Management of patients with chest discomfort is not straightforward when the discomfort has resolved and normal results are obtained on physical examination, electrocardiography (ECG) and measurement of baseline cardiac troponin levels. These patients have been defined as having "intermediate" risk of adverse cardiac outcomes in the subsequent six months.1 An unstructured approach to their management will lead, on the one hand, to inappropriate discharge and a "missed" myocardial infarction in 1%–5%2,3 and, on the other hand, to unnecessary or prolonged admissions in up to 50% of patients with chest pain.4
Chest pain clinical pathways have been designed to reduce the possibility of missing an infarction while facilitating early discharge of low risk patients. A United States study found that a structured approach to assessing intermediate-risk patients reduced costs5 and the incidence of missed myocardial infarctions from 4.5% to 0.4%.6
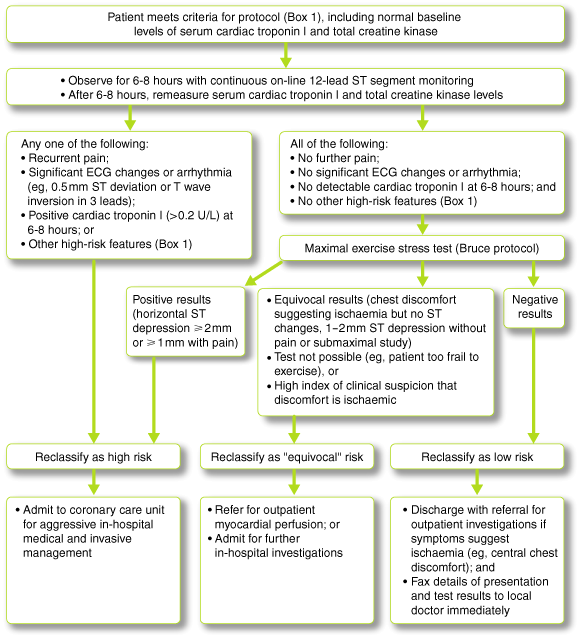
In 2000, the National Heart Foundation (NHF) and the Cardiac Society of Australia and New Zealand (CSANZ) published new Australian guidelines for management of unstable angina.1 These recommend use of a structured clinical pathway (accelerated chest pain assessment protocol) which allows intermediate-risk patients to be reclassified as low or high risk after a period of observation. We examined the outcomes of intermediate-risk patients managed with this protocol in a metropolitan tertiary care hospital.
The study was conducted at The Prince Charles Hospital, a tertiary-care hospital in Brisbane, QLD. As the study was a prospective audit of a clinical pathway, we did not seek patient consent nor permission from the hospital's research and ethics committee.
Subjects were consecutive patients who presented to the emergency department of the hospital between January 2000 and June 2001 and were managed with the accelerated chest pain assessment protocol (ACPAP). Criteria for use of ACPAP are listed in Box 1. They were used to identify patients at intermediate risk and to reduce the chance of including those with other diagnoses, such as aortic dissection or pulmonary embolism. The list is used as a checklist in the emergency department.
Serum levels of cardiac troponin I (Dimension, Dade Behring, Deerfield, Ill, USA) and total creatine kinase were measured at baseline. Patients with an initial positive cardiac troponin I were excluded from ACPAP and admitted to hospital forthwith. Myocardial infarction was defined as having occurred if both markers were elevated (troponin I > 0.2 μg/L, total creatine kinase > 160 U/L [women] or > 200 U/L [men]). This cut-off troponin level was selected as the analytic imprecision (coefficient of variation ≤ 10%) of the assay in our laboratory was 0.14 μg/L.
An ongoing educational program about the protocol for staff of the emergency and cardiology departments was begun before its introduction.
The protocol is outlined in Box 2. Continuous on-line 12-lead ST-segment monitoring was performed using the ST Guard (GE Marquette Corp, Milwaukee, Wis, USA). On weekends, exercise stress testing was performed by registrars and specially trained coronary care nurses. Cardiology registrars were responsible for patient reclassification as low or high risk. Reclassification of patients as low risk was audited at the end of the study by a senior cardiologist, who agreed with the decision in 406 of 409 patients.
