There is clear evidence that early reperfusion in patients suffering acute ST-elevation myocardial infarction (STEMI) reduces mortality and other complications.1-5 Although data suggest that early angioplasty gives the best results, access to this therapy is limited.6-9 In practical terms, thrombolytic therapy is the reperfusion strategy to which most patients have best access.
Outcome — specifically, size of infarct and mortality — is related to the time interval between symptom onset and reperfusion.10-12 The interval for which healthcare services can be accountable is the period between notification by the patient (in Australia, usually calling the ambulance service) and commencement of therapy — the so-called call-to-needle (CTN) time. Past efforts have focused largely on the hospital component of care, referred to as the door-to-needle (DTN) time, and with good effect.13,14 However, it has been suggested that CTN time is a more appropriate measure of healthcare system performance.15
In 1994, the British Heart Foundation (BHF) recommended that patients with STEMI should receive thrombolytic therapy within 90 minutes of calling for medical assistance.15 The United Kingdom Department of Health goes further, setting a target of 60 minutes from first contact with a healthcare professional to thrombolysis,16 although doubt has been raised about the practic-ability of this target.17 In Australia, the National Heart Foundation has stated that if patients cannot reach a hospital for thrombolytic therapy within 90 minutes of calling the emergency service, out-of-hospital thrombolysis should be considered.18
There is currently little evidence about how healthcare systems are performing against the BHF benchmark. One study reported a median CTN time for a metropolitan area of 95 minutes, with only 46% of patients treated within 90 minutes, and a median CTN time of 150 minutes (5% of patients treated within 90 minutes) in a rural area without prehospital thrombolysis.19 A pilot study in western Melbourne suggested that the 90-minute benchmark is being met in 64% of eligible cases.20
Our primary aim was to determine the proportion of patients in Victoria treated within the BHF CTN time of 90 minutes. Secondary aims were to determine the impact of treatment within 90 minutes and 60 minutes on mortality, the proportion of patients treated within 60 minutes, whether pre-arrival notification of receiving hospitals influenced CTN time, and to model the potential lives saved by achieving CTN times of between 60 and 90 minutes.
This study was a medical record review of patients with STEMI who arrived at any of the participating hospitals by ambulance and received thrombolysis. Data was collected from Melbourne metropolitan and rural hospitals in Victoria, and from the Metropolitan Ambulance Service (Victoria) (MAS) and Rural Ambulance Victoria (RAV). Twenty-nine hospitals (14 metropolitan and 15 rural) were approached to participate.
Eligible patients were those who arrived at hospital by ambulance and received thrombolysis for STEMI in the periods 1 January 1999 to 30 June 2000 and 1 January to 31 December 2001. These periods were defined by logistics and available funding.
Potentially eligible patients were identified from each hospital by various methods, including hospital databases and established audit processes. The clinical diagnosis of STEMI requiring thrombolysis was validated by research officers. Records with incomplete time data were excluded.
Information collected included patient age and sex and location of ambulance retrieval, clinical assessment variables (eligibility for study), onset of symptoms, mode of transport, ambulance call time, ambulance dispatch time, prenotification to receiving hospital, response time (time from call to the ambulance service and ambulance arrival at patient location), scene time (time from ambulance arrival to departure from patient location), transport time (departure from patient location to arrival at hospital), time that thrombo-lysis was commenced, final diagnosis and in-hospital mortality. Missing information in relation to ambulance transportation details was obtained from MAS and RAV records.
Data were analysed with descriptive statistics, χ2 analysis for comparison of proportions, Mann–Whitney U test for comparison of continuous variables, relative risk for mortality, and the κ statistic for inter-rater reliability, using Analysis-IT software.21 Multiple logistic regression was performed using SPSS.22 The variables included for logistic regression were onset-to-call time, sex, age, transport time, DTN time and CTN time, with the outcome being mortality.
A statistically significant result was one with a P value < 0.05. A clinically significant difference in time-interval data was considered to be more than 10 minutes.
The project was approved by the institutional ethics committees of participant hospitals.
Of the 29 hospitals approached, data were collected from 20 (11/14 metropolitan and 9/15 rural; see acknow-ledgements) or 69%.
