Osteoarthritis is the most common musculoskeletal disorder affecting Australians, the leading cause of pain and disability in the community,1,2 and the predominant condition leading to joint replacement surgery of the hip and knee.3 A number of modifiable factors, including obesity, injury, quadriceps strength, joint malalignment and occupational activities, contribute to both the onset and progression of osteoarthritis-related disability.4 Primary and secondary prevention strategies are needed to reduce the levels of disability and to slow the growing demand for total joint replacement surgery.
Here we describe details of the epidemiological features of osteoarthritis (OA) and joint replacement surgery in Australia.
The incidence, or number of new cases each year, is difficult to determine and will vary depending on whether a radiological or a clinical definition is used.
On the basis of international radiological survey data, the Australian Institute of Health and Welfare (AIHW) estimated that there are some 27 000 new cases of radiological OA among women each year (peak rate of onset of 13.5 per 1000 population in the 65–74 years age group) and about 15 500 new cases among men (peak rate of 9.0 per 1000 in those aged 75 years and over).5 This means more than 40 000 new cases of radiological OA each year, adding to the large pool of prevalent OA, which will continue to grow as our population ages. The accuracy of these estimates may be questionable, as they were derived from cross-sectional prevalence surveys. To date, no Australian prospective population-based studies have been reported. More recent radiological longitudinal surveys in the United Kingdom suggest that the incidence may be higher, with 20–30 women per 1000 aged 50 to 60 years developing new radiological knee, hip and spinal OA each year.6,7
Arthritis is self-reported by about 15% of Australians (ie, about three million; see Box 1). Osteoarthritis accounts for most of these.1,2
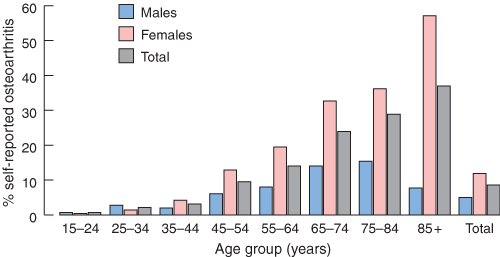
The prevalence of OA increases with age. Symptomatic OA is uncommon, occurring in fewer than 5% of people under the age of 40. Prevalence increases to 10% of men and 20% of women aged 45–65 years8 and even further to more than 50% of women aged 85 years and over (Box 2). Radiological prevalence surveys suggest much higher rates than this, with changes of OA being present on x-ray in more than 50% of people over the age of 65 years, and almost universally after 85 years. Not all radiological OA is associated with clinical symptoms, and not all symptomatic OA is associated with disability. More advanced radiological changes are more likely to be symptomatic. Female sex, lower educational level, obesity and poor muscle strength have been shown to be risk factors for developing symptoms and disability.4
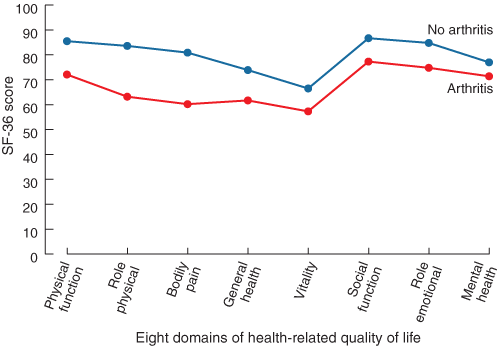
The impact of OA on individuals can be significant. In 1991, arthritis and rheumatism were the leading causes of disability among those aged 65 years and over living in the community, being reported by more than 40% of men and 50% of women.9 People with OA have more difficulty and take longer to perform activities of daily living, have less time available for leisure activities, depend significantly more on family and friends for assistance and spend more money on healthcare than age-matched and sex-matched peers in the general population.10,11 OA of the knee accounts for more dependence in walking, stair climbing, and other lower-extremity tasks than any other disease.12 When compared with values for the Australian general population, apart from the general health and mental health scores (which are similar), people with arthritis have poorer scores on six of the eight domains of the SF-36 measure of health-related quality of life13,14 (see Box 3).