Over the 18 months of the audit, 630 people who presented to the emergency department with chest pain met the criteria for intermediate risk and were managed with ACPAP. Most of the 630 patients (57%) were men, and mean age was 57 years (range, 27–87 years). Of the 630, 625 (99%) were directly contacted for 30-day follow-up, and 597 (95%) for six-month follow-up. For patients who could not be contacted, we excluded the possibility of admission to local hospitals and cardiac events known to their local doctor or listed on the Queensland Death Registry.
After application of ACPAP, 409 patients were reclassified as low risk (65%), 111 as equivocal risk (18%), and 110 as high risk (17%). Characteristics of the reclassified groups are shown in Box 3. Reclassified low-risk patients were younger and had lower rates of hypertension and prior coronary disease than higher-risk groups.
The mean length of hospital stay of all patients admitted with chest pain was 1.5 days in the 18 months after introduction of ACPAP, compared with 2.2 days in the previous year.
One hundred and eleven patients were reclassified as equivocal risk and admitted for further investigation. Reasons were:
exercise stress testing was not performed because of frailty or known coronary disease in 78 (70%);
they had an equivocal stress test result (poor exercise tolerance, pain but no ST depression or 1–2 mm ST depression without pain) in 16 (14%); and
there was a high clinical suspicion of coronary artery disease in 17 (15%).
Four hundred and nine low-risk patients were discharged after a mean stay in the chest pain unit of 14 hours:
326 had negative results on exercise stress testing;
46 had submaximal exercise stress tests (considered equivocal), but were discharged mainly because their coronary anatomy was known to be unsuitable for intervention; and
37 did not have exercise stress tests, often because delay was too great.
The 409 patients were referred either back to their local doctors (258 patients; 63%) or to the cardiology outpatient department (151; 37%), usually after further outpatient investigations; 36 low-risk patients (9%) were referred for outpatient myocardial perfusion or stress-echo study, three (1%) for exercise stress tests, 24 (6%) for upper gastrointestinal endoscopy, and 16 (4%) for abdominal ultrasound examination.
No deaths occurred in any group. Other adverse cardiac events are shown according to risk category in Box 4. Twenty-one high-risk patients (19%) had cardiac events within the six months: revascularisation (18 patients) and unplanned readmission with unstable angina (9) or AMI (2) (six patients had more than one event). In contrast, three low-risk patients (1%) had cardiac events in this period, all elective revascularisations. Nine equivocal-risk patients (8%) had cardiac events: revascularisation (8) and unplanned readmissions with unstable angina (5) (four had both).
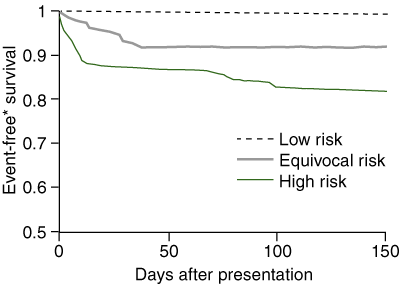
Event-free survival (freedom from death, revascularisation or readmission with unstable angina or AMI) is compared between the three groups in Box 5. Patients reclassified as low risk had excellent outcomes (no readmissions with unstable angina and only three elective revascularisation procedures), while high-risk and equivocal-risk groups had substantial numbers of cardiac events.
We found that ACPAP simplified and facilitated the effective management of patients at intermediate risk of adverse cardiac events at our hospital. Two-thirds of patients assessed with ACPAP were reclassified as low risk and discharged early a mean of 14 hours after presentation, allowing early return to work and normal activities; 1% of these patients had cardiac events (all elective revascularisations) by six-month follow-up, compared with 19% of high-risk patients. We have identified no missed AMIs since adopting the protocol. However, a low rate of missed AMI depends on the willingness of emergency staff to enrol patients with both "typical" and "atypical" symptoms in the protocol, particularly the elderly and those with diabetes, whose presentations are often "atypical" or even silent.
