Redback spiders, Latrodectus hasselti, are widow spiders,1 arguably the most medically significant spiders in the world, and certainly in Australia.2-5 Two major issues relating to redback spider bite remain unresolved. The first is the proportion of bites causing severe effects, and the second is the indications for antivenom and its route of administration.6 Many doctors in Australia believe that most redback spider bites (80%) cause minor effects,7,8 and, although a safe and effective intramuscular antivenom exists, doctors are reluctant to use it unless there is severe or systemic envenomation.9,10 Severe pain is often not regarded as an indication for administering the antivenom.
Redback spider antivenom is usually given intramuscularly, which remains the recommendation of CSL Ltd.11 However, redback spider antivenom was introduced without controlled studies to demonstrate efficacy or safety. Its introduction was based on a retrospective collection of 167 cases reported by Australian doctors suggesting it was effective.12
Here we report an analysis of the subset of bites by L. hasselti from a larger prospective cohort of 750 spider bites in Australia4 to better describe the clinical features, proportion of severe cases, and outcomes of redback spider bite. We also address two further issues: the effect of intramuscular antivenom in a smaller cohort of patients presenting to hospital and the diagnostic utility of early features of bites by L. hasselti which distinguish them from other spider bites.
Subjects were recruited prospectively over 39 months from 1 February 1999 to 30 April 2002. Most were a subgroup of a large, prospective study of all spider bites in Australia, conducted from 1 February 1999 to 30 April 2001.4 In the following 12 months, the same methodology was used, but only including redback spiders (this study), white-tail spiders,13 and mygalomorph spiders (unpublished).
Patients were recruited from Royal Prince Alfred Hospital and Royal Darwin Hospital emergency departments and from calls to New South Wales, Queensland and Western Australia poisons information centres. Cases were only included if a definite history of spider bite was obtained and the spider was collected at the time of the bite. All patients were seen or contacted within 24 hours of the bite, and then followed up by telephone after 1 week or until the clinical features resolved. Verbal and written consent for the study was obtained from all patients.
Spiders were either collected directly from the patient or mailed to the authors. Spiders were identified (species, sex and maturity) by an expert arachnologist (M G).
The utility of the initial features of L. hasselti bite (circumstances and early clinical features), versus all other spider bites (obtained from the large prospective study for comparison4), to predict whether the spider was L. hasselti was tested using the final taxonomic identification as a gold standard. The initial features we investigated were the person's activity at the time of the bite (dressing, putting on shoes) and the initial clinical effects ("increasing pain", local diaphoresis, severe pain, radiating pain).
For descriptive statistics, median and interquartile ranges (IQR) were used for data not normally distributed. Fischer's exact test was used for comparison of proportions and the Mann–Whitney test for comparing medians. Confidence intervals were calculated using StatMate.14 All statistical analysis was done using GraphPad Instat15 except for the treatment analysis, for which exact methods in StatXact16 were used for the small numbers.
Sixty-eight definite bites by redback spiders were recorded during the 39 months (27 male and 41 female subjects; age range, 5–83 years; median age, 35 years [IQR, 28–47 years]). Redback spider bites occurred across Australia (Box 1). Most bites occurred in the warmer months between December and April, and 90% occurred between 0800 and 2400 hours.
Bites occurred to all parts of the body. The median duration of all effects was 48 hours (IQR, 24–96 hours). Pain occurred in all bites and was severe in 42 (62%) (Box 2). The median duration of pain was 36 hours (IQR, 11–48 hours). Systemic effects occurred in 35% of redback spider bites (Box 2). The median duration of systemic effects was 1 day (IQR, 1–2 days).
Sixty-six bites were by female spiders (adult and juvenile), one was by an adult male spider and one by a juvenile (subadult) male spider. There was no significant difference between the effects of bites by juvenile and adult females. The adult male caused short-lived, mild pain only. The subadult male caused severe pain for 12 hours, but no systemic effects.
Of the 28 hospitalised patients, two received a combination of intravenous and intramuscular antivenom, two received intramuscular antivenom after 6 hours (16 hours and 24 hours), and six received intramuscular antivenom within 6 hours. The pain had resolved before presentation in one of the 18 patients not receiving antivenom; this patient was excluded from the analysis of antivenom effectiveness.
The six patients treated with intramuscular antivenom within 6 hours were compared with 17 patients not receiving antivenom. Baseline characteristics for these two groups were similar (Box 3). One of six treated patients (17%) had no pain at 24 hours, compared with two of 17 untreated patients (12%), which was not significantly different (+5%; 95% CI, –36% to +64%; P = 0.95) (Box 3). In all 12 patients with systemic effects, these lasted for 24 hours or longer.