OA is the third-largest contributor to life-years lost due to disability in Australia, equal to asthma (4.8% of total life-years lost due to disability), and only exceeded by depression (8.0%) and dementia (5.6%).15 Osteoarthritis is estimated to have accounted for about 60 000 disability-adjusted life-years (DALYs) lost in 2000.16
The economic impact of OA on society is also significant.15 The AIHW estimated that direct medical costs to the Australian healthcare budget attributable to OA in 1993–94 were in the order of $624 million.16 The major component costs were hospitalisation (43%; predominantly for joint replacement surgery), visits to general practitioners and specialists (13%), prescription and over-the-counter medications (9%), and allied healthcare (6%). Substantial swings in these have occurred since that time, with an increase in private-sector joint replacement surgery, and a significant increase in number and cost of prescription medications, because of the release and uptake of COX-2-selective non-steroidal anti-inflammatory drugs.
In Australia, musculoskeletal conditions are the third leading reason for a visit to a general practitioner (11%), behind respiratory problems (17%) and unspecified general problems (18%).17 Osteoarthritis is the second leading reason for patient visits to a rheumatologist.18
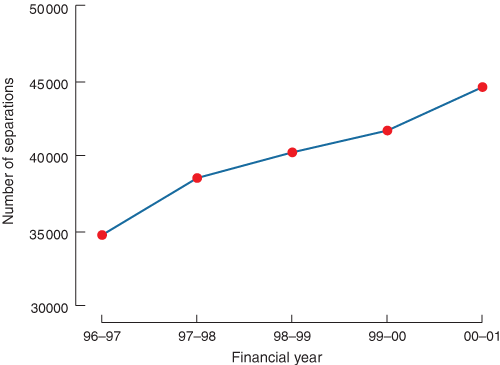
Hip and knee joint replacements are among the most cost-effective interventions available.19-23 However, the pressing demand makes joint replacement a significant burden on the healthcare budget. The total number of knee and hip replacements in Australian hospitals rose from 34 700 in 1996–97, to 44 552 in 2000–01; this is an increase of almost 30% in just 4 years (see Box 4). Figures for July 2001 to June 2002 just released report 52 788 hip and knee replacement procedures, having increased from 46 537 in the previous 12 months, and representing a further increase of 13.4%.
Ninety per cent of total hip replacements and more than 95% of total knee replacements are performed for OA.3 Most of the increase in the past 3 years has occurred in the private rather than the public sector (17.2% v 8.1%), and knee replacement surgery is increasing more rapidly than hip replacement surgery (17.2% v 9.9%).3 The rate of revision surgery for total joint replacement is also now starting to rise.
Despite the observed increase, it is likely that there is still a lot of unmet need. Determining the population need for total joint replacement surgery is a difficult task, and has not been formally undertaken in Australia. Many aspects of osteoarthritis need to be considered, including the incidence, prevalence and progression of the disease, together with the patients’ preferences for surgery and the treating doctors’ propensity for recommending surgery. This has recently been reviewed for total knee replacement surgery in England, where it was estimated that a doubling of the current rate of joint replacement surgery would be required just to meet existing need.24 The authors of that report proposed that this considerable unmet need was not just the result of healthcare services’ inability to keep up with demand, but also of patients and doctors not considering or offering it as a treatment option.
It is estimated that the need for total joint arthroplasty will increase in Australia because of a combination of rising prevalence of OA associated with increasing risk factors (age, obesity, joint injury), higher community expectations for enhanced quality of life, and improved surgical and anaesthetic techniques that enable the intervention to be offered more widely.
The aetiology of OA is multifactorial, and risk factors for its onset can be considered as either unmodifiable or potentially modifiable. The impact of different risk varies among men and women and for the different joints.
Key factors among those currently considered unmodifiable include age, genetics, family history, female sex and race.4,25,26
Sex and age differences: Before the age of 50 years, men have more radiological OA than women, and this is presumed to be largely because of OA secondary to knee trauma, while, after the age of 50 years, the prevalence among women increases dramatically.4 In Australia, self-reported symptomatic OA among those aged less than 50 years is infrequent, but rates are similar for men and women; this then also increases dramatically with age, particularly in women (see Box 2). Women have twice the risk that men have of developing bilateral knee OA, while men are more likely to develop unilateral OA of the knee. For OA of the hip, the prevalence is higher for women aged 65 years and over, while among individuals aged 55–64 years it is more common in men. For OA of the hand, women have 2.6 times the risk of men. Most studies show increasing risk of knee OA with age, and radiological surveys suggest that knee osteophyte (bony outgrowth) development increases by 20% per 5-year increase in age. Similarly, for hip OA, age increases the risk (odds ratio, 2.38 for ages 70–74 years compared with 55–59 years). Age is also closely associated with OA of the hand.4
Family history: This is a well-documented risk factor, with the occurrence of Heberden’s nodes having almost autosomal dominant inheritance. Despite this strong association, no single gene defect has been identified for all generalised OA. Twin studies now suggest that the heritability component of OA may be as high as 60%–65% for hip and hand OA, and around 40%–50% for knee OA.27 A genetic defect in the collagen type II gene has been identified in some families with premature onset of severe OA; however, this defect is not found in the wider OA community.