A limitation of the study was that it was a clinical audit and not a prospective controlled trial of differing strategies in managing chest pain. However, although observational, our study had the advantage of being large and prospective.
Since our study, the NHF and CSANZ have modified ACPAP to upgrade diabetes from an intermediate-risk to a high-risk feature. The new guidelines recommend invasive assessment and management of patients with diabetes with an acute coronary syndrome.7 However, in our audit, some patients with diabetes were reclassified to the low-risk group, but fortunately did not have a subsequent cardiac event.
Although early angiography is indicated in all high-risk patients, it was performed in only 41% during the index admission. This was not unreasonable, as many patients were frail or elderly, and some had known inoperable coronary anatomy. However, the only two late myocardial infarctions occurred in high-risk patients who were not managed according to the Australian guidelines — one patient who did not have angiography despite clear indications for doing so, and another who did not have early revascularisation and suffered an AMI after one month on a surgical waiting list.
Our results were similar to those of a recent US study which safely performed early stress testing in 1000 selected patients with chest pain suggestive of cardiac aetiology.8 Patients with negative stress test results had a low cardiac event rate at 30-day follow-up.8
The value of cardiac troponin levels to chest pain assessment protocols cannot be overestimated. Cardiac troponin level, particularly measured at 6–8 hours after presentation, is a very sensitive and specific marker of myocardial injury which confirms diagnosis, with the size of the rise closely correlating with prognosis.9-11 In addition, raised troponin levels identify patients who benefit from medical12,13 and invasive14 therapies. In 13 of the 14 patients with raised troponin levels who underwent angiography, coronary artery disease was confirmed. Cardiac troponin, used in concert with exercise–ECG stress testing, has previously been validated in the risk stratification of patients with chest pain.15 Although more sophisticated stress-testing methods (myocardial perfusion imaging or stress echocardiography) would be more sensitive in identifying patients with myocardial ischaemia, exercise–ECG stress testing is cheap, available in most hospitals, and able to be performed by appropriately trained junior staff.
This study confirmed that ACPAP is practical to implement. It uses readily available tests and can be applied in coronary care units, emergency department, or elsewhere in the hospital. However, it relies on a high standard of observation and a quick response to the development of high-risk features. Further studies might use newer, more sensitive biochemical tests of early ischaemia, or other methods of screening for coronary disease or provocable ischaemia.
The study also confirmed that ACPAP provides safe and effective risk stratification of patients at intermediate risk of adverse cardiac events, who otherwise pose management challenges. Follow-up of the reclassified risk groups validated the protocol, and, in particular, confirmed the safety of early discharge of the low-risk group. The protocol may greatly reduce or eliminate missed infarctions, allow early identification and treatment of high-risk patients, and reduce length of hospital stay. The chest pain protocol has been well accepted and rapidly incorporated into the "culture" of our hospital.
3: Characteristics of 630 patients managed with ACPAP (Accelerated Chest Pain Assessment Protocol)
|
|
Risk after reclassification |
|
||||||||
|
All (n = 630) |
Low (n = 409) |
