In Australia, the principles of natural justice are considered central to fair decision making in the courts and many tribunals.1,2 The principles can be summarised as follows:1
The right to a fair hearing. This requires a decision maker to allow a person whose interests may be adversely affected by a decision to present his or her case.
The rule against bias. This requires a decision maker to be unbiased in relation to the matter to be decided.
The evidence rule. This requires that a decision be based on the evidence provided, and not on irrelevant issues.
Human research ethics committees (HRECs) aim to protect the welfare and rights of participants in research.3 A secondary role is to facilitate research that is or will be of benefit to the researcher’s community or to humankind.3 While there is currently no statutory requirement for HRECs to apply the principles of natural justice, the principles would seem to be relevant to the assessment of research proposals. Indeed, some observers have argued that the decision making processes of HRECs may sometimes seem unfair.4,5
We hypothesised that natural justice principles would be variably understood and applied by different HRECs. To test our hypothesis, we conducted an Australia-wide survey of Chairs of HRECs.
The study was conducted between April and September 2002. We sent a postal questionnaire to the Chair of every HREC on a list of Australian HRECs from the Australian Health Ethics Committee of the National Health and Medical Research Council (NHMRC). The mail-out included a cover letter, a consent form, a “Do not wish to respond” form, and a prepaid return envelope.
The cover letter described the principles of natural justice,1 explained that published results would be non-identifying, and stated that the Austin Health HREC had approved the study. The cover letter and questionnaire gave specific examples of possible bias (conflict of interest), such as an HREC member standing to gain professionally or financially from the project (positive bias) or having a competing research interest (negative bias).3 Examples of questions asked in the survey are shown in Box 1.
Response rates. Of the 212 HRECs on the NHMRC list, 11 no longer existed as independent committees. Of the 201 remaining HRECs, 110 (55%) returned completed questionnaires, 56 (28%) declined to participate, and 35 (17%) did not reply. Across four broad groups of HRECs the response rates were as follows: 68 from 111 hospitals (61%); 20 from 38 universities (53%); 12 from 20 public institutions (60%); and 10 from 29 private institutions (34%).
Several Chairs who declined to take part in the survey commented on their reasons for not participating. Two felt that the study was unscientific and biased. One declined after receiving formal advice not to participate. (The advice was based on a confusion of “natural justice” with “natural law” — the latter involving philosophical concepts of society and religion.6) Two Chairs said they did not have the time or resources to complete the survey. One replied, “Having been involved with HRECs over many years I have never used these natural justice principles, nor have I felt the need”.
Familiarity with principles of natural justice. The degree of familiarity with the principles of natural justice varied widely, although the pattern was similar for the three components: bias, being heard, and evidence (ie, individual respondents were about equally familiar or unfamiliar with all three principles). Thirty-three per cent of respondents stated that they were very familiar with the principles, while 25% were completely unfamiliar with the principles.
About three-quarters of the respondents felt that natural justice principles should apply in decision making by HRECs, and also believed that their HREC usually applied these principles. However, about 5% strongly disagreed that natural justice principles should apply to HRECs, and 5% stated that their HREC never applied the principles of natural justice.
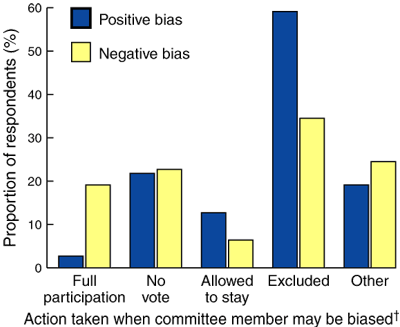
Positive and negative bias. About three-quarters of respondents said they would exclude a committee member from voting on a proposal if that member had a possible positive bias towards the project. However, less than half the respondents said they would exclude a member with a possible negative bias (Box 2). Several respondents commented that they had not previously considered issues of negative bias. Several replied that because they had a consensus approach to decisions that they felt issues of bias did not apply.
Methods available for initial submission of research proposals. Almost all the HRECs required that the initial submission of a research proposal be in written form. About half the respondents said their HREC may ask individual researchers to give an oral presentation, but only a third said that researchers themselves were allowed to request an oral presentation.
