Globalisation promised to be a “rising tide lifting all boats”. And it did — if your boats happened to be moored in Western Europe, North America, Oceania1,2 or the handful of Asian countries whose success owed more to breaking than following the liberalisation tenets now entrenched in World Trade Organization (WTO) rules.3 In other regions, global market integration has failed to increase growth, decrease poverty or usher in a new era of planetary health. The health and security risks posed by an economic globalisation unchecked by social and environmental stewardship are also becoming apparent. Improved health is essential to economic development for many of the world’s poorer countries;4 health declines can exacerbate poverty and increase the risk of “failed states” and regional conflicts.5 Inherently global health issues such as climate change, food and water scarcity, and resource depletion6 pose health threats requiring global-scale interventions.
Managing such interventions remains the business of individual nations and their foreign policies. Trade, development assistance and peacekeeping are the traditional terrain of foreign policy. But what might foreign policy look like if health were made one of its key policy goals?
This article is based on work undertaken for a recent Royal Commission on the Future of Health Care in Canada to answer this question.7 Our study set out to examine how contemporary globalisation and its trade agreements were affecting Canadians’ health and healthcare. As soon as this aim became known, Commission staff heard from trade officials that there was nothing to examine — globalisation and trade were good for our health and Canada’s public healthcare system was completely protected. So there is much to value in the principle of independent commissions.
Our approach was to create a simple typology for how health could figure in Canadian foreign policy:
as a human right;
as a means and goal of development;
as a global public good; and
as a trade commodity.7
The two principal international references to the right to health are in the United Nations Universal Declaration of Human Rights (“Everyone has the right to a standard of living adequate for the health and well-being of himself and of his family, including food, clothing, housing and medical care and social services”) and the UN International Covenant on Economic, Social and Cultural Rights (“the States parties to the present Covenant recognize the right of everyone to the enjoyment of the highest attainable standard of physical and mental health”). The Covenant recognises the resource limitations of developing countries and expects only progressive realisation of this right.8
In 2002, the UN Commission on Human Rights created the position of a Special Rapporteur to recommend measures to promote this right. Canada supported creation of this position; Australia and the United States were the only two countries to vote against it, claiming the 3-year position would cost too much. The Special Rapporteur’s first report has noted that the right to health is judiciable (meaning that it has been used in court cases in several countries) and applies both to healthcare and to underlying health determinants, such as access to safe and potable water and adequate sanitation, healthy environments, and access to health education.9
The exact standing of the right to health in Canada is not as clear as it is in countries that enshrine this right in their constitutions. Although international legal opinion suggests that this right overrides trade agreements or other multilateral accords,10 there are no means to enforce this beyond moral suasion. States “are obliged . . . to ensure that no international agreement or policy adversely impacts upon the right to health, and that their representatives in international organizations take due account of the right to health”, including “an analysis of the distributional impact of reforms on the well-being of different groups in society especially the poor and vulnerable . . . with a view to identifying appropriate mitigating or other measures”.9 To our knowledge, no state has yet done so with respect to trade agreement commitments.
Our study recommended that Canada entrench the right to health in legislation. While accepted by the Commission’s Final Report, little attention to this recommendation has since been given.
There is a growing literature confirming the obvious — sick people are hardly capable of performing well economically. Health is not only a development goal, but also a development means. Thus, three of the eight Millennium Development Goals directly address health, and most of the others concern basic health determinants (Box 1).
The World Health Organization (WHO) Commission on Macroeconomics and Health4 estimated the cost of a “set of essential interventions” at US$34 per capita per year. The former Director-General of WHO argued that “health systems which spend less than US$60 per capita are not able to even deliver a reasonable minimum of services”.12 Yet the world’s least-developed countries spend an average of just US$11 per capita annually on health, and other low-income countries spend US$25.13 The problem is not lack of effort or interest on the part of many poorer countries,14 but an inadequate pool of public resources. There remains, of course, the problem of ensuring that such funds are used for their intended purposes and are not misappropriated by corrupt or ineffective public officials. However, this is a responsibility of recipient countries, not donors.
