A growing awareness of the physical health needs of people with psychotic disorders has led to concern about their high prevalence of diabetes and “subclinical” abnormalities of glucose metabolism, such as impaired glucose tolerance.1 Concern has been expressed in recent years that the newer antipsychotic medications may have accelerated the development of diabetes in these people. The dilemma facing medical practitioners relates, on the one hand, to the high rate of medical comorbidity in people with psychosis, perhaps amplified by antipsychotic treatment, and, on the other hand, to the enhanced benefits of the newer agents in the management of the psychosis. Complicating the issue is the fact that people with psychosis are not very good advocates for their own medical health, and may face many barriers to adequate screening and treatment of medical problems, including diabetes.
To facilitate the optimal medical care of hyperglycaemia-related illness in people with psychosis in Australia, an expert group was convened to develop a consensus statement. The group was drawn from the disciplines of psychiatry, endocrinology, epidemiology, general practice, mental health nursing, and pharmacy, along with representatives of community and non-government organisations (see Acknowledgements). The group reviewed the relevant literature, developed a series of draft statements and subjected these to peer review by external consultants to arrive at a broadly accessible set of guidelines. After this process, representatives from the peak consumer and carer organisations across Australia met to develop a consumer-based initiative extending from the consensus document. The aim was to provide the impetus for change in the care of people with psychosis and potential metabolic-related medical comorbidity using simultaneous top-down and bottom-up approaches.
A number of important principles emerged. First, successful and optimal treatment of the psychotic disorder has priority. The advent of second-generation antipsychotic medications has allowed more effective and better-tolerated treatment of psychotic illnesses. Second, all people taking antipsychotic medication should be screened for diabetic risk. Protocols were suggested to help clinicians ensure that people with psychotic disorders receive appropriate and timely management of their physical disorders. This may sometimes require a more assertive approach than is currently the case. Finally, all health professionals involved in the care of a patient with a psychotic disorder, including the psychiatrist in charge, can contribute to the care of physical disorders, including diabetes and obesity. Consistent advice should be provided on diet, exercise and smoking, and the psychiatric team should assume responsibility for ensuring appropriate screening is undertaken, in close liaison with other healthcare providers.
Here, we outline the main findings of the consensus group. The full consensus statements for professionals and for consumers and carers are available at www.psychiatry.unimelb.edu.au/open/diabetes_consensus/.
Many case reports and series and a few larger studies based on administrative databases have described associations between antipsychotic treatment and the onset or exacerbation of diabetes.2-5 However, there are no long-term, randomised controlled trials to guide clinical practice in this area. The existing evidence suggests that the introduction of first-generation antipsychotic medications (FGAs, see Box 1) was associated with a two- to threefold increase in the prevalence of diabetes among treated patients6,7 (Level III evidence [derived from pseudorandomised controlled trials, comparative studies, single-arm studies or interrupted time series without a parallel control group8]). It also suggests that the obesity rate (and, by inference, potential for diabetes) is much higher in patients treated with depot FGAs than in the general population.9 The introduction of second-generation antipsychotic medications (SGAs, see Box 1) was associated with a further increase, variously estimated at 10%–50%10 (Level III evidence,Box 2). The contribution of improved screening for disorders of glucose metabolism is not known but this represents a potential artefact.
A group of American organisations led by the American Diabetes Association recently published the outcomes of a consensus development conference on antipsychotic drugs, obesity and diabetes.13 The conference recognised that SGAs are associated with adverse effects, including obesity, diabetes and dyslipidaemia. It concluded that clozapine and olanzapine are associated with greater weight gain and a higher occurrence of diabetes and dyslipidaemia than risperidone and quetiapine, which appeared to have intermediate effects. Aripiprazole and ziprasidone (not available in Australia) did not appear to be associated with significant weight gain, diabetes or dyslipidaemia, although they had not been used as extensively as the other agents. The conference recommended baseline screening and ongoing monitoring for the development of significant weight gain, dyslipidaemia and diabetes.
