Prescription drugs are used by a significant proportion of heroin users around the world, 1-4 including Australia.5 The American Medical Association reports that prescription drugs are involved in 70% of all drug-related deaths in the United States.4 Polydrug heroin-related deaths substantially increased the number of heroin-related deaths in Austria between 1987 and 1995.3 Similarly, increased heroin-related deaths in the past decade in Australia6 may be due in part to combined drug toxicity involving prescription drugs.7
Increasing use of heroin by younger people in recent years has been documented in other countries8 and reported anecdotally in Australia. Young heroin users remain a poorly studied population, despite the fact that heroin-related deaths in this group are less complicated by chronic ill health, and that younger users may be more receptive to interventions.
A common method of obtaining prescription drugs for use, trade or sale involves the fraudulent presentation of disease to multiple doctors and pharmacies — a behaviour known as “doctor shopping” or drug-seeking behaviour.9 Australian GPs write more than 15 million prescriptions per year for drugs known to be misused, with the main prescription drugs misused currently being narcotic analgesics and benzodiazepines, as well as stimulants, barbiturates and other sedative–hypnotic agents.9-11 Fraudulent presentation for such drugs is often difficult to identify, as many heroin users may also have a genuine medical need for the prescription drugs they seek.11,12
Although the economic costs of doctor shopping are well understood,9 the relationship between such behaviour and drug overdose is less clear. Many polydrug misusers progress from illicit drugs to prescription drug use as they become chronically ill.10 Such prescription drug use is thought to escalate over time, perhaps due to increasing ill health associated with long-term drug misuse.10 We sought evidence for such an escalation in drug-seeking behaviour by examining patterns of medical service provision and the supply of prescriptions to young adults who subsequently died of heroin-related causes.
As part of a larger research program investigating risk factors associated with heroin deaths in young adults,13 we examined 202 consecutive Victorian Coroner’s Court cases (from 6 January 1994 to 6 October 1999) of all heroin-related deaths of people aged under 25 years, excluding probable suicides. The information provided by the Coroner’s Court included the coroner’s report and patient’s name, date of birth, forensic toxicology report, autopsy report, circumstances of the death, sex, age and identifying code, but excluded other personal information. Toxicology reports included blood, tissue and/or urine screening tests for heroin, amphetamines, alcohol, barbiturates, benzodiazepines, cannabis, cocaine, opiates and associated metabolites, using previously described methods.
We obtained 1991–2000 Pharmaceutical Benefits Scheme (PBS) data and Medicare Benefits Schedule (MBS) data, which were matched by the HIC and identified with a code to preserve anonymity. The HIC was able to provide some PBS records for 155 cases and MBS records for 175 cases. PBS and MBS data include all government-subsidised prescription and medical services (excluding institutional supply such as within prisons or hospitals).
After describing the patterns of PBS and MBS use for the Coroner’s Court cases, we assessed changes to these rates of service over time using Huynh–Feldt corrected repeated-measures analysis of variance to control for differences between individuals and non-normally distributed data.
One hundred and forty-nine of the young adults who died of heroin-related overdose were men and 53 were women — a male bias similar to heroin-related deaths in New South Wales.5 The mean age was 21 years (range, 14–24 years).
Heroin, or its derivatives or metabolites, was detected in all but two subjects. Drugs other than heroin were present in 90% of the cases, with prescription and pharmacy drugs being present in 80% of cases, particularly benzodiazepines and other opioids (Box 1). Benzodiazepines were most common and were found more commonly in women than in men.
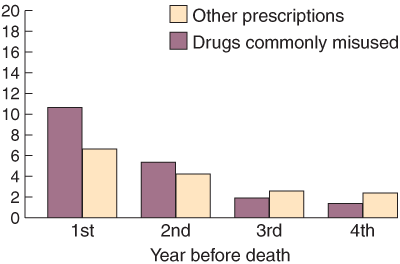
A total of 5860 PBS prescriptions were made out to the 155 subjects over the period from 1 January 1991 until their deaths. Benzodiazepines were the most commonly prescribed group of drugs in this group, accounting for 43% of all prescriptions. Opioids other than heroin accounted for 11% of prescriptions, and 8% of drugs were those prescribed for treating mental illness (eg, antidepressants and major tranquillisers). A further 12% were for anti-infection medicines and 3% for non-opioid analgesics.
