Advances in molecular biology are providing important insights into the genetic basis of a number of medical conditions, including hereditary cancer syndromes. Highly penetrant heritable (“germline”) mutations may account for 5%–10% of the common cancers, including breast, colorectal and prostate cancers, and melanoma.1 Genetic testing, in the context of genetic counselling, is offered by familial cancer services for an increasing number of genes.2
Identifying a genetic mutation in an affected individual means that other family members can choose to determine whether they too carry this disease predisposition. For those who undertake “predictive testing” and are found not to carry the mutation, the costly burden of continuous surveillance or medical intervention and anxiety is usually lifted — for them and their descendants. Those who do carry the mutation can, where possible, be selected for close monitoring and cancer-risk-reduction strategies (such as intense surveillance, prophylactic surgery, chemoprevention and lifestyle changes). Emerging evidence suggests that people who choose to undergo genetic testing are less likely to be anxious and depressed than those who prefer not to know.3,4 Furthermore, clinic attendance has direct psychosocial benefits arising from risk assessment and genetic counselling.5
Concerns have been raised regarding the potential for genetic information to result in disadvantage in the workplace, or in obtaining health, disability or life insurance. This is commonly labelled as “genetic discrimination” and has received considerable media coverage, with headlines in the broadsheet newspapers such as “Genetic testing could create a new underclass”, “Push to keep life insurers’ noses out of our genes” and “Beware the genetic ambush”.6-8 In the context of income protection or life insurance, “genetic discrimination” should, more correctly, refer to misuse of the result of a genetic test when there are no reliable actuarial data to support an underwriter’s decision. Indeed, for many hereditary cancer syndromes, there is clinical uncertainty both about disease penetrance and the precise efficacy of risk-reduction strategies. This means that correct actuarial determination of risk for a given individual may currently only be possible for a few cancer-related (and other) genetic conditions.9
There has been little systematic documentation in Australia to determine the prevalence of genetic discrimination. Barlow-Stewart and Keays described 48 cases of alleged genetic discrimination, which they defined as adverse treatment because of a positive result of a genetic test.10 Most cases (which were unverified) apparently followed a positive result of a genetic test for an inherited predisposition to cancer that affected access to life insurance. The extent to which applicants are denied life insurance after a formal application is uncertain. A nationwide prospective empirical study will hopefully provide further objective assessment in this area.11 It appears that Australian life insurance companies have to date received very few insurance applications involving the results of genetic testing. However, submissions to the Australian Law Reform Commission (ALRC) and the Australian Health Ethics Committee indicate that a perceived fear of genetic discrimination in life insurance has caused individuals to avoid genetic testing.12 Outside Australia, reports of discrimination have also been largely anecdotal, leading some to suggest that the anticipated “wave” of genetic discrimination has so far failed to materialise.13,14
Group life insurance that provides term life cover for groups of people linked together through employment or superannuation should not place an individual at risk of genetic discrimination. Similarly, health insurance operates on a legally binding community loading principle, stating that “ . . . insurance cannot be denied on the basis of a medical history and medical risk”.15 In contrast, individual applications that are subject to risk assessment, such as applications for voluntary life insurance or income-protection insurance, are potential targets for genetic discrimination. Little has been reported on what information insurance companies actually require from applicants. Therefore, for insurance companies operating in Australia, we determined what questions about familial cancer are currently asked on primary application and personal statement forms for voluntary life insurance (Box 1). There were substantial differences in clinical information required by different insurers. Most forms (20/21) required some degree of information about family history, although the depth of information requested varied. Only two application forms specifically asked whether the applicant had ever had genetic testing.
Industry policy for life insurance and genetic testing has been updated by the Investment and Financial Services Association (IFSA), which is a national, not-for-profit organisation representing the life insurance industry.17,19 Under their code of practice, insurers will not require an individual to undergo a genetic test, but will require results of any genetic testing previously undertaken by that individual.19 Insurers have stated that they will not use information from genetic tests obtained from an applicant to assess another family member’s risk, and that they will provide reasons for adjusting premiums or policy conditions. Importantly, IFSA policy states that, when assessing overall risk, an insurer will take into account the benefits of special medical monitoring, early medical treatment, compliance with treatment and its likelihood of success.
It remains to be determined whether this code of practice will be stringently adhered to and will alter commonly held fears about the potential for misuse of genetic information. So far, there has been one positive sign for insurance applicants considering genetic testing for haemochromatosis.20 An agreement between IFSA and the Murdoch Children’s Research Institute means that premiums will not be raised for individuals homozygous for the common C282Y haemochromatosis mutation, provided they have normal iron levels (with or without treatment) and there is no evidence of organ damage.