Race: All races can be affected by OA, but some Asians have a much lower occurrence of OA of the hip and hand, but a higher occurrence of OA of the knee.28-30 More knee OA is seen particularly among Chinese women when compared with North American women, and is independent of weight and anatomical alignment of the lower limbs.
The key potentially modifiable factors for the development of OA include injury, obesity and occupational overuse.31-35
Injury: Injury to a joint has long been recognised as a risk factor, and is the most important modifiable risk for knee OA in men. Meniscal and cruciate ligament tears increase the risk of subsequent development of OA by 5–10 times, with 40%–60% of long-term study participants having OA changes by the age of 20 years.36,37 It is evident that a significant interaction exists between age and injury and it is said that a major injury ages the knee by 30 years (Stefan Lohmander, Professor of Orthopaedics, Lund University, Sweden, personal communication). Although surgical repair is widely undertaken and appears to be associated with reduced pain and improved function in the short to medium term, longer-term studies are suggesting that it may not be as protective as once thought, with similar proportions of patients going on to develop OA. It has been suggested that the levels of proteases released at the time of injury stay elevated and tip the balance of the chondrocyte and articular cartilage towards degeneration rather than repair.
Epidemiological studies have also shown associations between hip trauma and hip OA.4
Obesity: There is a large body of evidence that identifies obesity as a risk factor for developing OA of the knee, particularly in women. Obesity is also associated with the development of disability and the radiological progression of OA once established. It was generally believed that the obesity was secondary to inactivity brought about by the painful joints. However, well designed epidemiological studies now show that the risk begins as early as the third decade of life.4 For every 2 units of body mass index (BMI) gain (equivalent to about 5 kg), the risk of OA of the knee is increased by 36%.38 Conversely, for every 5 kg decrease in body weight during the preceding 10 years, the risk of OA of the knee declines by more than 50%.38 People in the upper BMI quartile (> 30 kg/m3) have a 20-fold risk of developing bilateral OA of the knee. It is also likely that there is an interaction between obesity and malalignment in knee OA.39
The prevalence of obesity is increasing world wide, and this is evident in Australia.40 This may explain, in part, the more rapid rise in demand for knee replacements compared with hip replacements in recent years.
Reviews also confirm obesity to be a modest risk factor for OA of the hip (twofold increase). Some studies have suggested an association between OA of the hand and BMI, although this is not as consistent.
Occupational overuse: Occupational activity, perhaps through overuse and frequent minor injury, has long been recognised as a risk factor for OA. A number of epidemiological studies have shown a consistent association between hip osteoarthritis and farming in men, with agricultural workers who were active for 10 years having double the risk of those working less than 1year.
Radiological assessment of the hands of cotton mill workers documented more osteoarthritis than in age-matched controls, and linked specific joint sites (eg, distal interphalangeal joint or first carpometacarpal joint) with the nature of the repetitive tasks performed.
The strongest association with occupational activity has been shown with OA of the knee in men. It is estimated that up to 30% of all knee OA is attributable to occupational activity that involves repeated knee bending, kneeling, squatting, or climbing.4 These activities increase the risk two- to fourfold and, if combined with heavy lifting of more than 25 kg on a regular basis, increase risk fivefold.41
Fortunately, OA does not progress to a stage that requires joint replacement surgery in all who are affected. Earlier longitudinal studies suggest that only 30% of established cases of OA of the knee progress over a 10–12-year period.42
Obesity, weak quadriceps strength and malalignment have been shown to be significant potentially modifiable predictors of functional disability, as well as of progression of damage visible on x-ray, with female sex and generalised OA also being important influences.43 Inflammation, indicated by increased uptake on nuclear bone scans, may also predict progression.44,45
More recent studies suggest that joint-space narrowing apparent on x-rays of weight-bearing knees is a strong predictor of future progression, and that progression in patients with grade 2 narrowing (> 50% of joint-space width) may be greater than previously described, with 50% progressing to severe joint space narrowing within 7 years.46 Joint space narrowing has been shown to be a significant predictor of total joint arthroplasty.