Three of the six treated patients received repeated doses of antivenom. One patient who received six ampoules of antivenom had mild serum sickness with malaise, myalgia, rash and pruritus, which resolved over 5 days, and another developed a localised itchy rash after receiving two ampoules of antivenom. These were the only adverse reactions to antivenom, including the four patients not included in this analysis.
Currently, it is believed that many redback spider bites cause minor effects and require neither treatment nor hospital assessment.7,8 Although redback spider antivenom is believed to be effective, doctors are reluctant to use it unless there is severe systemic envenomation.
Two studies of hospitalised patients, involving 150 adults and 156 children with definite redback spider bites, demonstrated that 29% and 22%, respectively, had systemic envenomation; 21% of subjects in both studies received antivenom.10,17 In a small prospective study of nine patients with redback spider bites, more than half had severe effects, and eight received antivenom.18 These three studies, based on emergency department presentations, suffer from sample bias, and patients were not followed up. The largest study, of 2144 cases,19 consisted of reports to the antivenom manufacturer, and did not define the true spectrum of definite redback spider bite.
Our study shows that, when only definite cases are included, a much higher proportion of redback spider bites causes severe and ongoing effects than previously reported.10,17 Two-thirds of patients had pain persisting beyond 24 hours and, in 32%, pain was severe enough to prevent sleep in the first 24 hours. Thirty-five per cent of patients had systemic effects, similar to the proportion in previous studies, but our study showed that these lasted 1–2 days (earlier studies had not examined duration of systemic effects). Our study demonstrates that the severity of envenomation is related not only to the severity of pain and systemic features, but also to the duration of these effects.
Recently, the intramuscular use of redback spider antivenom has been questioned. One series of four patients demonstrated that intramuscular antivenom was ineffective, but intravenous antivenom administered after failure of intramuscular antivenom was effective.6 In our study, intramuscular antivenom was no better than no treatment when all patients were followed up over a week.
Because of the small number of patients in our cohort, the study lacked power to definitively demonstrate no difference between intramuscular antivenom and no treatment. However, we believe that an acceptable treatment effect would be that 80%–90% of patients are pain-free at 24 hours. We found that this is not occurring, with 17% (95% CI, 0–64%) pain-free at 24 hours. This is a poor treatment effect for any antivenom, as they usually have dramatic effects. There are considerable implications of this finding, and the use of intramuscular antivenom9 needs review. A randomised controlled trial of intravenous versus intramuscular antivenom would now be appropriate.
Previous bite reports have invariably involved female redback spiders, and it was widely believed that male spiders are too small to bite and envenom humans.8,9 This article includes the first report of bites by male redback spiders, one causing severe pain. Our study confirms that bites by male spiders are rare compared with bites by females. This is probably due to the small size of males (3–4 mm body length, indicative of smaller jaws, compared with females, measuring up to 14 mm), rather than the male spider being incapable of delivering an effective bite or lacking venom of similar potency to females.
Our study has some limitations, including whether the sample truly represents all patients with redback spider bites. However, there was clear case definition with expert identification of spiders, and the prospective nature and follow-up of all patients were superior to previous studies. Bites were included from poisons information centre calls and from emergency department presentations. As these populations may differ, it is important to include both. Spider bites for which the patient did not seek any medical attention were not included, and this may have biased the study to more severe bites.
Our study demonstrates that, in many patients, early referral to hospital for assessment of severe pain is appropriate. We believe antivenom should be administered in most cases for pain relief alone, although the smaller cohort analysis challenges the current practice of using intramuscular antivenom, which is based on anecdotal experience. Controlled trials are required to compare the efficacy and safety of intramuscular and intravenous antivenom, because it may be more appropriate to use the latter. It will be a challenge, particularly for primary care physicians and poisons information centre specialists, in identifying cases of redback spider bite and in determining which patients should be advised to seek further treatment. However, we have demonstrated that early features of bites can be used to assess whether the spider is a redback (Box 4).
1: Geographical distribution of redback spider bites
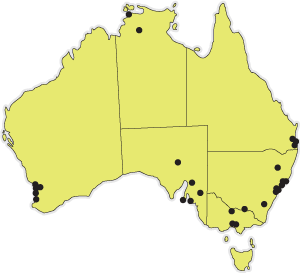
The map includes only the 56 cases collected in the study of all spider bites between 1 February 1999 and 30 April 2001.4 The 12 cases collected later are not included because the recruitment site differed, so the first 56 bites provide a more accurate geographical representation.
