Sudden death is a devastating complication of underlying cardiovascular disorder. In Australia and New Zealand, up to 80 000 people die suddenly each year from various causes.1 Although ischaemic heart disease accounts for most of these episodes, many other causes contribute.
Sudden cardiac death in the young (aged ≤ 35 years) has a structural basis in up to 80% of cases, 2,3 most commonly hypertrophic cardiomyopathy.4-6 In contrast, cardiac electrical disorders account for less than 10%.7 These arrhythmogenic disorders include long- QT syndrome,8 arrhythmogenic right ventricular dysplasia,9 idiopathic ventricular fibrillation, and Brugada syndrome.10 The latter is characterised by ST-segment elevation in the right precordial leads, frequently associated with right bundle branch block.10 In all these arrhythmogenic cardiac disorders there is no evidence of pathological abnormalities of the heart at postmortem examination, and death would be classified as being of unknown aetiology or unascertained. This label may under-estimate the incidence of arrhythmogenic causes of sudden death.
We sought to determine the frequency and potential causes of sudden cardiac death in a young Australian population.
The Department of Forensic Medicine at Westmead Hospital, Sydney, serves an area of New South Wales with over 2 million people. All autopsies performed in the Department from 1 January 1994 to 31 December 2002 were included in our study. All available demographic, clinical and autopsy data were collected from database files. In individuals who had died aged 35 years or younger, a detailed analysis and review of all records was performed to determine as accurately as possible the person’s clinical background and demographic details, the circumstances of the death, and the findings at autopsy. Police and ambulance documentation was also reviewed where available.
Sudden death was defined as death occurring within 24 hours of the onset of symptoms (the definition used by the World Health Organization). 1,7 If the death was witnessed, information regarding the circumstances of the death was obtained (eg, death during exercise). Coronary artery disease as the primary cause of death was defined on clinical grounds (eg, electrocardiographic evidence of myocardial infarction), and post-mortem findings (eg, presence of recent myocardial infarction, recent coronary artery thrombosis, or coronary artery stenosis greater than 50%).
All studies and data review were performed with maintenance of confidentiality and in strict accordance with the Central Sydney Area Health Service human ethics guidelines. The NSW Deputy State Coroner gave permission for the study to be performed.
Of the 10 199 autopsies (all coroner’s cases) performed from 1 January 1994 to 31 December 2002, there were 2986 deaths in people aged 35 years and younger, of which 652 were natural deaths. Non-cardiac natural deaths were identified in 413 (63.3%) subjects aged ≤ 35 years. The causes of these non-cardiac deaths are summarised in Box 1.
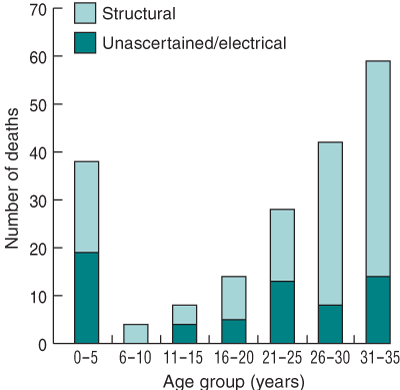
The remaining 239 deaths (36.7%) were identified as cardiac deaths, and included 60 unascertained cases, which we regarded as cardiac by exclusion. Of these 239 deaths, 46 were not sudden. Therefore, 193 sudden, natural and presumed cardiac deaths were identified (Box 2). Most sudden cardiac deaths in young people occurred in males (65%). This male predominance was also seen after excluding coronary artery disease deaths from the analysis (63% males, excluding coronary artery disease). The mean age at death in this group was 21.9 years. The distribution of sudden cardiac deaths within age groups is shown in Box 3. Although sudden cardiac death occurred in all age groups, there was an increased incidence in the first 5 years of life, and a second peak in the age group 31–35 years.
Of these 193 sudden cardiac deaths, 22% occurred during exercise and 38% during minimal exertion or at rest; 40% were not witnessed. The sudden death event occurred out of hospital in 82%. The most common cause of sudden cardiac death in this young population was “unascertained, presumed primary arrhythmogenic disorder” (60 subjects; 31%). These were sudden deaths in which the heart was structurally normal, both macroscopically and histologically, and there were no abnormalities on toxicological evaluation (Box 4).
Coronary artery disease was the second most common cause of sudden cardiac death in the young (24%; Box 2). Most (65%) coronary deaths in the younger age group occurred in individuals aged 30–35 years. Acute complications of congenital heart disease (eg, tetralogy of Fallot and transposition of the great vessels) caused 7% of sudden cardiac deaths in people aged ≤ 35 years, and arrhythmogenic right ventricular dysplasia was identified in 3%.
