Chronic pain is a common problem. Its prevalence, association with markers of social disadvantage and impact on working-age populations make it a significant public health problem in Australia.1 There is a growing emphasis on developing management strategies for chronic illnesses such as chronic pain.2 However, there are few Australian data on the prevalence of chronic pain and its impact on individuals and health services.3
Our study aimed to determine the clinical features, antecedents and impact of chronic pain in a population sample. Impact was defined to include pain-related disability and use of health services and analgesic medications.
The study was a telephone survey of randomly selected households in the Northern Sydney Health Area of Sydney, New South Wales, between July and September 1998. It was approved by the Northern Sydney Area Human Research Ethics Committee.
A sampling frame of residential telephone numbers was constructed by identifying telephone number prefixes for eligible exchanges, then randomly generating the remaining digits by computer.4 The Northern Sydney Health Area had a base population of about 760 000 in 1998, with a preponderance of females and people aged 65 years and over when compared with the population of NSW as a whole.5 The Health Area also has a higher proportion of people who are Australian-born or from an English-speaking background. Residents also report a higher level of education, professional employment and socioeconomic status than NSW generally.5
A respondent was randomly selected from eligible members of each household (English-speaking residents aged 18 years and over).
The questionnaire was delivered as a computer-assisted telephone interview (CATI), which allowed random selection of a respondent from each household, minimised variation between interviewers and reduced errors in question sequences and recording of data. The questionnaire comprised 50 items and was piloted with 78 people.
Chronic pain was defined as pain experienced every day for 3 months in the 6 months before interview.6 Pain severity was classified on the Chronic Pain Grade according to scores on three items about pain intensity and four about pain-related disability (Box 1).7 Respondents' self-reported doctor diagnoses were classified into categories from the International classification of diseases and related disorders (ICD-10).8
Respondents were asked whether they had sought help for their pain in the previous 6 months from three categories of healthcare practitioners — doctors, allied health professionals and alternative practitioners — and how many visits they had made to the practitioner they had seen most often for their pain problem in each of the three categories.
They were also asked about use of analgesic medications currently and in the previous 6 months, including those used intermittently and injected medications. Respondents could nominate up to four analgesic medications. Drugs were initially classified using MIMS.9
A post-stratification weight was used to adjust all percentages for the differences between the age and sex profile of the survey population and the estimated resident population of the Northern Sydney Health Area,5 as well as for household size. Trends in proportions by chronic pain grade were tested using the χ2 test for trend.
Interviews were completed by 2092 people (1169 women and 923 men; response rate, 73.4%). Their age and sex profiles were similar to those of the population of the Northern Sydney Health Area as a whole.5
Characteristics of chronic pain are shown in Box 1. High levels of pain-related disability (chronic pain grades III and IV) occurred in 27% of the 439 respondents with data available. Duration of pain was more than 1 year in 72% and more than 10 years in 21%.
Pain was most commonly in the back (45% of those with chronic pain), followed by the leg (42%), shoulder (29%), arm (22%) and neck (20%), with some respondents having pain in multiple sites.
Injury was the leading cause of chronic pain, followed by a health problem (Box 1). The most common type of injury was sports injury (13% of people with chronic pain), which was particularly common in men with chronic pain (21%). Work-related accidents and conditions were the nominated cause in 14% of people.
Thirty-five per cent of those with chronic pain reported having a diagnosed cause from a doctor, most commonly arthritis (48/474; 9%). When reported diagnoses were classified according to ICD-10 categories, diseases of the musculoskeletal system and connective tissues (M00–M99) were most common (127/474; 26%).
Of the 474 people with chronic pain, 374 (78%) had consulted a healthcare practitioner in the previous 6 months about their pain (Box 2). Medical practitioners were most likely to have been consulted (by 60% of people with chronic pain) compared with allied health practitioners (50%) and alternative practitioners (21%).