Osteophytes seen on plain x-ray have been shown to correlate more with symptoms than joint space narrowing, but do not appear to predict progression.47 A recent study confirms that bone marrow oedema, visible on magnetic resonance imaging, is a more sensitive marker of progression.48 It will be important to identify these factors to target those at high risk if we are to stem the tide of joint replacement surgery.
Nutritional factors, such as low antioxidant, vitamin C and vitamin D intake, have been shown in observational studies to be associated with increased risk of radiological progression of OA and onset of knee pain.4 However, increasing dietary intake of antioxidants or vitamins has not been proven to slow progression, or to modify symptoms, in controlled clinical trials.49,50 Further studies of the effect of dietary factors on OA are needed.
Prevention strategies aimed at reducing injury, ensuring appropriate rehabilitation, encouraging appropriate physical activity, reducing obesity and increasing muscle strength require urgent facilitation.
1: Self-reported musculoskeletal conditions among Australian men and women (combined) aged 25 years and over*
|
Age group (years) |
||||||||||
Condition |
25–34 |
35–44 |
45–54 |
55–64 |
65–74 |
75 + |
Total |
||||
Total arthritis |
5.2% |
11.3% |
21.4% |
37.8% |
47.7% |
52.4% |
14.6% |
||||
Total spinal problems |
6.1% |
8.1% |
9.2% |
8.0% |
5.2% |
4.4% |
5.1% |
||||
Osteoporosis |
0.2% |
0.5% |
1.3% |
3.4% |
6.2% |
8.1% |
1.4% |
||||
Total musculoskeletal conditions |
16.2% |
22.6% |
33.1% |
47.8% |
56.0% |
61.1% |
22.9% |
||||
* Data from the National Health Survey 1995.2 |
|||||||||||
- Lynette M March1
- Hanish Bagga2
- Florance and Cope Professorial Department of Rheumatology, Royal North Shore Hospital, St Leonards, NSW.
None identified.
- 1. Arthritis Foundation of Australia. Access Economics Report 2001. Available at: www.arthritisfoundation.com.au (accessed Jan 2004).
- 2. 1995 National health survey. Canberra: Australian Bureau of Statistics, 1996.
- 3. Australian Orthopaedic Association National Joint Replacement Registry Annual Report. Adelaide: AOA, 2003. Available at: www.dmac.adelaide.edu.au/aoanjrr/documents/aoanjrrreport_2003.pdf (accessed Jan 2004).
- 4. Felson DT, Zhang Y. An update on the epidemiology of knee and hip osteoarthritis with a view to prevention. Arthritis Rheum 1998; 41: 1343-1355.
- 5. Mathers C, Vos T, Stevenson C. The burden of disease and injury in Australia. Canberra: Australian Institute of Health and Welfare, 1999.
- 6. Hassett G, Hart DJ, Manek NJ, et al. Risk factors for progression of lumbar spine disc degeneration: the Chingford study. Arthritis Rheum 2003; 48: 3112-3117.
- 7. Hassett GM, Hart DJ, Spector TD, Antoniades L. Hip joint space width at the site of maximal joint space narrowing in Caucasian women: the Chingford study. Proceedings of the Annual European Congress of Rheumatology; 2003 June; Lisbon [abstract]. Available at: www.eular.org (accessed Jan 2004).
- 8. March LM, Schwarz JM, Carfrae BH, Bagge E. Clinical validation of self-reported osteoarthritis. Osteoarthritis Cartilage 1998; 6: 87-93.
- 9. March LM, Brnabic AJM, Skinner JC, et al. Musculoskeletal disability among elderly people in the community. Med J Aust 1998; 168: 439-442.
- 10. Gabriel SE, Crowson CS, Campion ME, O’Fallon WM. Indirect and non-medical costs among people with rheumatoid and osteoarthritis compared with non-arthritic controls. J Rheumatol 1997; 24: 43-48.