The average number of PBS scripts per patient increased in the 4 years before death, from an average of four per person per year in the fourth year before death to a peak of 17 in the year before death (F = 23.698; df = 135,1.98; P < 0.001). Although all prescriptions increased before death (Box 2), the prescription rates for benzodiazepines and for other opioids increased more than prescriptions for other drugs (F = 7.584; df = 135,1.96; P = 0.001).
A total of 16 383 MBS payments were made for services provided to the 175 subjects during the period from 1 January 1991 until their deaths. Most of the MBS services were for professional attendance (72.7%), mostly by GPs or other non-referred providers (95.1%). Pathology requests accounted for 22.7% of services, with the single most common request (16.4% of pathology services) being for the detection of misused drugs (MBS code 66343). Chemical tests (MBS category P2) generally were the most commonly requested pathology service in this patient group (37.7%), compared with microbiology (16.9%), haematology (7.2%) and immunology (0.7%).
In this study, 22% of individuals saw an average of more than 15 medical practitioners per year; 40% averaged more than 30 MBS services per year. Women were disproportionately represented (15 individuals; 32%) in the top half of MBS users, compared with men (33 individuals; 26%) (x2 = 4.998; df = 1; P = 0.025). Similarly, among individuals seeing more than 7.95 providers per year (50th percentile), there were 31 women (65%) compared with 55 men (44%) (x2 = 5.664; df = 1; P = 0.017). For 166 cases with more than 6 months data, men accessed an average of 35 services per year (95% CI, 19.1–50.2), and women accessed an average of 60 services per year (95% CI, 33.4–88.4), compared with state averages of 5 and 10 services per year for 15–24-year-old men and women, respectively.14
MBS service rates increased in the years leading up to death. In the 4 years before death (for which we have 138 cases with complete 4-year datasets), mean MBS service rates increased linearly (Box 3) to a peak of 18.3 in the year before death, from 8.3 in the fourth year before death (F = 26.283; df = 2.4,137; P < 0.001). Further data for a reduced number of cases (up to eight years before death) support this pattern (Box 4).
The number of different service providers used by victims also increased linearly in the years leading up to death, from an average of 4.2 service providers visited 4 years before death to 7.8 in the 12 months before death from overdose (F = 25.66; df = 2.4,137; P < 0.001). Examination of the dataset more than 4 years before death suggests that both medical service provision and the number of different providers accessed fall within the normal ranges for this age group in earlier years (Box 4). Considerable individual variation in doctor-shopping behaviour is apparent in the large range and standard deviation of these values. Patterns in the raw data suggest that some individuals were long-term doctor shoppers. For example, one patient received 600 medical services from 286 different practitioners over 14 months. Other patients rarely used medical services, such as a patient who saw only one doctor just four times in 3 years. Both groups, however, increased their patterns of usage in the 12 months before death.
We found high levels of polydrug and prescription drug use in heroin-related deaths, similar to those reported in other studies. 3,5,6 The lower incidence of alcohol detected in our study (22% compared with 60%5 and 37%6) may be due to the younger population sampled (mean age, 21 years), compared with the broader population of all heroin deaths (mean age, 315 and 306 years). The high frequency with which prescription drugs, particularly benzodiazepines and other opioids, are associated with heroin-related deaths reinforces concerns over the supply and source of these drugs from medical service providers.
Our data provide circumstantial evidence of drug-seeking behaviour before death, including increasing use of multiple doctors and disproportionate increases in prescriptions for drugs prone to misuse. The extent to which this behaviour predicts heroin-related death (rather than merely being a feature of ongoing heroin use itself) requires further investigation. Lifestyle characteristics typical of many young heroin users (such as homelessness, itinerancy, poverty and poor diet) may increase both the use of different doctors and the rate at which doctors are seen,15 as well as vulnerability to fatal overdose.16 The association between heroin addiction and psychopathology17 may also create a legitimate need for medical services. The relationship between declining physical or mental health before death and increasing medical visitation rates is well documented in chronically ill18 and suicidal19,20 patients, and both factors might contribute to the doctor-shopping behaviour exhibited by the patients in this study.