The American Food and Drug Administration (FDA) recently requested that all SGA manufacturers include a warning and additional information about a link between SGAs and hyperglycaemia and also recommended regular monitoring of blood glucose level. The FDA acknowledged that the relationship between SGAs and glucose abnormalities is complicated by an increased background risk of diabetes in people with schizophrenia and the growing incidence of diabetes in the general population.12
There have been case reports of apparent diabetic ketoacidosis occurring during treatment with SGAs. While this can be life-threatening, its incidence has not been clearly established. The full consensus document outlines the relevant literature for further consideration.
Antipsychotic medication can be both life-enhancing and life-saving for sufferers of psychosis. The Australian consensus group recognised that successful treatment of the psychotic disorder has priority over concerns about potential metabolic consequences. The latter need to be dealt with in their own right after the total risks and benefits of antipsychotic therapy have been estimated.14 Thus, selection of an antipsychotic medication for a particular patient should be driven more by its capacity to reduce psychiatric symptoms than its diabetic potential alone, particularly in the absence of definitive information about causality and risk.15
The consensus group considered that pre-existing diabetes may be a relative contraindication to the prescription of medications which are known to have adverse short-term effects on weight and metabolism. However, it is not an absolute contraindication, as effective treatment of the psychosis should be the primary aim.
Because of the high prevalence of hyperglycaemia, informed consent should be obtained from patients or their guardians, with acknowledgement of the requirement to monitor for diabetes.
The importance of weight gain to the development of type 2 diabetes is detailed in the recent American Diabetes Association position statement.13 A hierarchy of potential short-term weight gain exists among antipsychotic medications16 (Level II evidence [obtained from at least one properly designed randomised controlled trial]8). The advent of new SGAs might lead to fewer adverse metabolic consequences, but long-term “real world” data are lacking.
In the longer term, obesity seems to be less related to specific medications and more to behavioural factors, including diet and exercise. These relationships have been described in the “hare and tortoise” theory of antipsychotic-mediated weight gain.17 This theory suggests that some medications have the propensity to drive weight gain rapidly (the “hares”), while most others have a lesser potential that nonetheless results in weight gain in the longer term because of the interactions with the disease process itself and its social consequences (the “tortoises”). However, non-controlled descriptions of cross-sectional weight gain cannot be used to test hypotheses, and a prospective study of a controlled cohort from inception of antipsychotic treatment is required. People with psychosis are undoubtedly at risk of diabetes, but factors other than medication contribute to adverse metabolic outcomes. There is no evidence that people with psychosis are less vulnerable to the effects of obesity, and some evidence that they may be more vulnerable.
More research is required on the hypothesis that amelioration of psychiatric symptoms during treatment with medications such as clozapine and olanzapine is associated with the extent of weight gain.18 A proposed mechanism for a link involves a direct interaction between orexin peptides and dopamine systems in the prefrontal cortex.19 This suggests that, at least for some medications, weight gain may be a marker of decrease in symptoms.
A recent study found that, compared with a control group (without psychiatric illness, who were matched on parameters such as exercise level), people with unmedicated schizophrenia had an increased incidence of central obesity (a risk factor for cardiovascular disease and diabetes) and higher levels of plasma cortisol.20 Previous exposure to antipsychotic medications did not appear to influence the findings, as both medication-naive and medication-free patients had equally high levels of visceral fat. The findings suggested that the schizophrenic illness itself influenced fat distribution and associated risks.
There is no evidence that the natural history of diabetes differs between people with psychotic disorders or other mental illness and those without such disorders. However, people living with a psychotic disorder have a higher rate of other cardiovascular risk factors, including smoking and features of the metabolic syndrome, which are associated with weight gain and include hypertension and dyslipidaemia. These factors may contribute to a high rate of cardiovascular mortality. Premature mortality from medical disorders is well described among people with psychosis.1
The World Health Organization Global Burden of Disease Study estimated that, in 1990, psychiatric disorders accounted for five of the leading 10 causes of disability-adjusted life-years lost in people aged 15–44 years.21 Direct healthcare costs and indirect costs associated with schizophrenia are estimated at 0.3%–2% of gross domestic product in developed countries.22,23 People with diabetes are four times more costly to the national health system than those without the disorder. Therefore, the high prevalence of diabetes in psychotic disorders suggests that, from an economic perspective alone, particular attention is needed to this form of comorbidity.
