Traumatic brain injury (TBI) results from an external force to the brain causing transient or permanent neurological dysfunction. It is a relatively high-prevalence injury, being 10 times more common than spinal cord injury. The incidence is highest in people in the prime of their lives, coinciding with important events such as completing their education, developing their careers and establishing their families, and thus at a time when they are more likely to have financial problems. Much of the disability (and costs) associated with TBI is hidden, as survivors may have no physical evidence of their injury. Despite this, the consequences of TBI can severely and permanently change a person's life, resulting in family disruption, loss of income and earning potential, and considerable expense over a lifetime.1
The range of severity of TBI is broad, from concussion through to persistent vegetative states (Box 1).2,3 Most severe TBI in Australia follows motor-vehicle-related trauma. Whereas the introduction of safer car designs, airbags and other road traffic initiatives (eg, redesigning hazardous intersections, driver education campaigns, random breath testing, and reducing speed limits) have decreased the overall number of road fatalities, improvements in retrieval, neurosurgery and intensive care in the past few decades have enabled many people to survive injuries that previously would have been fatal. This combination of factors has meant that the challenge of TBI rehabilitation has not altered significantly in the past decade.
TBI displays an extremely varied spectrum of possible lesions and resulting potential disabilities. Moreover, each person has a different set of premorbid abilities and a different psychosocial situation. Because of this, the goals of rehabilitation need to be holistic, long term and individualised to each survivor and his or her family.
As there is a long timeframe for improvement, continuity of care is one of the most important goals in managing a person with traumatic brain injury. Families often take on much of this responsibility, but some degree of contact with medical and rehabilitation services will often be required for the rest of the person's life. Often it is the general practitioner who is expected to coordinate this care.
Recent estimates suggest that there are about 150 people admitted to hospital with TBI per 100 000 population per year.4 This figure probably underestimates the true incidence of TBI because of classification and diagnostic errors, as well as under-reporting of mild injury. Even without errors in data collection, a high proportion of people with mild TBI do not present to hospital. Severe and moderate head injuries account for 12–14 per 100 000 and 15–20 per 100 000 population, respectively. The incidence of mild TBI has been reported as 64–131 per 100 000.5,6
The incidence of TBI peaks in the age group 15–35 years, and is more common in males (male : female ratio, 3–4: 1). Much of this sex difference is thought to be related to risk-taking behaviour and is therefore potentially preventable. In Australia, motor-vehicle-related trauma accounts for about two-thirds of moderate and severe TBI, with falls and assaults being the next most common causes. Sporting accidents and falls account for a far greater percentage of mild injuries. Alcohol is associated with up to half of all cases of TBI.7
The forces inflicted on the head in TBI produce a complex mixture of diffuse and focal lesions within the brain. Damage resulting from an injury can be immediate (primary) or secondary in nature. Secondary injury results from disordered autoregulation and other pathophysiological changes within the brain in the days immediately after injury. Urgent neurosurgical intervention for intracerebral, subdural or extradural haemorrhages can mitigate the extent of secondary injury. Hypoxic or ischaemic injuries also significantly affect recovery and can be either primary or secondary in nature.
Focal injury: Because of the shape of the inner surface of the skull, focal injuries are most commonly seen in the frontal and temporal lobes, but can occur anywhere. Cerebral contusions are readily identifiable on computed tomography (CT) scans, but may not be evident on Day 1 scans, only becoming visible at Days 2 or 3. Deep intracerebral haemorrhages can result from arterial damage from either focal or diffuse damage.
Diffuse injury: Diffuse injury (referred to as diffuse axonal injury, or DAI) is only visible on CT scan in the worst 5%–10% of cases, and most commonly seen as multiple punctate subcortical lesions in and around the corpus callosum and deep white matter and/or as intraventricular haemorrhages. The most consistent effect of diffuse brain damage, even when mild, is the presence of altered consciousness. The depth and duration of coma provide the best guide to the severity of the diffuse damage.8 The majority of patients with DAI will not have any CT evidence to support the diagnosis. Other clinical markers of DAI include high speed of injury, absence of a lucid interval, and prolonged retrograde and anterograde amnesia.
The prognosis for recovery from DAI is different from that for stroke. Long-term studies of recovery from TBI show ongoing improvements for at least 2–5 years after injury.9 Explanations put forward for this difference are mostly speculative, incorporating concepts of various neural repair mechanisms, neuroplasticity and compensatory strategies. Longer-term improvement is thought to be the result of new learning.
Both in the acute stage and later rehabilitation, management is individualised to the person's particular pattern of deficits or disabilities. However, some broad outcomes to guide rehabilitation planning can be inferred from relatively simple injury severity markers.