The linking of PBS and MBS data to heroin-related deaths is a new approach to understanding factors contributing to such deaths. The study is constrained by the limitations of the data. Medicare cards are sometimes stolen and misused. Medical records could not always be matched because of administrative and database difficulties. Longer-term data are available only for older subjects who have held individual Medicare cards and records for a longer time. Medical and drug use data may be missing from the PBS and MBS because of time spent in prison. Nor does the PBS include all drugs prone to misuse (such as non-PBS prescriptions, pharmacy, illicit and many widely available drugs). The traditional method of self-reported drug use has the advantage of being able to examine use of all drugs, but suffers from a lack of verifiability. PBS data may provide an important method of verification for self-report studies of drug use.
Irrespective of whether young heroin users are accessing medical services for genuine physical and mental health needs, for access to prescription drugs of misuse, or both, the possibility that their increasing rates of attendance might be an indicator of overdose risk and an opportunity for intervention that cannot be ignored. GPs are ideally placed to advise injecting drug users of treatment options, but are often reluctant to become involved in identifying and managing substance misusers.12,21 When faced with difficult, persistent and often threatening patients, it is tempting to simply prescribe as requested, particularly if the patient is not a regular visitor and when the GP feels vulnerable (such as younger doctors or sole practitioners).
GPs in Australia used to be able to obtain a patient’s past 2 months of prescription history over the phone from the HIC if the patient was listed as a doctor shopper; however, this service was recently cancelled. PBS data for patients not defined as doctor shoppers are available with patient consent; however, this information takes weeks to provide and is therefore only useful if the patient returns to the practice.
The HIC defines individuals as doctor shoppers if, in one year, he or she has seen more than 15 different GPs, has had 30 or more Medicare consultations and has obtained more PBS prescriptions than appear to be clinically necessary.22 In our study, 22% of subjects saw more than 15 GPs, and 40% averaged more than 30 MBS services per year. Despite increasing doctor-shopping behaviour and patterns of prescription drug use,22 many of those who died of a heroin-related overdose did not meet the definition of a doctor shopper and would not be identified as such by the HIC or GPs. A longitudinal study of medical service use by young heroin users, in relation to patterns of both fatal and non-fatal overdose, is clearly warranted to assess the value of a relative increase in doctor-shopping behaviour, rather than as a “hurdle” criterion for high-rate doctor shopping, as a predictor of heroin-overdose risk. Such a study would require the cooperation and commitment of the HIC, as the procedure for obtaining MBS and PBS data for this research program was excessively complex and time-consuming.
A doctor-shopping helpline which used medical attendance and prescription records (like the MBS and PBS) to identify patients tagged as having an escalating profile of medical attendance would enable central doctor-shopping registers to identify not only high-rate doctor shopping, but also high-risk patients. GPs would then be in a stronger position to adopt appropriate treatment and intervention strategies.10,23 Doctor-shopping and drug-seeking behaviour currently tends to be seen primarily as an economic problem. We argue that further research into rapidly increasing drug-seeking behaviour by young heroin users may provide a clinical predictor of overdose risk and an important opportunity for intervention and fatality prevention.