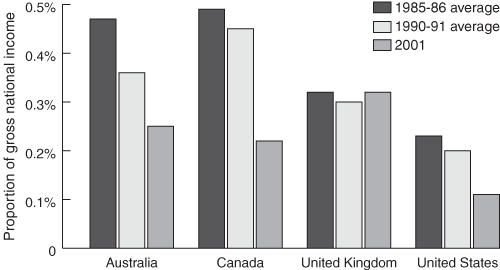
The past decade of unprecedented rise in wealth in developed countries also marked the decade of least concern for those left behind. The 1990s saw official development assistance rates plummet for almost every wealthy donor, although only a few European countries ever hit the internationally agreed target of 0.7% of GDP (now expressed as GNI, or gross national income). Canada’s drop was spectacular (Box 2) and Australia’s and the US’s not much better. The United Kingdom managed to regain the ground it lost under Margaret Thatcher’s rule, although it had very little ground to make up. The Canadian drop in aid is the more worrying, as a very small portion of it (around 4%, but scheduled to rise) goes to health, whereas a very high portion (~75%) is tied to buying Canadian products or to “technical cooperation” (payment of Canadian consultants, who often offer little of value to the recipient country). One positive change, however, is that civil society organisations in Africa can now bid against Canadian organisations on technical cooperation projects.
Canada announced in 2002 that development assistance budgets would increase by 8% a year in the coming years, with half of this growth going to Africa. Although a welcome start, this represents less than a third of the aid that might have gone to sub-Saharan African countries over the past decade had Canada’s contribution to this region remained at its 1990 level.16
Public goods are services or amenities that are undersupplied by the market and therefore require public provision or financing. The relatively new concept of global public goods may be described as public goods that are underprovided by local governments and are considered “global” because their benefits may accrue beyond national borders.
Are free trade agreements global public goods? Some claim that they are, on the assumption that they promote economic growth which, by definition, is a public good. Others argue that such agreements are global public “bads”, as they exacerbate the inequities in wealth, environmental pollution and resource depletion that usually accompany rapid growth. Consider the contradictory relationship between the Framework Convention on Tobacco Control (a recent global public good for health) and several trade agreements. In March 2002, Phillip Morris International stated that proposed Canadian regulations to prohibit use of the terms “mild” and “light” on tobacco packaging would violate North American Free Trade Agreement (NAFTA) Article 1105 (unfair expropriation) and Article 1110 (measures tantamount to expropriation of reasonably expected profits); as well as Article 20 of the Trade-Related Aspects of Intellectual Property Rights (TRIPS) agreement (unjustifiably encumbering use of a trademark) and Article 2.2 of the Agreement on Technical Barriers to Trade (creating unnecessary obstacles and not being the least trade restrictive method).17 Will the real global public good — private profit or public health — please stand up?
The most direct foreign health policy implication of the global public good concept is the need for wealthier countries to take disease control in poorer nations far more seriously. Each country can be judged partly by its response to the UN Global Fund to Fight AIDS, Tuberculosis and Malaria. Pledges received from government and the private sector to October 2003 amount to US$4.6 billion (out of a desirable US$10 billion a year), and many of these are in multi-year pledges. Canada’s 3-year pledge, equal to US$1.10 per capita annually, is less than the cost of a cup of coffee per Canadian per year. The UK’s contribution is equal to about US$3.40. Australia’s pledge has no equivalent, because it is not contributing any money. By contrast, Swedish and Dutch contributions amount to US$6.18 and US$7.61.18
Health is increasingly viewed as a trade commodity, as evinced in the major trade agreements TRIPS and the General Agreement on Trade in Services (GATS). Both have been cited as possible violations of human rights accords because of their potential deleterious impacts on access to essential health services.9
TRIPS requires WTO members to legislate patent protection for 20 years, although least-developed countries do not have to do this until 2016. This has sharply increased pharmaceutical costs and decreased the public funding available for primary healthcare or other programs in many countries, but especially poorer countries. TRIPS allows countries with public health emergencies to issue compulsory licences to allow the manufacture of generic drugs. However, this is not feasible for developing countries that lack such manufacturing capacity. A solution was achieved in August 2003 when the United States agreed that generic drugs could be produced for “parallel import” by countries lacking production facilities. Canada, which originally sided with the earlier US position in seeking a restrictive interpretation of “parallel importing”, surprised many in September 2003 when it became the first developed country to announce its intent to produce generic drugs for this purpose. The legislation is likely to become law when a new parliament convenes in early 2004.