Ultimately, third-party use of genetic tests could also fall under the jurisdiction of a proposed Human Genetics Commission of Australia (HGCA). The ALRC has recommended that an HGCA, in consultation with peak industry bodies and regulators, keep a watching brief on developments in the insurance industry in relation to the use of human genetic information.21 In the United Kingdom, a moratorium has been placed on the use of results of genetic tests by insurance companies for policies up to £500 000 for life insurance and £300 000 for critical illness, long-term care and income-protection insurance. Over these limits, genetic testing must be approved by the Genetics and Insurance Committee. To date, only the genetic test for Huntington’s disease has been approved.22
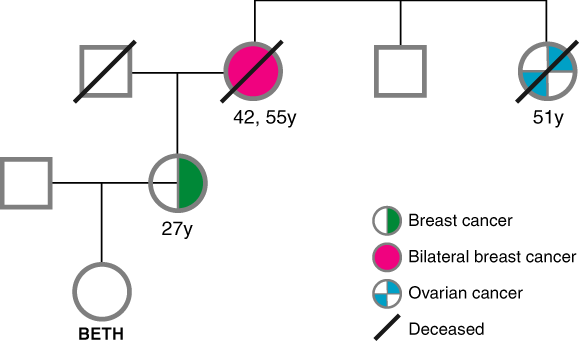
How would our findings on information required by underwriters (Box 1) affect a hypothetical person, whom we will call “Beth”, who has a significant maternal family history of breast and ovarian cancer (Box 2), although she herself has not been affected by cancer?
Beth’s premium may be modified for some insurance contracts on the basis of her immediate family history (regardless of genetic testing issues), which might become evident in 20 of 21 of the insurance applications we examined. Her grandmother’s and great-aunt’s diagnoses would not be evident to those 10 insurers who only required information about first-degree relatives. Parenthetically, if Beth’s mother did not have cancer (or if Beth’s familial cancer risk arose through her father), important information about her cancer risk could be missed by those 10 insurers who only sought information on first-degree relatives. On the other hand, Beth has a duty to disclose any relevant information (that she is aware of),22 and her insurer is entitled to use this information in considering her application. Under the Insurance Contracts Act 1984 (Cwlth),18 duty of disclosure refers to a “matter that a reasonable person in the circumstances could be expected to know”.
Beth’s insurer must in turn be able to justify (with actuarial or other data) how it has used this information.23 However, as mentioned above, there are few genetic conditions in which the result of a genetic test would have sufficient actuarial relevance to justify an increase in premium.
Beth’s mother has had a genetic test revealing a BRCA1 mutation. Beth can therefore consider predictive testing to determine whether she herself is at increased risk. If she tests “mutation negative”, her risk of breast cancer reverts to population risk. If her test is “mutation positive”, she faces a substantial increase in breast and ovarian cancer risk. However, her clinical outcome could be improved by close surveillance and adoption of risk-reduction strategies. For example, bilateral oophorectomy at age 40 years would reduce her subsequent risk of developing breast cancer by about 50% and her ovarian cancer risk by more than 85%.24,25
If Beth had attended a genetic counselling service and explored the possibility of testing, she would be required to state that she had “attended a doctor” (20 insurers) or “other health professional” (9 insurers). Under IFSA policy, Beth will not be required to undergo genetic testing. However, if she has already undertaken a predictive genetic test, this information would be directly requested in two insurance applications, but expected as a “duty of disclosure” in all applications.
The current IFSA code of conduct states that, even if the insurer is aware of Beth’s mother’s genetic test result, this will not be used to assess another family member’s risk. However, Beth has a duty to disclose to the insurer any information that may be pertinent. Therefore, if Beth is aware that her mother carries a BRCA1 mutation, she must reveal this to the insurer, even if she has not attended counselling or decided to have a genetic test. If Beth does not know her mother’s BRCA1 status, the insurer cannot use this information, even if the insurer has access to it (for example, if Beth’s mother had a policy with the same insurer).
Beth’s situation illustrates a problem that is commonly faced by individuals in families in which a gene mutation has been identified. This is relevant both for people with a family history of cancer as well as other genetic conditions. Individuals contemplating testing may need to consider the implications of their decision for other family members. A decision to be tested made by one family member may affect an insurance application made by another member of the same family.