The Glasgow Coma Scale (GCS). The GCS generates a score between 3 and 15 based on a person's abilities in eye opening and motor and verbal function. It is a quick and easy tool used to assess the severity of traumatic brain injury in the acute setting. The GCS gives a prognosis for survival rather than for functional outcomes.
Post-traumatic amnesia (PTA). The duration of PTA is the best indicator of the extent of cognitive and functional deficits after TBI. PTA is defined as that period of time in which the brain is unable to lay down continuous day-to-day memory. In Australia, the most common means of assessing PTA is the Westmead PTA Scale.10 The duration of PTA can be used as a guide to outcome (Box 1), and correlates well with the extent of DAI and with functional outcomes. For example, one study found 80% of patients with a PTA duration of less than 2 weeks had a good recovery, compared with 46% for those with a PTA duration between 4 and 6 weeks.11 Patients with additional hypoxic or ischaemic injury had a worse outcome for the same duration of coma.
The effects of TBI can be far-reaching and profound (Box 2). While TBI can cause long-term physical disability, it is the complex neurobehavioural sequelae that produce the greatest disruption to quality of life. Cognitive and behavioural changes, difficulties maintaining personal relationships and coping with school and work are reported by survivors as more disabling than any residual physical deficits.1
As with all rehabilitation, the goal is to help the person achieve the maximum degree of return to their previous level of functioning. TBI rehabilitation is best managed by a specialised interdisciplinary team of health professionals (Box 3); although such specialised teams are available in all regions of Australia, some States have more comprehensive services than others. TBI rehabilitation often consists of two phases — inpatient and community management.
Community rehabilitation follows discharge from an inpatient rehabilitation service. Helping a person with TBI return to maximum independence and participation in the community is an extremely difficult task. Family support, education and counselling are vital and likely to be needed for a prolonged period (see Case history, page 2945). The quality and availability of community services can be less than ideal and issues of cost may limit access. This applies particularly to adapted lifestyle-sustaining services.
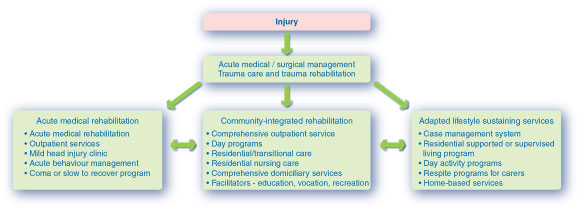
The flowchart (Box 4) shows a US model of care for people with TBI, listing program options for each stage of care. The arrows show the dynamic nature of the model, with the possibility of moving from one program to another as the person's needs change.12
Producing a global outcome measure after TBI is extremely difficult. Acute studies have traditionally used the Glasgow Outcome Scale with its broad categories of persistent vegetative state, severe disability, moderate disability and good recovery.13 This tool is too insensitive for use in rehabilitation, where the significant issues relate to functioning — how does the person function in self-care, and in daily activities in the community, at work or in the family? Are the disabilities physical, cognitive, behavioural or a result of psychological responses to these changes? Outcome measures exist for all of these areas.2 However, there are few evidence-based recommendations to guide TBI rehabilitation (see Evidence-based recommendations, page 294).
It is estimated that 70%–85% of all traumatic brain injuries fall into the mild category. While they rarely require inpatient rehabilitation, patients commonly report cognitive and behavioural changes from which they recover within 3–6 months;17 10%–15% remain symptomatic in the longer term with a persisting post-concussion syndrome: physical complaints including headache, cervical pain, vestibular symptoms; changes in taste and hearing; difficulty with attention and memory; and irritability, insomnia and sleeping difficulties. Interpersonal relationships and work may also be affected. This large group of people with TBI can face many years of impairment, possibly affecting health, education, occupation, and social and emotional functioning.18,19 Treatment involves patient and family education, reassurance and psychological support (see Case history).
Patients within these categories show a broad range of possible outcomes, and it is generally not possible to predict the extent of recovery in the initial weeks after the trauma. Many patients with a dire early prognosis successfully return to competitive employment. Most will be independently mobile and be physically, if not cognitively, capable of self-care and normal community living.
Determining the combination of cognitive, behavioural and physical deficits is an important first step in setting goals for rehabilitation. Prioritising goals should be undertaken with the assistance of both the person and their family. Patients for whom there is no support, or for whom such support is inadequate or inappropriate, fare worse despite the degree or type of rehabilitation.