We have described the causes of sudden natural death in the young (aged 35 years and younger) in a large Australian population over a 9-year period. The cause of death in 31% was unascertained. Such sudden deaths are presumed, from their circumstances, to be cardiac in nature. However, as the postmortem finding was of a structurally normal heart, a primary arrhythmogenic disorder would be considered the likely cause of death. Primary arrhythmogenic disorders are an important cause of sudden death in the young, and most are likely to be caused by underlying disease-causing genetic defects.
Interestingly, the commonest cause of sudden cardiac death in the United States4,11 and in most of Europe12 (hypertrophic cardiomyopathy) was a less frequent cause of sudden cardiac death in young Australians.
There are now more than 30 cardiovascular disorders in which a genetic cause has been identified; 13,14 many of these can lead to sudden unexpected cardiac death, particularly in the young. While structural genetic heart diseases have been shown to cause sudden death, the incidence of primary arrhythmogenic disorders of the heart in causing sudden death in the young has not been established, principally because the heart is likely to be structurally normal at autopsy in most cases.
That most primary arrhythmogenic disorders are likely to be caused by underlying genetic defects has significant implications for clinical management. Most of the cardiac genetic disorders that cause sudden death in the young are inherited as an autosomal dominant trait, with 50% of offspring from an affected individual being at risk of developing the same disease. Therefore, correct identification of such cases at autopsy will enable appropriate clinical screening of surviving family members. Family screening is particularly important with the advent of preventive therapies for sudden death (eg, the implantable cardioverter defibrillator).15 Implantable defibrillator therapy may explain the smaller proportion in our study of sudden cardiac deaths in young people caused by hypertrophic cardiomyopathy.
We are likely to have underestimated the incidence of primary arrhythmogenic causes of sudden cardiac death in young people. Primary arrhythmogenic disorders can be the underlying cause in a variety of other deaths. For example, deaths attributed to events such as drowning and motor-vehicle accidents may have been directly precipitated by a fatal ventricular arrhythmia. This has been illustrated in familial long-QT syndrome, where an association exists between swimming and development of ventricular arrhythmias and sudden death.16 Furthermore, recent studies suggest that up to 20% of sudden infant death syndrome (SIDS) deaths (which we considered a “non-cardiac” cause) are associated with gene defects that cause familial long-QT syndrome.17,18
Our results highlight the importance of correct diagnosis of genetic cardiac disorders, appropriate family screening of at-risk individuals, and initiation of preventive strategies, such as implantable defibrillator therapy.
1: Non-cardiac sudden deaths in young Australians
Cause of death |
Number (%) |
||||||||||
Deaths in infancy (eg, stillbirths, in-utero deaths, SIDS)* |
181 (43.8%) |
||||||||||
Pulmonary (eg, asthma, pulmonary embolism) |
88 (21.3%) |
||||||||||
Neurological (eg, epilepsy, subarachnoid haemorrhage) |
70 (16.9%) |
||||||||||
Gastrointestinal |
22 (5.3%) |
||||||||||
Others† |
52 (12.6%) |
||||||||||
Total |
413 (100%) |
||||||||||
* Sudden infant death syndrome (SIDS) deaths in 23 (13% of deaths in infancy). † Includes metabolic disorders (21%), hepatobiliary disease (12%), malignancy (6%) and septicaemia (6%). |
|||||||||||
2: Sudden cardiac deaths in young Australians
Cause of death |
Number (%) |
||||||||||
Unascertained, probable primary arrhythmia |
60 (31%) |
||||||||||
Coronary artery disease |
46 (24%) |
||||||||||
Hypertrophic cardiomyopathy/unexplained left ventricular hypertrophy |
29 (15%) |
||||||||||
Myocarditis (mostly viral) |
23 (12%) |
||||||||||
Congenital heart disease |
14 (7%) |
||||||||||
Other* |
21 (11%) |
||||||||||
Total |
193 (100%) |
||||||||||
* Includes aortic dissection (29%), valvular heart disease (24%), and arrhythmogenic right ventricular dysplasia (14%). |
|||||||||||
4: Characteristics of the 60 people ≤ 35 years for whom cause of death was not ascertained
Structurally normal heart at autopsy.
No abnormal histopathological findings in the heart at autopsy.
No other cause of death identified at autopsy (eg, pulmonary embolism, subarachnoid haemorrhage).
Normal results of a toxicological screen.
No pre-death clinical features to suggest other cause of sudden death (eg, epilepsy, asthma).
Received 11 September 2003, accepted 1 December 2003
- Alessandra Doolan1
- Christopher Semsarian2
- Neil Langlois3
- 1 Agnes Ginges Centre for Molecular Cardiology, Centenary Institute, Newtown, NSW.
