General practice is in crisis. It has a poor status within the profession,1 and general practitioners earn less than other medical practitioners2,3 — even for the same services, they command poorer fees than specialists in Australia.4 Their traditional place is outside the healthcare system (still dominated by hospitals), exerting considerably less influence from the "corner shops" of their private practices. The number of GP registrar applicants is little above the imposed restriction, and is falling (Box 1). Only 392 Australian-trained doctors (about a quarter of the cohort of junior doctors) applied for a GP registrar position for 2003. An additional 35% of applicants were overseas-trained, while only 31% were Australian-born (R Coote, General Practice Education and Training Ltd, Canberra, personal communication, May 2003). The picture is similar overseas.3
The perceived poor state of intellectual activity in general practice is more profound. GPs publish less research than specialists5 — vastly less in relation to their practising numbers.6 GP journals have lower (if slowly rising) citation indices. Compared with general practice overseas, we seem to be always catching up (Box 2).
More important, our patients are losing confidence in their GPs' ability to know them as a whole person (eg, their values and beliefs), to coordinate their care, and to provide it continuously.8 They commonly ask, "Are you only a GP?" — and worse, GPs themselves often reply "yes"! Continuing medical education for GPs is still dominated by specialists.
A competent and self-confident general practice workforce is good for a nation's health.9 Research comparing nations suggests that a strong, self-sufficient, self-assured, and respected primary healthcare sector leads to both improved quality and more cost-efficient care.9 For example, the Netherlands has one of the world's highest quality, most cost-effective primary care systems, while Belgium, until recently, seemed to lag far behind — differences that are surely attributable to the very different structure of their healthcare systems. Britain and Australia seem to lie between these two extremes.
To allow general practice to fail would be serious for Australia. We argue here that the many steps that have been instituted around the world are necessary to improve primary care, but need to focus more on the intellectual side of the discipline.
There are several reasons for the poor status of GPs within the profession. Market forces are obviously important: GPs are just less rare. Access to specialists is restricted by delays and waiting lists in public hospitals. One can usually see a GP in a day or two for a non-urgent problem, even in rural areas (where there is a relative scarcity of GPs). In private practice, specialists are much more likely to charge fees above the Medicare schedule fee. The Australian rate of bulk-billing (direct invoicing of Medicare for a discounted fee) in 2002 was 73% for vocationally registered GPs, 20% for obstetricians, and 9% for anaesthetists.10 General practice expertise is less deep (if very much broader), focuses on process more than content, and is harder to measure and explain to managers and politicians.11 We GPs are more expert at processes of care, such as communication skills, accommodating the psychosocial context, and continuity of care. We are less expert in diseases, leading to undervaluing of our skills.
Possible reasons for the poorer performance of GPs in research and publishing are many. GPs are relatively poorly represented in universities, with higher teaching loads per academic.12 This results not just from academic GPs being the "newest kids on the block", but also from the grander and more dominant status of biomedicine. There are not enough high-profile academic GPs to lead the discipline.13 In the competitive environment of academia, the rich get richer.
Solutions are probably many and complex. Simple responses from government, such as substantially increasing the remuneration of GPs, seem unlikely. However, overt inequities should be addressed, by paying the same amount to doctors of the same seniority for the same services. The costly Relative Values Study reported in 2001,14 but solutions have become mired in politics.
Some very attractive ideas for empowering GPs were initiated in the United Kingdom.15 Firstly, fund- (budget-) holding, and then Primary Care Trusts, put GPs at the core of health resource allocation. Similar schemes were introduced in the Netherlands and New Zealand.16 A crucial feature of these systems was their encouragement of professional autonomy, but GPs were less enamoured, and professional morale slipped further.17 In the UK and the Netherlands this may have been because more responsibility was forced on GPs than they wanted,17 and because resources for general practice decreased while expectations rose. Similarly in the United States, where "managed care" strengthened the gatekeeper role of primary care, a disproportionate share of unpopular cost containment fell to GPs.3 In the UK, the proposed new GP contract offers stepped increases in primary care investment,18 but the profession is still digesting its implications.
Divisions of General Practice are an Australian solution.19 They have helped GPs collaborate to improve local health services and to conduct ambitious projects such as the Coordinated Care Trials.20 This activity will probably continue to improve the status of GPs.