In Australia, mental health is identified as a National Health Priority Area in its own right and as a major theme across all other National Health Priority Areas, which include diabetes and vascular disease. The National Health Priorities Area Action Council has commissioned programs to ensure not only that the common mental health needs of those with physical conditions such as diabetes are recognised, but also that the physical health needs of those with specific mental illnesses such as schizophrenia are identified. Key non-government groups, such as the Mental Health Council of Australia, have also prioritised the need to improve the physical healthcare of those with mental illness.24
Recent reforms in mental health service delivery under the Better Outcomes in Mental Health Care initiative (2001–2004) provide new opportunities for promoting integrated physical and mental healthcare, based largely on expanded services and improved quality of mental healthcare by Australian general practitioners. The recognition and active management of diabetes in people with psychotic illness could be specifically targeted for attention under this strategy. Obesity and diabetes continue to increase in the general population, despite the efforts of the healthcare system to alter dietary and exercise habits. Barriers to healthcare in people with psychotic illness accentuate this.1
The National Health and Medical Research Council has developed draft guidelines on population screening for diabetes.25 These recommend more intensive screening of some groups within the population known to be at higher risk, for example on the basis of family history, ethnicity, age, a history of gestational diabetes, or other risk factors.
People with psychotic illnesses are such a high-risk group.1 They should be monitored for the metabolic syndrome (also known as metabolic syndrome X, comprising obesity, hyperinsulinaemia, dyslipidaemia, and hypertension27) and for diabetes. Monitoring is required when initiating antipsychotic treatment, increasing the dose or changing antipsychotic medication and also during continuing treatment.
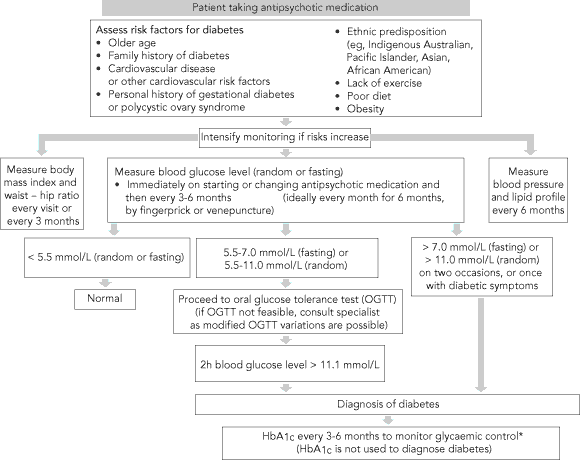
An algorithm for monitoring glucose metabolism in people treated with antipsychotic medication is shown in Box 3. Ideally, fasting or random blood glucose levels should be assessed monthly for 6 months after initiating or changing antipsychotic therapy, then at least twice yearly. In cases where there are repeated changes in the antipsychotic medication or dose, clinical judgement on appropriate glucose monitoring will be required. In any case, blood glucose measurements should be obtained a minimum of twice yearly. Laboratory blood glucose measurements or finger-prick measurements using a blood glucose meter are acceptable.
The consensus statement recognises the importance of early identification of abnormal glucose metabolism to assist in targeting preventive measures. Improved diet and increased physical activity in middle-aged, overweight members of the general population can reduce the progression of pre-diabetic states to diabetes,27 and the United Kingdom Prospective Diabetes Study demonstrated that appropriate treatment of diabetes reduces complications.28 There is little evidence on the effects of such interventions in people with psychotic disorders, but pilot studies indicate that exercise programs and dietary counselling can lead to healthier behaviours and improve a range of health outcomes.29
Exercise and dietary change can improve metabolic parameters even in the absence of weight loss. Thus, prevention of diabetes can be adopted as an objective which is independent of efforts to prevent or treat obesity. Practically, a range of approaches could be adopted for preventing diabetes in people with psychotic illness, from a “top down” approach within mental health services, through to approaches to individual patients by members of multidisciplinary teams. Medicare Benefits Schedule item numbers for enhanced primary care by general practitioners can facilitate an integrated approach to physical healthcare at the patient level. Modalities such as patient-held medical records could assist with monitoring of diabetes and coordination of preventive interventions.