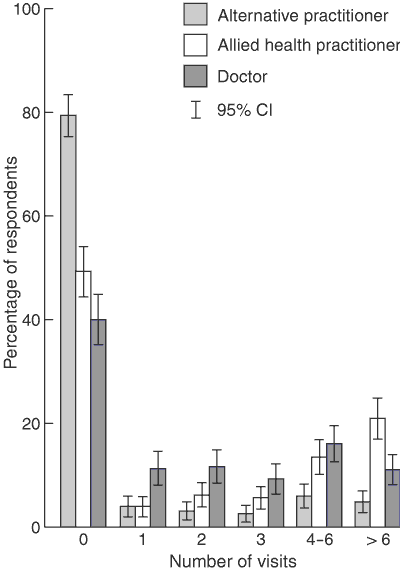
Multiple visits (more than three) were more commonly reported for allied health professionals (35%) than for medical practitioners (28%) or alternative practitioners (11%) (Box 3).
A third of people reported having imaging studies in the previous 6 months, most often x-ray (29%), followed by computed tomography (8%) (Box 2).
Analgesic medications were used by 343 people with chronic pain (71%), with oral medications used by 339 (70%) and injected medications by 48 (10%) (Box 4). Non-steroidal anti-inflammatory drugs and paracetamol were the most commonly used medications. Sixty-two of the 339 who used oral medications (19%) reported using three or more. Use of oral medications was mostly long term (six months or more) (73% of those who used oral medications) and on an intermittent basis (53%).
This study confirmed that chronic pain is a common problem, and often follows injury, either from sport or at work. Chronic pain is associated with substantial disability, frequent use of health services, and high levels of use of analgesic medications.
The rigorous sampling methods and the good response rate enhanced representativeness compared with other telephone-based studies of the prevalence of chronic pain.7,10,11
These findings are cross-sectional and rely on self-reported data from a single geographic area with a particular socio-demographic profile. We have shown previously that chronic pain is strongly associated with markers of social disadvantage.1 Further studies of non-urban or more socioeconomically diverse populations, with objective measures of variables such as health service use, are needed to confirm these findings. As chronic illness can affect many aspects of daily life, our findings do not represent the full impact of chronic pain on individuals and the community.
Injury was an important cause of chronic pain. Because of the Northern Sydney Health Area's demographic profile, the proportion of chronic pain cases caused by injury may be even higher in other areas. Other population studies have identified injury as a common cause of chronic pain.10-12 While injury is recognised as a state and national health priority,13 its importance as a cause of chronic pain in Australia has not previously been identified. This has particular public health significance, as injury, particularly sports injury, affects younger age groups and is amenable to prevention. Strategies focused on primary prevention of injury and secondary prevention of the progression from acute to chronic pain are needed, along with research to identify those most in need of this intervention. Similarly, work was also an important contributor to chronic pain, through injury and other effects.
Health service use was substantial. Similar levels of care-seeking have been seen in other studies,10 and pain has been identified as a frequent reason for GP consultation in Australia.14 In our study, physiotherapists and pharmacists were commonly accessed. However, despite the demonstrated efficacy of multi-disciplinary treatment of chronic pain, very few people with chronic pain had seen psychologists.
There was substantial use of over-the-counter oral analgesic medications, suggesting that self-medication and seeking advice from pharmacists may be important medication strategies in this group. Consequences of use of non-prescription medications can include inappropriate use, demand for particular products promoted by advertising, and problems in provision of unbiased quality information about non-pharmaceutical interventions.15 The role of pharmacists is important in this regard. Polypharmacy with analgesic medications — with its attendant risks16 — was common in this study, and may indeed have been underestimated, as we assessed a maximum of four analgesic medications.
A high proportion of people with chronic pain reported having had radiological or other types of imaging. This is of concern, given the evidence that these investigations are of limited use in diagnosing and managing chronic pain.17 However, the specific reasons for investigations were not elicited in this study.
Given the high prevalence of chronic pain, there is a large population at risk of developing pain-related behaviours of limited usefulness, such as over-reliance on analgesic medication and frequent use of health services.18 The association between pain-related disability and use of health services and analgesic medications underlines this concern. As many individuals access health services for their pain, this is an important intervention point to prevent the onset and maintenance of potentially dysfunctional pain behaviours. However, despite the accumulated evidence on the efficacy of various treatments for chronic pain, healthcare policy on chronic pain has been limited in Australia. For example, there are no national guidelines on management of chronic pain despite the existence of comprehensive acute pain management guidelines.19
In conclusion, this study provides new data about chronic pain in the community. It highlights the importance of understanding the pathways from injury to chronic pain, and of developing timely interventions to prevent progression from acute to chronic pain. The strong relationship between levels of pain-related disability and the use of health services and analgesic medication points to the need for a coordinated approach to managing and minimising pain-related disability. This needs to involve the wide range of healthcare professionals identified in this study (particularly general practitioners), patients with chronic pain, and, where appropriate, specialised multi-disciplinary teams in pain clinic settings.
