Effective management of chronic illness requires a close partnership between the patient and all healthcare providers.1 Patients with chronic disease are inevitably personally responsible for their own day-to-day care, and are often the best placed to gauge the severity of their symptoms and the efficacy of any treatment. As a result, they must be active participants in the treatment, and, indeed, must adopt self-management as a life long task.1,2 However, compliance with self-management regimens is often poor.3-5 This is hardly surprising when patients are confronted with such complex instructions as “monitor and track your blood pressure”, “recognise and report any symptoms”, “reduce your stress levels”, “monitor and track your blood sugar” and “take six prescription medications, all at different intervals”.
The problem of compliance, as well as the need to provide effective communication between patients with chronic illness and healthcare professionals to enhance care, highlights the need for the use of appropriate and cost-effective information and communications technology (ICT).6,7
Key application domains for ICT in healthcare delivery include telemedicine,8,9 telehealth (or e-health) and home telecare. Telemedicine, typically defined as “a system of healthcare delivery in which physicians examine patients through the use of telecommunications technology”,10 is very well developed in Australia.11 It may encompass telepsychiatry, teleradiology, telepathology, teledermatology and teleophthalmology. However, its primary function is to provide specialist consultation to distant communities, rather than to provide a tool for self-management of chronic disease. In contrast, telehealth incorporates a broad range of health-related activities, including patient and provider education, and health services administration, as well as patient care. In Australia, HealthConnect is an e-health initiative designed to provide patients with rapid access to general health information, reduce duplication of services, provide greater portability of health records and enhance the quality of information exchange between providers (see Box 1).
Clinical decision support is another important area of application of ICT. It is heavily dependent on ready access to medical knowledge databases, as well as sophisticated search engines, which automatically adapt and learn from the user’s search history. The Clinical Information Access Program (CIAP), which provides information resources to support evidence-based practice at the point of care, is an excellent example of such a service.12 Another example is the Quick Clinical project which is developing an experimental online information retrieval system for use in the clinical setting.13 Quick Clinical is designed around the specific information needs and resource constraints within the clinical context (Box 1).
Recent literature has identified home-based disease-management programs as an evolving and important application of telemedicine.14 Unlike the other applications outlined above, home telecare is a rapidly evolving subspecialty of telemedicine focused on providing care in a home or community setting,15 with the primary role of providing support for the patient rather than the health professional.
Typical applications include the management of chronic heart failure (CHF),16,17 asthma,18 diabetes19 and hypertension.20 These and other applications may be based around videophone systems which allow nurses or doctors to view and talk to the patient while collecting data from equipment that records vital signs.21
As is common for most telemedicine applications, a strong evidence base for cost effectiveness and improved healthcare outcomes is still not available.22 The reason for this is that most reports in the literature deal with short-term pilot projects and do not present either a business case or the potential for sustained viability.
In our review of 175 articles on telecare and telemedicine in chronic disease management, we found only four 22-25 that looked at cost-effectiveness. Reports on clinical outcomes and cost effectiveness of ICT for chronic disease are thus very limited,22-24 with the strongest evidence available for telepsychiatry and teledermatology.23 An attempt to carry out a formal meta-analysis of cost–benefit research considered 38 journal articles in which real costs or cost benefits had been considered, but concluded that their design or methods were inadequate for a formal meta-analysis, and that it was premature for any statements to be made on the cost effectiveness of telemedicine and telecare services.24
Probably the only large-scale study of home telecare that has any statistical validity is that by the Kaiser Permanente health maintenance organisation.25 This study examined the cost of delivering nursing services by means of remote video technology in the home healthcare setting, comparing an intervention group of 102 patients with a control group of 110 patients. Patients in the intervention group received video visits in addition to the standard inperson and telephone visits offered to the control group.
The total mean costs of care were US$1948 in the intervention group and US$2674 in the control group, the difference being mostly attributable to hospitalisation costs. The study concluded that, while patients were very pleased with the video technology, the potential for using video visits for reducing the number of actual caregiver visits was not fully realised.
The benefits of home telecare for managing CHF, however, have been extensively reported and some studies have found significant cost savings. One found an 83% decrease in the admission rate for those with CHF in the third quarter of the year after the intervention, compared with the third quarter of the year before the intervention (P = 0.008).26 Another reported that when a telecare group of patients with CHF was compared with patients receiving usual care, mean CHF-related readmission charges were 86% lower (US$5850 versus US$44 479), with fewer CHF-related emergency department visits (P = 0.034).27
It is thus clear that there is an urgent need to develop a business case for new telemedicine services. This should consider government policy, remuneration and the question of who pays, as well as analysing outcomes from long-term clinical trials evaluating healthcare outcomes and cost benefits.
