell KJ, et al. Interventions for treating obesity in children (Cochrane Review). In: The Cochrane Library, Issue 1, 2004. Chichester, UK: John Wiley & Sons, Ltd.
- 15. Drohan SH. Managing early childhood obesity in the primary care setting: a behavior modification approach. Pediatric Nursing 2002; 28: 599-610.
- 16. Dietz WH, Nelson A. Barriers to the treatment of childhood obesity: a call to action. J Pediatr 1999; 134: 535-536.
- 17. Whitaker RC. Obesity prevention in pediatric primary care. Arch Pediatr Adolesc Med 2003; 157: 725-727.
- 18. National Health and Medical Research Council. Clinical practice guidelines for the management of overweight and obesity in children and adolescents. Canberra: Commonwealth of Australia, 2003.
- 19. Saelens BE, Sallis JF, Wilfley DE, et al. Behavioral weight control for overweight adolescents initiated in primary care. Obes Res 2002; 10: 22-32.
- 20. Galuska D, Will J, Serdula M, Ford E. Are health care professionals advising obese patients to lose weight? JAMA 1999; 282: 1576-1578.
- 21. Dietz WH, Nelson A. Barriers to the treatment of childhood obesity: a call to action. J Pediatr 1999; 134: 535-536.
- 22. Little P. GP documentation of obesity: what does it achieve? Br J Gen Pract 1998; 48: 890-894.
- 23. Wake M, Waters E, Salmon L, et al. Parent-reported health status of overweight and obese Australian primary school children: a cross-sectional population survey. Int J Obes 2002; 26: 717-724.
- 24. Eden KB, Orleans CT, Mulrow CD, et al. Clinician counseling to promote physical activity. File Inventory, Systematic Evidence Review Number 9. August 2002. Rockville, Md: Agency for Healthcare Research and Quality. Available at: www.ahrq.gov/clinic/prev/phsacinv.htm (accessed Mar 2004).
- 25. King AC. Two year results of the activity counselling trial (ACT). Int J Behav Med 2000; 7: 188.
- 26. Sanci LA, Coffey CM, Veit FCM, et al. Evaluation of the effectiveness of an educational intervention for GPs in adolescent health care: a randomised controlled trial. BMJ 2000; 320: 224-229.
- 27. Gauthier BM, Hickner JM, Ornstein S. High prevalence of overweight children and adolescents in the Practice Partner Research Network. Arch Pediatr Adol Med 2000; 154: 625-628.
- 28. Wake M, Waters E, Salmon L, et al. Parent-reported health status of overweight and obese Australian primary school children: a cross-sectional population survey. Int J Obesity 2002; 26: 717-724.
- 29. Whitaker RC. Obesity prevention in pediatric primary care. Arch Pediatr Adolesc Med 2003; 157: 725-727.





Abstract
At least a quarter of primary school children in Australia are overweight or obese; the long-term impacts are likely to include chronic morbidity and loss of life-years.
Universal preventive strategies have so far had limited effectiveness, while secondary and tertiary referral services would be overwhelmed if they attempted to systematically manage a problem with such high prevalence.
Primary care services could play an important role in secondary prevention of overweight and mild obesity in children.
While reports of child obesity research have burgeoned since 1995, effectiveness trials of primary care interventions in primary-school-aged children have been neglected.
Randomised controlled trials of a primary care approach, although challenging, are essential to determine whether it does more good than harm.