Mechanisms for evaluating the scientific validity of a research proposal. Many HRECs used more than one mechanism to determine scientific validity: about a quarter used formal scientific committees to evaluate the evidence before consideration by the HREC, two-thirds consulted experts outside the HREC, and three-quarters reported that, in certain instances, the full HREC considered the scientific issues.
How HRECs communicate problems in research proposals to researchers. For research proposals deemed unacceptable, most HRECs used structured written comments, at least some of the time, to communicate the reasons for their decision to the researchers.
Researchers’ right of reply when a research proposal is deemed unacceptable. Many HRECs used more than one approach to giving researchers the right of reply. About half the respondents indicated that, when a proposal was considered unacceptable, the researchers would be invited to resubmit their case in person to a subsequent committee meeting. Half invited resubmission to a designated HREC member. Most encouraged written resubmission. One respondent indicated there was no right of reply.
Membership of HRECs. On average, about half the membership of HRECs was drawn from outside the institutions they served. Two-thirds of HREC members were appointed by external administrators.
Our results show that there is wide variation among HRECs in the understanding and application of natural justice principles.
A weakness of our study was that only 55% of potential respondents completed the questionnaire. The perception that the study was “unscientific” and “biased” (expressed by two HREC Chairs who declined to participate) may have been one reason why 28% of Chairs did not respond. An anonymous survey may have increased the primary response rate, but would not have allowed follow-up of non-responders.7 Another issue is that the views expressed by the HREC Chairs may have differed considerably from those of other HREC members. However, we felt that it was impractical to attempt to survey the views of every member of each HREC.
Bias. Avoiding possible positive bias may protect research participants by reducing the risk of HRECs approving inappropriate studies. Avoiding possible negative bias may facilitate approval of research that may ultimately benefit the community or humankind in general.
The NHMRC’s National statement on ethical conduct in research involving humans3 states that no member of an HREC should adjudicate on a study where they have any conflict of interest (possible bias). Its more recent Human research ethics handbook8 goes further, stating that a member with a conflict of interest should completely withdraw from the meeting and “should not discuss the project or attempt to influence the committee in any way”. This statement applies to both positive and negative bias.
In our survey, about three-quarters of respondents said they would exclude a committee member with a possible positive bias from voting on a proposal. McNeill et al,9 in one of the few studies of HREC processes, found that about half the HRECs surveyed had a policy of excluding members from reviewing their own projects (possible positive bias).
Another way to reduce the chance of bias (particularly positive bias) is to appoint HREC members from outside the institutions served by the HRECs. Our survey showed that about half of HREC members were externally appointed.
Fair hearing. Although natural justice requires an adequate opportunity to address the issues raised, the application of natural justice does not necessarily imply the right to a personal hearing.2 The ability to appear in person before an HREC may, however, promote better understanding between the HREC and the researchers.8 Another aspect of having a fair hearing is receiving clear communication from the HREC about its criticisms and the precise nature of any required changes. The combination of a written response followed by oral feedback may provide the best mechanism for clear communication.
Our survey showed that most HRECs require initial research proposals to be submitted in written form, and about half may invite researchers to give an oral presentation at a later stage. For proposals deemed unacceptable, most HRECs communicate their reasons via structured written comments.
Evidence. The evidence rule is a relatively recent addition to the Australian interpretation of natural justice but is now well established in courts of law.1 Nevertheless, two of our respondents disputed that the evidence rule was part of natural justice.
Chalmers et al4 and McNeill10 have suggested that the scientific aspects of a research proposal could be clarified before the proposal is reviewed by the full HREC. A scientific committee may be better placed to determine the relevant scientific issues and provide a fair hearing on these issues. The full HREC would then consider the ethical issues of a study approved by the scientific committee.
We found that only about a quarter of HRECs consulted formal scientific committees for this purpose.
The requirement for natural justice. Our results indicate that many HRECs are applying the principles of natural justice in various ways, even if some members are unfamiliar with the exact nature of the principles.