However, we believe that another essential for improving the status of general practice is strengthening its intellectual aspects, through promoting more and better critical thinking among GPs. How can we make that happen?
For the individual GP, becoming active in research — clearly a marker for critical thinking — is an obvious solution. Several research initiatives are in train in Australia or overseas (Box 3).
The multifaceted Primary Health Care Research, Evaluation and Development program is the most important Australian initiative, with federal government funding of $50 million over 5 years.21 It provides for a research institute and funds for conducting research, for research positions and for research-support positions in universities.
"Protected time" for GPs to undertake research, cordoned off from clinical demands, is provided in Australia through individual funding (eg, bursaries, fellowships, scholarships and grants for "novice researchers" in primary care).
Research networks allow GPs to participate actively not just in collecting data, but also in planning what data to collect, and why. In the UK, about 3800 general practices (36%) are linked to academic departments, increasingly through primary-care research networks.22 Even more impressively, in the Netherlands over 50% of GPs are engaged with their local medical school or the Dutch College of General Practitioners through either research networks,23 teaching (undergraduate and postgraduate) or both. In Australia, no data are available on the proportion of GPs involved in research networks, but it is likely to be fewer than 4%.
Embracing more clinical research might result in greater research uptake by GPs, as it is often more interesting to them. More clinical research is sorely needed in its own right, as most illness and disease is encountered in general practice.24 The Netherlands now has a special research fund for common clinical problems.25
Young GPs can be attracted to research through academic registrar positions, which provide a clear career route to general practice academia. However, there is currently less than one academic GP registrar position per 1000 practising GPs in Australia.
In promoting intellectual solutions in general practice, we need to avoid focusing too much on primary research. Not all GPs need to participate in research to enhance their practice, far less to lead it. Perhaps more important to critical thinking than generating research is using it.
In Australia, the National Institute for Clinical Studies has the responsibility of spinning the straw of research into the gold of improved clinical practice. It is turning its focus on to general practice. There is amazing collaboration between Dutch universities and GPs: universities create the research evidence and assist the Dutch College of General Practitioners to transform it into evidence-based guidelines "owned" by the discipline. These are widely respected and used, or rejected — for intellectual rather than territorial reasons.26 However, delivering evidence only in the form of guidelines is dangerous to critical thinking if the guidelines are more "cookbook recipes" for what to do than systematised summaries of the evidence that can inform decisions, as they should be.27
GPs can be encouraged to handle data and apply them to their practice routinely in several ways. Evidence-based medicine is clearly an important way of thinking critically every day, especially when it emphasises the process — application of properly interpreted research findings for individual patients — rather than simply doing the "right" thing. Thinking critically is not the only reason for practising this way; patients will increasingly demand this approach.28 There are other ways of applying evidence-based medicine in general practice,29 such as the use of individual medi-cation effectiveness tests. These are a clinical application of n-of-1 trials, in which doctors help patients collect data about their illnesses to decide optimal management.30
GP access to research training and support at reasonable cost would also increase critical thinking enormously. This is now available across most of Australia, but more important than availability seems to be the incentive to take it up.
Some initiatives might be subtle. Increasing the "critical mass" of academic GPs by amalgamating postgraduate and undergraduate teachers into single departments has been achieved already in several parts of Australia. Divisions of General Practice are beginning to see the value of critical thinking among their member GPs, and are forming closer relationships with suitable university departments.
When individual GPs feel that their peers command the intellectual basis of their discipline, see GP-generated research improving the care they deliver, and feel confident about finding the best information to help solve patient problems, then self-esteem, self-reliance and status will surely improve. Establishing a stronger intellectual basis for general practice will take time. We hope that the seeds are now sown. We have powerful role models to follow, and some exciting options to pursue, although we still need innovations. Which will prove most useful?
1: Applicants for general practice registrar positions in Australia relative to places*
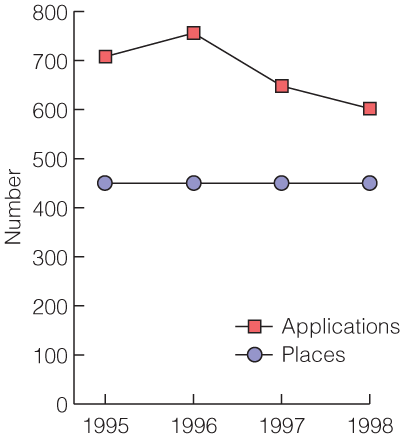
*R Coote, General Practice Education Australia Ltd, Canberra, personal communication, Feb 2003.
