To the Editor: Chronic suppurative otitis media is very common among Australian Aboriginal children, resulting in hearing loss and educational and social disadvantage.1 Reconstructive middle-ear surgery has been part of the accepted treatment for decades. However, there are no publications about long-term outcomes in Aboriginal populations.2 We report here the results of a study of long-term postoperative outcomes in Aboriginal children following reconstructive middle-ear surgery.
We studied all Aboriginal children aged ≤ 15 years who underwent middle-ear surgery for a tympanic membrane perforation (excluding cholesteatoma) in the Kimberley region of Western Australia between 1 October 1986 and 31 December 1995. Data had been collected prospectively during a previous study, and long-term follow-up was undertaken as part of a recent study of middle-ear surgery outcomes.2,3 Ethical approval was obtained from the WA Aboriginal Health Information and Ethics Committee.
The study population consisted of 93 children (57 girls, 36 boys), aged 5–15 years (mean, 10 years; median, 10 years) at the time of operation. Preoperative air–bone gap (ABG) measurements ranged from 8.75 to 58.75 dB (mean, 36.7 dB; median, 36.25 dB). The operations were performed by nine surgeons at three hospitals and included tympanoplasty using temporalis fascia (73%), dura (13%), and other graft materials (8%), and mastoidectomy (6%).
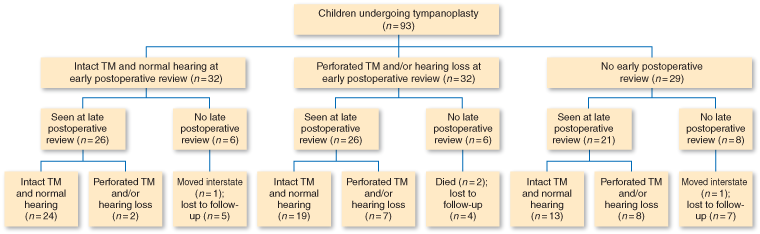
Sixty-four children (69%) underwent early postoperative review (median follow-up interval, 11 months) and 73 children (78%) underwent late postoperative review (median follow-up interval, 103 months). More of the patients had a late review because, at the time, additional resources were available to actively locate the patients for follow-up. At late postoperative review, 56/93 (60%) patients had a successful outcome (intact tympanic membrane and normal hearing) and 17/93 (18%) did not (20/93 [22%] did not undergo late postoperative review).
Of the 32 patients who had a successful outcome at the early postoperative review (median follow-up interval, 5 months), 26 (81%) underwent late postoperative review; 24/26 (92%) still had an intact tympanic membrane and ABG ≤ 25 dB at late postoperative review (median follow-up interval, 109 months) (Box). These findings indicate that successful tympanic membrane closure with hearing improvement after middle-ear surgery in Aboriginal children is probably longlasting.
The major limitation of our study is the absence of clinical information in the time period (mean, 8 years) between the early and late postoperative reviews. An unknown (but likely to be small) number of patients may have had further operations and/or conservative management, which may have influenced their ear health status at late postoperative review. Collection of these data would have been extremely difficult given the nomadic lifestyle of many patients and the logistical realities of remote-area healthcare.
Our findings support the current recommendation of the Office of Aboriginal and Torres Strait Islander Health that Aboriginal children should be offered tympanoplasty if conservative management of chronic suppurative otitis media is unsuccessful.4
- Donna B Mak1
- Alastair MacKendrick2
- Max K Bulsara3
- Sharon Weeks4
- Lewis Leidwinger5
- Harvey Coates6
- Francis J Lannigan6
- Deborah Lehmann
- 1 Kimberley Public Health Unit, Derby, WA
- 2 Nose and Throat Surgeon, Southern Corridor ENT Services, South Fremantle, WA
- 3 Biostatistical Consulting Service, School of Population Health, University of Western Australia, Crawley, WA
- 4 Disability Services Commission, West Perth, WA
- 5 Nose and Throat Surgeon, Department of Otorhinolaryngology – Head and Neck Surgery, Princess Margaret Hospital for Children, Subiaco, WA
- 6 Centre for Child Health Research, University of Western Australia, Telethon Institute for Child Health Research, Subiaco, WA. Correspondence: Dr Donna B Mak, 189 Royal Street, East Perth, WA 6000.
- 1. Morris PS. A systematic review of clinical research addressing the prevalence, aetiology, diagnosis, prognosis and therapy of otitis media in Australian Aboriginal children. J Paediatr Child Health 1998; 24: 487-497.
- 2. MacKendrick A. Ear surgery in Australian Aboriginal children – is it indicated and when is the best time? Aust J Otolaryngol 1999; 3: 240-242.
- 3. Mak DB, MacKendrick A, Weeks S, Plant AJ. Middle ear disease in remote Aboriginal Australia: a field assessment of surgical outcomes. J Laryngol Otol 2000; 114: 26-32.
- 4. Couzos S, Metcalf S, Murray R. A systematic review of existing evidence and primary care guidelines on the management of otitis media in Aboriginal and Torres Strait Islander populations. Canberra: Office of Aboriginal and Torres Strait Islander Health, 2001.