Although there are now many examples of home telecare services in the literature,28,29 and in the last few years a range of new technologies have become available (see Box 1), we will use as an example a locally developed Home Telecare System which integrates a range of e-health services and advanced ICT applications30 to manage chronic disease at home.
Key design specifications included low relative cost, modularity (pick and choose), simplicity of use, clinically relevant vital-signs monitoring, highly automated scheduling, provision of patient feedback, access to information services and very limited use of wearable devices to promote user compliance. The Home Telecare System is shown in Box 2. It is connected to a home personal computer and includes:
the ability to record electrocardiogram, blood pressure (auscultatory method), spirometry modules, patient weight and temperature; and
a wireless interface to an ambulatory patient-worn device for:
telephone voice connection on emergency button press; and
continuous monitoring of acceleration forces on the body to measure energy expenditure and record falls and stumbles.
In addition to monitoring clinical signs, the Home Telecare System can deliver questionnaire instruments which can be tailored to assess functional health status or a specific condition. The Home Telecare System also provides access to EDU-CATE (a comprehensive library of health education leaflets)31 and easy-to-use links to other validated Internet resources, and allows the patient to maintain a daily log of health service use. All data collection is scheduled by patients’ general practitioners on the basis of the severity of symptoms; data collected are then automatically synchronised and replicated on a central server and immediately available to the doctor for remote viewing from any web browser. This approach is seen as a workable intermediary between a stand-alone program that must be installed on each doctor’s computer, versus full integration into a standardised electronic health record. The latter is not currently possible due to the lack of clear international or Australian standards for such records. Our Web-based approach allows for ubiquitous access to patient data and provides a standard user interface (Web browser) with which most clinicians are familiar.
A clinical trial of the Home Telecare System is described in Box 3 and a clinical case study using the system in Box 4.
The transition from managing acute disease to managing chronic disease requires fundamental changes in healthcare service organisation and delivery, as well as recognition “that the patient with chronic disease is the principal care giver who must carry out the necessary actions continuously, interpret and report their results accurately and join in subsequent decisions”.32 Critical to this comprehensive healthcare strategy are the provision of Web-based health education, better management of demographic data, promotion of and support for self-management in community or home-based settings, and protocol-based regulation of clinical procedures and medications.
From our own studies and the evidence in the literature, it is probable that home telecare, supported by dedicated multidisciplinary care teams, can promote partnerships between the patient and other caregivers, facilitate patient self-management, improve compliance and medications management, and reduce the readmission rate for those with chronic disease.
1: Internet resources

Telehealth (or e-health) initiatives
HealthConnect (www.health.gov.au/healthconnect)
HealthInSite (www.healthinsite.gov.au/)
Clinical decision support
Quick Clinical (www.chi.unsw.edu.au)
New technologies
American TeleCare (www.americantelecare.com)
AMD Telemedicine (www.amdtelemedicine.com)
March Networks (www.marchnetworks.com)
SHL Telemedicine (www.shahal.co.il)
HomMed (www.hommed.com)
3: Clinical trial of the Home Telecare System
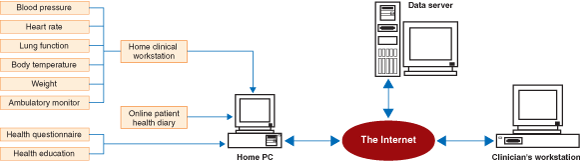
