Medical errors occur when people unintentionally use a wrong plan to achieve an aim, or fail to carry out a planned action as intended.1 Expert groups established to examine medical error in the United Kingdom,2 Australia3 and the United States4 have stressed the fundamental importance of incident reporting to identify when things go wrong. Progress is being made in each of these countries in establishing national mandatory and voluntary reporting systems. The report from the US Institute of Medicine4 stated that the functions of incident reporting were to hold healthcare providers accountable for performance (achieved through mandatory reporting), and to provide information to improve safety.
A recent US survey showed that people recognise the value of incident reporting in protecting patient safety: 62% of respondents believed voluntary reporting would reduce errors, rising to 71% if reporting was mandatory.5 Another survey found that 73% of American respondents favoured a mandatory reporting system and public accountability of medical error information, whereas 21% supported voluntary incident reporting.6
Despite recognition of the value of incident reporting, many errors go unreported by healthcare workers.7 Reasons for reluctance to report incidents have a common theme — that self-identification could result in personal repercussions.8-13 Within the medical profession, views about the reporting process range from providing clinicians with the option of reporting errors anonymously11 through to a fundamental requirement for transparency to retain professional ethics.14,15
Throughout this debate, the views of the key stakeholder group — the general public — on the question of anonymity versus transparency have not been reported.
The aims of our survey were to gauge Australian respondents’ opinion of (i) incident reporting, and (ii) disclosure of the identity of the healthcare worker(s) involved in a medical error.
The data for our study were collected in the 2002 South Australian Health Monitor survey.16,17 People aged 18 years or older living in metropolitan and country areas in South Australia were interviewed by telephone. The telephone numbers called were randomly selected from the respective telephone directories. The person in each household whose birthday was nearest to the date of the survey was interviewed. The survey was designed to have sufficient respondents to achieve a minimum of ± 2.0% accuracy, with 95% confidence intervals, for any questionnaire item.
A descriptive analysis was used to ascertain the proportion of respondents who wanted incident reporting and healthcare workers to be identified on incident reports, with 95% CIs provided. To identify predictors of attitudes towards incident reporting and healthcare worker anonymity, univariate analyses of demographic factors were undertaken by generalised linear modelling. Respondents who did not have a definite answer were excluded from the analyses (< 2% of respondents). In the analysis, respondents were weighted by age, sex and geographical region to be representative of the South Australian population (Box 1).18 The survey procedures of the STATA statistical software package20 were used for this analysis.
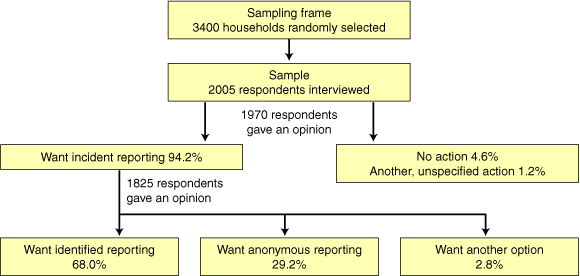
The survey was conducted between 4 and 14 April 2002. From the initial 3400 households randomly selected, 711 households were not able to be contacted on the telephone number listed (370 were disconnected or were fax/modem numbers, no contact was made for 274 despite six callbacks, and 67 were non-residential numbers), 420 people contacted refused to take part, 181 were unavailable or too sick or hearing impaired to take part, and 83 did not speak English. Thus, 2005 interviews were conducted, giving a response rate of 74.6%.
Based on the vignette, 1856 respondents, or 94.2% (95% CI, 93.0%–95.2%) of those with an opinion (n = 1970), believed that a report should be written when an error occurred. Ninety respondents, or 4.6% (95% CI, 3.7%–5.7%), thought reporting the incident was unnecessary and 24 respondents, or 1.2% (95% CI, 0.8%–1.9%), thought another, unspecified action should be taken.
There were no statistically significant differences in demographic profile between those who wanted incident reporting and those who did not.