1: Drugs other than heroin detected in blood or urine of 14–24-year-old victims of heroin-related deaths
Drug |
Total (n = 202) |
Men (n = 149) |
Women (n = 53) |
Odds ratio* (95% CI) |
|||||||
Benzodiazepines |
48.5% |
43.6% |
63.5% |
0.469 |
(0.247–0.892) |
||||||
Other opioids |
47.5% |
47.7% |
47.2% |
1.019 |
(0.544–1.910) |
||||||
Cannabis |
36.6% |
39.6% |
28.3% |
1.661 |
(0.840–3.284) |
||||||
Alcohol |
21.8% |
22.8% |
18.9% |
1.271 |
(0.579–2.794) |
||||||
Other |
15.3% |
15.4% |
15.4% |
1.207 |
(0.429–2.460) |
||||||
Antidepressants |
11.4% |
9.4% |
17.0% |
0.507 |
(0.205–1.252) |
||||||
Methadone |
9.9% |
9.4% |
11.3% |
0.812 |
(0.295–2.236) |
||||||
Stimulants |
9.4% |
7.4% |
15.1% |
0.448 |
(0.170–1.184) |
||||||
Major tranquillisers |
5.4% |
5.4% |
5.8% |
0.946 |
(0.241–3.705) |
||||||
* Odds ratio for men versus women. |
|||||||||||
4: Number of services and providers accessed in the years before death
Year before death |
Average number of services (SD) |
Range |
Average number of providers (SD) |
Range |
|||||||
First (n = 170) |
21.0 |
(27.8) |
0–272 |
9.3 |
(13.5) |
0–157 |
|||||
Second (n = 169) |
15.4 |
(24.4) |
0–224 |
7.3 |
(12.0) |
0–138 |
|||||
Third (n = 159) |
9.7 |
(12.0) |
0–95 |
5.0 |
(6.6) |
0–65 |
|||||
Fourth (n = 138) |
8.3 |
(9.8) |
0–74 |
4.2 |
(3.7) |
0–19 |
|||||
Fifth (n = 100) |
6.4 |
(7.2) |
0–45 |
3.5 |
(3.3) |
0–17 |
|||||
Sixth (n = 74) |
6.3 |
(6.6) |
0–32 |
3.5 |
(3.2) |
0–15 |
|||||
Seventh (n = 37) |
5.5 |
(4.1) |
0–17 |
3.1 |
(2.4) |
0–11 |
|||||
Eighth (n = 2) |
10.0 |
(7.1) |
5–15 |
4.5 |
(3.5) |
2–7 |
|||||
Received 18 November 2002, accepted 17 December 2003
- Raymond F Martyres1
- Danielle Clode2
- Jane M Burns3
- 1 Melbourne Division of General Practice, North Carlton, VIC.
- 2 Department of Zoology, University of Melbourne, Parkville, VIC.
- 3 beyondblue: the national depression initiative, Hawthorn West, VIC.
This research was conducted as part of the “Help understanding drug use” program conducted by the Melbourne Division of General Practice and funded by a grant from the Australian Divisions of General Practice. Data were obtained from the Health Insurance Commission, Australia, and the State Coroner’s Office of Victoria.
We would like to thank the Australian Divisions of General Practice for funding this research, and the Health Insurance Commission, Australia, the Victorian Institute of Forensic Medicine and the State Coroner’s Office of Victoria for providing data. The following individuals made significant contributions to the study: Dr Yvonne Bonomo, Ms Fleur Champion de Crespigny, Dr Andrew Chanen, Dr Malcolm Dobbin, Dr David Jacka, Dr John Jagoda, Mr Hal Rosemburg, Ms Lara Watson, Ms Mardie Whitla, Mr Kim Wyman and Professor Doris Young. We thank Dr Ian Gordon, Dr Mick Keogh and Dr Michael Nicholls for statistical advice.
None identified.
- 1. Steentoft A, Teige B, Holmgren P, et al. Drug addict deaths in Nordic countries: A study based on medicolegally examined cases in the five Nordic countries in 1991. Forensic Sci Int 1996; 77: 109-118.
- 2. Oliver P, Keen J, Mathers N. Deaths from drugs of abuse in Sheffield 1997–1999: what are the implications for GPs prescribing to heroin addicts? Fam Pract 2002; 19: 93-94.
- 3. Risser D, Uhl A, Stichenwirth M, et al. Quality of heroin and heroin-related deaths from 1987 to 1995 in Vienna, Austria. Addict 2000; 95: 375-382.
- 4. Lewis P, Gaule D. Dealing with drug-seeking patients: the Tripler Army Medical Centre Experience. Mil Med 1999; 164: 838-840.
- 5. Darke S, Ross J, Zador D, Sunjic S. Heroin-related deaths in New South Wales, Australia, 1992–1996. Drug Alcohol Depend 2000; 60: 141-150.
- 6. Gerostamoulos J, Staikos V, Drummer OH. Heroin-related deaths in Victoria: a review of cases for 1997 and 1998. Drug Alcohol Depend 2001; 61: 123-127.