The GATS agreement is more complicated. It is not the cause of healthcare privatisation, as some critics contend, but may accelerate a global trend in such privatisation, which almost invariably leads to inequalities in access. Essentially, GATS locks in current privatisation levels in committed sectors. The agreement does offer an exception for “a [government] service which is supplied neither on a commercial basis, nor in competition with one or more service suppliers” (GATS Article 1: 3b). However, this clause may collapse under challenge, as most countries allow some commercial or competitive provision of almost all public services, including healthcare.19
To date, 54 WTO members (many of which are developing countries) have made commitments to liberalise some health services under GATS.20 Once a service sector has been liberalised under GATS, there is no cost-free way of reversing it. For instance, Canada has opened up private health insurance under GATS. Should we wish to reverse this privatisation trend, our GATS commitments could trigger trade penalties, which may be monetary or in the form of liberalisation in other trade areas. The same would apply to any developing country wishing to revert to more publicly funded health services.
The message we conveyed to the Royal Commission was blunt: healthcare is not like other commercial services. It is essential to the creation and maintenance of a public good. Public healthcare systems arose in most countries because private systems proved inadequate and inequitable. Trade treaties — intended to promote private commercial interests — are no place to negotiate international rules for healthcare and other essential public goods such as education, water and sanitation. Indeed, the progressive liberalisation requirement of GATS may directly contravene the progressive realisation of the right to health under human rights covenants.
Canadian trade negotiators listened to this repeated argument from health and social policy activists, and put their trading partners on notice that Canada will not commit any of its health, education or social services under GATS. But GATS negotiations are ongoing. Many observers believe that pressures to liberalise health and other essential public services will continue unless stronger and internationally agreed exceptions for such services are created. There are at least two ways this can be done:
Create a general exception in the GATS agreement for countries to withdraw without penalty any commitments in services related to healthcare, water and sanitation, or education.
Create an agreement on international trade in these services independent of WTO and with the goal of achieving greater equity in health. The Canadian government worked for 7 years to create international consensus for such a convention to protect cultural diversity rights — are essential health-promoting public services any less important?
If health is to be a central plank in foreign policy, there are a few essential nails we must use to hammer it in securely.
Human rights and the right to health must be accepted as superordinate to trade agreements in national legislation.
All international negotiations and agreements must be assessed for how they actively support the right to health or do not weaken any government’s ability to protect this right.
Development assistance levels must be meaningful, reaching at least the 0.7% target, untied, and giving priority to the critical development sectors of health, education, and water and sanitation.
Global public goods such as the global funds for disease eradication should be supported more substantially; and new international conventions created to regulate international trade in health, education, and water and sanitation services so that greater equity in access, rather than greater liberalisation, is the explicit goal.
Trade rules must be fair. One size does not fit all. Developing countries need exemptions to become rich using the same policies and practice that today’s wealthy countries once used.
1: Millennium Development Goals (Goals 1–7)11
Goal 1: Eradicate extreme poverty and hunger
Target 1: Halve, between 1990 and 2015, the proportion of people whose income is less than one dollar a day.
Target 2: Halve, between 1990 and 2015, the proportion of people who suffer from hunger.
Goal 2: Achieve universal primary education
Target 3: Ensure that, by 2015, children everywhere, boys and girls alike, will be able to complete a full course of primary education.
Goal 3: Promote gender equality and empower women
Target 4: Eliminate gender disparity in primary and secondary education, preferably by 2005, and to all levels of education no later than 2015.
Goal 4: Reduce child mortality
Target 5: Reduce by two-thirds, between 1990 and 2015, the under-5 mortality rate.
Goal 5: Improve maternal health
Target 6: Reduce by three-quarters, between 1990 and 2015, the maternal mortality ratio.
Goal 6: Combat HIV/AIDS, malaria and other diseases
Target 7: Have halted by 2015, and begun to reverse, the spread of HIV/AIDS.
Target 8: Have halted by 2015, and begun to reverse, the incidence of malaria and other major diseases.
Goal 7: Ensure environmental sustainability
Target 9: Integrate the principles of sustainable development into country policies and programs and reverse the loss of environmental resources.
Target 10: Halve, by 2015, the proportion of people without sustainable access to safe drinking water.
Target 11: By 2020, to have achieved a significant improvement in the lives of at least 100 million slum dwellers.
- Ronald Labonte1
- Saskatchewan Population Health and Evaluation Research Unit, Universities of Saskatchewan and Regina, Saskatoon, SK, Canada.
For helpful editorial comments, I thank Ted Schrecker, Research Associate in Global Health, SPHERU, University of Saskatchewan.
R L received an honorarium from the Canadian Centre for Policy Alternatives for his contribution to the research on which this article is based.
- 1. Milanovic B. The two faces of globalization: against globalization as we know it. World Dev 2003; 31: 667-683.