- 11. Yelin E, Callahan LF. The economic cost and social and psychological impact of musculoskeletal conditions. National Arthritis Data Work Groups. Arthritis Rheum 1995; 38: 1351-1362.
- 12. Creamer P, Lethbridge-Cejku M, Hochberg MC. Factors associated with functional impairment in symptomatic knee osteoarthritis. Rheumatology (Oxford) 2000; 39: 490-496.
- 13. 1995 National Health Survey SF-36 report. Canberra: Australian Bureau of Statistics, 1997.
- 14. Lapsley HM, March LM, Tribe KL, et al. Living with osteoarthritis: patient expenditures, health status, and social impact. Arthritis Rheum 2001; 45: 301-306.
- 15. March LM, Bachmeier CJ. Economics of osteoarthritis: a global perspective. Baillieres Clin Rheumatol 1997; 11: 817-834.
- 16. Mathers C, Penn R. Health system costs of injury, poisoning and musculoskeletal disorders in Australia 1993–94. (Health and Welfare Expenditure Series no. 6). Canberra: Australian Institute of Health and Welfare, 1999.
- 17. Britt H, Sayer GP, Miller G, et al. General practice activity in Australia 1998–99. Canberra: Australian Institute of Health and Welfare, 1999.
- 18. Lybrand S. Health related quality of life and the burden of disease in Australian rheumatology practice [Masters thesis]. Brisbane: University of Queensland, 2003.
- 19. Hirsch HS. Total joint replacement: a cost-effective procedure for the 1990s. Med Health R I 1998; 81: 162-164.
- 20. Rissanen P, Aro S, Sintonen H, et al. Costs and cost-effectiveness in hip and knee replacements. A prospective study. Int J Technol Assess Health Care 1997; 13: 575-588.
- 21. Liang MH, Cullen KE, Larson MG, et al. Cost-effectiveness of total joint arthroplasty in osteoarthritis. Arthritis Rheum 1986; 29: 937-943.
- 22. Lavernia CJ, Guzman JF, Gachupin-Garcia A. Cost effectiveness and quality of life in knee arthroplasty. Clin Orthop 1997; 345: 134-139.
- 23. O’Shea K, Bale E, Murray P. Cost analysis of primary total hip replacement. Ir Med J 2002; 95: 177-180.
- 24. Juni P, Dieppe P, Donovan J, et al. Population requirements for knee replacement surgery: a cross-sectional study. Rheumatology 2003; 42: 516-521.
- 25. Felson DT, Lawrence RC, Dieppe PA, et al. Osteoarthritis: new insights. Part 1: the disease and its risk factors. Ann Intern Med 2000; 133: 635-646.
- 26. Sowers MF. Epidemiology of risk factors for osteoarthritis: systemic factors. Curr Opin Rheumatol 2001; 13: 447-451.
- 27. Spector TD, Cicuttini F, Baker J, et al. Genetic influences on osteoarthritis in women: a twin study. BMJ 1996; 312: 940-943.
- 28. Nevitt MC, Xu L, Zhang Y, et al. Very low prevalence of hip osteoarthritis among Chinese elderly in Beijing, China, compared with whites in the United States. Arthritis Rheum 2002; 46: 1773-1779.
- 29. Zhang Y, Xu L, Nevitt MC, et al. Lower prevalence of hand osteoarthritis among Chinese subjects in Beijing compared with white subjects in the United States: the Beijing Osteoarthritis study. Arthritis Rheum 2003; 48: 1034-1040.
- 30. Felson DT, Nevitt MC, Zhang Y, et al. High prevalence of lateral knee osteoarthritis in Beijing Chinese compared with Framingham Caucasian subjects. Arthritis Rheum 2002; 46: 1217-1222.
- 31. Hunter DJ, March L, Sambrook PN. Knee osteoarthritis: the influence of environmental factors. Clin Exp Rheumatol 2002; 20: 93-100.
- 32. Felson DT, Zhang Y, Anthony JM, et al. Weight loss reduces the risk for symptomatic knee osteoarthritis in women. The Framingham Study. Ann Intern Med 1992; 116: 535-539.
- 33. Sharma L. Local factors in osteoarthritis. Curr Opin Rheumatol 2001; 13: 441-446.