Whether psychosis itself increases the risk of diabetes, and whether specific antipsychotic medications have differential effects on glucose metabolism during long-term use, remains uncertain, and the mechanisms of any such links remain obscure. Evidence on the effects of diabetes, the benefits of treatment and the benefits of preventive activities are derived almost entirely from the general population. Even when specific evidence is derived from people with psychotic disorders, those recruited into trials are not necessarily representative of those in the community. Given the very substantial public health consequences of diabetes in those with psychotic disorders, programs evaluating relative risks, strategies for improving outcomes, and the development of education and training programs for service providers, consumers and carers, remain a high priority.
1 Glossary
First-generation antipsychotic medications (FGAs): These are also known as “typical” or “conventional” antipsychotic medications. The prototypical agent, chlorpromazine, was first used in the mid-1950s. Other medications in this class include fluphenazine, thioridazine, haloperidol, droperidol, flupenthixol and zuclopenthixol.
Second-generation antipsychotic medications (SGAs): These are also known as “a typical” antipsychotic medications. The prototypical agent, clozapine, was first used in Australia in the mid-1990s. Other members of the class available in Australia are amisulpride, aripiprazole, olanzapine, quetiapine and risperidone.
Impaired glucose metabolism: A general term encompassing diabetes and the “pre-diabetic” disorders of impaired glucose tolerance (IGT, characterised by normal fasting blood glucose level but elevated 2-hour glucose level on the oral glucose tolerance test) and impaired fasting glucose (IFG, elevated fasting glucose level but normal 2-hour result on the oral glucose tolerance test).
Glycosylated haemoglobin (HbA1c): A marker of long-term glycaemic control, expressed as a percentage. The average blood glucose level in the past 60 days can be estimated with the formula (HbA1c × 2) − 6.0 mmol/L.
2 Estimated prevalence of diabetes before and after development of antipsychotic medications
Era |
Rate in people with psychosis |
Population rate |
|||||||||||||
Pre-antipsychotic medications |
2.5%–4.2%6,7 |
Unknown |
|||||||||||||
First-generation antipsychotics (since 1952) |
17%6 |
3.4% (Busselton, 1981)11 |
|||||||||||||
Second-generation antipsychotics (since 1990) |
19%10 |
7.5% (Australia, 2000)12 |
|||||||||||||
- Tim J R Lambert1
- Leon H Chapman2
- 1 Office for Psychiatric Evaluation and Educational Newmedia, University of Melbourne, Royal Melbourne Hospital, VIC.
- 2 International Diabetes Institute, Melbourne, VIC.
The consensus documents (professional and consumer) were developed with an unrestricted educational grant from Eli Lilly Australia. The company did not participate in any meetings, nor exert any editorial influence on the consensus statements. The co-chairs also thank the consensus group and the external consultants who provided so much of their time to the project. Participants in the project were:
Consensus working group: Mr Simon Bell (pharmacist, Sydney), Dr Nicholas Carr (general practitioner, Melbourne), Dr Leon Chapman (co-chair; diabetologist, Melbourne), Dr Michael D’Emden (endocrinologist, Brisbane), Mr Steven Elsom (mental health nurse, Melbourne), Dr Grace Groom (Mental Health Council of Australia, Canberra), Professor Scott Henderson (psychiatrist, Canberra), Professor Ian Hickie (psychiatrist, Sydney), Associate Professor Linda Hoffman (endocrinologist, Hobart), Associate Professor Tim Lambert (co-chair; psychiatrist, Melbourne), Dr Alan Rosen (psychiatrist, Sydney), Professor Bruce Singh (psychiatrist, Melbourne), Professor Tim Welborn (endocrinologist, Perth), Dr Peter Wynn Owen (psychiatrist, Perth).