At these 20 hospitals, there were 2256 presentations of patients with STEMI who received thrombolysis during the study period. Inter-rater reliability with respect to study eligibility and electrocardiographic criteria was assessed for 62 patients (2.7% of screened cases) with very good agreement (κ, 0.88). However, only 1147 patients met the study criteria (Box 1).
The patients were predominantly male (69% [797]). Patients were aged 21–93 years (median, 67 years). About a quarter of the study group (26% [293/1147]) were from rural areas. Most patients (81.4% [896/1101, missing data for 46]) received their thrombolysis in hospital emergency departments.
Median CTN time was 83 minutes (range, 29–894 minutes). Median DTN time was 37 minutes (range, 0–853 minutes). Most patients (61% [697]) received thrombolysis within the BHF 90-minute benchmark. Only 15% (169) received thrombolysis within 60-minutes.
Patients treated in smaller rural centres were less likely to receive thrombolysis within 90 minutes; 40% (36/89) of those in small rural areas (< 50 000 population) were treated within 90 minutes compared with 60.8% (124/204) of those in larger rural areas (> 50 000 population) and 62.9% (537/854) of those in metropolitan areas (P = 0.0002, omnibus χ2 test).
There were 98 in-hospital deaths (8.5%). Patients with CTN times over 90 minutes had an increased risk of dying (relative risk, 1.8; 95% CI, 1.3–2.7) compared with those with CTN times within 90 minutes. Patients with CTN times over 60 minutes had a relative risk of death of 2.2 (95% CI, 1.1–4.8) compared with those with CTN within 60 minutes.
A comparison of patients with CTN times within and over 90 minutes in terms of age, sex and percentage with a final diagnosis of acute myocardial in-farction showed that the group with CTN times over 90 minutes had a significantly higher median age (68 years; range, 21–93 years v 65.5 years; range, 25–93 years; P = 0.0043), but the differences between the groups in male: female ratio (2.45 v 2.04) and in percentage of patients with a final diagnosis of acute myocardial infarction (98% v 99%) were not significant.
Box 2 shows a comparison of time intervals for patients with CTN times within and over 90 minutes. Those with CTN times longer than 90 minutes had a clinically significant delay between symptom onset and calling an ambulance. The largest difference between the groups was in DTN time, with the group with CTN time longer than 90 minutes having a clinically and statistically significant difference in DTN time (P < 0.0001).
A comparison of time intervals for patients with CTN time over 90 minutes based on geographical location of treating hospital is shown in Box 3. Patients in smaller rural centres had longer onset-to-call times. Among rural patients, 12.6% (37/293) had response times of more than 30 minutes, and 20.5% (60/293) had transport times in excess of 30 minutes — seven in excess of 60 minutes.
Patients for whom there was pre-notification of the receiving hospital by the ambulance service were more likely to have CTN times less than 90 minutes (P = 0.0017), as were patients who received thrombolysis in hospital emergency departments (P < 0.0001). Patients with transport times over 20 minutes were significantly less likely to achieve CTN times less than 90 minutes compared with those with shorter transport times (116/308 [38%] v 581/839 [69%]; P < 0.0001).
In the logistic regression analysis, controlling for the other variables, CTN time remained significantly associated with mortality, with an odds ratio of 1.007 (95% CI, 1.003–1.011; P = 0.001).
There is clear evidence that morbidity and mortality resulting from STEMI increase with time from symptom onset to reperfusion.10,11 Therefore the concept of CTN time as a measure of healthcare-system performance makes intuitive sense, although it is not entirely clear how the BHF 90-minute benchmark and the UK Health Department 60-minute benchmarks were derived.
Given the population concentration in metropolitan Melbourne and the fact that 11 of 14 metropolitan hospitals participated, our study population represents the vast majority of eligible patients in Victoria. We have shown that the BHF benchmark is only being met for 61% of such patients and that thrombolysis within 90 minutes is associated with a significantly reduced risk of mortality from STEMI.
CTN time remained significantly associated with mortality after controlling for the effects of other variables (odds ratio, 1.007). As CTN time is a continuous variable measured in minutes, this odds ratio refers to the effect of each one-minute reduction in CTN time, and the effect is exponential with multiple-minute changes in CTN time. It is of concern that the benchmark is being achieved for such a small proportion of eligible patients.