1: Characteristics and causes of pain among 474 respondents with chronic pain
|
No. of respondents* |
||||||||||
Chronic pain grade† (n =439)‡ |
|
||||||||||
Grade I |
163 (39%) |
||||||||||
Grade II |
147 (35%) |
||||||||||
Grade III |
67 (14%) |
||||||||||
Grade IV |
62 (13%) |
||||||||||
Cause of pain (n = 468) |
|
||||||||||
Injury |
173 (38%) |
||||||||||
Sports injury |
54 (13%) |
||||||||||
Work accident |
20 (4%) |
||||||||||
Car accident |
39 (8%) |
||||||||||
Home accident |
32 (7%) |
||||||||||
Other injury |
28 (6%) |
||||||||||
Health problem |
132 (29%) |
||||||||||
Illness |
55 (11%) |
||||||||||
Work-related (not involving an accident) |
42 (9%) |
||||||||||
Other health problem§ |
35 (8%) |
||||||||||
No clear reason |
163 (32%) |
||||||||||
Don't know |
6 (1%) |
||||||||||
* Percentages are age- and sex-adjusted. † Chronic pain grades: I = low disability–low intensity; II = low disability–high intensity; III = high disability–moderately limiting; and IV = high disability–severely limiting. ‡ Some respondents did not reply to all questions. § Medical intervention (21), stress (4), posture (3), other (7). |
|||||||||||
2: Use of health services for pain in the previous 6 months among 474 people with chronic pain
|
No. of respondents* |
||||||||||
Practitioners consulted |
|
||||||||||
Medical practitioner |
292 (60%) |
||||||||||
General practitioner |
264 (55%) |
||||||||||
Orthopaedic surgeon |
65 (13%) |
||||||||||
Rheumatologist |
31 (6%) |
||||||||||
Anaesthetist |
24 (5%) |
||||||||||
Neurologist |
19 (4%) |
||||||||||
Pain specialist |
16 (3%) |
||||||||||
Other† |
41 (8%) |
||||||||||
Allied health professional |
245 (50%) |
||||||||||
Physiotherapist |
140 (28%) |
||||||||||
Pharmacist |
113 (24%) |
||||||||||
Chiropractor |
57 (12%) |
||||||||||
Acupuncturist |
39 (7%) |
||||||||||
Hydrotherapist |
20 (4%) |
||||||||||
Occupational therapist |
18 (3%) |
||||||||||
Other‡ |
15 (2%) |
||||||||||
Alternative practitioner |
99 (21%) |
||||||||||
Masseur |
73 (16%) |
||||||||||
Naturopath |
28 (6%) |
||||||||||
Osteopath |
19 (4%) |
||||||||||
Herbalist |
13 (3%) |
||||||||||
Other§ |
11 (3%) |
||||||||||
Imaging studies |
157 (33%) |
||||||||||
X-ray |
137 (29%) |
||||||||||
Computed tomography |
39 (8%) |
||||||||||
Bone scan |
21 (4%) |
||||||||||
Magnetic resonance imaging |
14 (2%) |
||||||||||
Scan (type unknown) |
21 (5%) |
||||||||||
* Percentages are age- and sex-adjusted. † Neurosurgeon (11), other physician (11), psychiatrist (10), other surgeon (8), sports physician (1). ‡ Podiatrist (5), social worker (4), psychologist (3), dentist (2), nutritionist (1). § Homeopath (7), yoga therapist (3), unspecified (1). |
|||||||||||
4: Use of medications for pain currently or in previous 6 months among 474 people with chronic pain
|
No. of respondents* |
||||||||||
Oral medications |
339† (70%) |
||||||||||
Paracetamol |
153 (31%) |
||||||||||
NSAIDs |
143 (31%) |
||||||||||
Vitamins, minerals, herbal and natural preparations |
83 (17%) |
||||||||||
Combined simple analgesics‡ |
70 (13%) |
||||||||||
Topical rubifacients |
38 (8%) |
||||||||||
Combined opioid analgesics§ |
35 (8%) |
||||||||||
Anxiolytics, sedatives, antipsychotics |
14 (3%) |
||||||||||
Opioid analgesics |
7 (2%) |
||||||||||
Steroids |
7 (1%) |
||||||||||
Anticonvulsants |
6 (1%) |