2: Comparison of general practice characteristics between Australia and other countries7
|
Netherlands |
United Kingdom |
Australia |
||||||||
Workforce numbers crisis |
1960s |
1960s |
2000s |
||||||||
Total numbers of GPs (FTE) |
9500 |
32 430 |
20 000 |
||||||||
Population |
16 million |
60 million |
20 million |
||||||||
GPs per head of population |
1684 |
1850 |
1000 |
||||||||
Patient registration with GPs |
Yes |
Yes |
No |
||||||||
Vocational registration |
1970s |
1970s |
1990s |
||||||||
Substantial government investment in building GP research capacity |
1980s |
1990s |
2000s |
||||||||
Postgraduate training and teaching workforce in continuity with universities |
All |
None |
Rare and recent* |
||||||||
GPs in research networks |
> 50% |
< 36% |
< 4%? |
||||||||
FTE = full time equivalent. * For example, in North Queensland, Melbourne and Western Australia. |
|||||||||||
3: Strategies for improving critical thinking among Australian general practitioners (GPs)
Strategy |
Achievements in Australia (and overseas) |
What is still needed |
|||||||||
Research |
|
|
|||||||||
Increased research in general practice |
Primary Health Care Research, Evaluation and Development (PHC-RED) program |
More dedicated funding |
|||||||||
Increased relevance of research in general practice |
Special research fund for common clinical problems (Netherlands) |
Greater focus (and funding) on clinical research, as well as health services research |
|||||||||
Continuity between university departments and postgraduate general practice teaching |
In some centres (North Queensland, Melbourne, Western Australia) |
|
|||||||||
Research networks |
Australian Sentinel Practice Research Network (ASPReN), based on the American Sentinel Practice Research Network (extensive research networks in the UK and Netherlands) |
More local networks centred on university departments of general practice and rural health |
|||||||||
More "bag-carrying" GP researchers |
"Protected time" (fellowships, and bursaries); higher degree opportunities |
More networks, closer links between academia and GPs (Divisions) |
|||||||||
Research training courses and workshops |
Available in many parts of Australia at different levels of expertise |
|
|||||||||
Critical thinking |
|
|
|||||||||
Increased critical thinking among GPs |
n-of-1 trials; uptake of evidence-based medicine workshops |
More interventions to increase use of research by GPs |
|||||||||
Increasing critical thinking in clinical general practice |
Establishment of National Centre for Clinical Studies (NICS) (comparable to National Institute for Clinical Effectiveness [NICE] in the UK; college–university links in the Netherlands) |
|
|||||||||
Links between university and clinical GPs (research into practice) |
|
|
|||||||||
Career path into academic general practice |
Academic registrars (< 1 per 1000 practising GPs) |
More positions |
|||||||||
- Chris B Del Mar1
- George K Freeman2
- Chris van Weel3
- 1 Centre for General Practice, University of Queensland Medical School, Herston, QLD.
- 2 Centre for Primary Healthcare and General Practice, Imperial College, London, UK.
- 3 Department of General Practice, University Medical Centre, Nijmegen, Netherlands.
None identified.
- 1. Moore G, Showstack J. Primary care medicine in crisis: toward reconstruction and renewal. Ann Intern Med 2003; 138: 244-247.
- 2. Ginsburg PB. Payment and the future of primary care. Ann Intern Med 2003; 138: 233-234.
- 3. Sandy LG, Schroeder SA. Primary care in a new era: disillusion and dissolution? Ann Intern Med 2003; 138: 262-267.
- 4. Commonwealth Department of Health and Ageing. Medicare Benefits Schedule (MBS), 1 November 2002 with 1 May 2003 supplement. Available at: www.health.gov.au/pubs/mbs/ (accessed May 2003).
- 5. Is primary-care research a lost cause? Lancet 2003; 361: 977.
- 6. Askew DA, Glasziou PP, Del Mar CB. Research output of Australian general practice: a comparison with medicine, surgery and public health. Med J Aust 2001; 175: 77-80.