Of even more concern is the disparity between urban and rural settings. Longer CTN times occur in rural settings despite a sophisticated prehospital system with good communications and response times. Our data suggest that part of the problem lies within hospitals (DTN times), but other issues relate to geography (distance from a thrombo-lysis-capable facility), between-agency processes (eg, prior notification of receiving hospitals) and ineffective use of resources (in Victoria, paramedics do not administer thrombolysis).
All these parts of the continuum need attention to effectively reduce CTN times. However, given the large area of Victoria (227 000 square kilometres), the concentration of population in Melbourne (70%) and lack of thrombolysis-capable hospitals in some rural and semi-rural areas, it is unlikely a single solution will meet the needs of all regions. Similar problems are also evident in the United Kingdom and North America.19,23
The biggest single factor distinguishing patients for whom CTN times less than 90 minutes were achieved was DTN time. This is not surprising, as most patients were in metropolitan areas with relatively short transport times. Strategies that have been shown to reduce DTN time include prehospital electrocardiography,24,25 thrombo-lysis delivery in the emergency department,26-28 fast-track pathways29 and nurse-initiated thrombolysis.30 Another strategy highlighted by our data is notifying the receiving hospital in advance of a patient who may need thrombolysis. At present, the usefulness of this strategy is limited, as it relies in part on paramedics recognising ST elevation. At the time of our study, Victorian ambulances only had limb-lead monitors, so anterior ST elevation could not be identified. Availability of equipment capable of viewing limb and chest ECG leads and transmitting that information to the receiving hospital might significantly reduce DTN times. Such equipment is available and has been shown to be effective.31
Our study also showed that patients with transport times over 20 minutes were less likely to be treated within 90 minutes. Detailed analysis of the data identified several regions where this is a consistent problem (some in rural areas and others in outer metropolitan suburbs). For these regions, additional strategies such as prehospital thrombolysis need to be considered. How this might be delivered may vary, as not all regions have advanced-skills ambulance officers and a minimum volume of exposure is needed for practitioners to retain skills. Models might include paramedic-initiated thrombolysis at home or en route, local doctor-initiated thrombolysis or nurse-initiated thrombolysis at a local clinic.
Some authors have advocated a wholesale move to prehospital thrombolysis. There is good evidence that prehospital thrombolysis can reduce mortality, but this is mainly based on research in regions with long prehospital times.31 Implementation would require an increase in training, resources and equipment for ambulance services or general practitioners. In metropolitan areas, where transport times to a thrombolysis-capable hospital are short, this would be difficult to justify, as the reduction in CTN time is likely to be very small. On the other hand, in areas with long prehospital times, the case for prehospital thrombolysis is strong.
It is our view that strategies to reduce CTN should be region-specific, taking into account case load, geography and resources, and should be developed and "owned" by local healthcare services. This approach is most likely to produce a system that will work and be sustainable.
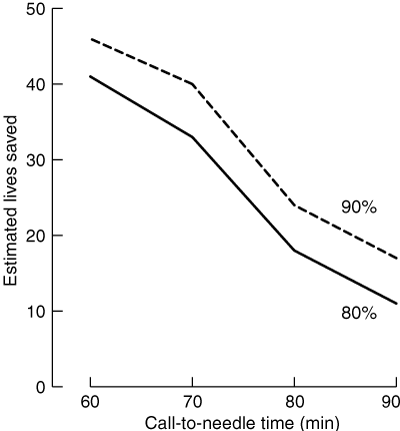
From our data, basing an analysis on dichotomous mortality rates and assuming that CTN time is the major factor in mortality, it is possible to estimate potential lives saved by reduced CTN times. As shown in Box 4, if 80% of patients had had a CTN time of less than 90 minutes, an estimated 11 lives would have been saved (95% CI, 7–20). If 90% had been treated within 90 minutes, an estimated 17 lives (95% CI, 11–26) would have been saved, and if 80% had been treated within 70 minutes, the estimated mortality reduction is 33 lives (95% CI, 24–43).
Although not the primary focus of our study, we found that there are considerable delays in patients with STEMI calling an ambulance. As increased time from symptom onset to treatment has been shown to be associated with increased mortality,10,11 this is clearly an area where improvement would be desirable. Strategies might include community education and access to health advice lines.