- 2. Weisbrot M, Baker D, Kraev E, Chen J. The scorecard on globalization 1980–2000: twenty years of diminished progress. Centre for Economic and Policy Research, 2001. Available at: http://www.cepr.net/globalization/scorecard_on_globalization.htm (accessed Sep 2002).
- 3. Stiglitz J. Globalization and its discontents. New York: WWNorton, 2003.
- 4. Commission on Macroeconomics and Health. Macroeconomics and health: investing in health for economic development. Geneva: World Health Organization, 2001. Available at: www3.who.int/whosis/cmh/cmh_report/report.cfm (accessed May 2003).
- 5. Price-Smith A. The health of nations: infectious disease, environmental change, and their effects on national security and development. Cambridge, Mass: MIT Press, 2002.
- 6. Labonte R, Spiegel J. Setting global health research priorities. BMJ 2003; 326: 722-723.
- 7. Blouin C, Foster J, Labonte R. Canada’s foreign policy and health: toward policy coherence. Commission for the Future of Health Care in Canada, 2002. Available at: www.spheru.ca/www/html/Reports/Reports_globalization.htm (accessed May 2003).
- 8. Nygren-Krug H. 25 questions & answers on health & human rights. Geneva: WHO, 2002.
- 9. Hunt P. Economic, social and cultural rights: the right of everyone to the enjoyment of the highest attainable standard of physical and mental health: Report of the Special Rapporteur. Geneva: UN Commission on Human Rights, 2003. (Document E/CN.4/2003/58.)
- 10. Evan T. A human right to health? Third World Q 2002; 23: 197-215.
- 11. Deverajan S, Miller M, Swanson E. Goals for development: history, prospects and costs. Washington, DC: World Bank, 2002.
- 12. Brundtland G. [Speech to] Winterthur Massive Effort Advocacy Meeting. Geneva: WHO. 3 October 2000. Available at: http://www.who.int/director-general/speeches/2000/english/20001003_massive_effort.html (accessed Feb 2003).
- 13. Global Forum on Health. The 10/90 report on health research 2001–2002. Geneva: Global Forum on Health, 2002. Available at: www.globalforumhealth.org/pages/index.asp (accessed Feb 2003).
- 14. Social Watch. Social Watch Report No. 6. The social impact of globalisation in the world. Montevideo: Instituto del Tercer Mundo, 2002. Available at: http://www.socialwatch.org/en/informeImpreso/informe2002.htm (accessed Jan 2004).
- 15. Organisation for Economic Co-operation and Development. Development Co-operation: 2002 Report. DAC Journal 2003; 4. Available at: http://www.oecd.org/document/62/0,2340,en_2649_37413_2503486_119687_1_1_37413,00.html (accessed Mar 2003).
- 16. Canadian Council for International Cooperation. New initiatives for Africa: a Canadian response to NEPAD. A CCIC Briefing Note. Ottawa: CCIC, 2002.
- 17. BRIDGES Weekly Trade News Digest 2002; 6: 1, p.9.
- 18. Labonte R, Schrecker T, Sanders D, Meeus W. Fatal indifference: the G8, Africa and global health. Cape Town: University of Cape Town Press, 2004.
- 19. Canadian Centre for Policy Alternatives. Putting health first: Canadian health care reform, trade treaties and foreign policy. 2002. Available at: www.healthcarecommission.ca (accessed Dec 2002).
- 20. Adlung R, Carzaniga A. Health services under the General Agreement on Trade Services. In: Vieira C, Drager N, editors. Trade in health services: global, regional and country perspectives. Washington: Pan-American Health Organization, 2002: 13-33. Available at: www.paho.org/English/HDP/HDD/06Adlu.pdf (accessed May 2003).





Abstract
Foreign policy, especially trade policy, can have dramatic but rarely considered effects on public health.
International human rights covenants oblige governments to scrutinise their foreign policy, including trade policy, for its impact on the progressive realisation of the right to health.
Health is both a means and an end of development policy, but government investments in health are inadequate to reduce health disparities within and between nations. Few donor countries provide the agreed target of 0.7% of gross national income for development aid or toward reaching the Millennium Development Goals.
The progressive liberalisation requirement of the General Agreement on Trade in Services (GATS), if applied to commitments in health care, education, and water and sanitation services, may conflict with the progressive realisation obligation of the right to health. Alternatives to regulating trade in such essential services are proposed in this article.