There is currently neither a statutory requirement for HRECs to apply the principles of natural justice, nor is there relevant case law in this area. In other administrative areas, judges have attempted to define tests for the need to apply natural justice in a given situation. In an important Australian High Court decision, Justice Mason concluded:
The law has now developed to a point where it may be accepted that there is a common law duty to act fairly, in the sense of according procedural fairness (natural justice), in the making of administrative decisions which affect rights, interests and legitimate expectations, subject only to the clear manifestation of a contrary statutory intention.11
Do the decisions of an HREC materially affect the interests of a biomedical PhD student or someone employed as a clinician–researcher? Does the successful passage of a multicentre study through other HRECs provide a legitimate expectation of success? One contributor to the NHMRC handbook8 commented:
HRECs might consider if, when, and how they apply natural justice. The effect of a decision on the rights and interests of participants as well as the interests and legitimate expectations of researchers could be considered when going through the HREC process.8,11 Further, the potential benefit to the broader community could be considered.3,8,11 Minimising possible bias and optimising communication may both improve protection of participants and facilitate research.
Received 19 June 2003, accepted 23 October 2003
- Gabrielle L Van Essen1
- David A Story2
- Stephanie J Poustie3
- Max M J Griffiths4
- Cynthia L Marwood5
- 1 Austin Health, Austin Hospital, Heidelberg, VIC.
- 2 Kew, VIC.
Our study was funded by the Research Fund of the Department of Anaesthesia, Austin Health.
None identified.
- 1. Allars M. Introduction to Australian administrative law. Sydney: Butterworths, 1994.
- 2. Forbes J. Justice in tribunals. Sydney: Federation Press, 2002.
- 3. National Health and Medical Research Council. National statement on ethical conduct in research involving humans. Canberra: NHMRC, 1999.
- 4. Chalmers D, Pettit P, on behalf of the Australian Health Ethics Committee. Towards a consensual culture in the ethical review of research. Med J Aust 1998; 168: 79-82.
- 5. Jamrozik K, Kolybaba M. Are ethics committees retarding the improvement of health services in Australia? Med J Aust 1999; 170: 26-28.
- 6. Robertson D. The penguin dictionary of politics. 2nd ed. London: Penguin Books, 1993.
- 7. Alreck P, Settle R. The survey research handbook. 2nd ed. New York: McGraw-Hill, 1995.
- 8. National Health and Medical Research Council. Human research ethics handbook. Commentary on the National Statement on Ethical Conduct in Research Involving Humans. Canberra: NHMRC, 2002.
- 9. McNeill PM, Berglund CA, Webster IW. Reviewing the reviewers: a survey of institutional ethics committees in Australia. Med J Aust 1990; 152: 289-296.
- 10. McNeill P. The ethics and politics of human experimentation. Cambridge: Cambridge University Press, 1993.
- 11. Kioa v Minister for Immigration and Ethnic Affairs (Kioa v West). (1985) 159 CLR 550 at 584.





Abstract
Objective: To determine how familiar human research ethics committees (HRECs) are with the principles of natural justice and whether they apply these principles.
Design and setting: A postal survey conducted between April and September 2002 of the Chairs of all HRECs registered with the Australian Health Ethics Committee of the National Health and Medical Research Council (NHMRC) in 2001.
Main outcome measures: HRECs’ reported familiarity with, and application of, three principles of natural justice: (1) the hearing rule, requiring a decision maker to allow a person affected by a decision to present his or her case; (2) the rule against bias, requiring a decision maker to be unbiased in the matter to be decided; and (3) the evidence rule, requiring that a decision be based on the evidence provided, and not irrelevant issues.
Results: From 201 Chairs of HRECs Australia-wide, we received 110 completed questionnaires (55% response rate). About 33% of respondents were very familiar with the principles of natural justice, and 25% completely unfamiliar. Most respondents felt that natural justice should be, and usually is, applied by HRECs. In cases of possible positive bias of an HREC member towards a research proposal, 70% of respondents said they would exclude the member from decision making. In cases of possible negative bias, 43% said they would exclude the HREC member.
Conclusion: The degree of familiarity with principles of natural justice varies widely among Chairs of HRECs. While many respondents felt that HRECs usually apply natural justice, responses to questions about bias suggest that HRECs do not always exclude members with possible bias, contrary to NHMRC guidelines.