Social disability. A combination of deficits leads to a greater degree of social disability than would be expected from isolated single deficits. Neuropsychological assessments can help to delineate the extent and type of cognitive disability that a person may experience. This information can be used to help develop individualised compensatory strategies. Community living skills, domestic and household duties, communication (reading, writing, using the telephone), money management, time management, driving and public transport and social skills may require retraining. TBI can affect competency to make important financial decisions, to comply with medical management, to give informed consent, and to make other life decisions. An order to appoint a guardian or administrator may be required in specific situations. Guardianship boards or tribunals operate in all States and Territories of Australia [Contact information — ACT, (02) 6217 4283; NSW, (02) 9555 8500; NT, (08) 8899 2609; QLD, 1300 780 666; SA, (08) 8269 7575; TAS, (03) 6233 3085; VIC, 1800 123 155, (03) 9628 9900; WA, (08) 9278 7350. Contact information for all States and Territories is available at: <http://www.justice.qld.gov.au/guardian/gaat/contact.htm>].
Retraining and reskilling. Return to work is an important factor that contributes to satisfaction and quality of life. On first returning to the community, people with TBI may have reduced awareness of their cognitive deficits, and can fail or do badly if pressured to return to work, study or household responsibilities too soon. Vocational and leisure options may include retraining, reskilling, on-the-job training or supported employment services.
Behavioural management. Behavioural changes may alienate family and friends, with families sometimes perceiving the person as a "difficult stranger". Aggression, substance misuse or lack of empathy particularly strain relationships for others, who may see the patient as unmotivated and lazy. Ignorance and misperceptions of families, coworkers and healthcare professionals about the effects of TBI may make matters worse. Behavioural management may be necessary to increase independence and reduce maladaptive social behaviour: agitation, irritability, combative outbursts, lethargy and abnormal or foul language.
Drug therapy. Drugs are sometimes useful in the management of traumatic brain injury, particularly for mood disorders, such as depression and anxiety. Regaining insight into the changes caused by TBI is often accompanied by an increase in depressive symptoms. Depression is common following TBI, with a reported prevalence of 10%–60%.20 Increased suicidal ideation has also been reported to occur for many years after TBI.
The newer antidepressants, such as the selective serotonin reuptake inhibitors (SSRIs), are most commonly used. Mood stabilisers (eg, carbamazepine and sodium valproate) can be used to reduce the anger dyscontrol sometimes exhibited by those with executive dysfunction. When anticonvulsant medication is required, phenytoin is not commonly used owing to its adverse cognitive effects, but carbamazepine and sodium valproate can be used. Dopaminergic and psychostimulant drugs have also been reported to be useful in a variety of specific post-TBI syndromes. However, as with all psychotropic medication, care must be taken to monitor the possible increased risk of seizures and reduced cognition.
Traditionally, children have been reported to have better outcomes than adults after TBI. However, while fewer focal deficits may be apparent, children appear to develop blunting across all areas of higher cognitive functioning. These deficits may not become apparent until later in the child's development. Children with TBI face difficulties because of impaired new learning, inability to take on social cues, and behavioural, educational and schooling problems.21 These problems pose difficulties for parents, teachers and healthcare workers. There may be a poor fit between the needs of children with TBI, and typical school educational programs. Parents are faced with many challenges, including coping with changed academic aspirations for their child. Specialist paediatric brain injury rehabilitation services are available in Victoria, South Australia, Queensland and New South Wales.
TBI is a heterogeneous disorder of major public health significance. Rehabilitation services, matched to the needs of people with TBI, as well as community-based non-medical services, are required to optimise outcomes over the course of recovery. Both the person with TBI and their social support networks should have access to rehabilitation services through the entire course of recovery, which will continue for many years after the injury. The services required will alter as the person's needs change over time. Survivors of severe TBI face the challenge of resuming a meaningful life for themselves and their families. However, severe TBI is not curable, and medical and rehabilitation management may not ultimately be able to provide the improvement desired by the patient and his or her family.