- 34. Hart DJ, Doyle DV, Spector TD. Incidence and risk factors for radiographic knee osteoarthritis in middle-aged women: the Chingford Study. Arthritis Rheum 1999; 42: 17-24.
- 35. Felson DT, Zhang Y, Hannan MT, et al. The incidence and natural history of knee osteoarthritis in the elderly. The Framingham Osteoarthritis Study. Arthritis Rheum 1995; 38: 1500-1505.
- 36. MacNicol MF, Thomas NP. The knee after meniscectomy [editorial]. J Bone Joint Surg Br 2000; 82: 157-159.
- 37. McNicholas MJ, Rowley DI, McGurty D, et al. Total meniscectomy in adolescence. A thirty-year follow-up. J Bone Joint Surg Br 2000; 82: 217-221.
- 38. Hart DJ, Spector TD. The relationship of obesity, fat distribution and osteoarthritis in women in the general population: the Chingford Study. J Rheumatol 1993; 20: 331-335.
- 39. Sharma L, Lou C, Cahue S, Dunlop DD. The mechanism of the effect of obesity in knee osteoarthritis: the mediating role of malalignment. Arthritis Rheum 2000; 43: 568-575.
- 40. Cameron AJ, Welborn TA, Zimmet PZ, et al. Overweight and obesity in Australia: the 1999–2000 Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Med J Aust 2003; 178: 427-432. <eMJA full text>
- 41. Coggon D, Croft P, Kellingray S, et al. Occupational activity and osteoarthritis of the knee. Arthritis Rheum 2000; 43: 1443-1449.
- 42. Schouten JS, van den Ouweland FA, Valkenburg HA. A 12 year follow up study in the general population on prognostic factors of cartilage loss in osteoarthritis of the knee. Ann Rheum Dis 1992; 51: 932-937.
- 43. Spector TD, Hart DJ, Doyle DV. Incidence and progression of osteoarthritis in women with unilateral knee disease in the general population: the effect of obesity. Ann Rheum Dis 1994; 53: 565-568.
- 44. McCarthy C, Cushnaghan J, Dieppe P. The predictive role of scintigraphy in radiographic osteoarthritis of the hand. Osteoarthritis Cartilage 1994; 2: 25-28.
- 45. Dieppe P, Cushnaghan J, Young P, Kirwan J. Prediction of the progression of joint space narrowing in osteoarthritis of the knee by bone scintigraphy. Ann Rheum Dis 1993; 52: 557-563.
- 46. Wolfe F, Lane NE. The long-term outcome of osteoarthritis: rates and predictors of joint space narrowing in symptomatic patients with knee osteoarthritis. J Rheumatol 2002; 29: 139-146.
- 47. Spector TD, Hart DJ, Byrne J, et al. Definition of osteoarthritis of the knee for epidemiological studies. Ann Rheum Dis 1993; 52: 790-794.
- 48. Felson DT, McLaughlin S, Goggins J, et al. Bone marrow edema and its relation to progression of knee osteoarthritis. Ann Intern Med 2003; 139: 330-336.
- 49. McAlindon TE, Jacques P, Zhang Y, et al. Do antioxidant micronutrients protect against the development and progression of knee osteoarthritis? Arthritis Rheum 1996; 39: 648-656.
- 50. McAlindon TE, Felson DT, Zhang Y, et al. Relation of dietary intake and serum levels of vitamin D to progression of osteoarthritis of the knee among participants in the Framingham Study. Ann Intern Med 1996; 125: 353-359.





Abstract
Arthritis affects around 3 million people in Australia, representing about 15% of the population.
Osteoarthritis is the leading cause of pain and disability among the elderly.
Osteoarthritis is the third leading cause of life-years lost due to disability.
Obesity and joint injury are important potentially modifiable risk factors for the development of osteoarthritis.
Obesity is also an important predictor of progression of osteoarthritis.
Currently, about 19 000 hip and 20 000 knee replacements are performed for osteoarthritis in Australia each year.
Prevalence of osteoarthritis and the need for total joint replacement surgery are likely to increase because of a combination of increasing risk factors (age, obesity, injury), increasing expectations for improved quality of life, and improved surgical and anaesthetic techniques making surgery possible for more people.
Services to provide these cost-effective procedures need to be increased.
Primary and secondary prevention programs aimed at reducing obesity, preventing injury and improving rehabilitation and physical activity are urgently required.