- 2 Department of Forensic Medicine, Westmead Hospital, Wentworthville, NSW.
C S is the recipient of a National Heart Foundation of Australia fellowship. A D is the recipient of an Australian Postgraduate Award. The research is supported by project grants from the National Heart Foundation of Australia and the National Health and Medical Research Council.
None identified
- 1. Tunstall-Pedoe H, Kuulasmaa K, Amouyel P, et al. Myocardial infarction and coronary deaths in the World Health Organization MONICA Project: registration procedures, event rates, and case-fatality rates in 38 populations from 21 countries in four continents. Circulation 1994; 90: 583-612.
- 2. Bowker TJ, Wood DA, Davies MJ, et al. Sudden, unexpected cardiac or unexplained death in England: a national survey. QJM 2003; 96: 269-279.
- 3. Semsarian C, Maron BJ. Sudden cardiac death in the young. Med J Aust 2002; 176: 148-149. <MJA full text>
- 4. Maron BJ, Shirani J, Poliac LC, et al. Sudden death in young competitive athletes – clinical, demographic and pathological profiles. JAMA 1996; 276: 199-204.
- 5. Semsarian C, Seidman CE. Molecular medicine in the 21st century. Intern Med J 2001; 31: 53-59.
- 6. Chung J, Tsoutsman T, Semsarian C. Hypertrophic cardiomyopathy: from gene defect to clinical disease. Cell Res 2003; 13: 9-20.
- 7. Virmani R, Burke AP, Farb A. Sudden cardiac death. Cardiovasc Pathol 2001; 10: 275-282.
- 8. Moss AJ. Long QT syndrome. JAMA 2003; 289: 2041-2044.
- 9. Thiene G, Basso C, Danieli G, et al. Arrhythmogenic right ventricular cardiomyopathy. Trends Cardiovasc Med 1997; 7: 84-90.
- 10. Brugada P, Brugada J. Right bundle-branch block, persistent ST segment elevation and sudden cardiac death: a distinct clinical and electrocardiographic syndrome. A multicenter report. J Am Coll Cardiol 1992; 20: 1391-1396.
- 11. Maron BJ. Hypertrophic cardiomyopathy: a systematic review. JAMA 2002; 287: 1308-1320.
- 12. Maron BJ, Olivotto I, Spirito P, et al. Epidemiology of hypertrophic cardiomyopathy-related death: revisited in a large non-referral-based patient population. Circulation 2000; 102: 858-864.
- 13. Milewicz DM, Seidman CE. Genetics of cardiovascular disease. Circulation 2000; 102: 103-111.
- 14. Priori SG, Barhanin J, Hauer R, et al. Genetic and molecular basis of cardiac arrhythmias: impact on clinical management. Circulation 1999; 10: 518-528.
- 15. Maron BJ, Shen W, Link MS, et al. Efficacy of implantable cardioverter-defibrillators for the prevention of sudden death in patients with hypertrophic cardiomyopathy. N Engl J Med 2000; 342: 365-373.
- 16. Moss AJ, Robinson JL, Gessman L, et al. Comparison of clinical and genetic variables of cardiac events associated with loud noise versus swimming among subjects with the long QT syndrome. Am J Cardiol 1999; 84: 876-879.
- 17. Schwartz PJ, Segantini A. Cardiac innervation, neonatal electrocardiography and SIDS. A key for a novel preventive strategy? Ann N Y Acad Sci 1988; 533: 210-220.
- 18. Schwartz PJ, Stramba-Badiale M, Segantini A, et al. Prolongation of the QT interval and the sudden infant death syndrome. N Engl J Med 1998; 338: 1709-1714.





Abstract
Objectives: To determine the causes of sudden cardiac death in people aged 35 years or younger.
Design and setting: A review of all autopsies performed between 1 January 1994 and 31 December 2002 at a major Sydney forensic medicine department serving an area with over 2 million people.
Main outcome measures: Incidence of various types of cardiac disease causing sudden death in those aged ≤ 35 years; proportion of deaths in which no cause was found at autopsy.
Results: There were 10 199 autopsies performed during the study period. Of these, 2986 (29.2%) deaths occurred in people aged ≤ 35 years; 193 were classified as sudden cardiac deaths. The cause of sudden death in this group was not established in 60 (31%), and was presumed to be due to primary arrhythmogenic disorders. Coronary artery disease occurred in 46 (24%), hypertrophic cardiomyopathy/unexplained left ventricular hypertrophy in 29 (15%), and myocarditis in 23 (12%).
Conclusions: Unexplained deaths, presumed to result from sudden primary arrhythmogenic causes, occur in young Australians with structurally normal hearts. That underlying disease-causing genetic defects may be involved has clinical implications for family members.