Limitations inherent in multicentre, record-review research apply to our study. Individual hospitals were responsible for identifying eligible patients, and some may have been missed. However, it is unlikely that there was any systematic bias. The study protocol did not allow us to collect data on infarct size or location, or comorbidities. These may have varied between the groups, partly accounting for the difference in mortality, although with a sample of this size it is not very likely.
Generalisability of our data to other settings might also be questioned. Although the geography and population density of Victoria is different from other countries, the issues of DTN time, transport times to thrombolysis-capable facilities, the role of prehospital thrombolysis and the effective use of resources are common to all countries with the Anglo-American model of prehospital care.
The question of an appropriate CTN-time benchmark remains. Our study validated the impact on mortality of the BHF 90-minute benchmark (relative risk, 1.8). Although Victoria is meeting the BHF benchmark in only 61% of cases, we consider that attaining this benchmark is feasible with modest process changes and resources. The UK Health Department 60-minute benchmark showed a modest further reduction in mortality (relative risk, 2.2), but was only achieved for 15% of patients, suggesting that it is not feasible without major changes to service delivery and a massive input of resources. We recommend the adoption of the BHF benchmark, with targets of 90% achievement for metropolitan and urban areas and 80% for rural areas, acknowledging the issues of transport and distance. Future further reductions in CTN time should be the long-term aim.
1: Flow diagram showing how the study sample was derived

STEMI = ST-elevation myocardial infarction. ECG = electrocardiogram. Catheter laboratory = transferred to catheter laboratory prior to thrombolysis.
2: Analysis of time intervals from call to treatment for patients with call-to-needle (CTN) times within and over 90 minutes
Time interval (min) |
CTN time ≤ 90 minutes (n = 697) (median [range]) |
CTN time > 90 minutes (n = 450) (median [range]) |
Difference between medians (95% CI) |
||||||||
Onset to call |
49 (0–2918) |
67 (0–6552) |
18 (5–19) |
||||||||
Dispatch time |
2 (0–27) |
2 (0–86) |
0 (0) |
||||||||
Response time |
8 (0–29) |
11 (0–69) |
3 (3–4) |
||||||||
Scene time |
15 (1–44) |
16 (1–85) |
1 (1–3) |
||||||||
Transport time |
13 (1–50) |
19 (2–145) |
6 (5–7) |
||||||||
Door-to-needle time |
29 (0–68) |
59 (6–853) |
30 (28–33) |
||||||||
3: Comparison of time intervals from call to treatment for patients with call-to-needle times over 90 minutes by geographical location of treating hospital
Time interval (min) |
Metropolitan (median [range]) |
Large rural (median [range]) |
Small rural (median [range]) |
||||||||
Onset to call |
57 (0–5593) |
52 (0–936) |
87 (0–6552) |
||||||||
Dispatch time |
1 (0–36) |
2 (0–86) |
2 (0–36) |
||||||||
Response time |
9 (0–43) |
8 (0–65) |
10 (1–69) |
||||||||
Scene time |
15 (1–85) |
17 (1–46) |
17 (2–51) |
||||||||
Transport time |
15 (1–65) |
13 (1–70) |
20 (2–145) |
||||||||
Door-to-needle time |
36 (0–365) |
38 (8–853) |
43 (9–272) |
||||||||
Large rural = centres with > 50 000 population. Small rural = centres with < 50 000 population. |
|||||||||||
Received 1 October 2002, accepted 13 February 2003
- Anne-Maree Kelly1
- Debra Kerr2
- Ian Patrick3
- Tony Walker4
- 1 Joseph Epstein Centre for Emergency Medicine Research, Western Hospital, Footscray, VIC.
- 2 Clinical and Non-emergency Operations, Metropolitan Ambulance Service, Doncaster, VIC.
- 3 Clinical and Education Services, Rural Ambulance Service (Victoria), Ballarat, VIC.