Equivocal (n = 111) |
High (n = 110) |
P |
||||||
Age in years (mean [SD]) |
56.6 (12.5) |
53.6 (11.7) |
62.7 (12.6) |
60.9 (11.5) |
0.001 |
||||||
Serum cholesterol level (mean [SD]) |
4.9 (1.1) |
5.0 (1.1) |
4.7 (1.0) |
4.8 (1.1) |
NS |
||||||
Diabetes |
72 (11%) |
44 (11%) |
14 (13%) |
14 (13%) |
NS |
||||||
Smokers |
123 (20%) |
91 (22%) |
17 (15%) |
15 (14%) |
NS |
||||||
Hypertension |
70 (11%) |
31 (8%) |
22 (20%) |
17 (15%) |
0.001 |
||||||
Prior coronary disease* |
45 (7%) |
20 (5%) |
11 (10%) |
14 (13%) |
0.01 |
||||||
* History of myocardial infarction, angina, 50% lesion at coronary angiography or previous coronary revacularisation. |
|||||||||||
4: Outcomes in 630 patients, by risk category after reclassification by ACPAP
|
|
Risk after reclassification |
|||||||||
Outcome |
Total |
Low |
Equivocal |
High |
|||||||
Acute myocardial infarction |
8 (1%) |
0 |
0 |
8 (7%) |
|||||||
During initial admission |
6 (1%) |
0 |
0 |
6 (5%) |
|||||||
Within 30 days |
1 (0.2%) |
0 |
0 |
1 (1%) |
|||||||
Within 1–6 months |
1 (0.2%) |
0 |
0 |
1 (1%) |
|||||||
Coronary angiography |
104 (17%) |
24 (6%) |
21 (19%) |
59 (53%) |
|||||||
During initial admission |
56 (9%) |
0 |
11 (10%) |
45 (41%) |
|||||||
Within 30 days |
23 (4%) |
13 (3%) |
3 (3%) |
7 (6%) |
|||||||
Within 1–6 months |
25 (4%) |
11 (3%) |
7 (6%) |
7 (6%) |
|||||||
Revascularisation* |
29 (5%) |
3 (0.7%) |
8 (7%) |
18 (16%) |
|||||||
During initial admission |
17 (3%) |
0 |
3 (3%) |
14 (13%) |
|||||||
Within 30 days |
3 (0.5%) |
1 (0.2%) |
2 (2%) |
0 |
|||||||
Within 1–6 months |
9 (2%) |
2 (0.5%) |
3 (3%) |
4 (4%) |
|||||||
Unplanned readmission with unstable angina or AMI |
16 (3%) |
0 |
5 (5%) |
11 (10%) |
|||||||
Within 30 days |
9 (1%) |
0 |
4 (4%) |
5 (5%) |
|||||||
Within 1–6 months |
7 (1%) |
0 |
1 (0.9%) |
6 (5%) |
|||||||
AMI = acute myocardial infarction. |
|||||||||||
6: Relationship between results of exercise stress tests and revascularisations in 450 patients
|
Result of exercise stress test |
||||||||||
|
Positive (n = 34) |
Equivocal (n = 66*) |
Negative (n = 347†) |
||||||||
Angiography |
26 (76%) |
14 (21%) |
17 (5%) |
||||||||
Coronary artery disease confirmed |
21 (62%) |
5 (8%) |
3 (1%) |
||||||||
Revascularisation |
6 (18%) |
1 (2%) |
3 (1%) |
||||||||
* Included four patients who were classified as high risk for other reasons (eg, a small rise in troponin I level) but underwent exercise stress testing for clinical reasons. † Included 21 patients classified as equivocal- or high-risk for other reasons. |
|||||||||||
Received 21 August 2002, accepted 10 January 2003
- Con N Aroney1
- Heather L Dunlevie2
- JH Nicholas Bett3
- Cardiology Department, The Prince Charles Hospital, Brisbane, Qld, Australia.
This study was supported in part by the Australian Government National Demonstration Hospitals Program — Phase 3.
Dr Aroney is chairman of the Clinical Issues Committee of the National Heart Foundation and principal author of the Management of unstable angina guidelines — 2000, which advocate use of a structured assessment protocol for intermediate-risk patients.
- 1. Aroney CN, Boyden AN, Jelinek MV, et al. Management of unstable angina. Guidelines–2000. Med J Aust 2000; 173 Suppl 16 Oct: S65-S88.
- 2. McCarthy BD, Beshansky JR, D'Agostino RB, Selker HP. Missed diagnoses of acute myocardial infarction in the emergency department: results from a multicenter study. Ann Emerg Med 1993; 22: 579-582.
- 3. Jesse RL, Kontos MC. Evaluation of chest pain in the emergency department. Curr Probl Cardiol 1997; 22: 149-236.
- 4. Lee TH, Rouan GW, Weisberg MC, et al. Clinical characteristics and natural history of patients with acute myocardial infarction sent home from the emergency room. Am J Cardiol 1987; 60: 219-224.