Health professionals and patients should also be aware that the information required by insurance companies varies greatly. However, specific information requested by insurers is perhaps less pertinent given the universal duty of disclosure that continues until a policy has been issued.
The National Health and Medical Research Council guidelines suggest that:
Before they decide to have a genetic test, individuals should be acquainted through [“pre-test”] genetic counselling with the possible implications for themselves and their blood relatives for insurance and employment of having the test”.26
Resources are available to assist both patients and health professionals in this area.17,27
It is important not to lose sight of the fact that insurance concerns are one of many issues facing individuals considering genetic testing. Patients should also be reminded that these concerns do not extend to health insurance or group life insurance in Australia. Health professionals can also play a critical role in ensuring that these concerns are viewed as part of “the big picture”, particularly when genetic testing could lead to improved clinical management options and better health outcomes.
1: Determining what information about familial cancer and genetic testing is requested in insurance application forms
Methods
A list of 40 registered life insurance companies was obtained from the Australian Prudential Regulation Authority (APRA) website16 and compared with the membership of the Investment and Financial Services Association (IFSA)17 to ascertain the total number of companies offering life and income-protection insurance in Australia. Various insurance companies underwrite each other and use common application forms, but we were able to identify a sample of 21 independent versions of insurance application forms in common use. Primary insurance application forms (comprising the application and a personal statement form) were obtained from insurance companies by a phone request or from the Internet and analysed with respect to various categories of required information. Underwriting practice often follows the primary application, with a request for information from a doctor (with consent).
Results
Information requested in 21 independent primary insurance application forms |
Number of insurers |
||||||||||
Personal history of cancer? |
21 |
||||||||||
First-degree relative with cancer? |
10* |
||||||||||
First- or second-degree relative with cancer? |
4* |
||||||||||
Cancer in extended family? |
6* |
||||||||||
Ever attended a doctor? |
20 |
||||||||||
Ever attended another health professional? |
9 |
||||||||||
Ever attended counselling (any type)? |
3 |
||||||||||
Ever had genetic testing? |
2 |
||||||||||
Genetic testing result in a family member |
0 |
||||||||||
Ever had a blood test? |
13 |
||||||||||
Ever been refused an insurance application? |
18 |
||||||||||
Duty of disclosure |
21 |
||||||||||
* Information about first-degree relatives was required on 10 forms, about both first- and second-degree relatives on another four forms, and about the extended family on another six forms. |
|||||||||||
All application forms required details about a personal history of cancer. Each personal statement also contained a section about the client’s duty of disclosure, which is legislated in the Insurance Contracts Act 1984 (Cwlth).18 This mandates disclosure, before the insurance contract is entered into, of all information that (a) could be relevant to the insurer’s decision to accept the risk, or (b) a reasonable person in the circumstances could be expected to know is relevant.
- Elly L Lynch1
- Rebecca J Doherty2
- Clara L Gaff3
- Finlay A Macrae4
- Geoffrey J Lindeman5
- Familial Cancer Centre, Royal Melbourne Hospital, Parkville, VIC.
We thank Mr David Mico from IFSA for helpful advice, Dr Mac Gardner for comments, and the referees for constructive recommendations for the manuscript. The Royal Melbourne Hospital Familial Cancer Centre is supported by the Victorian Family Cancer Genetics Service, established by Department of Human Services, Victoria.
None identified.
- 1. Lynch HT, Boman BM, Lynch JF. Familial predisposition to malignancy. In: Schein PS, editor. Medical oncology. 2nd ed. New York: McGraw-Hill, 1993: 121-142.
- 2. Genetic services (hospitals supplying genetic testing and counselling and their contact numbers). Available at: www.nbcc.org.au/pages/info/risk/genserv.htm (accessed Sep 2003).
- 3. Lerman C, Hughes C, Lemon SJ, et al. What you don't know can hurt you: adverse psychologic effects in members of BRCA1-linked and BRCA2-linked families who decline genetic testing. J Clin Oncol 1998; 16: 1650-1654.
- 4. Butow PN, Lobb EA, Meiser B, et al. Psychological outcomes and risk perception after genetic testing and counselling in breast cancer: a systematic review. Med J Aust 2003; 178: 77-81. <MJA full text>
- 5. Meiser B, Butow PN, Barratt AL, et al. Long-term outcomes of genetic counseling in women at increased risk of developing hereditary breast cancer. Patient Educ Couns 2001; 44: 215-225.