- 7. Zador D, Sunjic S, Darke S. Heroin-related deaths in New South Wales, 1992: toxicological findings and circumstances. Med J Aust 1996; 164: 204-207. <eMJA full text>
- 8. Hopfer CJ, Khuri E, Crowley TJ, Hooks S. Adolescent heroin use: a review of the descriptive and treatment literature. J Subst Abuse Treat 2002; 23: 231-237.
- 9. Dobbin M. Prescription drug abuse. Melbourne: Department of Human Services, 1998.
- 10. Longo LP, Parran T, Johnson B, Kinsey W. Addiction: Part II. Identification and management of the drug-seeking patient. Am Fam Physician 2000; 61: 2401-2408.
- 11. White J, Taverner D. Drug-seeking behaviour. Aust Prescriber 1997; 20: 68-70.
- 12. Bendtsen P, Hensig G, Ebeling C, Schedin A. What are the qualities of dilemmas experienced with prescribing opioids in general practice? Pain 1999; 82: 89-96.
- 13. MDGP Help understanding drug use: HUDU – you can. Melbourne: Melbourne Division of General Practice, 2002.
- 14. Health Insurance Commission. Annual Report 1999–2000. Canberra: HIC, 2000.
- 15. Borgois P. The moral economics of homeless heroin addicts: confronting ethnography, HIV risk, and everyday violence in San Francisco shooting encampments. Subst Use Abuse 2001; 33: 2323-2351.
- 16. Warner-Smith M, Darke S, Lynskey M, Hall W. Heroin overdose: causes and consequences. Addict 2001; 96: 1113-1125.
- 17. Chen C, Tsai S, Su L, et al. Psychiatric co-morbidity among male heroin addicts: differences between hospital and incarcerated subjects in Taiwan. Addict 1999; 94: 825-832.
- 18. Latimer EA, Verrilli D, Welch WP. Utilization of physician services at the end of life: differences between the United States and Canada. Inquiry 1999; 36: 90-100.
- 19. Pirkis J, Burgess P. Suicide and recency of health care contacts — a systematic review. Br J Psychiatry 1998; 173: 462-474.
- 20. Appleby L, Amos T, Doyle U, et al. General practitioners and young suicides: a preventative role for primary care. Br J Psychiatry 1996; 168: 330-333.
- 21. Jacka D, Clode D, Patterson S, Wyman K. Attitudes and practices of general practitioners training to work with drug-using patients. Drug Alcohol Rev 1999; 18: 287-291.
- 22. Health Insurance Commission. Doctor shopping. Canberra: HIC, 2002.
- 23. Pope D, Fernandes CMB, Bouthillette F, Etherington J. Frequent users of the emergency department; a program to improve care and reduce visits. Can Med Assoc J 2000; 162: 1017-1020.





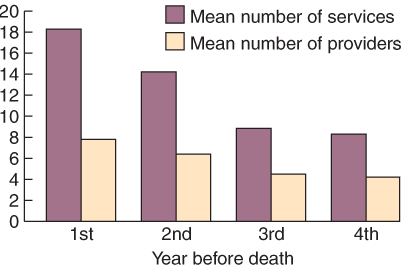
Abstract
Objective: To identify prescription drug-seeking behaviour patterns among young people who subsequently died of heroin-related overdose.
Design: Linkage of Medicare and Pharmaceutical Benefits Scheme and Coroner’s Court records from Victoria.
Subjects: Two hundred and two 15–24-year-olds who died of heroin-related overdose between 6 January 1994 and 6 October 1999.
Main outcome measures: Patterns of use of medical services and prescription drugs listed on the Pharmaceutical Benefits Scheme in the years before death, and use of all drugs just before death.
Results: Polydrug use was reported in 90% of toxicology reports, and prescription drugs were present in 80% of subjects. Subjects accessed medical services six times more frequently than the general population aged 14–24 years, and more than half of all prescribed drugs were those prone to misuse, such as benzodiazepines and opioid analgesics. A pattern of increasing drug-seeking behaviour in the years before death was identified, with doctor-visitation rates, number of different doctors seen and rates of prescriptions peaking in the year before death.
Conclusions: An apparent increase in “doctor shopping” in the years before heroin-related death may reflect the increasing misuse of prescription drugs, but also an increasing need for help. Identification of a pattern of escalating doctor shopping could be an opportunity for intervention, and potentially, reduction in mortality.