2: Clinical effects and circumstances of 68 redback spider bites
Features of bites |
No. |
Percentage (95% CI) |
|||||||||
Pain |
|||||||||||
Severe pain |
42 |
62% (49%–73%) |
|||||||||
Pain > 24 hours |
45 |
66% (54%–77%) |
|||||||||
Severe pain > 24 hours |
38 |
56% (43%–68%) |
|||||||||
Unable to sleep for first 24 hours |
22 |
32% (22%–45%) |
|||||||||
Increasing pain in first hour |
37 |
54% (42%–67%) |
|||||||||
Radiating pain (proximal limb) |
26 (20) |
38% (27%–51%) |
|||||||||
Abdominal/chest pain* |
8 |
12% (5%–22%) |
|||||||||
Other local/regional effects |
|||||||||||
Local or regional diaphoresis |
23 |
34% (23%–46%) |
|||||||||
Redness/red area |
50 |
74% (61%–83%) |
|||||||||
Swelling |
5 |
7% (2%–16%) |
|||||||||
Puncture marks |
4 |
6% (2%–14%) |
|||||||||
Systemic effects† |
24 |
35% (24%–48%) |
|||||||||
Nausea |
16 |
24% (14%–35%) |
|||||||||
Vomiting |
3 |
4% (1%–12%) |
|||||||||
Headache |
7 |
10% (4%–20%) |
|||||||||
Malaise |
7 |
10% (4%–20%) |
|||||||||
Lethargy |
7 |
10% (4%–20%) |
|||||||||
Generalised diaphoresis |
3 |
4% (1%–12%) |
|||||||||
Bite site |
|||||||||||
Distal extremity |
31 |
46% (33%–58%) |
|||||||||
Proximal limb |
18 |
26% (17%–39%) |
|||||||||
Trunk |
14 |
21% (12%–32%) |
|||||||||
Head/neck |
5 |
7% (2%–16%) |
|||||||||
Circumstances of bite |
|||||||||||
Putting on shoe |
19 |
28% (18%–40%) |
|||||||||
Dressing |
7 |
10% (4%–20%) |
|||||||||
* Includes pain radiating to groin/abdomen and chest/breast. † Less common systemic effects included anorexia, dizziness, generalised myalgia and hypertension. |
|||||||||||
3: Characteristics of hospital patients who were and were not treated with intramuscular antivenom, and comparison with non-hospital patients
Characteristics |
Hospital patients |
Non-hospital patients (n = 40) |
|||||||||
Not treated with antivenom (n = 17) |
Treated with antivenom (n = 6) |
||||||||||
Number |
% (95% CI) |
Number |
% (95% CI) |
Number |
% (95% CI) |
||||||
Males |
6 |
35% |
1 |
17% |
17 |
43% |
|||||
Median (IQR) age (years) |
34 |
41 |
39 |
||||||||
Distal bite region |
9 |
53% |
2 |
33% |
16 |
40% |
|||||
Severe pain |
12 |
71% |
5 |
83% |
21 |
53% |
|||||
Initial systemic features |
8 |
47% |
4 |
67% |
9 |
23% |
|||||
Median (IQR) pain duration (hours) |
48 |
48 |
24 |
||||||||
Unable to sleep because of pain |
7 |
41% |
2 |
33% |
10 |
25% |
|||||
No pain at 24 hours |
2 |
12% |
1 |
17% |
18 |
45% |
|||||
Systemic effects > 24 hours |
8 |
47% |
4 |
67% |
9 |
23% |
|||||
4: Diagnostic utility of circumstances and early clinical effects of spider bites in differentiating bites by redback spiders, L. hasselti (68 cases), from all other types of biting spiders in Australia*
Diagnostic feature |
Sensitivity (95% CI) |
Specificity (95% CI) |
Positive predictive value (95% CI) |
Negative predictive value (95% CI) |
LR |
P |
|||||
Circumstances |
|
|
|
|
|
|
|||||
Dressing |
— |
— |
— |
— |
— |
0.291 |
|||||
Putting on shoes |
28% |
95% |
0.35 |
0.93 |
5.4 |
< 0.0001 |
|||||
Early clinical effects |
|
|
|
|
|
|
|||||
"Increasing pain" over first hour |
54% |
98% |
0.74 |
0.96 |
29 |
< 0.0001 |
|||||
Diaphoresis (local or regional) |
34% |
99.7% |
0.92 |
0.94 |
117 |
< 0.0001 |
|||||
Pain radiating |
38% |
96% |
0.46 |
0.94 |
8.8 |
< 0.0001 |
|||||
Severe pain |
62% |
75% |
0.20 |
0.95 |
2.5 |
< 0.0001 |
|||||
* Included from a previous study (694 cases).4 LR = Likelihood ratio. |
|||||||||||
- Geoffrey K Isbister1
- Michael R Gray2
- 1 Discipline of Clinical Pharmacology, University of Newcastle, Waratah, NSW.
- 2 Division of Invertebrate Zoology, Australian Museum, Sydney, NSW.
We would like to acknowledge the large number of people who have made this study possible, including the poison information specialists from the NSW, WA and QLD poison information centres, and the nursing staff and doctors in many emergency departments around Australia who have assisted in recruiting cases via the poisons information centres. Particular thanks to a number of clinicians who have made it possible to organise the study or given advice regarding the design of the study, including Bart Currie. Thanks to David Henry, Ian Whyte, Nick Buckley, Bart Currie and Patricia McGettigan for comments on the methodology and David Sibbritt for review of the statistical analysis. Thanks to Tony Smith for commenting on the manuscript.