Of those in favour of incident reporting, and who had an opinion regarding anonymous or identified reporting (n = 1825), 1242 respondents, or 68.0% (95% CI, 65.5%–70.5%), thought that the healthcare worker should identify him- or herself on the incident report form, even though this may lead to disciplinary action; 532 respondents, or 29.2% (95% CI, 26.7%–31.7%), thought that, to encourage reporting, the report should be anonymous; and 51 respondents, or 2.8% (95% CI, 2.1%–3.7%), favoured other, unspecified options. The results are summarised in Box 2.
There were no statistically significant differences in demographic profile between those who wanted healthcare workers to be identified on incident reports and those who did not.
We found that nearly all respondents believed healthcare workers should report errors, even when the outcome of the error was transient and had no long-term health effects on the patient. Our findings relate to a minor medical error, but nevertheless concur with those of a US survey relating to serious injury or harm from medical errors: 94% of consumers believed that these medical errors should be reported, either on a voluntary or mandatory basis.6 Two-thirds of our respondents who were in favour of incident reporting believed that healthcare workers should have to identify themselves, despite the suggestion in the survey question that this might discourage people from reporting mistakes.
Reasons for favouring a system where transparency is assured are likely to be complex. Reluctance to accept anonymity may reflect scepticism about whether information will be effectively managed by healthcare institutions if those who make the report are not identified, and that the interests of the healthcare worker and/or hospital could be placed above those of the consumer.21 By withholding the reporter’s details, people might assume that patient details are also withheld, and that the incident might not be fully investigated.
In Australia, there has been considerable attention focused on clinical errors and perceived lack of transparency by the medical profession in dealing with patients and their families.22 This, in conjunction with the recent medical indemnity crisis, can only serve to further diminish public confidence in healthcare safety and lead to a call for greater organisational transparency.
That two-thirds of respondents wanted identified reporting may also indicate that people still regard errors to be the result of a particular person not performing to a perceived standard. Consumer doubts about safety are likely to be fuelled by media coverage of adverse events, which in some countries is greater than ever before,23 and often focuses attention on individual negligent clinicians.
The individualising of errors is contrary to current quality improvement philosophy, which promotes a system-based approach to the handling of errors. There is recognition that serious errors are usually linked to the failure of multiple systems and the involvement of many individuals.12 Incident reporting in Australia was designed by anaesthetists as an anonymous reporting system, which is said to enable the reporting of a “rich mass of ‘human factors’ information that would not otherwise be reported”.11 The establishment of an anonymous reporting system has been successful in identifying problems, and is purported to have resulted in significant improvements in the delivery of anaesthesia.24
The public desire for identified incident reporting provides a challenge for quality improvement programs to meet the needs of both consumers and healthcare workers. It is likely that both the public and healthcare workers need to be educated about the complexities of errors in hospitals, and the vulnerability of healthcare workers to making mistakes. It is also the responsibility of hospital administrators and clinicians to ensure that an open and transparent system of disclosing errors to consumers is fostered.
It will be a challenge to achieve open disclosure if recent findings in the United States also reflect sentiment in Australia: 62% of consumers, as opposed to 14% of physicians, believed that hospital reports of serious medical errors should be released to the public.5
Our study has several limitations. Firstly, to decrease the burden on respondents, we used a single vignette relating to a minor error, so the outcome has limited generalisability. We chose a minor error, assuming that if respondents favoured incident reporting for minor errors they would be unlikely to oppose incident reporting for more serious errors. A recent survey supports this. When given a medical error vignette with two different patient outcomes — one resulting in death and the other in complete recovery — respondents were more likely to support imposing fines, suspending healthcare workers from duty, and initiating malpractice lawsuits if the medical error led to the patient’s death.5 In limiting the vignette to only two questions, we were unable to explore community preferences regarding whether information obtained through incident reporting should be made available to the patient, or evaluate opinion on revealing patient identity as part of the process.
Secondly, the way in which the vignette was worded focused on an individual who made a mistake. Had the vignette outlined a system flaw, or had respondents been made aware of modern theories of accident causation and prevention, their responses may have been different. Finally, the sampling frame was restricted to consenting adults who were listed in the telephone directory, spoke English and were well enough to speak on the telephone. While a response rate of 74.6% was achieved, results are representative only of this population.