Evidence-based recommendations
Community rehabilitation – Multidisciplinary community rehabilitation after severe traumatic brain injury yields benefits in functioning (E2).15
Seizures – Prophylactic anti-epileptic agents are effective in reducing early seizures in traumatic brain injury, but there is no evidence that they reduce occurrence of late seizures, or have any effect on death and neurological disability (E2).16
Cognitive rehabilitation – Use of prosthetic aids for memory strategies in cognitive rehabilitation is effective (E2).16
Employment – Supported employment and systematic rehabilitation efforts improve the vocation of survivors of traumatic brain injury (E32).16
Injury severity category |
Initial Glasgow Coma Scale |
Duration of post-traumatic amnesia |
|||||||||
Mild |
12–15 |
Less than 24 hours |
|||||||||
Moderate |
9–11 |
1–7 days |
|||||||||
Severe |
3–8 |
1–4 weeks |
|||||||||
Very severe |
— |
More than 4 weeks |
|||||||||
2: Consequences of traumatic brain injury
Neurological impairment (motor, sensory and autonomic)
Motor function impairment – coordination, balance, walking, hand function, speech
Sensory loss – taste, touch, hearing, vision, smell
Sleep disturbance – insomnia, fatigue
Medical complications – spasticity, post-traumatic epilepsy, hydrocephalus, heterotopic ossification
Sexual dysfunction
Cognitive impairment
Memory impairment, difficulty with new learning, attention and concentration; reduced speed and flexibility of thought processing; impaired problem-solving skills
Problems in planning, organising, and making decisions
Language problems – dysphasia, problems finding words, and impaired reading and writing skills
Impaired judgement and safety awareness
Personality and behavioural changes
Impaired social and coping skills, reduced self-esteem
Altered emotional control; poor frustration tolerance and anger management; denial, and self-centredness
Reduced insight, disinhibition, impulsivity
Psychiatric disorders – anxiety, depression, post-traumatic stress disorder, psychosis
Apathy, amotivational states
Common lifestyle consequences
Unemployment and financial hardship
Inadequate academic achievement
Lack of transportation alternatives
Inadequate recreational opportunities
Difficulties in maintaining interpersonal relationships, marital breakdown
Loss of pre-injury roles; loss of independence
3: The rehabilitation team
Patient and patient's family
General practitioner
Rehabilitation medicine physician
Rehabilitation nurse
Allied health professionals: physiotherapist, occupational therapist, speech pathologist, social worker
Neuropsychologist, clinical psychologist
Vocational rehabilitation services and counsellors
Other medical specialties: neurosurgery, orthopaedic surgery
5: Case history
A 32-year-old carpenter sustained a moderate traumatic brain injury in a motor-vehicle accident. Twelve months after the accident, he has mild residual upper-limb spasticity. He lives at home with his girlfriend of 5 years. She reports difficulty coping with his demands because of continuing angry outbursts, irritability and low frustration threshold with everyday life activities. He has not returned to work, and is frustrated about work as well as social issues.
Together with his partner he attends an outpatient consultation. A referral is made to the local traumatic brain injury outpatient unit. An assessment confirms his frustration with social and work issues. He has low self-esteem and mild depression related to feelings of inadequacy since his injury. He feels unable to communicate this to his partner. He has withdrawn from her and his usual circle of friends, as he feels they do not understand his situation. He was a social drinker before his accident, but he admits to recently increasing his alcohol consumption. Before his injury he did not have any psychiatric diagnosis.
The patient and partner agree to attend an outpatient program twice weekly, incorporating sessions with the neuropsychologist and social worker targeting his angry outbursts. He will have individual and group therapy sessions to learn to express anger in a more socially acceptable way and to interact with other people. His GP is contacted, and agrees to reinforce the strategies and monitor progress.
He is given a diary to document the frequency and type of temper episodes and what triggers the episodes. He is advised to avoid triggers, and avoidance strategies are modelled and practised. Complex tasks are simplified to avoid frustration (eg, use of lists). Positive reinforcements and rewards are identified, and his partner is involved in these strategies. He is given calm, consistent feedback by all members of the multidisciplinary team.

He is referred to an occupational therapist, who is asked to liaise with his employer and to discuss work issues, and alternative employment and retraining. He works on improving his attention and concentration span during everyday tasks using computerised cognitive remediation exercises. A return to driving is suggested as a way of improving his feelings of confidence and self-worth. A referral to a drug and alcohol service is made at the patient's request.
A community case manager is appointed and ongoing regular review with his GP and rehabilitation team is arranged. However, his social, cognitive and behavioural disabilities limit insight and compliance with these rehabilitation strategies.
Cognitive remediation using a computer.
Some useful web sites
Brain Injury Association of Queensland: www.biaq.com.au
South West Brain Injury Rehabilitation Service: www.swbirs.nsw.gov.au/resources.htm
Headway Victoria: www.headwayvictoria.org.au/
Brain Foundation Victoria: www.brainfoundation.org.au/links.html
Commonwealth Rehabilitation Service (CRS) Australia: http://www.crsrehab.gov.au/
The Children's Hospital, Westmead: www.chw.edu.au/prof/services/rehab/brain_injury/about.htm
Traumatic Brain Injury National Data Center (USA): www.tbindc.org
- 1. US National Institutes of Health. Rehabilitation of persons with traumatic brain injury. NIH Consensus Statement 1998 Oct 26-28; 16(1): 1-41. Available at: http://consensus.nih.gov/cons/109/109_statement.htm (accessed Jan 2003).