- 7. Harding G. The supply and distribution of general practitioners. In: General practice in Australia: 2000. Canberra: Commonwealth Government Publisher, 2000: 41-73.
- 8. Safran DG. Defining the future of primary care: what can we learn from patients? Ann Intern Med 2003; 138: 248-255.
- 9. Starfield B. Is primary care essential? Lancet 1994; 344: 1129-1133.
- 10. Elliot A. Decline in bulk billing: explanations and implications. Canberra: Commonwealth Government, Information and Research Services, 2002.
- 11. Haslam D. "Schools and hospitals" for "education and health". BMJ 2003; 326: 234-235.
- 12. Kamien M. Has Australian academic general practice really come of age? Med J Aust 2001; 175: 81-83.
- 13. Van Der Weyden MB. Australian general practice at a fork in the road: which way forward? [editorial]. Med J Aust 2001; 175: 62-63. <MJA full text>
- 14. Medicare Schedule Review Task Force. Relative value study. Australian Department of Health and Aged Care, 2001. Available at: http://www.health.gov.au/rvs/index.htm. (accessed May 2003).
- 15. Wilkin D. Primary care budget holding in the United Kingdom National Health Service: learning from a decade of health service reform. Med J Aust 2002; 176: 539-542. <MJA full text>
- 16. Malcolm L. GP budget holding in New Zealand: lessons for Britain and elsewhere? BMJ 1997; 314: 1890-1892.
- 17. Evans J, Lambert T, Goldacre M. GP recruitment and retention: a qualitative analysis of doctors' comments about training for and working in general practice. Occas Pap R Coll Gen Pract 2002: iii-vi, 1-33.
- 18. GP Committee of the BMA and the NHS Confederation. Investing in general practice: The New General Medical Services Contract. London: British Medical Association, National Health Service Confederation, 2003.
- 19. Pegram R, Sprogis A, Buckpitt J. Divisions of general practice: a status review. Aust Health Rev 1995; 18: 78-94.
- 20. Commonwealth Department of Health and Aged Care. The Australian Coordinated Care Trials: summary of the final technical national evaluation report on the first round of trials. Canberra: Commonwealth of Australia; 2001. (Report No. 2911.)
- 21. Shah NC, Pond D, Heaney S. Research capacity building in general practice. The new Australian scene. Aust Fam Physician 2002; 31: 201-204.
- 22. Society for Academic Primary Care. New century, new challenges. A report from the heads of Departments of General Practice and Primary Care in the medical schools of the United Kingdom. London: Royal College of General Practitioners, 2002.
- 23. van Weel C. General practice research networks: gateway to primary care evidence. Med J Aust 2002; 177: 62-63. <eMJA full text>
- 24. Green LA, Yawn BP, Lanier D, Dovey SM. The ecology of medical care revisited. N Engl J Med 2001; 344: 2021-2024.
- 25. Dutch College of General Practitioners (NHG). Fund for common disorders. NHG, 2003. Available at: http://nhg.artsennet.nl/index.asp?s=2749 (accessed May 2003).
- 26. Grol R, Dalhuijsen J, Thomas S, et al. Attributes of clinical guidelines that influence use of guidelines in general practice: observational study. BMJ 1998; 317: 858-861.
- 27. Del Mar C. Guiding guidelines into practice [editorial]. Aust Prescriber 2001; 24: 50-51.
- 28. Muir Gray JA. The resourceful patient. Oxford: eRosetta Press, Alden Group, 2002.
- 29. Del Mar CB, Glasziou PP. Ways of using evidence-based medicine in general practice. Med J Aust 2001; 174: 347-350.
- 30. Nikles CJ, Glasziou PP, Del Mar CB, et al. Preliminary experiences with a single-patient trials service in general practice. Med J Aust 2000; 173: 100-103.





Abstract
General practice is suffering a crisis of status, as shown by financial, power and intellectual markers.
This is serious as a strong general-practice workforce is important to deliver cost-effective, high-quality healthcare.
We argue that strengthening the intellectual aspects of general practice (particularly critical thinking) is essential.
Most strategies to achieve this centre on research, with many initiatives in Australia and overseas to enhance research by general practitioners; there is still insufficient clinical research in general practice.
Other ways to improve critical thinking include promoting use of evidence-based medicine, provided it is not implemented only via "cook-book" guidelines.
Other innovations are desperately needed.