||||||||||
Antidepressants |
6 (1%) |
||||||||||
Other |
14 (3%) |
||||||||||
Don't know |
9 (2%) |
||||||||||
Injected medications |
48 (10%) |
||||||||||
Anti-inflammatories |
27 (6%) |
||||||||||
Opioids |
15 (3%) |
||||||||||
Other |
4 (0.6%) |
||||||||||
Don't know |
7 (1%) |
||||||||||
NSAIDs = non-steroidal anti-inflammatory drugs. * Percentages are age- and sex-adjusted. † One person did not answer the question. ‡ Combined simple analgesics = combinations of paracetamol/acetominophen or aspirin plus low doses of codeine (< 30 mg). § Combined opioid analgesics = prescription-only combinations of paracetamol/acetominophen plus dextropropoxyphene or higher doses of codeine (≥ 30 mg). |
|||||||||||
5: Association between chronic pain grade, medication and health service use among 417 respondents with chronic pain*
|
Chronic pain grade |
|
|||||||||
|
Grade I (n = 155) |
Grade II (n = 140) |
Grade III (n = 67) |
Grade IV (n = 55) |
P † |
||||||
Analgesic use |
|
|
|
|
|
||||||
Oral opioid or combination opioid |
10 (7%) |
16 (10%) |
17 (26%) |
21 (39%) |
< 0.001 |
||||||
≥ 2 oral medications |
39 (28%) |
46 (32%) |
32 (45%) |
29 (52%) |
< 0.001 |
||||||
Health service use |
|
|
|
|
|
||||||
GP visit for pain in previous 2 weeks |
6 (4%) |
20 (10%) |
18 (25%) |
20 (38%) |
< 0.001 |
||||||
Services used for pain in previous 6 months |
|
|
|
|
|||||||
≥ 4 doctor visits‡ |
8 (5%) |
22 (13%) |
22 (30%) |
25 (50%) |
< 0.001 |
||||||
≥ 6 other health professional visits‡ |
21 (15%) |
40 (26%) |
31 (42%) |
28 (50%) |
< 0.001 |
||||||
Hospital admission |
5 (2%) |
2 (1%) |
8 (14%) |
19 (41%) |
< 0.001 |
||||||
Radiological investigation |
34 (22%) |
33 (25%) |
34 (52%) |
33 (65%) |
< 0.001 |
||||||
* 417 respondents had complete data available for all variables. † χ2 test for trend. ‡ Upper quartile of visits. |
|||||||||||
Received 9 September 2002, accepted 20 May 2003
- Fiona M Blyth1
- Michael J Cousins2
- Lyn M March3
- 1 University of Sydney Pain Management and Research Centre, Royal North Shore Hospital, NSW.
- 2 University of Sydney Department of Rheumatology, Royal North Shore Hospital, NSW.
We thank Dr Michael Von Korff for helpful suggestions during study planning and the Epidemiology and Surveillance Branch, NSW Health Department for providing the sampling frame and device. This study is part of a series funded by a program grant to the Pain Management and Research Centre as a National Health and Medical Research Council (NHMRC) Centre of Clinical Excellence in Hospital Based Research and by research grants from the Joint Coal Board, Workcover Australia, Northern Sydney Area Health Service and the Centre for Anaesthesia and Pain Management Research. Dr Blyth was funded by an NHMRC postgraduate training scholarship. The funding sources had no role in study design, collection, analysis or interpretation of data or publication.
None identified.
- 1. Blyth FM, March LM, Brnabic AJM, et al. Chronic pain in Australia: a prevalence study. Pain 2001; 89: 127-134.
- 2. Von Korff M, Glasgow RE, Sharpe M. ABC of psychological medicine. Organising care for chronic illness. BMJ 2002; 325: 92-94.
- 3. Helme RD, Gibson SJ. Pain in the elderly. In: Jensen TS, Turner JA, Wiesenfeld-Hallin Z, editors. Proceedings of the 8th World Congress on Pain. Seattle: IASP Press, 1997: 919-944.