A clinical trial was carried out over at least 3 months in metropolitan Sydney and in Wagga Wagga (a regional centre) with 22 patients aged 58–82 years. All patients had a primary diagnosis of chronic heart failure and/or chronic obstructive pulmonary disease. Some patients were monitored continuously for more than 8 months. The Home Telecare System set up in the patients’ homes is shown in the Figure. All patients, despite having almost no prior computer experience, were able to use the system effectively with less than 1 hour of training. A final report on this trial is available on the internet (www.gpcg.org/publications/docs/projects2001/GPCG_Project4.1_01.pdf). In summary:
|
|||||||||||
A: Spirometer; B: Home clinical workstation; C: Antenna for ambulatory monitoring; D: ECG plate electrodes; E: Blood pressure cuff. |
|||||||||||
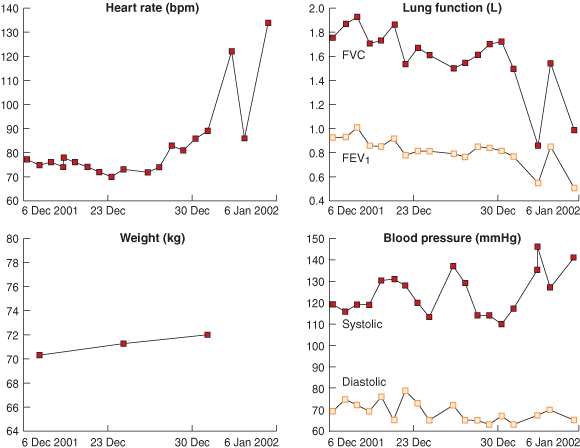
4: Clinical case study involving the Home Telecare System
A 58-year-old woman with smoking- related chronic obstructive pulmonary disease was enrolled into the Home Telecare System trial. She underwent automated monitoring of her lung function, temperature, heart rhythm, weight and blood pressure, and these data were reviewed regularly by her general practitioner. The data subsequently showed the development of sinus tachycardia, decreasing forced expiratory volume in one second (FEV1) and forced vital capacity (FVC), and increased weight (presumably due to fluid retention) (see graphs). The GP contacted the patient and was told that she was acutely short of breath. The GP arranged for her to be admitted directly to hospital, where she was diagnosed with lung infection and mild heart failure. She was discharged after two days of antibiotic and diuretic therapy. | |||||||||||
 |
|||||||||||
- Branko G Celler1
- Nigel H Lovell2
- Jim Basilakis
- Centre for Health Informatics, Biomedical Systems Laboratory, Sydney, NSW.
The Home Telecare System described in this paper is being commercialised by MedCare Systems Pty Ltd [ABN 65 050 042 192] located at the Australian Technology Park, Eveleigh, NSW 1430. B G C and N H L are Directors of the company and J B holds a small shareholding.
- 1. Lorig KR, Bodenheimer T, Holman H, Grumbach K. Patient self-management of chronic disease in primary care. JAMA 2002; 288: 2469-2475.
- 2. Lorig K, Holman H. Self-management education: context, definition, and outcomes and mechanisms. Proceedings of the 1st Chronic Disease Self-Management Conference, Sydney Australia, August 2000. Available at: www.chronicdisease.health.gov.au/pdfs/lorig.pdf (accessed Jul 2003).
- 3. Lorig KR, Sobel DS, Stewart AL, et al. Evidence suggesting that a chronic disease self-management program can improve health status while reducing utilization and costs: a randomized trial. Med Care 1999; 37: 5-14.
- 4. Battersby M, Reece M, Collins J, et al. Chronic disease self-management education — an Australian experience. Proceedings of the 1st Chronic Disease Self-Management Conference, Sydney, Australia, August 2000. Available at: www.chronicdisease.health.gov.au/pdfs/battersby.pdf (accessed Jul 2003).
- 5. Lorig KR, Ritter P, Stewart AL, et al. Chronic disease self-management program — 2 year health status and health care utilisation outcomes. Med Care 2001; 39: 1217-1223.
- 6. Lovell NH, Celler BG. Information technology in primary health care. Int J Med Inf 1999; 55: 9-22.
- 7. Celler BG, Lovell NH, Chan DK. The potential impact of home telecare on clinical practice. Med J Aust 1999; 171: 518-521. <MJA full text>
- 8. Loane M, Wootton R. A review of guidelines and standards for telemedicine. J Telemed Telecare 2002; 8: 63-71.
- 9. Bashur RL, Reardon TG, Shannon GW. Telemedicine: a new healthcare delivery system. Annu Rev Public Health 2000; 21: 613-637.
- 10. Preston J, Brown FW, Hartley B. Using telemedicine to improve healthcare in distant areas. Hosp Community Psychiatry 1992; 43: 25-32.
- 11. Mitchell J. The telemedicine industry in Australia: from fragmentation to integration. Canberra: Department of Industry, Science and Tourism, 1998.
- 12. Ayers D, Wensley M. The Clinical Information Access Project. Med J Aust 1999; 171: 544-546.