This work was supported by a grant from the Australian Rotary Health Research Fund. We acknowledge the contribution of Tania Kerr for data collection and database management, the support of the Boards of Management of MAS and RAV, and the administrative staff of MAS and RAV for their help in finding missing data items. The study would not have been possible without the assistance of local researchers G Braitberg, M Geluk (Austin Hospital), L Bridgford, H McKee (Albury Base Hospital), M Bryant (Western Hospital), L Pouw, A MacLean (Box Hill Hospital), J Stickland, C Tauschke, G Campain (Ballarat Base Hospital), J Wassertheil, R Martin, S White (Frankston Hospital), J Ferguson, M Taylor, J Lake (Bendigo Hospital), A Rosengarten (Maroondah Hospital), M Ryan, D Eddey (Geelong Hospital), T Kambourakis, P Rosengarten (Monash Medical Centre), M Geaboc, H Blazko (Goulburn Valley Hospital), D Taylor, P Cameron (Royal Melbourne Hospital), A Wolff (Wimmera Health Care Group: Horsham), S Dilley (St Vincent's Hospital), R Lowen, C Winter, M Burggraaff, J Neal (Latrobe Regional Hospital), S Priestley (Sunshine Hospital), H Connor, J Bennett, A North (Central Gippsland Health Service: Sale), G Benton (Wangaratta Hospital), P Crossley (Williamstown Hospital), G Scott (Werribee Mercy Hospital), G Cooper (Metropolitan Ambulance Service), and M Ford (Rural Ambulance Victoria).
None identified.
- 1. European Co-operative Study Group for Streptokinase Treatment in Acute Myocardial Infarction. Streptokinase in acute myocardial infarction. N Engl J Med 1979; 301: 797-802.
- 2. ISIS-2 (Second International Study of Infarct Survival) Collaborative Group. Randomised trial of intravenous streptokinase, oral aspirin, both, or neither among 17 187 cases of suspected acute myocardial infarction: ISIS-2. Lancet 1988; 2: 349-360.
- 3. White HD, Norris RM, Brown MA, et al. Effect of intravenous streptokinase on left ventricular function and early survival after acute myocardial infarction. N Engl J Med 1987; 317: 850-855.
- 4. O'Rourke M, Baron D, Keogh A, et al. Limitation of myocardial infarction by early infusion of recombinant tissue-type plasminogen activator. Circulation 1988; 77: 1311-1315.
- 5. Rothbaum DA, Linnemeier TJ, Landin RJ, et al. Emergency percutaneous transluminal coronary angioplasty in acute myocardial infarction: a 3 year experience. J Am Coll Cardiol 1987; 10: 264-272.
- 6. de Boer MJ, Hoorntje JC, Ottervanger JP, et al. Immediate coronary angioplasty versus intravenous streptokinase in acute myocardial infarction: left ventricular ejection fraction, hospital mortality and reinfarction. J Am Coll Cardiol 1994; 23: 1004-1008.
- 7. Stone GW, Grines CL, Browne KF, et al. Implications of recurrent ischemia after reperfusion therapy in acute myocardial infarction: a comparison of thrombolytic therapy and primary angioplasty. J Am Coll Cardiol 1995; 26: 66-72.
- 8. Nunn CM, O'Neill WW, Rothbaum D, et al. Long-term outcome after primary angioplasty: report from the primary angioplasty in myocardial infarction (PAMI-I) trial. J Am Coll Cardiol 1999; 33: 640-646.
- 9. Weaver WD, Simes RJ, Betriu A, et al. Comparison of primary coronary angioplasty and intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review. JAMA 1997; 278: 2093-2098.
- 10. Boersma E, Maas ACP, Deckers JW, et al. Early thrombolytic treatment in acute myocardial infarction: reappraisal of the golden hour. Lancet 1996; 348: 771-775.
- 11. Koren G, Weiss AT, Hasin Y, et al. Prevention of myocardial damage in acute myocardial ischemia by early treatment with intravenous streptokinase. N Engl J Med 1985; 313: 1384-1389.
- 12. Turi ZG, Stone PH, Muller JE, et al. Implications for acute intervention related to time of hospital arrival in acute myocardial infarction. Am J Cardiol 1986; 58: 203-209.
- 13. Cummings P. Improving time to thrombolytic therapy for myocardial infarction by using a quality assurance audit. Ann Emerg Med 1992; 21: 1107-1110.
- 14. Moses HW, Bartolozzi JJ, Koester DL, et al. Reducing delay in the emergency room in administration of thrombolytic therapy for acute myocardial infarction associated with ST elevation. Am J Cardiol 1991; 68: 251-253.
- 15. Weston CF, Penny WJ, Julian DG. Guidelines for the early management of patients with myocardial in-farction. British Heart Foundation Working Group. BMJ 1994; 308: 767-771.