- 2. Rosenthal M, Griffith ER, Bond MR, et al. Rehabilitation of the adult and child with traumatic brain injury. 2nd ed. Philadelphia: FA Davis, 1990.
- 3. Kay T, Harrington DE, Adams R, et al. Definition of mild traumatic brain injury. J Head Trauma Rehabil 1993; 8: 86-87.
- 4. Fortune N, Wen X. The definition, incidence and prevalence of acquired brain injury in Australia. Canberra: Australian Institute of Health and Welfare, 1999. (Catalogue DIS 15.)
- 5. Tate RL, MacDonald S, Lulham JM. Incidence of hospital treated traumatic brain injury in an Australian community. A N Z J Public Health 1998; 22: 419-423.
- 6. Kraus JK, Black MA, Hessol N, et al. The incidence of acute brain injury and serious impairment in a defined population. Am J Epidemiol 1984; 119: 186-201.
- 7. Bell KR, Sandell ME. Brain Injury rehabilitation. Post acute rehabilitation and community integration. Arch Phys Med Rehabil 1998; 79: S21-S25.
- 8. Sandell ME, Bell KR, Michaud LJ. Brain injury rehabilitation. Traumatic brain injury, prevention, pathophysiology and outcome prediction. Arch Phys Med Rehabil 1998; 79: S3-S9.
- 9. Olver JH, Ponsford JL, Curran CA. Outcome following traumatic brain injury: a comparison between 2 and 5 years after injury. Brain Injury 1996; 10: 841-848.
- 10. Shores EA, Marosszeky JE, Sandanam J, et al. Preliminary validation of a clinical scale for measuring the duration of PTA. Med J Aust 1986; 144: 569-572.
- 11. Katz DI. Neuropathology and neurobehavioural recovery from closed head injury. J Head Trauma Rehabil 1992; 7: 1-15.
- 12. Horn LJ. Systems of care for the person with TBI. Phys Med Rehab Clin North Am 1992; 3: 475-492.
- 13. Jennet B, Bond MR. Assessment of outcome after severe brain damage. Lancet 1975; 1: 480-484.
- 14. Powell J, Heslin J, Greenwood R. Community based rehabilitation after severe traumatic brain injury: a randomised controlled trial. J Neurol Neurosurg Psychiatry. 2002; 72: 193-202.
- 15. Schierhout G, Roberts I. Anti-epileptic drugs for preventing seizures following acute traumatic brain injury (Cochrane Review). In: The Cochrane Library, Issue 1, 2003. Oxford: Update Software.
- 16. Chesnut RM, Carney N, Maynard H, et al. Rehabilitation for traumatic brain injury. Rockville, Md: Agency for Health Care Policy and Research. Evidence Report/Technology Assessment 2, 1999: 1-176. Available at: http://hstat.nlm.nih.gov/hq/Hquest/screen/DirectAccess/db/3309 (accessed February 2003).
- 17. Stevens M. Post concussion syndrome. Framingham, Mass: National Head Injury Foundation, 1982. 82-001.
- 18. Mateer CA, D'Arcy RCN. Current concepts and aproaches to management. In: Raskin SA, Mateer CA, editors. Neuropsychological management of mild traumatic brain injury. New York: Oxford University Press, 2000: 3-22.
- 19. Ponsford JL, Willmott C, Rothwell A, et al. Factors influencing outcome following mild traumatic brain injury in adults. J Int Neuropsychol Soc 2000; 6: 568-579.
- 20. Joseph AB, Wroblewski B. Depression, antidepressants and traumatic brain injury. J Head Trauma Rehabil 1995; 10: 90-95.
- 21. Cockrell J. Paediatric brain injury rehabilitation. In: Horn LJ, Zasler ND, editors. Medical rehabilitation of traumatic brain injury. Philadelphia: Hanley and Belfus, 1996: 171-198.





Abstract
Traumatic brain injury (TBI) commonly affects younger people and causes life-long impairments in physical, cognitive, behavioural and social function. The cognitive, behavioural and personality deficits are usually more disabling than the residual physical deficits. Recovery from TBI can continue for at least 5 years after injury.
Rehabilitation is effective using an interdisciplinary approach, and close liaison with the patient, family and carers. The focus is on issues such as retraining in activities of daily living, pain management, cognitive and behavioural therapies, and pharmacological management.
The social burden of TBI is significant, and therefore family education and counselling, and support of patient and carers, is important.
General practitioners play an important role in providing ongoing support in the community, monitoring for medical complications, behavioural and personality issues, social reintegration, carer coping skills and return-to-work issues.