- 13. Walther M, Nguyen K, Garsden H, et al. Architecture for an on-line and just-in-time decision-support for general practice. Melbourne: Health Insurance Commission, 2002. Available at: www.chi.unsw.edu.au/Publications/Documents/Clinical%20Decision%20Support/HIC2002%20QC.pdf (accessed Jul 2003).
- 14. Field MJ, Grigsby J. Telemedicine and remote patient monitoring. JAMA 2002; 288: 423-425.
- 15. Kinsella A. Home telecare in the United States. J Telemed Telecare 1998; 4: 195-200.
- 16. Kinsella A, Warner I. Telehealth and managing congestive heart failure. Caring 1998; 17: 14-18.
- 17. De Lusignan S, Wells S, Johnson P, et al. Compliance and effectiveness of 1 year’s home telemonitoring. The report of a pilot study of patients with chronic heart failure. Eur J Heart Fail 2001; 3: 723-730.
- 18. Steel S, Lock S, Johnson N, et al. A feasibility study of remote monitoring of asthmatic patients. J Telemed Telecare 2002; 8: 290-296.
- 19. Tsang MW, Mok M, Kam G, et al. Improvement in diabetes control with a monitoring system based on a hand-held, touch-screen electronic diary. J Telemed Telecare 2001; 7: 47-50.
- 20. Bondmass M, Bolger N, Castro G, Avitall B. The effect of home monitoring and telemanagement on blood pressure control among African Americans. Telemed J 2000; 6: 15-23.
- 21. Rooney E, Studenski S, Roman L. A model for nurse case-managed home care using televideo. J Am Geriatr Soc 1997; 45: 1523-1528.
- 22. Roine R, Ohinmaa A, Hailey D. Assessing telemedicine: a systematic review of the literature. CMAJ 2001; 165: 765-771.
- 23. Hersh W, Helfand M, Wallace J, et al. A systematic review of the efficacy of telemedicine for making diagnostic and management decisions. J Telemed Telecare 2002; 8: 197-209.
- 24. Whitten P, Kingsley C, Grigsby J. Results of a meta-analysis of cost-benefits research: is this a question worth asking? J Telemed Telecare 2000; 6 (Suppl 1): S4-S6.
- 25. Johnston B, Wheeler L, Deuser J. Outcomes of the Kaiser Permanente Tele-Home Health Research Project. Arch Fam Med 2000; 9: 40-45.
- 26. Roglieri JL, Futterman R, McDonough KL, et al. Disease management interventions to improve outcomes in congestive heart failure. Am J Manag Care 1997; 3: 1831-1839.
- 27. Jerant AF, Azari R, Nesbitt TS. Reducing the cost of frequent hospital admissions for congestive heart failure. Med Care 2001; 39: 1234-1245.
- 28. Gilbert JA. Disease management hits home. Health Data Manag 1998; 6: 54-60.
- 29. Hooper GS, Yellowlees P, Marwick TH, et al. Telehealth and the diagnosis and management of cardiac disease. J Telemed Telecare 2001; 7: 249-256.
- 30. Lovell NH, Magrabi F, Celler BG, et al. Methodologies for web-based acquisition, storage and retrieval of biomedical signals. IEEE Eng Med Biol Mag 2001; 20: 38-44.
- 31. Panasetis P, Harris M, Lovell NH, et al. EDU-CATE (Computer Access To Education). The computerised patient education leaflets project. Health Informatics 1998; 7: 154-158.
- 32. Holman H, Lorig K. Patients as partners in managing chronic disease: partnership is a prerequisite for effective and efficient health care. BMJ 2000; 320: 526-527.






Abstract
Information and communications technology (ICT) is increasingly being used in management of chronic illness to facilitate shared services (virtual health networks and electronic health records), knowledge management (care rules and protocols, scheduling, information directories), as well as consumer-based health education and evidence-based clinical protocols.
Common applications of ICT include home monitoring of vital signs for patients with chronic disease, as well as replacing home visits by nurses in person with telemedicine videophone consultations.
A patient-managed Home Telecare System with integrated clinical signs monitoring, automated scheduling and medication reminders, as well as access to health education and daily logs, is presented as an example of ICT use for chronic disease self-management.
A clinical case study demonstrates how early identification of adverse trends in clinical signs recorded in the home can either avoid hospital readmission or reduce the length of hospital stay.