Eliciting consumer opinion on healthcare is progressively being seen as an important tool in improving clinical care.25 National and state quality improvement activities which focus on identifying system rather than individual flaws, as well as open-disclosure policies, will both assist the public in accepting healthcare worker anonymity and give healthcare workers the confidence to identify themselves on incident reports without fear of recrimination.
1: Demographic profile of the respondent sample (n = 2005), which was weighted by age, sex and geographical region to be comparable with the total population of South Australia in 2000 (n = 1 497 600)18
Variable |
Men |
Women |
Total |
SA Census 2001*19 |
|||||||
Age (years) |
n = 980 |
n = 1020 |
n = 2000 |
|
|||||||
18–39 |
406 |
41.4% |
407 |
39.9% |
813 |
40.6% |
|
|
|||
40–59 |
349 |
35.6% |
346 |
33.9% |
695 |
34.8% |
|
|
|||
60+ |
225 |
23.0% |
267 |
26.2% |
492 |
24.6% |
|
|
|||
Residence |
n = 981 |
n = 1024 |
n = 2005 |
|
|||||||
Country |
263 |
26.8% |
258 |
25.2% |
521 |
26.0% |
|
|
|||
Metropolitan |
718 |
73.2% |
766 |
74.8% |
1484 |
74.0% |
|
|
|||
Annual household income ($) |
n = 913 |
n = 889 |
n = 1802 |
n = 514 598† |
|||||||
≤ 20 000 |
173 |
18.9% |
245 |
27.5% |
418 |
23.2% |
84 306 |
16.4% |
|||
20 001–80 000 |
522 |
57.2% |
509 |
57.3% |
1031 |
57.2% |
354 933 |
69.0% |
|||
80 001+ |
218 |
23.9% |
135 |
15.2% |
353 |
19.6% |
75 359 |
14.6% |
|||
Country of birth |
n = 981 |
n = 1024 |
n = 2005 |
n = 1 458 912 |
|||||||
Australia |
763 |
77.8% |
814 |
79.5% |
1577 |
78.7% |
1 099 591 |
75.4% |
|||
Europe |
|
|
|
|
|
|
|
|
|||
UK/Ireland |
106 |
10.8% |
118 |
11.5% |
224 |
11.2% |
127 274 |
8.7% |
|||
Other |
57 |
5.8% |
36 |
3.5% |
93 |
4.6% |
75 723 |
5.2% |
|||
Asia |
10 |
1.0% |
12 |
1.2% |
22 |
1.1% |
34 948 |
2.4% |
|||
Other |
45 |
4.6% |
44 |
4.3% |
89 |
4.4% |
121 376 |
8.3% |
|||
| * 2001 Census data for annual household income and country of birth are provided for comparison. These data were not available for weighting the respondent sample when the survey was conducted in April 2002. † Census data missing for 52 476 households. | |||||||||||
- Sue M Evans1
- Jesia G Berry2
- Brian J Smith3
- Adrian J Esterman4
- 1 Clinical Epidemiology and Health Outcomes Unit, The Queen Elizabeth Hospital, Adelaide, SA.
- 2 Flinders Centre for Epidemiology and Biostatistics, Flinders University, Adelaide, SA.
We would like to thank the South Australian Department of Human Services Centre for Population Studies in Epidemiology for conducting the Health Monitor survey. We would also like to thank staff of the Clinical Epidemiology and Health Outcomes Unit, Mr Adrian Heard and Mr Colin McIver for their contribution to the project.
None identified.
- 1. Runciman WB, Merry AF, Tito F. Error, blame and the law in health care — an antipodean perspective. Ann Intern Med 2003; 138: 974-979.
- 2. Expert Group on Learning from Adverse Events in the NHS. An organisation with a memory. London: Stationery Office, 2000.
- 3. Australian Council for Safety and Quality in Health Care. National Action Plan 2002. Canberra: Safety and Quality Council, 2002.
- 4. Kohn LT, Corrigan JM, Donaldson MS. To err is human: building a safer health system. Washington, DC: National Academy Press, 2000: 1-16.
- 5. Blendon RJ, DesRoches CM, Brodie M, et al. Views of practicing physicians and the public on medical errors. N Engl J Med 2002; 347: 1933-1940.