Consultant review group: Mr John Bell (pharmacist, Sydney), Dr Elsa Bernardi (psychiatrist, Sydney), Dr Grant Blashki (general practitioner, Melbourne), Professor Vaughan Carr (psychiatrist, Newcastle), Professor David Castle (psychiatrist, Melbourne), Professor Stanley Catts (psychiatrist, Brisbane), Professor Donald Chisholm (endocrinologist, Sydney), Professor Michael Clinton (clinical nurse, Perth), Professor David Copolov (psychiatrist, Melbourne), Ms Linda Fellows (pharmacist, Perth), Mr Tony Fowke (National Consumer and Carer Forum, Perth), Associate Professor Tim Greenaway (endocrinologist, Hobart), Professor Mark Harris (general practitioner, Sydney), Ms Brenda Happell (clinical nurse, Melbourne), Dr Dan Haupt (Washington State University, USA), Ms Barbara Hocking (SANE Australia, Melbourne), Professor Assen Jablensky (psychiatrist, Perth), Professor Jayashri Kulkarni (psychiatrist, Melbourne), Dr Johanna Lammersma (psychiatrist, Adelaide), Ms Janet Meagher (National Consumer and Carer Forum, Sydney), Dr John Newcomer (Washington State University, USA), Professor Saxby Pridmore (psychiatrist, Hobart), Mr Rob Ramjan (Schizophrenia Fellowship of NSW, Sydney), Associate Professor Geoff Riley (psychiatrist, Fremantle), Ms Liz Stewart (National Consumer and Carer Forum, Sydney), Dr Julie Thompson (general practitioner, Moe), Mr Keith Wilson (Mental Health Council of Australia, Fremantle).
Carer and consumer groups: Association of Relatives and Friends of the Mentally Ill (ARAFMI), GROW Self Help/Mutual Help Groups, Australian Mental Health Consumer Network (AMHCN), Carers Australia, Consumers Health Forum, beyondblue: the national depression initiative, state representatives (carer and consumer) from the Australian Capital Territory, New South Wales, Northern Territory, Queensland, South Australia, Western Australia and Tasmania.
T J R L was paid an honorarium to attend the initial consensus meeting. He has served on advisory boards for Janssen-Cilag, Eli Lilly, Pfizer, Lundbeck, Sanofi, Novartis and Faulding; has received funding for unrestricted research from Eli Lilly, Novartis, Janssen-Cilag, Bristol-Myers Squibb, Pfizer and AstraZeneca; and has received travel assistance to attend meetings from Eli Lilly, Novartis, Janssen-Cilag, AstraZeneca and Bristol-Myers Squibb.
- 1. Lambert T, Velakoulis D, Pantelis C. Medical comorbidity in schizophrenia. Med J Aust 2003; 178 (9 Suppl 5): S67-S70. <MJA full text>
- 2. Newcomer J, Haupt D, Fucetola R, et al. Abnormalities in glucose regulation during antipsychotic treatment of schizophrenia. Arch Gen Psychiatry 2002; 59: 337-345.
- 3. Gianfrancesco F, Grogg A, Mahmoud R, et al. Differential effects of risperidone, olanzapine, clozapine, and conventional antipsychotics on type 2 diabetes: findings from a large health plan database. J Clin Psychiatry 2002; 63: 920-930.
- 4. Henderson D, Ettinger E. Schizophrenia and diabetes. Int Rev Neurobiol 2002; 51: 481-501.
- 5. Livingstone C, Rampes H. Atypical antipsychotic drugs and diabetes. Practical Diabetes Int 2003; 20: 327-331.
- 6. Thonnard-Neumann E. Phenothiazines and diabetes in hospitalized women. Am J Psychiatry 1968; 124: 978-982.
- 7. McKee H, D’Arcy P, Wilson P. Diabetes and schizophrenia — a preliminary study. J Clin Hosp Pharmacol 1986; 11: 297-299.
- 8. National Health and Medical Research Council. A guide to the development, implementation and evaluation of clinical practice guidelines. Canberra: NHMRC, 1999.
- 9. Silverstone T, Smith G, Goodall E. Prevalence of obesity in patients receiving depot antipsychotics. Br J Psychiatry 1988; 153: 214-217.
- 10. Sernyak MJ, Leslie DL, Alarcon RD, et al. Association of diabetes mellitus with use of atypical neuroleptics in the treatment of schizophrenia. Am J Psychiatry 2002 ;159: 561-566.
- 11. Glatthaar C, Welborn TA, Stenhouse NS, Garcia-Webb P. Diabetes and impaired glucose tolerance. A prevalence estimate based on the Busselton 1981 survey. Med J Aust 1985; 143: 436-440.
- 12. Dunstan D, Zimmet P, Welborn T, et al. The rising prevalence of diabetes and impaired glucose tolerance: the Australian Diabetes, Obesity and Lifestyle Study. Diabetes Care 2002; 25: 829-834.