None identified.
- 1. Bettini S, Maroli M. Venoms of Theridiidae, Genus Latrodectus. In: Bettini S, editor. Arthropod venoms. Berlin: Springer-Verlag, 1978; 149-189.
- 2. Stallybrass FC. Spider bites. Lancet 1969; 1: 572.
- 3. Clark RF, Wethern-Kestner S, Vance MV, Gerkin R. Clinical presentation and treatment of black widow spider envenomation: a review of 163 cases. Ann Emerg Med 1992; 21: 782-787.
- 4. Isbister GK, Gray MR. A prospective study of 750 definite spider bites, with expert spider identification. QJM 2002; 95: 723-731.
- 5. Vetter RS, Visscher PK. Bites and stings of medically important venomous arthropods. Int J Dermatol 1998; 37: 481-496.
- 6. Isbister GK. Failure of intramuscular antivenom in redback spider envenomation. Emerg Med (Fremantle) 2002; 14: 436-439.
- 7. Nicholson GM, Graudins A. Spiders of medical importance in the Asia-Pacific: atracotoxin, latrotoxin and related spider neurotoxins. Clin Exp Pharmacol Physiol 2002; 29: 785-794.
- 8. White J. Envenoming and antivenom use in Australia. Toxicon 1998; 36: 1483-1492.
- 9. White J, Cardoso JL, Hui WF. Clinical toxicology of spider bites. In: Meier J, White J, editors. Handbook of clinical toxicology of animal venoms and poisons. Boca Raton, Fl: CRC Press, 1995; 259-330.
- 10. Jelinek GA, Banham NG, Dunjey SJ. Red-back spider-bites at Fremantle Hospital, 1982–1987. Med J Aust 1989; 150: 693-695.
- 11. White J. CSL antivenom handbook. 2nd edn. Melbourne: CSL Ltd, 2001.
- 12. Wiener S. Redback spider bite in Australia: an analysis of 167 cases. Med J Aust 1961; 2: 44-49.
- 13. Isbister GK, Gray MR. White-tail spider bite: a prospective study of 130 definite bites by Lampona species. Med J Aust 2003; in press.
- 14. GraphPad StatMate [computer program]. Version 1.0. San Diego: GraphPad Software, Inc, 1995.
- 15. GraphPad InStat [computer program]. Version 3.05 San Diego: GraphPad Software, Inc, 2000.
- 16. StatXact [computer program]. Version 4.0. Cambridge, Mass: Cytel Software Corporation, 1998.
- 17. Mead HJ, Jelinek GA. Red-back spider bites to Perth children, 1979–1988. J Paediatr Child Health 1993; 29: 305-308.
- 18. Fisher MM, Bowey CJ. Urban envenomation. Med J Aust 1989; 150: 695-698.
- 19. Sutherland SK, Trinca JC. Survey of 2144 cases of red-back spider bites: Australia and New Zealand, 1963–1976. Med J Aust 1978; 2: 620-623.





Abstract
Objective: To determine the spectrum of severity and early diagnostic predictors of redback spider bites (Latrodectus hasselti ), and to examine the effect of intramuscular redback antivenom.
Design and setting: Prospective cohort study of calls to New South Wales, Queensland and Western Australian poisons information centres and presentations to Royal Prince Alfred Hospital and Royal Darwin Hospital emergency departments.
Patients: 68 people with definite redback spider bites in which the spider was immediately collected and expertly identified (1 February 1999 to 30 April 2002).
Interventions: Intramuscular redback spider antivenom in a smaller cohort of hospitalised patients.
Main outcome measures: Pain severity and duration, local effects and systemic envenomation (effects, prevalence, and persistence > 24 hours).
Results: The median duration of effects was 48 hours (interquartile range, 24–96 hours). Pain occurred after all bites and was severe in 42 (62%). Forty-five patients (66%) had pain lasting longer than 24 hours, and 22 (32%) were unable to sleep because of pain. Systemic effects occurred in 24 (35%). Increasing pain over one hour occurred in 37 cases (54%), and local/regional diaphoresis in 23 (34%); both these features were highly predictive of L. hasselti bites compared with bites of other spiders. One of six patients treated with intramuscular antivenom (17%) had no pain at 24 hours, compared with two of 17 untreated patients (12%) (difference, 5%; 95% CI, –36% to +64%; P = 0.95). There was no difference in duration of systemic effects with antivenom administration.
Conclusions: Most redback spider bites cause severe and persistent effects. Intramuscular antivenom appears to be less effective than previously thought and its use by this route needs review.