- 6. Kaiser Family Foundation/Agency for Healthcare Research and Quality. National Survey on Americans as Health Care Consumers: an update on the role of quality information. Rockville, Md: Henry J Kaiser Family Foundation, 2000.
- 7. Leape LL. Error in medicine. JAMA 1994; 272: 1851-1857.
- 8. Vincent C, Stanhope N, Crowley-Murphy M. Reasons for not reporting adverse incidents: an empirical study. J Eval Clin Pract 1999; 5: 13-21.
- 9. Lawton R, Parker D. Barriers to incident reporting in a healthcare system. Qual Saf Health Care 2002; 11: 15-18.
- 10. Leape LL. Why should we report adverse incidents? J Eval Clin Pract 1999; 5: 1-4.
- 11. Runciman W, Merry A, Smith AM. Improving patients’ safety by gathering information. Anonymous reporting has an important role. BMJ 2001; 323: 7308.
- 12. Cohen MR. Why error reporting systems should be voluntary. BMJ 2000; 320: 728-729.
- 13. Sucov A, Shapiro MJ, Jay G, et al. Anonymous error reporting as an adjunct to traditional incident reporting improves error detection. Acad Emerg Med 2001; 8: 498-499.
- 14. Barach P, Small SD. Reporting and preventing medical mishaps: lessons from non-medical near miss reporting systems. BMJ 2000; 320: 759-763.
- 15. Kaplan H, Barach P. Incident reporting: science or protoscience? Ten years later. Qual Saf Health Care 2002; 11: 144-145.
- 16. Department of Human Services. Centre for Population Studies in Epidemiology. Brief report, Number 2002-12. The Health Monitor Survey Methodology. Available at: www.dhs.sa.gov.au/pehs/PROS/br-monitor-method02-12.pdf (accessed Apr 2004).
- 17. Taylor AW, Wilson DH, Wakefield M. Differences in health estimates using telephone and door-to-door survey methods — a hypothetical exercise. Aust N Z J Public Health 1998; 22: 223-226.
- 18. Australian Bureau of Statistics. Estimated resident population by age and sex in statistical local areas, South Australia. Canberra: ABS, 2001. (Catalogue No. 3235.4.)
- 19. Australian Bureau of Statistics. 2001 Census. Basic community profile, South Australia [data file]. Canberra: ABS, 2002. (Catalogue no. 2001.0.)
- 20. STATA statistical software, release 7.0. College Station, Tex: Stata Corporation, 2001.
- 21. Hebert PC, Levin AV, Robertson G. Bioethics for clinicians: 23. Disclosure of medical error. CMAJ 2001; 164: 509-513.
- 22. McLean J, Walsh M. Lessons from the inquiry into obstetrics and gynaecological services at King Edward Memorial Hospital 1990-2000. Australian Council for Safety and Quality in Health Care, 2002. Aust Health Rev 2003; 26(1): 12-23.
- 23. Ali NY, Lo TY, Auvache VL, White PD. Bad press for doctors: 21 year survey of three national newspapers. BMJ 2001; 323: 782-783.
- 24. Gaba DM. Anaesthesiology as a model for patient safety in health care. BMJ 2000; 320: 785-788.
- 25. Cleary PD. The increasing importance of patient surveys. Now that sound methods exist, patient surveys can facilitate improvement. BMJ 1999; 319: 720-721.





Abstract
Objectives: To seek public opinion on the reporting of medical errors and the anonymity of healthcare workers who report medical errors.
Design and participants: A random, representative survey of 2005 South Australians in April 2002, using telephone interviews based on a vignette provided.
Main outcome measures: When a medical error occurs (i) whether the incident should be reported, and (ii) whether the report should disclose the healthcare worker’s identity.
Results: (i) Most respondents (94.2%; 95% CI, 93.0%–95.2%) believed healthcare workers should report medical errors. (ii) 68.0% (95% CI, 65.5%–70.5%) of those in favour of reporting believed the healthcare worker should be identified on the report, while 29.2% (95% CI, 26.7%–31.7%) favoured anonymous reporting.
Conclusions: Most respondents believed that, when a healthcare worker makes an error, an incident report should be written and the individual should be identified on the report. Respondents were reluctant to accept healthcare worker anonymity, even though this may encourage reporting.