- 13. American Diabetes Association, American Psychiatric Association, American Association of Clinical Endocrinologists, North American Association for the Study of Obesity. Consensus development conference on antipsychotic drugs and obesity and diabetes. Diabetes Care 2004; 27: 596-601.
- 14. Lambert T, Castle D. Pharmacological approaches to the management of schizophrenia. Med J Aust 2003; 178 (9 Suppl 5): S57-S61. <MJA full text>
- 15. Koller E, Cross J, Doraiswamy P, Schneider B. Risperidone-associated diabetes mellitus: A pharmacovigilance study. Pharmacotherapy 2003; 23: 735-744.
- 16. Allison D, Mentore J, Heo M, et al. Antipsychotic-induced weight gain: a comprehensive research synthesis. Am J Psychiatry 1999; 156: 1686-1696.
- 17. Lambert T. Hares and tortoises: long-term antipsychotic-associated weight gain. In: 7th Biennial Australian Schizophrenia Conference; 24-26 Oct 2002; Sydney, NSW.
- 18. Meltzer H. Putting metabolic side effects into perspective: Risks versus benefits of atypical antipsychotics. J Clinical Psychiatry 2001; 62 Supplement 27: 35-39.
- 19. Fadel J, Bubser M, Deutch A. Differential activation of orexin neurons by antipsychotic drugs associated with weight gain. J Neuroscience 2002; 22: 6742-6746.
- 20. Thakore J, Mann J, Vlahos A, et al. Increased visceral fat distribution in drug-naive and drug-free patients with schizophrenia. Int J Obesity 2002; 26: 137-141.
- 21. Murray C, Lopez A, editors. The global burden of disease: a comprehensive assessment of mortality and disability from diseases, injuries and risk factors in 1990 and projected to 2020. Cambridge, MA: Harvard University Press, 1996.
- 22. Knapp M. Costs of schizophrenia. Br J Psychiatry 1997; 171: 509-518.
- 23. Access Economics. Schizophrenia: costs. An analysis of the burden of schizophrenia and related suicide in Australia. Melbourne: SANE Australia; 2002.
- 24. Groom G, Hickie I, Davenport T. Out of hospital, out of mind: a report detailing mental health services in Australia in 2002 and community priorities for national mental health policy for 2003-2008. Canberra: Mental Health Council of Australia; 2003.
- 25. National Health and Medical Research Council. A guide to the development, implementation and evaluation of clinical practice guidelines. Canberra: NHMRC, 1999. Available at: www.health.gov.au/nhmrc/publications/pdf/cp30.pdf (accessed 2004).
- 26. Ryan M, Thakore J. Physical consequences of schizophrenia and its treatment: the metabolic syndrome. Life Sci 2002; 71: 239-257.
- 27. Tuomilehto J, Lindstrom J, Eriksson J, et al. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 2001; 344: 1343-1350.
- 28. American Diabetes Association. Implications of the United Kingdom Prospective Diabetes Study. Diabetes Care 2000; 23 Supplement 1: S27-S31.
- 29. Aquila R. Management of weight gain in patients with schizophrenia. J Clin Psychiatry 2002; 63 Suppl 4: 33-36.





Abstract
Psychotic illness and its treatment are associated with an increased rate of diabetes and worsening blood sugar control.
The newer, second-generation antipsychotic agents are more likely to produce this effect than the first-generation agents, but both contribute to the problem.
The effect is usually related to insulin resistance through weight gain, but other mechanisms may exist.
Diabetic ketoacidosis is rare.
Management of psychosis takes priority over concerns about the potential metabolic sequelae of treatment, but the prevalence of the latter requires that all patients taking antipsychotic agents be actively screened and treated.
Patients treated with antipsychotic agents need baseline and regular checks, including weight, blood glucose and lipid levels and blood pressure.
Management of psychosis with its attendant medical problems requires a multidisciplinary approach, with primary health practitioners playing a central role.
Mortality and medical morbidity is higher in those with psychosis than expected; preventive measures, combined with early detection and treatment of hyperglycaemia and other metabolic problems, is a key public health issue.