- 6. Sweet M. Genetic testing could create a new underclass. Sydney Morning Herald 1996; 6 Sep: 3.
- 7. Ragg M. Push to keep life insurers' noses out of our genes. Sydney Morning Herald 2000; 7 Aug: 1.
- 8. Farrant D. Beware the genetic ambush. The Age (Melbourne) 2001; 15 Nov: 17.
- 9. Human Genetics Society of Australia (HGSA) policy, March 1999. Predictive genetic testing and insurance. Available at: www.hgsa.com.au/policy/pgti.html (accessed Sep 2003).
- 10. Barlow-Stewart K, Keays D. Genetic discrimination in Australia. J Law Med 2001; 8: 250-262.
- 11. Otlowski MF, Taylor SD, Barlow-Stewart KK. Australian empirical study into genetic discrimination. Genet Med 2002; 4: 392-395.
- 12. Australian Law Reform Commission. Protection of Human Genetic Information. Discussion paper 66. Canberra: Info Access, 2002. Available at: www.austlii.edu.au/au/other/alrc/publications/dp/66/ (accessed Sep 2003).
- 13. Bonn D. Genetic testing and insurance: fears unfounded? Lancet 2000; 355: 1526.
- 14. Nowlan W. Human genetics. A rational view of insurance and genetic discrimination. Science 2002; 297: 195-196.
- 15. National Health Act 1953 (Cwlth). Section 73(2A).
- 16. Australian Prudential Regulation Authority (APRA) website. Available at: www.apra.gov.au (accessed Sep 2003).
- 17. Investment and Financial Services Association. Life insurance and genetic testing in Australia (Fact Sheet, March 2002). Available at: www.ifsa.com.au (accessed Sep 2003). [Click on — Site map, Publications, Fact sheets.]
- 18. Insurance Contracts Act 1984 (Cwlth). Section 21(1).
- 19. Investment and Financial Services Association. Genetic testing policy. January 2002. (IFSA Standard No. 11.00.) Available at: www.ifsa.com.au/ (accessed Sep 2003). [Click on — Site map, Standards and guidance notes.]
- 20. Delatycki M, Allen K, Williamson R. Insurance agreement to facilitate genetic testing [letter]. Lancet 2002; 359: 1433.
- 21. Australian Law Reform Commission. Essentially yours. Protection of human genetic information. ALRC 96. Canberra: ALRC, March 2003. Available at: www.austlii.edu.au/au/other/alrc/publications/reports/96/ (accessed Sep 2003).
- 22. Genetics and Insurance Committee, Department of Health, United Kingdom. Available at: www.doh.gov.uk/genetics/gaic/index.htm (accessed Sep 2003).
- 23. Disability Discrimination Act 1992 (Cwlth). Section 46.
- 24. Kauff ND, Satagopan JM, Robson ME, et al. Risk-reducing salpingo-oophorectomy in women with a BRCA1 or BRCA2 mutation. N Engl J Med 2002; 346: 1609-1615.
- 25. Rebbeck TR, Lynch HT, Neuhausen SL, et al. Prophylactic oophorectomy in carriers of BRCA1 or BRCA2 mutations. N Engl J Med 2002; 346: 1616-1622.
- 26. National Health and Medical Research Council. Familial aspects of cancer: a guide to clinical practice. Clinical practice guidelines. Canberra: NHMRC, November 1999. (Catalogue No. 993839X.) Available at: www.health.gov.au/nhmrc/publications/synopses/cp67syn.htm (accessed Sep 2003).
- 27. The Centre for Genetics Education. Royal North Shore Hospital, Sydney. Genetics information and life insurance products in Australia. Available at: www.genetics.com.au/ (accessed Sep 2003).





Abstract
The potential for discrimination when applying for insurance can be of concern for individuals with a family history of cancer or of a genetic disorder and who are considering genetic counselling or genetic testing. The actual incidence of “genetic discrimination”, however, is not known, despite considerable media coverage of this issue.
The clinical details required by insurers have received less attention. We obtained primary application and personal statement forms used by 21 different underwriters of voluntary life insurance and found substantial differences in the information requested about family history and genetic testing.
All insurance applications, however, contained a duty of disclosure that would require revealing the result, if known by the applicant, of a genetic test in a family member. Therefore, decisions made by family members can affect insurance applications, and people considering genetic testing may also need to consider the implications of the results for other family members.
Health practitioners should balance the potential benefits of appropriate genetic testing against potential restriction to life and income-protection insurance when advising people about genetic testing.