- 5. Roberts RR, Zalenski RJ, Mensah EK, et al. Costs of an emergency department-based accelerated diagnostic protocol vs hospitalization in patients with chest pain: a randomized controlled trial. JAMA 1997; 278: 1670-1676.
- 6. Graff LG, Dallara J, Ross MA, et al. Impact on the care of the emergency department chest pain patient from the chest pain evaluation registry (CHEPER) study. Am J Cardiol 1997; 80: 563-568.
- 7. Heart Foundation. Information for Health Professionals. Management of unstable angina guidelines 2000. Addendum July 2002. Available at www.heartfoundation.com.au/prof/index_fr.html (accessed Feb 2003).
- 8. Amsterdam EA, Kirk JD, Diercks DB, et al. Immediate exercise testing to evaluate low-risk patients presenting to the emergency department with chest pain. J Am Coll Cardiol 2002; 40: 251-256.
- 9. Ohman EM, Armstrong PW, Christenson RH, et al. Cardiac troponin T levels for risk stratification in acute myocardial ischemia. GUSTO IIA Investigators. N Engl J Med 1996; 335: 1333-1341.
- 10. Lindahl B, Venge P, Wallentin L. Relation between troponin T and the risk of subsequent cardiac events in unstable coronary artery disease. The FRISC study group. Circulation 1996; 93: 1651-1657.
- 11. Antman EM, Tanasijevic MJ, Thompson B, et al. Cardiac-specific troponin I levels to predict the risk of mortality in patients with acute coronary syndromes. N Engl J Med 1996; 335: 1342-1349.
- 12. Lindahl B, Venge P, Wallentin L. Troponin T identifies patients with unstable coronary artery disease who benefit from long-term antithrombotic protection. Fragmin in Unstable Coronary Artery Disease (FRISC) Study Group. J Am Coll Cardiol 1997; 29: 43-48.
- 13. Heeschen C, Hamm CW, Goldmann B, et al. Troponin concentrations for stratification of patients with acute coronary syndromes in relation to therapeutic efficacy of tirofiban. PRISM Study Investigators. Platelet Receptor Inhibition in Ischemic Syndrome Management. Lancet 1999; 354: 1757-1762.
- 14. Cannon CP, Weintraub WS, Demopoulos LA, et al. Comparison of early invasive and conservative strategies in patients with unstable coronary syndromes treated with the glycoprotein IIb/IIIa inhibitor tirofiban. N Engl J Med 2001; 344: 1879-1887.
- 15. Lindahl B, Andren B, Ohlsson J, et al. Risk stratification in unstable coronary artery disease. Additive value of troponin T determinations and pre-discharge exercise tests. FRISK Study Group. Eur Heart J 1997; 18: 762-770.





Abstract
Objective: To determine the feasibility, safety and effectiveness of a structured clinical pathway for stratification and management of patients presenting with chest pain and classified as having intermediate risk of adverse cardiac outcomes in the subsequent six months.
Design: Prospective clinical audit.
Participants and setting: 630 consecutive patients who presented to the emergency department of a metropolitan tertiary care hospital between January 2000 and June 2001 with chest pain and intermediate-risk features.
Intervention: Use of the Accelerated Chest Pain Assessment Protocol (ACPAP), as advocated by the Management of unstable angina guidelines — 2000 from the National Heart Foundation and the Cardiac Society of Australia and New Zealand.
Main outcome measure: Adverse cardiac events during six-month follow-up.
Results: 409 patients (65%) were reclassified as low risk and discharged at a mean of 14 hours after assessment in the chest pain unit. None had missed myocardial infarctions, while three (1%) had cardiac events at six months (all elective revascularisation procedures, with no readmissions with acute coronary syndromes). Another 110 patients (17%) were reclassified as high risk, and 21 (19%) of these had cardiac events (mainly revascularisations) by six months. Patients who were unable to exercise or had non-diagnostic exercise stress test results (equivocal risk) had an intermediate cardiac event rate (8%).
Conclusions: This study validates use of ACPAP. The protocol eliminated missed myocardial infarction; allowed early, safe discharge of low-risk patients; and led to early identification and management of high-risk patients.