- 16. National Service Framework. Coronary heart disease emerging findings. London: Department of Health, 1998.
- 17. Rawles J. Call to needle times after acute myocardial infarction. New standard of 60 minutes has been proposed but may be too rigorous [letter]. BMJ 1999; 318: 1554.
- 18. Guidelines: Reperfusion therapy for acute myocardial infarction. Canberra: Heart Foundation of Australia, December 2000.
- 19. Rawles J, Sinclair C, Jennings K, et al. Call to needle times after acute myocardial infarction in urban and rural areas in northeast Scotland: prospective observational study. BMJ 1998; 317: 576-578.
- 20. Kelly AM, Kerr D. Benchmarking ambulance call-to-needle times for thrombolysis after acute myocardial infarction in Australia: a pilot study. Intern Med J 2002; 32: 138-142.
- 21. Analysis-IT for Microsoft Excel [computer program]. Leeds, UK: Analyse-It Software Ltd, 2000.
- 22. SPSS [computer program]. Version 11.0. Chicago: SPSS Inc., 2002.
- 23. Kapasi H, Kelly L, Morgan J. Thrombolysis in the air. Air-ambulance paramedics flying to remote communities treat patients before hospitalization. Can Fam Physician 2000; 46: 1313-1319.
- 24. Millar-Craig MW; Joy AV; Adamowicz M, et al. Reduction in treatment delay by paramedic ECG diagnosis myocardial infarction with direct CCU admission. Heart 1997; 79: 456-461.
- 25. Kereiakes DJ, Gibler WB, Martin LH, et al. Relative importance of emergency medical system transport and the prehospital electrocardiogram on reducing hospital time delay to therapy for acute myocardial infarction: a preliminary report from the Cincinnati Heart Project. Am Heart J 1992; 123: 835-840.
- 26. Letovsky E, Allen T. Initiating thrombolytic therapy for acute myocardial infarction. Whose job is it anyway? CMAJ 1996; 154: 509-511.
- 27. Parry G, Wrightson WN, Hood L, et al. Delays to thrombolysis in the treatment of myocardial infarction. J R Coll Physicians Lond 1993; 27: 19-23.
- 28. Hourigan CT, Mountain D, Langton PE, et al. Changing the site of delivery of thrombolytic treatment for acute myocardial infarction from the coronary care unit to the emergency department greatly reduces door to needle time. Heart 2000; 84: 157-163.
- 29. Pell ACH, Miller HC, Robertson CE, et al. Effect of "fast track" admission for acute myocardial infarction on delay to thrombolysis. BMJ 1992; 304: 83-87.
- 30. Wilmhurst P, Purchase A, Webb C, et al. Improving door to needle times with nurse initiated thrombolysis. Heart 2000; 84: 262-266.
- 31. O'Rourke MF, Cook A, Carroll G, et al. Accuracy of a portable interpretive ECG machine in diagnosis of acute evolving myocardial infarction. Aust N Z J Med 1992; 22: 9-13.





Abstract
Objective: To determine the proportion of patients in Victoria treated within the British Heart Foundation 90-minute call-to-needle (CTN) time benchmark for thrombolysis of ST-elevation myocardial infarction (STEMI), and to validate the British Heart Foundation 90-minute benchmark with respect to mortality.
Design: Cohort study.
Setting: 20 hospitals and two ambulance services in the State of Victoria, Australia.
Participants: 1147 patients with STEMI transported to hospital by ambulance and eligible for thrombolysis.
Main outcome measures: CTN time, and in-hospital mortality.
Results: Median CTN time was 83 minutes (mean, 93.2 min; range, 29–894 min). Median door-to-needle (DTN) time was 37 minutes (mean, 46.5 min; range, 0–853 min). 61% of patients received thrombolysis within the 90-minute benchmark. Patients with CTN times > 90 minutes had an increased risk of dying (relative risk, 1.8; 95% CI, 1.3–2.7). Factors associated with CTN time < 90 minutes were lower DTN time, prior notification of the receiving hospital and transport time less than 20 minutes.
Conclusion: The British Heart Foundation CTN time benchmark is being met for 61% of eligible STEMI patients in Victoria. Strategies to reduce CTN time should be region-specific, and should include attempts to reduce DTN and to enhance ambulance–hospital communication. Prehospital thrombolysis may be appropriate for some regions.