- 4. Blyth FM, March LM, Shellard D, Cousins MJ. The experience of using random digit dialling methods in a population-based chronic pain study. Aust N Z J Public Health 2002; 26: 511-514.
- 5. Australian Bureau of Statistics. 1998 estimated resident population [electronic]. Health Outcomes Information Statistical Toolkit (HOIST). Sydney: Epidemiology and Surveillance Branch, NSW Health Department (accessed Feb 2000).
- 6. Classification of chronic pain. Descriptions of chronic pain syndromes and definitions of pain terms. Prepared by the International Association for the Study of Pain, Subcommittee on Taxonomy. Pain 1986; Suppl 3: S1-S226.
- 7. Von Korff M, Ormel J, Keefe F, Dworkin SF. Grading the severity of chronic pain. Pain 1992; 50: 133-149.
- 8. World Health Organization. International classification of diseases and related disorders (ICD-10). Geneva: World Health Organization, 1992.
- 9. MIMS online [computer file]. Version 1.1. Sydney: HCN (Vendor); 1 May 1999–31 July 1999 edition. Available at: www.ciap.health.nsw.gov.au (accessed May 1999).
- 10. Crook J, Rideout E, Browne G. The prevalence of pain complaints in a general population. Pain 1984; 18: 299-314.
- 11. Bowsher D, Rigge M, Sopp L. Prevalence of chronic pain in the British population: a telephone survey of 1037 households. Pain Clin 1991; 4: 223-230.
- 12. Birse TM, Lander J. Prevalence of chronic pain. Can J Public Health 1998; 89: 129-131.
- 13. Australian Bureau of Statistics. National health survey: injuries. Canberra: ABS, 1995. (Catalogue no. 4384.0.)
- 14. Britt H, Sayer G, Miller GC, et al. General practice activity in Australia 1998-1999. General Practice Series No. 2. Canberra: Australian Institute of Health and Welfare, 1999.
- 15. Bessell TL, Hiller JE, Sansom LN. "Pharmacist only" medicines. Aust N Z J Public Health 1999; 23: 661-662.
- 16. Kung F, Gibson SJ, Helme RD. Factors associated with analgesic and psychotropic medications use by community-dwelling older people with chronic pain. Aust N Z J Public Health 1999; 23: 471-474.
- 17. Loeser JD. Mitigating the dangers of pursuing cure. In: Cohen MJM, Campbell JN, editors. Pain treatment centres at a crossroads: a practical and conceptual reappraisal, progress in pain research and management. Vol 7. Seattle: IASP Press, 1996: 101-108.
- 18. Von Korff M, Dworkin SF, Le Resche L, Kruger A. An epidemiologic comparison of pain complaints. Pain 1988; 32: 173-183.
- 19. National Health and Medical Research Council. Acute pain management: information for general practitioners. Canberra: Commonwealth of Australia, 1999.





Abstract
Objectives: To describe the clinical features, antecedents and impact of chronic pain.
Design: Telephone survey of randomly selected household respondents.
Setting: Northern Sydney Health Area, metropolitan Sydney, July to September 1998.
Participants: 2092 English-speaking residents aged 18 years or over.
Main outcome measures: Age- and sex-adjusted prevalence of chronic pain (pain experienced every day for 3 months in the previous 6 months), pain-related disability, and use of health services and analgesic medications.
Results: Chronic pain affected 474/2092 respondents (22.1%; 95% CI, 20.2%–24.0%), with high levels of pain-related disability in 129/439 (27%). Nominated causes of chronic pain were injury in 173 (38%), most commonly sports injury (54; 13%), and a health problem in 132 (29%). Pain was work-related in 62 (14%). A musculoskeletal condition was the leading diagnosis (127; 26%). Of the 474 with chronic pain, 374 (78%) had consulted at least one health practitioner for pain in the previous 6 months, comprising medical practitioners (consulted by 292 [60%] and including general practitioners [55%]), allied health professionals (245; 50%), and alternative practitioners (99; 21%). Current or recent use of oral analgesic medications (often over-the-counter preparations) was common (339; 70%). Higher levels of pain-related disability were associated with greater use of medications and health services.
Conclusions: Our study shows that chronic pain is common and often results from injury. It highlights the importance of timely interventions to prevent progression from acute to chronic pain and the need for a coordinated approach to managing pain-related disability.